Weapons of Mass Effect/Terror: Content for the Emergency Physician
- Oct 3rd, 2017
- Brandon Roe
- categories:
Authors: Brandon Roe, DO (EM Resident Physician, Lakeland Health), Kristen Whitworth, DO (EM Resident Physician, Lakeland Health), and Jereme Long, DO (EM Attending Physician, Lakeland Health) // Edited by: Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center) and Alex Koyfman, MD (@EMHighAK – EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital)
Introduction
Increasing political tensions, terrorist groups, and general turmoil faced around the world makes the possibility of a biological, chemical, or other attack on American soil a true reality. In the event of such an attack, one must depend on the knowledge, preparedness, and action of Emergency Physicians and others to act in a timely manner in order to care for the injured.
Case presentations
Case 1
A 47-year-old male with no known past medical history presents to your emergency department for fever, chills, cough, and shortness of breath. He felt well up until three days ago when he began to experience a mild cough. His symptoms have progressed and now he is having a difficult time breathing. Further history reveals that he works at a local government office building and several of his colleagues have similar symptoms. During your exam the nurse alerts you that 4 more patients who work in the same office building are checking in for respiratory complaints. The patient reveals that several days ago there appeared to be a strange white powder on a letter he had received.
Initial vital signs reveal Temp 101, BP 110/60, P 110, RR 28, O2 92% on RA
On physical exam he is in mild respiratory distress. He is tachypnic and has rhonchi throughout his left lung. He has no obvious skin lesions.
You feel he is likely septic and begin your work-up to include blood/sputum cultures and CXR.
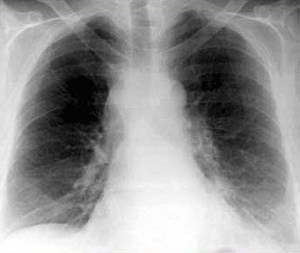
Case 2
You are working an overnight shift when you get a call from EMS. They report that there has been a mass casualty event and over 30 people have been exposed to an unknown gas while waiting at the subway station. They are en route to your facility with the first victim.
EMS arrives with a 30 yo F who is in obvious distress. She has profuse secretions coming from her eyes, nose, and mouth. You notice she has profound weakness during your exam. While you and your staff obtain vital signs and place her on the monitor she begins to seize.
Diagnosis: Sarin Toxicity
Background
The use of Weapons of Mass Destruction (WMD) has been around for ages and was primarily used during times of war by the military. Previously, it has been thought that the use of this type of weapon on a civilian population would be inconceivable, but now we know that the threat does indeed exist. Several attacks have occurred including but not limited to the use of Sarin by Syria from 2013-2017, and anthrax laced letters dispersed throughout the United State’s eastern coast in 2001(1). Although an average emergency physician will see hundreds to thousands of patients with chest pain, he or she may never see a case of anthrax or any victim of a WMD. However, since the possibility exists, those on the front lines of medical care need to be prepared and proficient.
Weapons of Mass Destruction can be broken down into several categories. The military uses the acronym CBRNE: Chemical, Biologic, Radiologic, Nuclear, and Explosive (1). In this review article we will focus on the most common types of WMDs.
Biological weapons
The development of biologic weapons began about a century ago. By WWII, biologic weapons research programs around the world were booming with field testing of the bubonic plague in Japan, and the weaponization of anthrax and botulinum toxin in the USA (2,3). Britain also had an active anthrax program. The Geneva Protocol of 1925 prohibited the use of biological weapons, but that did not stop its development in rogue nations. In the 1990’s Iraq had thousands of liters of anthrax spores, botulinum toxin, and aflatoxin which were weaponized into bombs and SCUD missiles (3,4,5).
Biologic weapons can be composed of bacteria, fungi, viruses, or toxins derived from microorganisms. Biologic weapons are broken down into high, moderate, and low risk categories based on the agent’s ability to cause an outbreak, ease of dissemination, and mortality risk. The high-risk group includes anthrax, smallpox, plague, botulism, tularemia, and several viral hemorrhagic fevers. The moderate risk group includes ricin, Q fever, equine encephalitis viruses, and staphylococcal enterotoxin B. (3,6)
In order for us to intervene on potentially disastrous outbreaks, we must avoid early closure and keep an open mind when evaluating our patients. When a disease pattern does not make sense, such as an “influenza” outbreak when it is not flu season, we should think of other possible etiologies. In this section we will focus on a few of the high-risk biologic weapons.
