Authors: Scott Fitter, PharmD, BCCCP (Clinical Pharmacy Specialist-ED, Loma Linda University Medical Center, Assistant Professor, Loma Linda University School of Pharmacy); Kimberly Won, PharmD, BCCCP, (Assistant Professor- Department of Pharmacy Practice, Chapman University School of Pharmacy); Kayvan Moussavi, PharmD, BCCCP (Assistant Professor- Department of Pharmacy Practice, Marshall B. Ketchum University College of Pharmacy) // Reviewed by Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Case:
You are working in a rural ED when a 55-year-old, 80 kg male is brought in with sudden onset chest pain. He is diaphoretic and clutching his chest. An EKG shows ST-segment elevations in leads II, III, and aVF. You highly suspect STEMI and begin further workup. Due to an ongoing snowstorm, the closest PCI center is a four-hour drive and three-hour helicopter flight. If this patient were found to have a STEMI, would he be a candidate for systemic thrombolysis?
Introduction:
Mechanism of Action
Thrombolytics (also called fibrinolytics) serve as plasminogen activators (convert plasminogen to plasmin), which break the crosslinks between fibrin molecules to destabilize the structural integrity of blood clots [1-3]. Thrombolytics can be categorized as fibrin non-selective (e.g. urokinase and streptokinase) or fibrin-selective (e.g. alteplase, tenecteplase, reteplase) [1]. Fibrin-non-selective agents degrade both fibrinogen and fibrin, which produces broad lytic action throughout the body [1]. This widespread fibrin degradation and fibrinogen generation (fibrinogenesis) may increase the risk of hemorrhage, thrombosis, and tissue edema [1]. Fibrin-selective agents (also referred to as tissue plasminogen activators [tPA]) convert plasminogen to plasmin more effectively in the presence of fibrin [1,4,5]. A thrombus is composed of fibrin monomers that are cross-linked via lysine side chains [1]. tPA binds to lysine, which helps localize effects to a thrombus, minimize activation of circulating plasminogen, and can decrease unwanted effects (e.g. hemorrhage) [1]. Once bound, tPA catalyzes plasminogen conversion to plasmin by cleaving an arginine-valine bond [1]. This leads to plasmin break down of a clot by degrading the fibrin matrix of the thrombus [1].
Available Agents
Currently or previously available thrombolytics in the United States include the first-generation agents urokinase (Kinlytic™) and streptokinase, second generation tPA alteplase (Activase®), and third generation tPA agents tenecteplase (TNKase®) and reteplase (Retavase®) [1]. Although streptokinase (not available in United States) and urokinase may be less costly than newer agents, their lack of specificity and less favorable adverse effect profiles (i.e. higher risk of hemorrhage) limits their clinical utility [1-3]. Therefore, this article will primarily focus on newer agents (e.g. alteplase, tenecteplase, reteplase).
Indications
Current labeled indications for thrombolytics include [5-7]:
- Acute ischemic stroke
- Pulmonary embolism
- Acute myocardial infarction
- Catheter clearance
Off-label indications include [8-11]:
- Prevention of limb amputation due to frostbite
- Mechanical prosthetic valve thrombosis
- Clearance of pleural effusions
- Management of plastic bronchitis
Contraindications
Contraindications for the use of thrombolytics vary depending upon their indication [5-7]. In general, thrombolytics should be avoided in the following scenarios [5-7]:
- Active bleeding
- Recent intraspinal surgeries (within 2 months) or head trauma (within 3 months)
- Presence of intracranial conditions that could increase the risk of bleeding
- Known bleeding disorders
- Severe, uncontrolled hypertension (unresponsive to therapy)
- Suspected aortic dissection
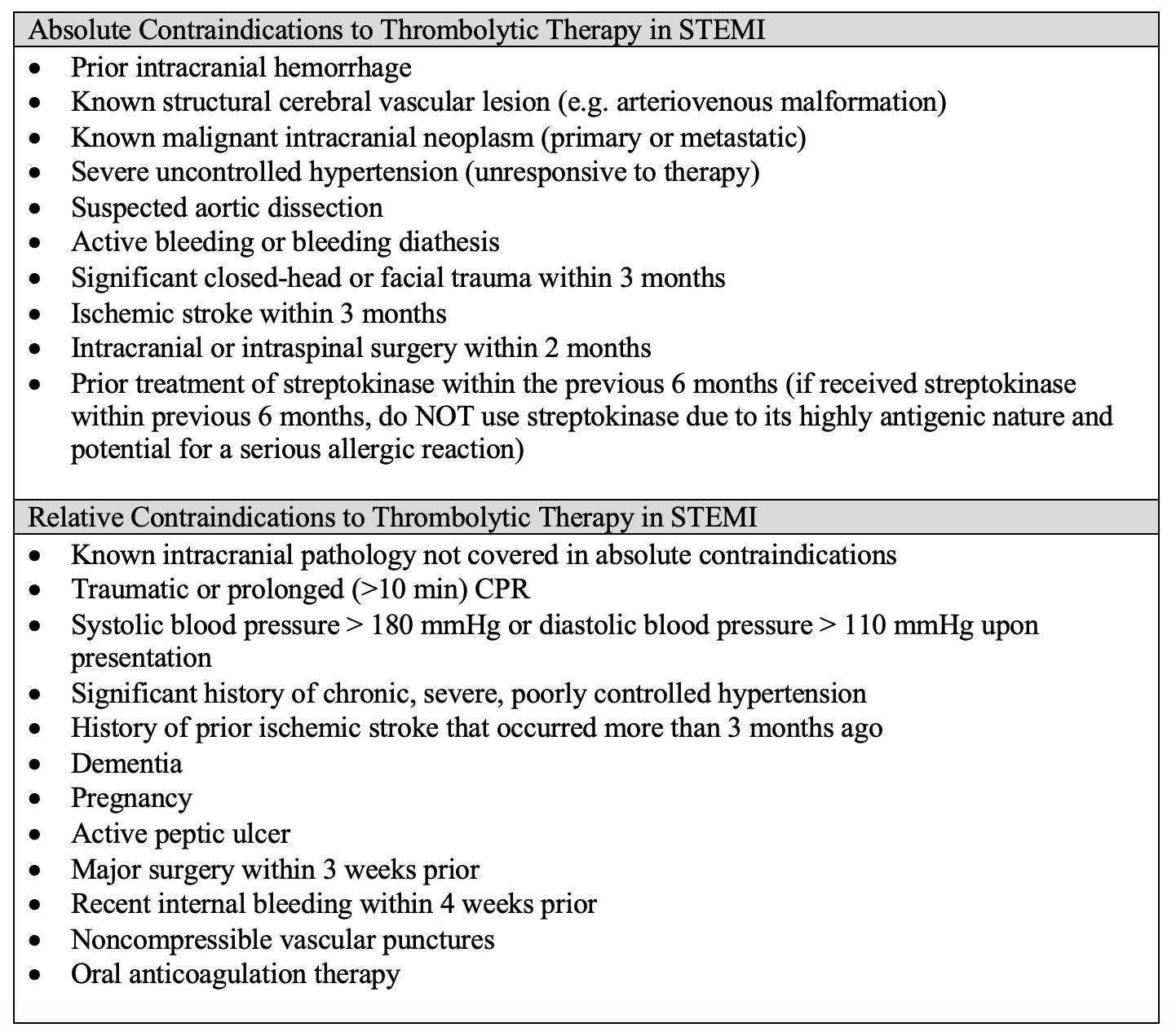
The list of additional relative and absolute contraindications for use of thrombolytics is extensive and primarily relates to the diagnosed condition, severity of symptoms, symptom onset, conditions that increase the risk of bleeding (e.g. recent prior ischemic stroke, gastrointestinal (GI) malignancy or bleed, infective endocarditis, aortic arch dissection, resistant hypertension), coagulopathy, and concurrent anticoagulant or antiplatelet usage (Table 1) [5-7,12-14].
Table 1.
Complications and Their Treatments
