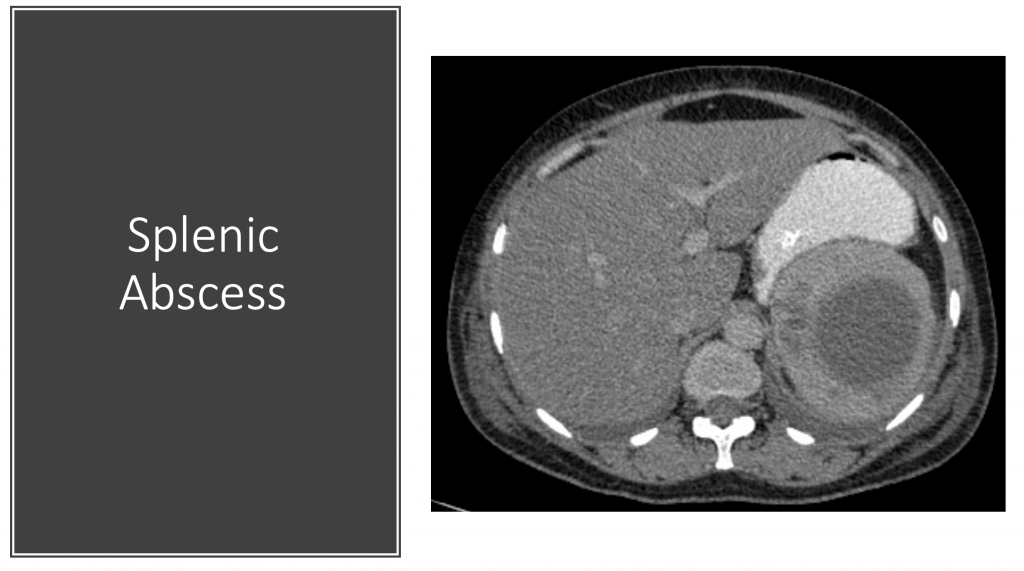
Splenic Abscess: ED Presentation, Evaluation, and Management
A splenic abscess can be a difficult disease to diagnose. This post from Alec Pawlukiewicz provides you with pearls and pitfalls in the evaluation and management of this condition.
Splenic Abscess: ED Presentation, Evaluation, and Management Read More »