Authors: Paolo N. Grenga, MD (EM Resident Physician, University of Rochester Emergency Medicine Residency), Ryan P. Bodkin, MD (EM Program Director, University of Rochester Emergency Medicine Residency), Jason M. Rotoli, MD (EM Assistant Program Director, University of Rochester Emergency Medicine Residency), and Howard Silberstein, MD (Associate Professor of Neurosurgery, Pediatrics, Neurology, Orthopedics) // Edited by: Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center) and Alex Koyfman, MD (@EMHighAK – EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital)
Case
A 9-year-old male is brought to the pediatric emergency department by his mother with complaints of headache and vomiting. He has a history of medulloblastoma for which he has had radiation therapy and resection with remission on recent MRI and has a VP shunt for persistent hydrocephalus. He has normal vital signs, is afebrile and is in mild discomfort but non-toxic appearing.
CSF Shunts: An Overview
Placement of a CSF shunt is a surgical option for management of hydrocephalus. Knowledge of the structure and function of CSF shunts is important to know before evaluating them for possible malfunction or infection. These systems typically include a ventricular catheter, a reservoir, valve and distal tubing. The ventricular catheter routes CSF away from the ventricles to the shunt tubing, which can terminate in the peritoneum (most commonly), right atrium or other distal sites. The valve dictates the pressure at which CSF flow. The reservoir provides access to the shunt system for diagnostic access and measurement of CSF pressure and sampling [1,2].

CSF Shunt Complications – Shunt Failure and Shunt Infection
Causes of CSF Shunt Failure
Shunt failures occur in ~14% of children within the first month and ~50% within the first year of placement. Signs and symptoms with high positive predictive value (PPV) for shunt failure include nausea and vomiting (PPV 79%), irritability (PPV 78%), decreased level of consciousness (PPV 100%) and bulging fontanelle (92%). For a given patient, each episode of shunt failure tends to be characterized by similar symptoms [3]. What, though, does shunt failure actually mean?
Undershunting
Undershunting is often caused by occlusion of shunt flow, which can occur by multiple mechanisms. Intra-luminal obstruction can occur from blood, brain, inflammatory cells from infection or tumor. Extraluminal obstruction from disconnection, kinking or fracture of the shunt system may also occur.
Undershunting can result in high intracranial pressure (ICP). Acute symptoms of high ICP include headache, nausea, vomiting, lethargy, ataxia and rarely, seizures. In infants, symptoms may include apnea, bradycardia or irritability. Acute signs of increased ICP include gaze palsies and decreased visual acuity. Infants with shunt obstruction may display bulging fontanelles or prominent scalp veins [1].
Overshunting
Intracranial hypotension
Also, known as low ICP syndrome, intracranial hypotension is thought to be caused by a siphoning effect by the column of CSF in the shunt tube when the patient is erect [1]. Patients may present with symptoms similar to a spinal headache, except that they are relieved when recumbent [4].
Slit ventricles
“Slit ventricles” refers to complete collapse of the ventricles. While most patients with slit ventricles are asymptomatic, about 12% of all shunted patients will develop slit ventricle syndrome (SVS). The exact pathophysiology of SVS is not completely understood but multiple subtypes of SVS have been described.

It is exceedingly important to note that ventricle size does not necessarily correlate with ICP. Many patients with slit ventricles are asymptomatic. Conversely, patients with normal ventricle size may have increased or decreased ICP.
Subdural hematoma
Subdural hematomas (SDH) may occur due to tearing of bridging veins on brain collapse from overshunting. Patients at increased risk for SDH in this setting include those with craniocerebral disproportion (large head with relatively little brain parenchyma), elderly patients or patients with brain atrophy [1].
CSF Shunt Infection
Children with shunt infections have relatively high morbidity including increased risk of seizures and lower IQ and have mortality rates as high as 15% [1]. Most cases of shunt infection occur within the first six months of surgery [4, 5].
Patients with shunt infections may present with non-specific symptoms including fever, nausea, vomiting, lethargy, anorexia, irritability as well as signs of shunt failure. In pediatric patients 2 months of age or older, the absence of these decreases the likelihood of shunt failure or infection [4]. Neonates may display apneic episodes, anemia, hepatosplenomegaly and stiff neck. Erythema and tenderness along shunt tubing can be associated with infection. Evaluate for signs of intra-abdominal infection, including abdominal tenderness and peritonitis, as the shunt tubing often courses within the peritoneum. In one case series, less than half of all cases of CSF shunt infections were associated with fever. The absence of fever, therefore, does not mean shunt infection is not possible [2].
Causative organisms in decreasing order of incidence include s. epidermidis (50%), s. aureus (20%), gram-negative rods (15%) and Propionibacterium acnes. The highest morbidity and mortality are seen with gram-negative infections. [2,3].
As with any patient, working up a patient for possible shunt infection starts with a thorough history and physical examination. Certain histories may suggest infection at a site that is not the shunt. These include presence of sick contacts with similar symptoms, diarrheal illness (uncommon in patients with shunt infection), symptomatology consistent with otitis media, tonsillitis/pharyngitis, URI/pneumonia, UTI or appendicitis [1]. If the shunt has been present for > 1 year, the shunt tract is normal (I.e. no swelling, erythema or other infectious signs) and an alternative source of the fever is identified, shunt infection is less likely [6].
Case, Continued
The patient continues to complain of headache and nausea. His mother notes that the patient has had the headache for a few days now and that his symptoms appear to worsen as the day progresses. She denies any recent febrile illnesses, sick contacts or trauma. He is neurologically normal, has no photophobia, meningismus or signs of inflammation along his shunt tract. He prefers to lay down.
Could it be the Shunt? Working up CSF Shunt Complications
Differential Diagnosis
When evaluating patients with known CSF shunts, it is important to assess whether the patient’s symptoms are consistent with that expected in shunt failure or shunt infection, outlined above. Note, however, that presentations of CSF complications can be idiosyncratic and may occur in the absence of classical signs of elevated ICP. Note also that shunt infection and shunt failure are two different pathologies, though the former may cause the latter. Presence of one does not guarantee that of the other.
History
Of crucial importance in working up these patients is early involvement of a neurosurgeon. Important historical details to provide them are listed below:

Laboratory Studies [1]
There are no laboratory tests to assess for shunt malfunction. Laboratory tests for shunt infection, however, are similar to those of CNS infection (meningitis, encephalitis, intracranial abscess).
Serum white blood cell count – note that this can be normal in ~ 1/4th of these patients
ESR – tends to be elevated
Blood cultures – positive in < 1/3rd of cases
CSF studies
- WBC – usually not > 100 cells/mm3
- Gram stain – positive 50% of the time
- Protein – tends to be elevated
- Glucose – may be decreased or normal
- Culture – negative in ~40% of cases (though more likely to be positive if WBC > 20K)
- Opening pressure (if there is concern for increased ICP)
Imaging Studies
Shunt Series
The shunt series refers to plain films visualizing the entire course of the VP shunt. This modality is useful for visualizing fractures of the tubing as well as disconnection or migration of the shunt tip. If available, obtain the most recent shunt series for comparison to new studies obtained on ED presentation [1].
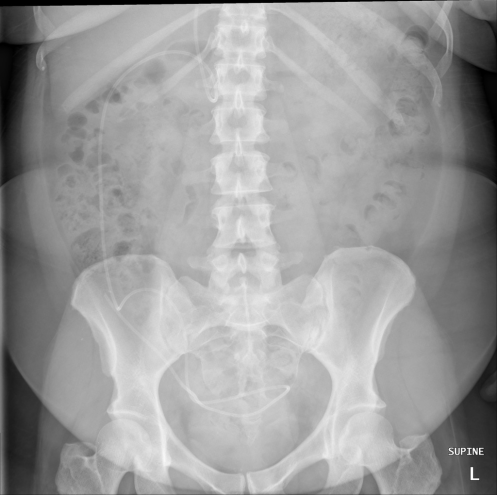

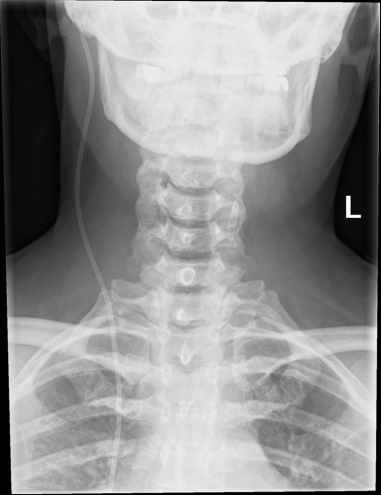
https://radiopaedia.org/cases/normal-shunt-series

http://ep.bmj.com/content/early/2017/01/10/archdischild-2016-311078
Note that disconnection or migration noted on a shunt series does not equate to shunt malfunction. No radiographic test can alone diagnose CSF shunt malfunction [7]. Disconnected shunt may continue to function by CSF flow through fibrous tract [1].
CT
Head CT is often paired with the aforementioned shunt series during ED evaluation for potential CSF shunt malfunction. A retrospective study of over 400 cases of pediatric patients presenting to the ED with symptoms suggestive of possible shunt malfunction showed that 22 patients with normal head CT were found to have a shunt malfunction. The same study also noted that six patients with signs and symptoms suggestive of shunt malfunction had normal head CTs and abnormal shunt series, suggesting that if a head CT is to be obtained in these patients, it should always be accompanied by a shunt series [7]. Another retrospective study, however, notes that the diagnostic yield of shunt series is relatively low in diagnosing shunt malfunction compared to using symptoms + CT and that its added financial costs and increased radiation exposure obviate its use [8].
Note, however, that children with CSF shunts are at elevated risk for malignancies secondary to ionizing radiation exposure. Case studies of patients followed from birth who received dozens of head CTs for shunt surveillance or revisions were later diagnosed with head and neck cancers. Cumulative exposures for these patients were estimated to total ~ 4000 mrems [9]. Care should be taken to proceed with CT imaging only if indicated and to use low-dose CT protocols (i.e. ALARA) when appropriate [3, 10].
MRI
Initial studies suggest that fast-sequence MRI scans can provide high resolution images of the ventricular system but that shunt hardware is difficult to visualize [1,9].
Ultrasound
The optimal method of evaluation in infants with open fontanelles. If the fontanelles are closed, CT may be required [1].
To Tap or Not to Tap?
One question that often arises is whether or not a patient’s shunt needs to be tapped. Indications for tapping a CSF shunt are listed below:

Every shunt system has a finite number of taps it may withstand and there is a risk of introducing infection into the system with every shunt tap. The decision to tap a shunt should be made in consultation with a neurosurgeon and should be deliberately goal directed.
Case, Continued
Your patient’s clinical condition is stable. His headache and nausea improve with symptomatic therapy (Tylenol, Zofran by mouth), though incompletely. Non-contrasted head CT shows appropriately-sized ventricles. His shunt series shows no kinks or disconnects in the system. The on-call neurosurgeon was called prior to obtaining imaging and is en route to evaluate the patient from the OR.
Emergency Department Management [12]
Early consultation with a neurosurgeon is mandatory if there is concern about shunt malfunction or infection.
Shunt Failure
- Neurosurgical emergency
- Rapidly make the diagnosis and involve a neurosurgeon early
- Provide supportive care for elevated ICP, if present
- IV dexamethasone – early ICP reduction
- IV Acetazolamide – ICP reduction over hours
- Emergency reservoir puncture should be done only in consultation with a neurosurgeon
- Hospital admission with neurosurgical consultation
Shunt Infection
- Neurosurgical emergency
- Rapidly make the diagnosis and involve a neurosurgeon early
- Discuss need for LP vs shunt tap with neurosurgeon
- Administer early antibiotics
- Hospital admission with neurosurgical consultation
Case Resolution
The shunt reservoir is tapped by neurosurgery and shows mildly elevated CSF pressures. The patient is admitted overnight to the neurosurgery service and the valve settings adjusted. His headache persisted and worsened, however, requiring shunt revision by upgrading the valve hardware. The procedure is uncomplicated and the patient’s symptoms resolve. He is discharged with neurosurgery follow up on hospital day three.
References / Further Reading
- Greenberg, Mark S. Handbook of Neurosurgery: Seventh Edition. New York: Tieme Publishers New York, 2010.
- Key, Craig B., Rothrock, Steven G., Falk, Jay. “Cerebrospinal fluid shunt complications: An emergency medicine perspective.” Pediatric Emergency Care (1995) 11(5):265-273
- Sivaganesan, A., Krishnamurthy, R., Sahni, D. and Viswanathan, C. “Neuroimaging of ventriculoperitoneal shunt complications in children.” Pediatric Radiology (2002) 42:1029-1046.
- Piatt Jr, Joseph H., Garton, Hugh J.L. “Clinical Diagnosis of Ventriculoperitoneal Shunt Failure Among Children with Hydrocephalus.” Pediatric Emergency Care (2008) 24 (4):201-210
- Rekate, Harold L. “Shunt-related headaches: the slit ventricle syndromes.” Childs Nerv Syst (2008) 24:423-430.
- Kim, Tommy Y., Stewart, G., Voth, M., Moynihan, James A., Brown, L. “Signs and Symptoms of Cerebrospinal Fluid Malfunction in the Pediatric Emergency Department.” Pediatric Emergency Care. (2006) 22(1): 28-34
- Pitetti, Raymond. “Emergency Department Evaluation of Ventricular Shunt Malfunction.” Pediatric Emergency Care (2007) 23 (3): 137-141.
- Shuaib, W., Johnson, J., Pande, V., Salastekar, N., Kang, J., He, Q., Khosa, Faisal Khosa. “Ventriculoperitoneal Shunt Malfunction: Cumulative Effect of Cost, Radiation, and Turnaround Time on the Patient and the Health Care System.” American Journal of Roentgenology. (2014) 202:13-17.
- Smyth, Matthew D., Narayan, P., Tubbs, R. S., Leonard, Jeffrey R., Park, T. S., Loukas, M., and Grabb, Paul A. “Cumulative diagnostic radiation exposure in children with ventriculoperitoneal shunts: a review.” Childs Nerv Syst (2008) 24:493-497.
- “ALARA.” United States Nuclear Regulatory Commission – Protecting People and the Environment. N.p., n.d. Web. 05 Aug. 2017.
- Wallace, Adam N., McConathy, Jonathan., Menias, Christine O., Bhalla, Sanjeev., Wippold II, Franz J. “Imaging Evaluation of CSF Shunts.” American Journal of Roentgenology. (2014) 202:38-53.
- Madsen, Michael A. “Emergency Department Management of Ventriculoperitoneal Cerebrospinal Fluid Shunts.” Annals of Emergency Medicine. (1986) 99-112









4 thoughts on “Complications of CSF Shunts: ED Presentations, Evaluation and Management”
Pingback: Länkar v13-15 | Internmedicin
Pingback: Länkar v13- | Internmedicin
Pingback: March 18th Didactics – Lakeland Health EM Blog
Pingback: Asynchronous Learning March 2023 – Lakeland Health EM Blog