Bleeding is the most notable complication associated with the use of thrombolytics [12,15]. Intracranial hemorrhage (ICH) is the most common and most concerning bleeding event, with reported incidence of 1-2% and 2-7% of patients receiving alteplase for acute myocardial infarction and acute ischemic stroke, respectively [15-18]. Bleeding can be internal or external and develop at any site (e.g. GI, genitourinary, arterial or venous puncture, etc.) [5,12]. Additionally, the effects of thrombolytics may persist for longer than expected based on the individual drug half-lives (Table 2) [1,15]. For example, the effects of alteplase on the coagulation system may last for more than 24 hours despite alteplase having a half-life of only 4-8 minutes [1,15]. If life-threatening hemorrhage (e.g. ICH) develops, general acute management recommendations (i.e. within 24 hours of thrombolytic administration) include [4,12,15]:
- Stop thrombolytic infusion
- Order relevant labs or imaging (e.g. CBC, PT/INR, fibrinogen, head CT)
- Administer cryoprecipitate (contains fibrinogen, factor VIII, fibronectin, factor XIII, and von Willebrand Factor) or antifibrinolytic (e.g. tranexamic acid, aminocaproic acid) if cryoprecipitate contraindicated or unavailable
- Order relevant consults (e.g. hematology, neurosurgery)
- Provide supportive care (e.g. blood pressure management, intracranial pressure management, temperature, glucose control)
Table 2: Summary of Thrombolytic Agents
Hypersensitivity, including urticarial or anaphylactic reactions, can also occur after thrombolytic administration [5,12,19]. Angioedema has been observed 5 to 720 minutes after alteplase infusions for the treatment of acute ischemic stroke and acute myocardial infarction; however, median onset is typically 60 minutes [5,20,21]. tPAs like alteplase can increase bradykinin production because plasmin cleaves bradykinin from high-molecular-weight kininogen [22]. Bradykinin can lead to vasodilation, plasma extravasation, and mucosal edema, which characterize angioedema [22]. The incidence of orolingual angioedema secondary to alteplase use ranges from 1.3-5.1% [19,22,23]. Patients using angiotensin-converting enzyme (ACE) inhibitors prior to alteplase may be at higher risk of angioedema, possibly due to ACE inhibitors increasing bradykinin concentrations prior to treatment [19,22]. Severity may range from mild to life-threatening with mild orolingual angioedema typically limited to the anterior tongue and lips and more severe cases involving the larynx, palate, floor of mouth, or oropharynx [12]. Recommendations for management of orolingual angioedema include [12,19,24]:
- Discontinue thrombolytic and hold ACE inhibitors
- Maintain airway
- Edema involving larynx, palate, floor of mouth, or oropharynx with rapid progression (within 30 minutes) poses higher risk of requiring intubation
- Administer methylprednisolone, diphenhydramine, and famotidine
- Administer epinephrine if further increases in angioedema
- Because epinephrine may worsen coronary ischemia due to inotropic and chronotropic effects, consider using routes with less systemic absorption (e.g. nebulization) or less likely to result in inadvertent overdose (e.g. subcutaneous or intramuscular) [12,25]
- Agents used for hereditary or ACE inhibitor-related angioedema (e.g. icatibant, C1 esterase inhibitor) can also be considered
- Supportive care
Thrombolytic Use in STEMI:
Scenarios for Use
Though primary percutaneous coronary intervention (PCI) is the preferred reperfusion strategy for acute ST-elevation myocardial infarction (STEMI), thrombolytic therapy is recommended by the American Heart Association (AHA), American College of Cardiac Foundation (ACCF), American College of Emergency Physicians (ACEP), Society for Cardiovascular Angiography and Interventions, and the European Society of Cardiology (ESC) when a patient, without contraindications to thrombolytic therapy, presents within 12 hours of ischemia symptom onset to an institution without PCI capability, or if the anticipated time that PCI can be performed at a PCI-capable institution is greater than 120 minutes from the first medical contact [13,14,26]. When thrombolytic therapy is administered within 6 hours of symptom onset, it can decrease the incidence of major adverse cardiac events (MACE) and prevent approximately 30 early deaths per 1000 patients [13,14,26,27]. Additionally, the AHA/ACCF and ESC guidelines state that thrombolytic therapy may also be considered for patients who present with ongoing ischemia within 12-24 hours of symptom onset and are hemodynamically unstable or have a large area of myocardium at risk [13,14]. Thrombolytic therapy should NOT be administered to patients with ST depression, except when a true posterior (inferobasal) MI is suspected or when associated with ST elevation in lead aVR [13,27]. Contraindications to use in STEMI are similar to those for other indications (Table 1).