Anthrax
Bacillus anthracis is a spore forming gram positive bacillus which is the culprit for anthrax. B. anthracis is commonly found in soil and generally only causes disease in those with significant exposure to soil such as farmers and ranchers. There are several manifestations of the disease, which include cutaneous, gastrointestinal, and inhalational (3).
Cutaneous anthrax occurs from direct inoculation with anthrax spores into a breakdown in the skin. This form of anthrax represents 95% of naturally occurring cases (3). After inoculation the infected individual develops a painless red macule which ulcerates and becomes a brown-black necrotic eschar. Most lesions heal spontaneously, however 10-20% will advance to septicemia and death (3,7).

Nausea, vomiting, fever, sepsis and GI hemorrhage can result from gastrointestinal anthrax. This occurs when undercooked meat from an infected animal is ingested. Mortality is at least 50% even alongside antibiotic administration (8).
Inhalational anthrax is the most common form in regards to biologic WMD’s. It results when the spores of B. anthracis are aerosolized and inhaled. There is an incubation period of 1-6 days. Shortly thereafter patients develop mediastinitis resulting in fever, malaise, cough, and chest discomfort. This may improve for 1-2 days; however, the disease then progresses to severe respiratory distress, bacteremia, shock, meningitis, and death within approximately 24-36 hours (3,9). The mortality rate was thought to be 100% even with antibiotic administration; although, in the most recent outbreak in 2001, 6 of the 11 people infected survived with antibiotic therapy and supportive care (8,10,11).

Treatment involves antibiotic therapy and supportive care. The antibiotics of choice are Ciprofloxacin or Doxycycline for 60 days. The initial therapy should include hospital admission and IV antibiotics. Patients should receive ciprofloxacin or doxycycline along with 1-2 other antibiotics with activity against anthrax such as rifampin, penicillin, clindamycin, or imipenem. If there are a large amount of affected patients and your hospital is unable to accommodate inpatient treatment, in such a case oral antibiotics are an option for those who are not septic (3,11)
Plague
The plague is a potential biologic weapon that could be aerosolized into a communicable form as there is no available vaccine. Yersinia pestis is a gram negative bacillus found naturally in flea vectors and rodent hosts. It has been particularly deadly and is responsible for over 200 million deaths and 3 major pandemics (3,12,13).
There are three forms of plague: bubonic, septicemic, and pneumonic. Bubonic plague is the most common form. It has an incubation period of 2-10 days followed by fever, malaise, and enlarged lymph nodes known as ‘buboes’. This can progress to the septicemia form in approximately 23% of patients with bubonic plague (13). Arterial thrombosis may occur causing gangrene which led to the pandemics nick-name “The Black Death.” Bubonic plague has a 60% mortality if left untreated (12). Primary pneumonic plague occurs when infected respiratory droplets are inhaled, and could be disastrous if used as a biologic weapon. There is a 2-3 day incubation period followed by cardiovascular collapse. The patients will experience hemoptysis, hematemesis, hemorrhagic diarrhea, and potentially DIC. Pneumonic plague is almost always fatal unless treatment is initiated within 24 hours (14).
Diagnoses can be made with gram stain in addition to cultures of blood, sputum, or lymph node aspirate. Treatment is similar to anthrax with IV Ciprofloxacin or Doxycycline and supportive care being the first line therapy. It is imperative that those with pneumonic plague be isolated with droplet precautions to prevent further spread (3,14).
Botulism
Botulinum toxin is a toxin produced by Clostridium botulinum and has been weaponized by several countries. Aerosolized botulinum toxin is stable, easy to produce, and extremely lethal, all of which makes it a serious threat for use as a biologic weapon (15).
Botulinum toxin inhibits acetylcholine release which causes dysphonia, dysarthria, dysphagia, and diplopia, and ultimately leads to a symmetric descending flaccid paralysis. Treatment is mainly supportive with early airway management as death is usually a result of respiratory failure. Progression of the illness is halted by an antitoxin, which blocks the action of the circulating neurotoxin. The CDC retains a repository from which one is able to obtain the antitoxin (16).
