Authors: Samantha LeDonne MD and Debashree Sengupta MD (Emergency Resident Physicians, Icahn School of Medicine at Mount Sinai; @SamanthaLeDonne @Debashree_S) // Edited by: Stephen Alerhand MD (Ultrasound Fellow and Attending Physician, Icahn School of Medicine at Mount Sinai; @SAlerhand) and Manpreet Singh (Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center; @MPrizzleER)
Introduction
The ancestors of today’s ultrasound machines used in the mid-twentieth century were open water-bath scanners. These earliest ultrasound machines involved immersing the human body within a tank made from post-war military surplus materials [1]. Although we have since shifted from water to oil to now ultrasound gel as the conducting medium, water baths can still be helpful in the evaluation of distal extremity injuries.

Ultrasound has an established role in evaluating distal extremity injuries such as abscesses, fractures, or lacerations. To begin with, unlike x-ray, it does not expose patients to radiation, an important consideration when dealing with pediatric patients. According to Javadzadeh et al, water bath ultrasound had higher sensitivity (94.44 CI 74.24–99.01) and specificity (95.24 CI 74.24–99.01) for distal upper extremity fractures when compared with traditional gel ultrasound techniques, which only showed a sensitivity and specificity of 83.33 and 90.48 respectively [2]. Additionally, conventional ultrasound involves placing pressure on the area of interest which can be painful for the patient. Even when a generous amount of ultrasound gel decreases the need for significant pressure during transducer contact, it is still difficult to obtain diagnostic information without causing some discomfort. Moreover, the amount of pressure needed to obtain an image often distorts the superficial soft tissue, making evaluation even more difficult and at times inaccurate[3]. The following two cases illustrate two different ways to evaluate hand pain.
Case #1
42 year old male presents to the ED 12 days after a boxing injury to the right hand, associated with a bite to the 4th digit MCP joint. The patient completed a course of Augmentin, but there continues to be swelling, pain, redness, and warmth to the dorsal aspect of the finger. Hand ultrasound was performed to evaluate for abscess formation. Ultrasound was performed using gel and direct placement of the linear probe over the affected area. The patient complained of increasing pain due to the pressure. Distortion of the tissues made evaluating the size of the fluctuance difficult. An area of echogenicity was visualized deep to the epidermis, with surrounding cobblestoning. Orthopedics (covering Hand) was consulted, and the patient was taken to the OR for incision and drainage and washout.
Case #2
13 year old male presents to the ED with complaints of left 5th digit pain after jamming his finger playing basketball. There is obvious swelling of the digit and pain with manipulation. The patient’s hand was placed in a water bath, and the linear probe was used to evaluate for fracture. The patient remained comfortable throughout the evaluation. A step-off was seen in the proximal portion of the middle segment of the phalanx. X- ray was performed and confirmed the diagnosis of acute traumatic fracture of the left fifth middle phalanx.
Using the Water Bath
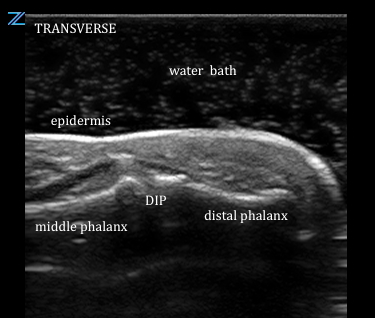
Fill a basin with warm water and have the patient place his/her hand inside. Use the water as a contrast medium. Without actually touching the high-frequency linear transducer (7.5 to 10 MHz) to the patient’s skin, evaluate the body part in question. Make sure to increase the depth of your screen since the water will take up some of the superficial part of the image. This puts the superficial structures of interest within the screen’s focal zone. When evaluating the fingers, begin with a long axis view to better visualize the layers: skin, subcutaneous tissue, tendon, bone. In the transverse view, visualizing multiple fingers simultaneously can help easily differentiate between normal and abnormal [4]. Notice the contrast enhancement and superior diagnostic quality when using the water bath as a medium for sound transmission.




Indications
Shallow skin ulcers (felons)
Subcutaneous masses
Fractures
Osteomyelitis
Foreign body (see prior Emdocs post: http://www.emdocs.net/ultrasound-for-retained-radiolucent-foreign-body-in-soft-tissue/)
Vascular lesions
Tendon injuries
Conclusions
Using water baths for distal extremity ultrasound is a shift back to the original ultrasound machines, but this offers some important advantages. By submerging the patient’s extremity in the water bath, you replace the need for ultrasound gel or contact between the ultrasound transducer and the patient’s skin, thus eliminating discomfort and distortion of the superficial tissue. Using water also avoids compression of these superficial structures. Moreover, this technique may take special importance in the pediatric population, in which providers and parents alike seek to avoid radiation and the patients themselves may not cooperate for the diagnostic tests either.
Ultrasound used in this way can help uncover pathology at the level of the skin, bone, joints, and more. One case study shows how it can help distinguish a felon with a focal fluid collection from a simple cellulitis, thereby saving the patient from an incision [4]. It has been shown to be superior to the standard ultrasound in the evaluation of shallow skin ulcers, subcutaneous masses, vascular malformations, osteomyelitis, and foreign bodies [5]. Interestingly, the water bath method has also been getting attention beyond emergency medicine – there have been some rumors in the OB community about water bath breast ultrasounds replacing screening mammograms [6], and there is at least one case report of a water bath system being used to detect a testicular tumor [7].
Take Home Points
– Ultrasound of the extremity is useful for evaluation of numerous pathologies including: laceration, foreign body, tendon injury, abscess, and fracture.
– Distal extremity ultrasound can be challenging due to patient discomfort and distortion of superficial structures from direct transducer contact.
– Use of water bath mitigates the need for direct contact with the area of interest, leading to higher quality images and less patient discomfort.
The authors wish to acknowledge Dr. Ee Tay for her ultrasound teaching and mentorship.
References/Further Reading:
- “Soundwave Portrait in the Flesh.” LIFE, 20 Sept. 1954, pp. 71–72.
- Javadzadeh HR, Davoudi A., Davoudi F. et al. Diagnostic value of “bedside ultrasonography” and the “water bath technique” in distal forearm, wrist, and hand bone fractures. Emerg Radiol (2014) 21: 1. https://link.springer.com/article/10.1007/s10140-013-1161-5
- Blaivas M, Lyon M, Brannam L, Duggal S, Sierzenski P. Water bath evaluation technique for emergency ultrasound of painful superficial structures. Am J Emerg Med. 2004 Nov;22(7):589-93.
- Butts C. Tips for Assessing Hands and Feet with Ultrasound. Emergency Medicine News. Jul 2016. http://journals.lww.com/em-news/blog/PhotographED/Pages/post.aspx?PostID=136
- Krishnamurthy R, Yoo JH, Thapa M, Callahan MJ. Water-bath method for sonographic evaluation of superficial structures of the extremities in children. Pediatric Radiology. March 2013, 43,1:41–47. https://link.springer.com/article/10.1007/s00247-012-2592-y.
- Waknine Y. FDA Approves 3-D Breast Ultrasound Device. http://www.medscape.com/viewarticle/818992. Medscape. January 10, 2014.
- Bockrath JM, Schaeffer AJ, Kies MS, Neiman HL. Ultrasound identification of impalpable testicle tumor. J Urol. 1983 Aug;130(2):355-6.