Patients who receive thrombolytic therapy should be immediately transferred to a PCI-capable institution and assessment of reperfusion should be conducted at 60 to 90 minutes post-thrombolytic therapy [13,14]. Lack of resolution of ST elevations is associated with a worse prognosis, and immediate coronary angiography and rescue PCI should be considered in those patients [13,14].
Clinical Pearls and Pitfalls:
Timing and Benefits of Thrombolytic Therapy
If the decision is made for thrombolytic therapy, the thrombolytic agent should be administered as soon as possible, ideally within 30 minutes of first medical contact, since the mortality benefit of fibrinolysis decreases as the time from symptom onset to thrombolytic administration increases [27-31]. The 2017 ESC guideline suggests a goal of 10 minutes from STEMI diagnosis to thrombolytic administration based on findings from the STREAM trial [14,32]. Delays in thrombolytic therapy have been associated with impaired myocardial perfusion grades and poorer epicardial flow grades [28,33]. The greatest benefit of thrombolytic therapy is seen in high-risk patients when the thrombolytic agent is given within 2 hours of symptom onset demonstrated significant reductions in mortality [31,34].
To shorten the symptom onset to thrombolytic administration, some areas allow thrombolytic therapy to be administered in the pre-hospital setting after a STEMI is determined by a 12-lead electrocardiogram [13,14]. Though prehospital thrombolytic therapy is not common in the United States due to lack of resources and specialty-trained emergency medical responders, there are some regions in other countries, including the United Kingdom and Europe, where prehospital thrombolytics are administered due to increase transit times to a PCI-capable facility [13,14,34-40].
Several studies have demonstrated the safety and benefits of administering prehospital thrombolytic therapy for STEMI, including an approximately 60-minute reduction in administering thrombolytic therapy from symptom onset and a 17% risk reduction in all-cause hospital mortality [32,34,35,38,41-47]. In the CAPTIM trial, there was no significant difference in the composite outcome (death, nonfatal reinfarction, and nonfatal disabling stroke within 30 days) or mortality between patients who received PCI or prehospital fibrinolytics [43]. However, a subgroup analysis of the CAPTIM study showed a significantly lower 5-year mortality rate for patients who received thrombolytics within 2 hours of symptom onset compared to primary PCI, but there was no difference in those who received thrombolytics after 2 hours [45]. In contrast, the ASSENT-4 trial, which compared primary PCI versus facilitated PCI (patients received tenecteplase prior to PCI) was stopped early due to it showing a higher in-hospital mortality and higher stroke rate in patients randomized to the facilitated PCI group [48]. Additionally, the STREAM trial, a multicenter, open-label, randomized, parallel-group trial comparing thrombolytic therapy followed by timely coronary angiography to primary PCI reported no difference in the primary end point of 30-day composite death from any cause, shock, congestive heart failure, or reinfarction between the two groups (12.4% vs. 14.3%, p=0.21) [32]. Though the overall rate of intracranial hemorrhage was significantly greater in the fibrinolysis group (1% vs 0.2%, p=0.04), after amending the protocol for a lower dose of tenecteplase in patients 75 years old and greater, the difference between the groups was not statistically significant (0.5% vs. 0.3%, p=0.45) [32]. More recently, the EARLY-MYO trial, a multicenter, randomized noninferiority trial in China comparing early catheterization after half-dose alteplase compared to primary PCI, found that half-dose alteplase plus rescue PCI was noninferior (and even superior) to primary PCI for the primary endpoint of complete epicardial and myocardial reperfusion after PCI (thrombolysis in myocardial infarction [TIMI] flow grade 3) and ST-segment resolution 70% [49].