Smallpox
Though smallpox has been thought to be eradicated, the Soviet Union is known to have weaponized the virus, and several countries are thought to have stocks of it. Smallpox is caused by the variola virus, and is known to be very contagious with 20-30 infections per index case, and a 30% mortality in the unimmunized. Transmission is generally due to respiratory droplets or aerosols (3,17,18,19).
Smallpox begins with fever, malaise, headache, and backache following a 12-14 day incubation period. The characteristic rash then develops 2-3 days following the onset of symptoms. Death usually occurs during the second week of the illness (3). Antiviral therapy, including cidofovir and ribavirin, are available; however, these may only be beneficial in the first 1-2 days (17). Rapid post-exposure vaccine has also shown to offer protection over Smallpox. The vaccine initially stopped being utilized in 1980 when the virus was essentially eradicated, but it has since been reinstated. In 2002-2003 military personal and some civilians began receiving vaccinations (20,21).

Viral hemorrhagic fever
Dengue, Lassa, Hanta, Ebola viruses, amongst other viruses that can cause fever, malaise, and increased capillary permeability resulting in bleeding, are potential biologic agents that could be utilized as a weapon. They are all highly contagious through an aerosolized route. Each virus has its own pathophysiology and disease process which is beyond the scope of this review. Treatment is generally supportive but isolation is extremely important as these viruses are acutely contagious (3,22).
Radiation Exposure
Nuclear weapons programs have been around for years, but as of late, the development of more sophisticated nuclear weapons programs is a reality for many countries. This may represent an increased threat to the American people and more reason for us as medical providers to be prepared and knowledgeable about radiation exposure. Radioactive material can be dispersed via “dirty bombs” or radiologic dispersal devices which combine radioactive material and conventional explosives. This could cause blast injuries, radiation exposure injuries, and mass hysteria (23,24).
Alpha and beta particles, positrons, neutrons, x-rays, and gamma rays are all forms of ionizing radiation that can displace an electron from an atom generating charged particles. These charged particles can then lead to injury. It is important to know the most common types of injuries we are most likely to see from radiation exposure (23,24).
Neutron radiation has variable penetration and can cause whole-body irradiation. It is found in nuclear power plants as well as weapon assembly plants. This irradiation is caused from Gamma particles and X-rays, which can penetrate several centimeters into the tissue. Beta particles can penetrate only millimeters into the skin and are responsible for skin contamination, which can result in serious burns. However, both beta and alpha particles, if exposed internally (i.e. inhalation or ingestion), can cause internal contamination (23,24).
Depending on the level of exposure, radioactive particles can cause interruption of cellular reproduction or cell death with rapidly dividing cells being the most sensitive. The nomenclature and measurement of radiation exposure is cumbersome. As a frame of reference, background radiation exposure is 620 mrem and the acceptable radiation dose limit for the general public is an additional 100 mrem. For reference, 1 CT abd/pelvis = 1000 mrem. The lethal dose of radiation is approximately 350,000-450,000 mrem (23,24).
Radiation exposure can cause many local and systemic side effects. Partial body exposure generally causes local effects such as radiation burns. These types of burns are similar to thermal burns but develop over a longer period of time. Radiation burns are treated similar to thermal burns and may require skin grafting. Acute radiation syndrome can develop after whole body gamma radiation exposure. This syndrome generally develops within 24 hours and has 4 phases: prodrome, latent, manifest illness, and recovery/death. The prodrome phase includes nausea, vomiting, diarrhea, hypotension, fatigue and is dose dependent. The latent phase is a symptom-free phase which is also dose dependent with low doses causing a longer latent period, and the opposite being true for higher doses of exposure. The manifest illness phase includes hematopoietic, GI, CV, and CNS syndromes. Radiation exposure damages bone marrow stem cells causing destruction of hematopoietic cell lines with lymphocytes being the most affected. The lymphocyte count is the best current predictor of radiation exposure severity. Medical management with blood products may improve survival. The initial radiation insult can cause apoptotic death of the GI mucosa inducing vomiting and diarrhea. This can result in massive GI fluid and electrolyte losses. Supportive care with fluid and electrolyte replacement is required. Cardiovascular and CNS syndrome can lead to hypotension unresponsive to conventional treatment causing circulatory collapse within 72 hours of onset. The last phase presumes recovery or death. Recovery can last anywhere from several weeks to two years, whereas those who do not recover can be expected to perish within several months (23).