Adjunctive Agents Given with Thrombolytic Therapy
The 2013 AHA/ACCF and 2017 ESC guidelines recommend that dual antiplatelet therapy with aspirin (162-325 mg loading dose) and clopidogrel (300 mg loading dose in patients <75 years old or 75 mg in patients ≥75 years old) should be administered before or with thrombolytic therapy [13,14]. Aspirin 81 mg daily should be continued indefinitely, and clopidogrel 75 mg daily should be continued for at least 14 days, or one year if patient undergoes rescue PCI after receiving thrombolytic therapy [13]. If patients undergo subsequent PCI after thrombolytic therapy, patients can be switched from clopidogrel to another P2Y12 inhibitor (e.g. ticagrelor, prasugrel) 48 hours after thrombolytic therapy [13]. The TREAT trial, an international, multicenter, randomized, open-label trial that randomized STEMI patients less than 75 years old to receive either ticagrelor or clopidogrel after undergoing thrombolytic therapy, found no difference between groups for the combined outcome of cardiovascular mortality, myocardial infarction or stroke, as well as major, fatal and intracranial bleeding [50]. However, patients who received ticagrelor had a significantly higher rate of any bleeding (10.2% vs. 6.2%; p<0.01), bleeding that required medical attention (3.8% vs. 2.1%; p<0.01), and minimal bleeding based on the TIMI, PLATO, and Bleeding Academic Research Consortium classifications (p<0.01) [50]. These findings further support current recommendations for use of clopidogrel over other P2Y12 inhibitors in patients receiving thrombolytic therapy for acute myocardial infarction [13,14]. Notably, patients older than 75 years were excluded from major trials that established the safety of antiplatelet dosing during thrombolysis [50,51]. In these older patients, providers may wish to skip the loading dose and start with a maintenance dose instead (i.e. administer clopidogrel 75 mg instead of 300 mg) [50,51].
Anticoagulation therapy is also recommended to help improve vessel patency and prevent re-occlusion [13,14]. Anticoagulation with enoxaparin (< 75 years old: 30 mg IV bolus, followed in 15 minutes by 1 mg/kg subcutaneouslyevery 12 hours [maximum of 100 mg for the first 2 doses]; in 75 years old: no IV bolus, 0.75 mg/kg subcutaneously every 12 hours [maximum 75 mg for the first two doses]) or unfractionated heparin (UFH) (60 units/kg loading dose [maximum 4000 units] IV, followed by 12 units/kg/hour IV [maximum initial infusion rate 1000 units/h] adjusted to maintain aPTT 1.5-2 times control) should be given for at least 48 hours or until revascularization, or for the duration of the patient’s hospital stay up to 8 days [13,14]. For anticoagulation therapy extending beyond 48 hours, the ACC/ACCF guidelines recommend enoxaparin due to low molecular weight heparins demonstrating better outcomes compared to UFH [13,52-56]. In the ASSENT-3 trial, patients who received full-dose tenecteplase with weight-adjusted UFH for 48 hours had a significantly higher rate of in-hospital infarction, in-hospital refractory ischemia and non-intracranial hemorrhage bleeding compared those who received full-dose tenecteplase and enoxaparin for 7 days or half-dose tenecteplase with weight-adjusted low-dose UFH plus a 12-hour infusion of abciximab [55]. Compared to UFH, low-molecular weight heparins are less protein-bound and have less platelet activation, thus, making their effects more predictable and potentially more favorable to use in combination with thrombolytic agents [55]. Patients who have a history of heparin-induced thrombocytopenia (HIT) can receive bivalrudin; however, bivalrudin has not been studied with thrombolytic agents [13,14]. Fondaparinux should not be used as the sole anticoagulant for patients referred for PCI and is contraindicated for patients with a creatinine clearance <30 mL/min [13,14]. If patients qualify for fondaparinux use, 2.5 mg IV followed by 2.5 mg subcutaneously daily starting the following day is recommended [13].
Glycoprotein IIb/IIIa (GP IIb/IIIa) inhibitors have been investigated with reteplase, alteplase, and tenecteplase [55,57-62]. Overall, GP IIb/IIIa inhibitors significantly reduce the risk for recurrent infarction, but significantly increase the risk of bleeding and are not recommended for routine adjunct therapy with thrombolytic agents with or without anticoagulants [13,14,29].
Thrombolytic Agents of Choice for STEMI
Streptokinase, tenecteplase, alteplase, and reteplase are all approved for reperfusion therapy in STEMI (streptokinase only available outside the United States) [5-7,63]. The AHA/ACCF and ESC guidelines recommend fibrin-specific agents (e.g. alteplase, reteplase, tenecteplase) over the non-fibrin-specific agents (e.g. streptokinase) due to their associated increased risk of all-cause mortality [13,14,28,29,64]. Details of fibrin-specific agents used for STEMI are summarized in Table 2. In general, fibrin-specific agents have prolonged half-lives compared to streptokinase and are less likely to cause allergic reactions [65]. A large systematic review and network meta-analysis of randomized controlled trials concluded that there was no significant difference in mortality risk between tenecteplase, reteplase or accelerated infusion alteplase plus parenteral anticoagulants; however, streptokinase and non-accelerated infusion alteplase were associated with an increased risk of all-cause mortality [29].
Streptokinase is the proto-typical tissue plasminogen activator (tPA) that was discovered in 1933 [66]. The GISSI and ISIS trials were among the first landmark studies to demonstrate its mortality benefit compared to placebo in AMI [67,68]. Though streptokinase demonstrated a significant decrease in mortality when compared to placebo, it was found to be associated with an increase in all-cause mortality in comparison to other fibrin-specific agents [28,29]. Furthermore, streptokinase is antigenic (i.e. high risk for allergic reaction) and should not be given to a patient who has received streptokinase (or anistreplase) within the prior 6 months due to increased risk of a serious allergic reaction [13,63]. Thus, streptokinase is less preferred for thrombolytic therapy in acute MI if other fibrin-specific agents are available.
Alteplase is a recombinant human tPA that is widely available in the United States [5]. It is fibrin-specific and has FDA-approved indications for STEMI, pulmonary embolism, and acute ischemic stroke [5]. Although alteplase has two FDA-approved dosing strategies for STEMI (90-minute infusion vs 3-hour infusion), the 90-minute infusion (also known “accelerated infusion alteplase”) is more commonly used and recommended by the AHA/ACCF and ESC guidelines due to increased all-cause mortality seen with the 3-hour alteplase infusion (also referred to as “non-accelerated infusion alteplase”) [13,14]. Furthermore, the RAPID I trial demonstrated significantly more rapid, complete and sustained thrombolysis of the infarcted coronary artery with reteplase compared to the non-accelerated infusion alteplase [69]. Accelerated infusion alteplase had a 14% reduction in mortality in comparison to streptokinase plus subcutaneous or intravenous heparin; however, accelerated infusion alteplase was associated with increased risk of bleeding, including a significantly higher report of hemorrhagic strokes [28,29]. The investigators of the Assessment of the Safety and Efficacy of a New Thrombolytic (ASSENT-2) trial found no difference in 30-day mortality between accelerated infusion alteplase and tenecteplase in almost 17,000 patients with an acute STEMI who presented within 6 hours of symptom onset [17].
Of the fibrin-specific agents available, reteplase is the only one that is not weight-based, which may allow for easier dosing. Reteplase is administered as two 10-unit slow IV boluses over 2 minutes that are administered 30 minutes apart [7]. A one-year follow-up of the GUSTO III trial showed no significant differences in mortality between reteplase and accelerated infusion alteplase [70]. However, in the RAPID II trial, reteplase achieved a significantly greater patency (TIMI grade 2 or 3) or complete patency (TIMI grade 3) at 90 minutes compared to accelerated infusion alteplase (83.4% vs 73.3%, p=0.03; 59.9% vs 45.2%, p=0.01, respectively) [71].
Tenecteplase has the shortest administration time and is the most fibrin-specific of the three fibrin-specific agents [6,13,65]. It is administered as one IV bolus over 5 seconds and the selected dose is weight-dependent [6]. For patients 75 years or older, a reduced dose of tenecteplase should be considered [14,26]. In the ASSENT-2 trial, tenecteplase and alteplase had similar reductions in 30-day mortality and rates of intracranial hemorrhage; however, tenecteplase had fewer non-cerebral bleeding and less need for blood transfusions [17]. In comparison to other thrombolytic-based regimens, tenecteplase plus parenteral anticoagulants was associated with a lower risk of all-cause mortality within 30-35 days, as well as major bleeding [29].
Case Resolution:
Further work-up reveals the patient is having a STEMI. Because the nearest PCI center is more than 2 hours away, you feel that fibrinolysis is indicated. Screening reveals that the patient has no contraindications to thrombolytic therapy. Your hospital carries alteplase, so you order an accelerated regimen with a 15 mg IV bolus followed by 50 mg (0.75 mg/kg x 80 kg = 60 mg but maximum for this dose is 50 mg) over 30 minutes, followed by 35 mg (0.5 mg/kg x 80 kg = 40 mg but maximum for this dose is 35 mg) over 60 minutes. You also order aspirin 162 mg orally followed by 81 mg daily, unfractionated heparin (UFH) 4000 units (60 units/kg x 80 kg = 4800 units but maximum for this dose is 4000 units) IV followed by 12 units/kg/hour IV adjusted to aPTT 50-70 seconds (1.5-2 times control at the hospital’s lab), and clopidogrel 300 mg orally followed by 75 mg daily. You contact the nearest PCI center to arrange transport for diagnostic coronary angiography and subsequent monitoring. Fortunately, the storm appears to be easing and the patient is tolerating fibrinolysis with stable vital signs. An ambulance crew will be available to transfer the patient within the next hour.
Take Home Points:
- Thrombolytics (also called fibrinolytics) serve as tissue plasminogen activators (work by converting plasminogen to plasmin), which break the crosslinks between fibrin molecules to destabilize the structural integrity of blood clots.
- Thrombolytics can be useful when treating life-threatening clotting disorders (e.g. acute ischemic stroke, pulmonary embolism, STEMI).
- In general, thrombolytics should be avoided in patients with active hemorrhage or at high risk of hemorrhage in a critical location (e.g. recent spinal or intracranial surgery or trauma).
- Bleeding (internal and external) and hypersensitivity reactions (e.g. angioedema) can occur after thrombolytic administration.
- Non-selective thrombolytics (e.g. urokinase, streptokinase) tend to cause more adverse effects compared to fibrin-selective thrombolytics (e.g. alteplase, tenecteplase, reteplase).
- Thrombolytic therapy for STEMI is recommended if the anticipated time to PCI is greater than 120 minutes from the first medical contact, the patient presents within 12 hours of ischemic symptom onset, and does not have any contraindications to thrombolytic therapy.
- Fibrin-selective thrombolytic agents (e.g. tenecteplase, reteplase, alteplase) are preferred over non-selective agents (e.g. urokinase, streptokinase) for STEMI.
- Patients treated with thrombolytics for STEMI should receive concurrent antiplatelet agents (e.g. aspirin with clopidogrel) and anticoagulants (e.g. enoxaparin, UFH).
- Due to increased risk of bleeding, GP IIb/IIIa inhibitors should not be used with thrombolytics when treating STEMI.
Relevant emDOCs Posts:
http://www.emdocs.net/life-threatening-complications-with-tpa-what-emergency-physicians-should-know/
References:
- Bivard A, Lin L, Parsonsb MW. Review of stroke thrombolytics. J Stroke 2013;15(2):90-8 doi: 10.5853/jos.2013.15.2.90.
- Tanswell P, Modi N, Combs D, et al. Pharmacokinetics and pharmacodynamics of tenecteplase in fibrinolytic therapy of acute myocardial infarction. Clin Pharmacokinet 2002;41(15):1229-45.