In the case of a nuclear explosion or mass casualty event, it is important to realize that radiation exposure is not an acute life-threatening event and that those who have sustained traumatic injuries or other acute life threatening problems must be treated first. Personal protective equipment, decontamination, and radiation monitors are important. Protocols should be in place with occasional drills to ensure all personnel are well trained and prepared. Overall, supportive care is the mainstay. Radiation Emergency Assistance Center/Training Site is a resource that can be of assistance in the event of radiation exposure (23).
Chemical agents
Nerve agents
Nerve agents have been used for decades and remain in use today. The most recent use is the use of sarin in the Syrian Civil War in 2013 resulting in 800 civilian casualties (25). Nerve agents such as sarin, tabun, and soman are organophosphate compounds that bind to acetylcholinesterase. These agents were developed and are preferred over insecticide organophosphates due to their increased CNS activity and higher lethality (23,26,27). In the event of an exposure, acetylcholine remains bound to the post synaptic receptor causing excessive cholinergic stimulation resulting in the classic “DUMBELS” presentation with Defecation, Urination, Miosis, Bradycardia / Bronchospasm / Bronchorrhea, Emesis, Lacrimation, and Salivation. Cholinergic overstimulation in the peripheral nervous system causes muscular weakness that can progress to complete paralysis. Seizure and coma develop secondary to cholinergic overstimulation on the brain (23,28).
Treatment should be guided at counteracting cholinergic excess. Large amounts of atropine will be required to counteract the muscarinic effects (DUMBELS). Pralidoxime (2-PAM) should be given to counteract the nicotinic effects (muscle weakness and paralysis). Benzodiazepines should be used in the event your patient has seizures. Treatment will be based on severity and will be patient dependent. Those with low exposure and only eye findings may be treated with atropine eye drops or scopolamine but those with bradycardia, increased secretions or other systemic effects will require intravenous atropine and pralidoxime (23,29,30).
Vesicants
Mustard gas was first used as a chemical warfare agent in World War 1. It was used because it is readily absorbed in the skin causing both local and systemic toxicity. Initial exposure may not induce symptoms for several hours therefore worsening the exposure (23,31).
The symptoms produced by mustard exposure vary by the body areas affected. Exposed skin can lead to severe burning, erythema, and blister formation. Eyes are among the most sensitive to mustard exposure leading to photophobia, ocular pain, conjunctivitis, and ultimately corneal clouding and vision changes. The respiratory system is the next to be affected leading to cough, rhinorrhea, mucus membrane necrosis. Ultimately, severe exposures may lead to respiratory failure. GI symptoms such as nausea, vomiting, and diarrhea as well as CNS symptoms can be present (3,23,33).
Decontamination is the first step in the treatment process. Beyond that, treatment is primarily supportive and will depend on the symptoms present (31).
Explosives and Improvised Explosive Devices
Improvised explosive devices (IED’s) compromise a wide range of explosive devices that are assembled by terrorists with materials readily available or stolen. They can be comprised of either high order or low order explosives or a combination of both. High order explosives are military quality and produce a supersonic over-pressure shock wave. Examples of high order explosives are TNT, C-4, and dynamite. Low order explosives such as gun powder, do not produce this pressure wave. IED’s are often packed with metal objects, such as nails and ball bearings, to inflict maximal damage upon detonation. The severity of injuries from an explosion are determined by the location of the explosion, type and amount of explosive used, the proximity and position of victims in relation to the blast, and if the explosion occurred in an open or closed space.
Injuries related to an explosion are divided into categories including primary, secondary, tertiary and quaternary. Primary injuries are a direct effect of the blast wave from a high order explosive. Injuries are secondary to the rapid air pressure changes and occur at air/fluid interfaces and in gas containing organs. Concussion, globe rupture, bowel perforation, tympanic membrane (TM) rupture, middle ear injury and blast lung injury are examples of primary injuries. Blast lung injury is secondary to tearing of the alveolar-capillary interface and presents similar to acute respiratory distress syndrome (ARDS) or contusion and has a mortality of up to 70% (32). Hemothorax and pneumothorax may be accompanying complications. Pulmonary lacerations can also result in arterial air embolism.