- Hilleman DE, Tsikouris JP, Seals AA, Marmur JD. Fibrinolytic agents for the management of ST-segment elevation myocardial infarction. Pharmacotherapy 2007;27(11):1558-70 .
- Frontera JA, Lewin JJ, Rabinstein AA, et al. Guideline for Reversal of Antithrombotics in Intracranial Hemorrhage: A Statement for Healthcare Professionals from the Neurocritical Care Society and Society of Critical Care Medicine. Neurocrit Care 2016;24(1):6-46 doi: 10.1007/s12028-015-0222-x.
- Activase [package insert]. South San Francisco, CA: Genentech, Inc.; 2018.
- TNKase [package insert]. South San Francisco, CA: Genentech, Inc.; 2018.
- Retavase [package insert]. Cary, NC: Chiesi USA, Inc.; 2020.
- Rathjen NA, Shahbodaghi SD, Brown JA. Hypothermia and cold weather injuries. Am Fam Physician 2019;100(11):680-86.
- Lim WY, Lloyd G, Bhattacharyya S. Mechanical and surgical bioprosthetic valve thrombosis. Heart 2017;103(24):1934-41 doi: 10.1136/heartjnl-2017-311856.
- Rahman NM, Maskell NA, West A, et al. Intrapleural use of tissue plasminogen activator and DNase in pleural infection. N Engl J Med 2011;365:518-26.
- Rubin BK. Plastic Bronchitis. Clin Chest Med 2016;37(3):405-8 doi: 10.1016/j.ccm.2016.04.003.
- Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2019;50 doi: 10.1161/STR.0000000000000211.
- O’Gara PT, Kushner FG, Ascheim, DD, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2013;61(4):e78-140 doi: 10.1016/j.jacc.2012.11.019.
- Ibanez B, James S, Agewall S, et al. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J 2018;39(2):119-77 doi: 10.1093/eurheartj/ehx393.
- Yaghi S, Willey JZ, Cucchiara B, et al. Treatment and Outcome of Hemorrhagic Transformation After Intravenous Alteplase in Acute Ischemic Stroke: A Scientific Statement for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke 2017;48(12):e343-e61 doi: 10.1161/STR.0000000000000152.
- Boden WE, Eagle K, Granger CB. Reperfusion strategies in acute ST-segment elevation myocardial infarction: a comprehensive review of contemporary management options. J Am Coll Cardiol 2007;50(10):917-29 doi: 10.1016/j.jacc.2007.04.084.
- Van de Werf F. Single-bolus tenecteplase compared with front-loaded alteplase in acute myocardial infarction: the ASSENT-2 double-blind randomised trial. Lancet 1999;354(9180):716-22 doi: 10.1016/s0140-6736(99)07403-6.
- INJECT Investigators. Randomised, double-blind comparison of reteplase double-bolus adminsitration with streptokinase in acute myocardial infarction (INJECT): trial to investigate equivalence. Lancet 1995;246:329-36.
- Hill MD, Lye T, Moss H, et al. Hemi-orolingual angioedema and ACE inhibition after alteplase treatment of stroke. Neurology 2003;60:1525-27.
- Pinho J, Alves JN, Oliveira L, et al. Orolingual angioedema after thrombolysis is not associated with insular cortex ischemia on pre-thrombolysis CT. J Neurol Sci 2016;369:48-50
- Huford R, Rezvani S, Kreimei M, et al. Incidence, predictors and clinical characteristics of orolingual angio-oedema complicating thrombolysis with tissue plasminogen activator for ischaemic stroke. J Neurol Neurosurg Psychiatry 2015;86:520-23
- Engelter ST, Fluri F, Buitrago-Tellez C, et al. Life-threatening orolingual angioedema during thrombolysis in acute ischemic stroke. J Neurol 2005;252(10):1167-70 doi: 10.1007/s00415-005-0789-9.
- Hill MD, Buchan AM, Canadian Alteplase for Stroke Effectiveness Study Investigators. Thrombolysis for acute ischemic stroke: results of the Canadian Alteplase for Stroke Effectiveness Study. CMAJ 2005;172(10):1307-12 doi: 10.1503/cmaj.1041561.
- Fugate JE, Kalimullah EA, Wijdicks EFM. Angioedema after tPA: what neurointensivists should know. Neurocrit Care 2012;16:440-43.
- Zarar A, Khan AA, Adil MM, et al. Anaphylactic shock associated with intravenous thrombolytics. American Journal of Emergency Medicine 2014;32:113.e3-13.e5.
- Promes SB, Glauser JM, Smith MD, et al. Clinical Policy: Emergency Department Management of Patients Needing Reperfusion Therapy for Acute ST-Segment Elevation Myocardial Infarction. Ann Emerg Med 2017;70(5):724-39 doi: 10.1016/j.annemergmed.2017.09.035.
- Fibrinolytic Therapy Trialists Collaborative Group. Indications for fibrinolytic therapy in suspected acute myocardial infarction: collaborative overview of early mortality and major morbidity results from all randomised trials of more than 1000 patients. Lancet 1994;343:311-22.
- GUSTO Investigators. An international randomized trial comparing four thrombolytic strategies for acute myocardial infarction. N Engl J Med 1993;329(10):673-82.
- Jinatongthai P, Kongwatcharapong J, Foo CY, et al. Comparative efficacy and safety of reperfusion therapy with fibrinolytic agents in patients with ST-segment elevation myocardial infarction: a systematic review and network meta-analysis. Lancet 2017;390(10096):747-59 doi: 10.1016/s0140-6736(17)31441-1.