Patients who suffer from primary blast injury are more likely to have greater injuries from secondary and tertiary injuries. Secondary injuries are caused by the impact of airborne debris from the blast wind. The debris may be from the bomb itself or from the environment. These injuries can present as penetrating or blunt trauma and compromise the majority of the injuries of patients presenting to the emergency department (33). Any penetrating trauma should be treated as highly contaminated. Tertiary injuries are caused by a victim being thrown by the blast into an object or from structural collapse. These injuries may present as blunt trauma, crush injuries, fractures, amputations, or head injuries. Emergency physicians should keep complications such as rhabdomyolysis, compartment syndrome and acute kidney injury in mind for those victims with prolonged extrication. Quaternary injuries comprise all other injuries including burns, radiation exposure, inhalation injury, chemical exposure, asphyxia, and exacerbation of chronic disease. Decontamination is of the upmost importance with chemical or radiation exposure. The potential for cyanide and carbon monoxide toxicity should be kept in mind as well.
Triage after an explosion is unique as approximately 50% of victims will arrive in the emergency department in the first hour (33,34). This first wave is composed of the “walking wounded” as the less injured victims bypass EMS and present to the hospital by other means of transportation. The initial number of victims seen can help estimate the remaining causalities and plan for the need for further resources.
ATLS protocol should be followed for victims presenting to the emergency department. Secondary and tertiary injuries may distract from primary blast injuries. Secondary and tertiary surveys should focus on ENT, ocular and neurological examination. While it is classically taught that blast victims with an intact TM are at low risk for primary blast injuries, one study found that an intact TM missed up to 50% pts with PBI to the lung (35). A perforated TM should, however, raise suspicion for additional primary blast injuries. Any patient with a tympanic membrane rupture or complaint of chest pain or shortness of breath should receive a chest x-ray to assess for blast lung injury. Even if the chest x-ray is unremarkable, observation should be considered as blast lung injury may present up to 48 hours after injury. An arterial blood gas can be helpful as oxygen desaturation may be an early sign of injury. If there is evidence of blast lung injury, provide supplemental oxygen as needed and be cautious with fluid administration to avoid fluid overload. Positive pressure ventilation should be avoided if possible, however if necessary, small tidal volumes and low pressures are preferred to decrease risk of pneumothorax or arterial air embolism (36).
Case Resolutions
Case 1
Due to the presentation and multiple coworkers with similar symptoms you had a high suspicion for inhalational anthrax. You immediately started broad spectrum antibiotics with activity against Bacillus anthraces. Despite adequate resuscitation and treatment, the patient continued to deteriorate requiring intubation with ventilator support as well as vasopressor support. His preliminary blood culture results returned as gram positive bacilli. The patient continued to deteriorate and ultimately died. Due to your astute clinical skills and by immediately alerting the proper authorities of your concern for anthrax, the spread of the disease was quickly contained and the “letter writer” was incriminated.
Case 2
You are suspicious for nerve agent exposure and therefore immediately begin decontamination in order to prevent further exposure and keep you and your staff safe. You contact local authorities and report your concern. Intravenous access is established and the seizure is aborted with a benzodiazepine. Atropine and Pralidoxime are also administered due to your concern for nerve agent exposure. The patient ultimately requires intubation due to frequent apneic episodes and her excessive secretions. She is transferred to the ICU and recovers over the next several days. The other exposed patients are divided between all the nearby hospitals and treated similarly. The subway was evacuated and the perpetrator was arrested.
Key Points
- Weapons of Mass Destruction include: Chemical, Biologic, Radiologic, Nuclear, and Explosive (CBRNE).
- Recognizing patterns of symptoms or groups of patients with similar symptoms will help you identify when a WMD has been used.
- Early identification is key in limiting the spread of exposure when dealing with WMD.
- Decontamination is priority in order to limit further exposure and protect you and your hospital staff.
- Periodically take time to review signs, symptoms, and treatments so you will be prepared to take care of patients affected by WMD.
This post is sponsored by www.ERdocFinder.com, a supporter of FOAM and medical education, who with their sponsorship are making FOAM material more accessible to emergency physicians around the world.
References/Further Reading
- Schultz, C. H., Koenig, K.L.: Weapons of Mass Destruction. In Marx, J. A., & Rosen, P. Rosen’s emergency medicine: Concepts and clinical practice, 8e (pp 2469-2478). Philadelphia, PA: Elsevier/Saunders;2010
- Harris S: Japanese biological warfare research on humans: a case study of microbiology and ethics.Ann N Y Acad Sci. 1992;666:21–52.CrossRef [PubMed: 1297279]
- Suchard JR. Biological Weapons. In: Hoffman RS, Howland M, Lewin NA, Nelson LS, Goldfrank LR. eds.Goldfrank’s Toxicologic Emergencies, 10e New York, NY: McGraw-Hill;2015. http://accessemergencymedicine.mhmedical.com/content.aspx?bookid=1163§ionid=65103493. Accessed September 04, 2017.
- Seelos C: Lessons from Iraq on bioweapons. 1999;398:187–188.CrossRef [PubMed: 10094038]
- Zilinskas RA: Iraq’s biological weapons: the past as future? 1997;278:418–424.CrossRef [PubMed: 9244334] [JAMA and JAMA Network Journals Full Text]
- Centers for Disease Control and Prevention: Biological and chemical terrorism: strategic plan for preparedness and response. MMWR Morbid Mortal Wkly Rep.2000;49(RR04):1–14.
- McGovern TW, Christopher GW, Eitzen EM: Cutaneous manifestations of biological warfare and related threat agents.Arch Dermatol. 1999;135:311–322. [PubMed: 10086453][Archives of Dermatology Full Text]
- Friedlander AM: Anthrax. In: Sidell FR, Takafuji ET, Franz DR, eds: Medical Aspects of Chemical and Biological Warfare. Washington, DC: Office of the Surgeon General; 1997:467–478.
- Centers for Disease Control and Prevention: Notice to readers: considerations for distinguishing influenza-like illness from inhalational anthrax. MMWR Morbid Mortal Wkly Rep.2001;50:984–986.
- Franz DR, Jahrling PB, Friedlander AM et al.: Clinical recognition and management of patients exposed to biological warfare agents. 1997;278:399–411.CrossRef [PubMed: 9244332] [JAMA and JAMA Network Journals Full Text]
- Inglesby TV, O’Toole T, Henderson DA et al.: Anthrax as a biological weapon 2002: updated recommendations for management. 2002;287:2236–2252.CrossRef [PubMed: 11980524] [JAMA and JAMA Network Journals Full Text]
- McGovern TW, Christopher GW, Eitzen EM: Cutaneous manifestations of biological warfare and related threat agents. Arch Dermatol. 1999;135:311–322. [PubMed: 10086453][Archives of Dermatology Full Text]
- McGovern TW, Friedlander AM: Plague. In: Sidell FR, Takafuji ET, Franz DR, eds: Medical Aspects of Chemical and Biological Warfare.Washington, DC: Office of the Surgeon General; 1997:479–502.
- Franz DR, Jahrling PB, Friedlander AM et al.: Clinical recognition and management of patients exposed to biological warfare agents. 1997;278:399–411.CrossRef [PubMed: 9244332] [JAMA and JAMA Network Journals Full Text]
- Arnon SS, Schechter R, Inglesby TV et al.: Botulinum toxin as a biological weapon: medical and public health management. 2001;285:1059–1070. CrossRef [PubMed: 11209178] [JAMA and JAMA Network Journals Full Text]
- Geyer HL. In: Hoffman RS, Howland M, Lewin NA, Nelson LS, Goldfrank LR. eds. Goldfrank’s Toxicologic Emergencies, 10e New York, NY: McGraw-Hill; 2015. http://accessemergencymedicine.mhmedical.com/Content.aspx?bookid=1163§ionid=65094000. Accessed September 04, 2017.
- Henderson DA, Inglesby TV, Bartlett JG et al.: Smallpox as a biological weapon: medical and public health management. 1999;281:2127–2137.CrossRef [PubMed: 10367824] [JAMA and JAMA Network Journals Full Text]
- McClain DJ: Smallpox. In: Sidell FR, Takafuji ET, Franz DR, eds: Medical Aspects of Chemical and Biological Warfare.Washington, DC: Office of the Surgeon General; 1997:539–559.
- Eichner M: Case isolation and contact tracing can prevent the spread of smallpox.Am J Epidemiol. 2003;158:118–128. CrossRef [PubMed: 12851224]
- Centers for Disease Control and Prevention: Secondary and tertiary transfer of vaccinia virus among US military personnel—United States and worldwide 2002-2004. MMWR Morbid Mortal Wkly Rep.2004;53:103–105.