- Pinto DS, Frederick PD, Chakrabarti AK, et al. Benefit of transferring ST-segment-elevation myocardial infarction patients for percutaneous coronary intervention compared with administration of onsite fibrinolytic declines as delays increase. Circulation 2011;124(23):2512-21 doi: 10.1161/CIRCULATIONAHA.111.018549.
- Boersma E, Maas ACP, Deckers JW, et al. Early thrombolytic treatment in acute myocardial infarction: reappraisal of the golden hour. Lancet 1996;348(9030):771-75 doi: 10.1016/s0140-6736(96)02514-7.
- Armstrong PW, Gershlick AH, Goldstein P, et al. Fibrinolysis or primary PCI in ST-segment elevation myocardial infarction. N Engl J Med 2013;368(15):1379-87 doi: 10.1056/NEJMoa1301092.
- Gibson CM, Murphy SA, Kirtane AJ, et al. Association of duration of symptoms at presentation with angiographic and clinical outcomes after fibrinolytic therapy in patients with ST-segment elevation myocardial infarction. J Am Coll Cardiol 2004;44(5):980-7 doi: 10.1016/j.jacc.2004.05.059.
- Weaver WD, Cerqueira M, Hallstrom AP, et al. Prehospital-initiated vs hospital-initiated thrombolytic therapy: the myocardial infarciton triage and intervention trial. JAMA 1993;270:1211-16.
- Morrow DA, Antman EM, Sayah A, et al. Evaluation of the time saved byprehospital initiation of reteplase forST-elevation myocardial infarction. J Am Coll Cardiol 2002;40(1):71-77 doi: 10.1016/s0735-1097(02)01936-8.
- Welsh RC, Travers A, Senaratne M, et al. Feasibility and applicability of paramedic-based prehospital fibrinolysis in a large North American center. Am Heart J 2006;152(6):1007-14 doi: 10.1016/j.ahj.2006.06.022.
- Crowder JS, Hubble MW, Gandhi S, et al. Prehospital administration of tenecteplase for ST-segment elevation myocardial infarction in a rural EMS system. Prehosp Emerg Care 2011;15(4):499-505 doi: 10.3109/10903127.2011.598609.
- Larson DM, Duval S, Sharkey SW, et al. Safety and efficacy of a pharmaco-invasive reperfusion strategy in rural ST-elevation myocardial infarction patients with expected delays due to long-distance transfers. Eur Heart J 2012;33(10):1232-40 doi: 10.1093/eurheartj/ehr403.
- Gibler WB, Kereiakes DJ, Dean EN, et al. Prehospital diagnosis and treatment of acute myocardial infarction: a north-south perspective. Am Heart J 1991;121:1-11.
- Godfrey A, Borger J. EMS Prehospital Administration of Thrombolytics for STEMI: StatPearls [Internet], 2020.
- European Myocardial Infarction Project Group. Prehospital thrombolytic therapy in patients with suspected acute myocardial infarction. N Engl J Med 1993;329:383-9.
- Morrison LJ, Verbeek PR, McDonald AC, et al. Mortality and prehospital thrombolysis for acute myocardial infarction: a meta-analysis. JAMA 2000;283:2686-92.
- Bonnefoy E, Lapostolle F, Leizorovicz A, et al. Primary angioplasty versus prehospital fibrinolysis in acute myocardial infarction: a randomised study. Lancet 2002;360(9336):825-29 doi: 10.1016/s0140-6736(02)09963-4.
- Danchin N, Blanchard D, Steg PG, et al. Impact of prehospital thrombolysis for acute myocardial infarction on 1-year outcome: results from the French Nationwide USIC 2000 Registry. Circulation 2004;110(14):1909-15 doi: 10.1161/01.CIR.0000143144.82338.36.
- Bonnefoy E, Steg PG, Boutitie F, et al. Comparison of primary angioplasty and pre-hospital fibrinolysis in acute myocardial infarction (CAPTIM) trial: a 5-year follow-up. Eur Heart J 2009;30(13):1598-606 doi: 10.1093/eurheartj/ehp156.
- Westerhout CM, Bonnefoy E, Welsh RC, et al. The influence of time from symptom onset and reperfusion strategy on 1-year survival in ST-elevation myocardial infarction: a pooled analysis of an early fibrinolytic strategy versus primary percutaneous coronary intervention from CAPTIM and WEST. Am Heart J 2011;161(2):283-90 doi: 10.1016/j.ahj.2010.10.033.
- Roule V, Ardouin P, Blanchart K, et al. Prehospital fibrinolysis versus primary percutaneous coronary intervention in ST-elevation myocardial infarction: a systematic review and meta-analysis of randomized controlled trials. Critical Care 2016;20(1):359 doi: 10.1186/s13054-016-1530-z.
- ASSENT-4 PCI Investigators. Primary versus tenecteplase-facilitated percutaneous coronary intervention in patients with ST-segment elevation acute myocardial infarction (ASSENT-4 PCI): randomised trial. Lancet 2006;367(9510):569-78 doi: 10.1016/s0140-6736(06)68147-6.
- Pu J, Ding S, Ge H, et al. Efficacy and Safety of a Pharmaco-Invasive Strategy With Half-Dose Alteplase Versus Primary Angioplasty in ST-Segment-Elevation Myocardial Infarction: EARLY-MYO Trial (Early Routine Catheterization After Alteplase Fibrinolysis Versus Primary PCI in Acute ST-Segment-Elevation Myocardial Infarction). Circulation 2017;136(16):1462-73 doi: 10.1161/CIRCULATIONAHA.117.030582.