- Centers for Disease Control and Prevention: Update: adverse events following civilian smallpox vaccination—United States 2004. MMWR Morbid Mortal Wkly Rep.2004;53:106–107.
- Borio L, Inglesby T, Peters CJ et al.: Hemorrhagic fever viruses as biological weapons: medical and public health management. 2002;287:2391–2405.CrossRef [PubMed: 11988060] [JAMA and JAMA Network Journals Full Text]
- Lopez AM, Stephani JA. Radiation Injuries. In: Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds.Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016. http://accessemergencymedicine.mhmedical.com/content.aspx?bookid=1658§ionid=109426307. Accessed September 04, 2017.
- Anderson PD, Bokor G: Nuclear and radiological terrorism: continuing education article.J Pharm Pract 26: 171, 2013. [PubMed: 23492820]
- Dolgin E: Syrian gas attack reinforces need for better anti-sarin drugs.Nat Med 19: 1194, 2013. [PubMed: 24100968]
- Brennan RJ, Waeckerle JF, Sharp TW, Lillibridge SR: Chemical warfare agents, emergency medical and emergency public health issues.Ann Emerg Med 34: 191, 1999. [PubMed: 10424921]
- Sidell FR, Borak J: Chemical warfare agents: II. Nerve agents.Ann Emerg Med 21: 865, 1992. [PubMed: 1610046]
- Walter FG (ed): Advance Hazardous Life Support Provider Manual. Tucson, AZ: Arizona Board of Regents, 2014.
- Sidell FR, Takafuji ET, Franz DR (eds): Textbook of Military Medicine, Part I: Warfare, Weaponry and the Casualty, Medical Aspects of Chemical and Biological Warfare. Washington, DC: Office of the Surgeon General, 1997.
- Lee EC: Clinical manifestations of sarin nerve gas exposure.JAMA 290: 659, 2003. [PubMed: 12902371] [JAMA and JAMA Network Journals Full Text]
- Wattana M, Bey T: Mustard gas or sulfur mustard: an old chemical agent as a new terrorist threat. Prehosp Disaster Med 2009;241:19–29 [PubMed: 19557954]
- Borak J, Sidell FR: Agents of chemical warfare: sulfur mustard.Ann Emerg Med.1992;21:303–308.CrossRef [PubMed: 1536492]
- Mallonne S, Shariat S, Stennies G, et al. Physical injuries and fatalities resulting from the Oklahoma City bombing. 1996;276(5):382–387.
- Garner J, Brett SJ. Mechanisms of injury by explosive devices. Anesthesiol Clin.2007;25(1):147–160.
- Gutierrez de Ceballos JP, Fuentes FT, Diaz DP, et al. Casualties treated at the closest hospital in the Madrid, March 11, terrorist bombings. Crit Care Med.2005;33(1 suppl):S107–S112.
- Peters P. Primary blast injury: an intact tympanic membrane does not indicate the lack of a pulmonary blast injury. Mil Med. 2011 Jan;176(1):110-4.
- Sorkine P, Szold O, Kluger Y, et al. Permissive hypercapnia ventilation in patients with severe pulmonary blastJ Trauma. 1998;45(1):35–38.
- US Department of Health and Human Services: Radiation Emergency Medical Management, https://www.remm.nlm.gov/index.html. Accessed Sept 5, 2017.
Image Credits
Image 1: CXR showing hilar fullness http://img.medscape.com/fullsize/migrated/editorial/clinupdates/2003/2427/nierengarten.fig1.jpg
Image 2: Smallpox rash
Suchard JR. Biological Weapons. In: Hoffman RS, Howland M, Lewin NA, Nelson LS, Goldfrank LR. eds. Goldfrank’s Toxicologic Emergencies, 10e New York, NY: McGraw-Hill;2015. http://accessemergencymedicine.mhmedical.com/content.aspx?bookid=1163§ionid=65103493. Accessed September 04, 2017.
Image 3: Black eschar of necrotic tissue seen in cutaneous anthrax. http://www.infectionlandscapes.org


One thought on “Weapons of Mass Effect/Terror: Content for the Emergency Physician”