- Berwanger O, Lopes RD, Moia DDF, et al. Ticagrelor Versus Clopidogrel in Patients With STEMI Treated With Fibrinolysis: TREAT Trial. J Am Coll Cardiol 2019;73(22):2819-28 doi: 10.1016/j.jacc.2019.03.011.
- Sabatine MS, Cannon CP, Gibson CM, et al. Addition of clopidogrel to asprin and fibrinolytic therapy for myocardial infarction with ST-segment elevation. N Engl J Med 2005;352(12):1179-89.
- Ross AM, Molhoek P, LUndergan C. A randomized comparison of low-molecular-weight heparin enoxaparin and unfractionated heparin adjunctive to t-PA thrombolysis and aspirin (HART II). Circulation 2001;104:648-52.
- Baird SH, McBride SJ, Trouton TG, Wilson C. LMWH versus unfractionated heparin following thrombolysis in myocardial infarction. J Am Coll Cardiol 1998;31 (suppl A)(191A).
- Wallentin L, Dellborg DM, LIndahl B. The low-molecular-10 weight heparin dalteparin as adjuvant therapy in acute myocardial infarction: the ASSENT Plus study. Clin Cardiol 2001;24 (suppl 3):I12-14.
- ASSENT-3 Investigators. Efficacy and safety of tenecteplase in combination with enoxaparin, abciximab, or unfractionated heparin: the ASSENT-3 randomised trial in acute myocardial infarction. Lancet 2001;358(9282):605-13 doi: 10.1016/s0140-6736(01)05775-0.
- Antman EM, Morrow DA, McCabe CH, et al. Enoxaparin versus unfractionated heparin with fibrinolysis for ST-elevation myocardial infarction. N Engl J Med 2006;354:1477-88.
- Topol EJ, GUSTO V Investigators. Reperfusion therapy for acute myocardial infarction with fibrinolytic therapy or combination reduced fibrinolytic therapy and platelet glycoprotein IIb/IIIa inhibition: the GUSTO V randomised trial. Lancet 2001;357(9272):1905-14.
- Herrmann HC, Moliterno DJ, Ohman EM, Stebbins AL, Bode C, Betriu A. Facilitation of early percutaneous coronary intervention after reteplase with or without abciximab in acute myocardial infarction: results from the SPEED (GUSTO-4 Pilot) Trial. J Am Coll Cardiol 2000;36(5):1489-96.
- Antman EM, Gibson CM, De Lemos JA, Giugliano RP, McCabe CH, Coussement P. Combination reperfusion therapy with abciximab and reduced dose reteplase: results from TIMI 14. The Thrombolysis in Myocardial Infarction (TIMI) 14 Investigators. Eur Heart J 2000;21(23):1944-53.
- Brener SJ, Zeymer U, Adgey AAJ, Vrobel TR, Ellis SG. Eptifibatide and low-dose tissue plasminogen activator in acute myocardial infarction: the integrilin and low-dose thrombolysis in acute myocardial infarction (INTRO AMI) trial. J Am Coll Cardiol 2002;39(3):377-86.
- Gibson CM, Jennings LK, Murphy SA, Lorenz DP. Association between platelet receptor occupancy after eptifibatide (integrilin) therapy and patency, myocardial perfusion, and ST-segment resolution among patients with ST-segment-elevation myocardial infarction: an INTEGRITI (Integrilin and Tenecteplase in Acute Myocardial Infarction) substudy. Circulation 2004;110(6):679-84.
- Antman EM, Louwerenburg HW, Baars HF, Wesdorp JCL, Hamer B. Enoxaparin as adjunctive antithrombin therapy for ST-elevation myocardial infarction: results of the ENTIRE-Thrombolysis in Myocardial Infarction (TIMI) 23 Trial. Circulation 2002;105(14):1642-9
- Streptase [package insert]. Ottawa, Ontario: CSL Behring Canada, Inc.; 2007.
- GUSTO III Investigators. A comparison of reteplase with alteplase for acute myocardial infarction. N Engl J Med 1997;337:1118-23.
- Llevadot J, Giugliano RP, Antman EM. Bolus fibrinolytic therapy in acute myocardial infarction. JAMA 2001;286:442-49.
- Tillett WS, Garner RL. The fibrinolytic activity of hemolytic streptococci. J Exp Med 1933;58(4):485-502.
- GISSI Investigators. Effectiveness of intravenous thrombolytic treatment in acute myocardial infarction. Lancet 1986;1:397-402.
- ISIS-2 Collaborative Group. Randomised trial of intravenous streptokinase, oral aspirin, both, or neither among 17,187 cases of suspected acute myocardial infarction: ISIS-2. Lancet 1988;2:349-60.
- Smalling RW, Bode C, Kalbfleisch J. More rapid, complete, and stable coronary thrombolysis with bolus administration of reteplase (r-PA) compared with alteplase infusion in acute myocardial infarction. Circulation 1995;91:2725-32.
- Topol EJ, Ohman EM, Armstrong PW, Wilcox R, Skene AM, Aylward P. Survival outcomes 1 year after reperfusion therapy with either alteplase or reteplase for acute myocardial infarction: results from the global utilization of streptokinase and t-PA for occluded coronary arteries (GUSTO) III trial. Circulation 2000;102:1761-65.
- Bode C, Smalling RW, Berg G, et al. Randomized Comparison of Coronary Thrombolysis Achieved With Double-Bolus Reteplase (Recombinant Plasminogen Activator) and Front-Loaded, Accelerated Alteplase (Recombinant Tissue Plasminogen Activator) in Patients With Acute Myocardial Infarction. Circulation 1996;94(5):891-98.
- Lexicomp Online, Lexi-Drugs Online, Hudson, Ohio: UpToDate, Inc.; 2021; May 7, 2021.









