Originally published at CoreEM.net, dedicated to bringing Emergency Providers all things core content Emergency Medicine available to anyone, anywhere, anytime. Reposted with permission.
Follow Dr. Swaminathan, Dr. Jacob Avila, and CORE EM on twitter at @EMSwami and @Core_EM
Written by Rana Biary, MD and Edited by Anand Swaminathan, MD
Definition: A hemoglobinopathy characterized by an abnormal elevation of methemoglobin (MetHb) – hemoglobin in which iron (ferrous Fe2+) has been oxidized(ferric Fe3+). An abnormal MetHb level is any level > 1%.
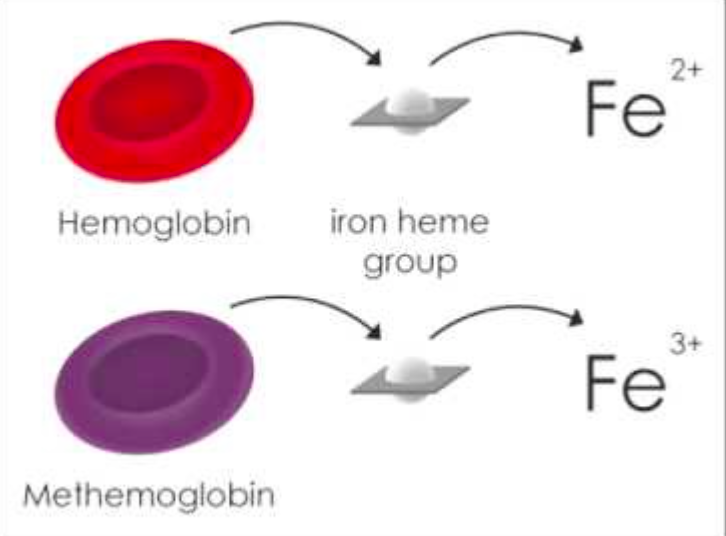
Mechanism of Action
- Pathophysiology
- Oxidized iron sites on MetHb unable to bind oxygen
- Remaining binding sites with increased affinity for binding oxygen
- Causes a leftward shift in the oxyhemoglobin dissociation curve
- Results in decreased tissue oxygen delivery
- Normal situation
- Red cells constantly exposed to oxidant stress
- NADH MetHb reductase keeps oxidative stress in check by reducing MetHb to Fe2+ state
- Methemoglobinemia occurs when either
- There is an deficiency of the reducing enzyme (NADH MetHb reductase)
- There is increased oxidative stress that cannot be handled by the body
- Presence of MetHb renders pulse-oximetry readings inaccurate
Common Causative Agents
- Benzocaine
- Dapsone
- Nitroglycerin
- Nitrofurantoin
- Nitroprusside
- Phenazopyridine
- Sodium Nitrite
- Amyl nitrite
- Contaminated well water
- Isobutyl Nitrite (“poppers”)
Signs + Symptoms
- Low O2 saturation that does not respond to supplemental O2
- Key diagnostic feature (sat < 85% w/o response to 100% FiO2)
- Wavelength averaging by the pulse oximeter causes a falsely low O2 reading
- Since there is no true decrease in O2 saturation, there will be no response to 100% FiO2
- Severity of symptoms correlates closely to MetHb level and severity of impaired O2 delivery
- Symptoms will be worse for any MetHb level in patients with baseline impairment of O2 delivery (i.e. CHF, pneumonia, COPD, anemia)

- MetHb: < 15%
- May be asymptomatic
- Low pulse oximeter reading
- MetHb: 15-20%
- Cyanosis (peripheral and central)
- Fatigue
- Chocolate brown colored blood
- MetHb: 20-50%
- Dyspnea
- Headache
- Exercise intolerance
- Dizziness
- Syncope
- Weakness
- MetHb: 50-70%
- Tachypnea
- Metabolic acidosis
- Dysrhythmias
- Seizures
- CNS depression
- Coma
- MetHb > 70%
- Severe hypoxemia
- Death

- Source identification, removal (if possible) and decontamination
- Basic Supportive Care
- Provide 100% FiO2 – lack of response should raise suspicion of methemoglobinemia
- Due to unreliability of pulse oximetry, O2 saturation should not be sole indication for advanced airway management
- Diagnostic Testing
- Blood gas
- Venous blood gas (VBG) adequate
- Arterial blood gas (AG) if obtained, will reveal a normal PaO2
- Co-oximeter panel for MetHb level
- Can use a venous or arterial sample
- Half-life 1-3 hours
- Blood gas
- Obtain toxicology consultation (800-222-1222 in US)
- Methylene Blue
- Mechanism of action
- Converted to cofactor for NADPH MetHb reductase
- Helps increase reduction of MetHb
- Which patients should get treatment?
- MetHb < 25% with symptoms
- Abnormal vital signs
- Metabolic acidosis
- End organ dysfunction (i.e. AMS, seizures)
- MetHb > 25% regardless of symptoms
- MetHb < 25% with symptoms
- Dosing
- 1-2 mg/kg IV
- Medication can cause local painful reaction
- Minimize with slower infusion (over 5 minutes)
- Flush line after infusion completed
- Clinical improvement should occur rapidly
- Warning: Will cause transient decrease in puse-ox level due to color of medication
- Mechanism of action
Take Home Points
- Methemoglobinemia can result from exposure to a number of different medications. The most common are dapsone and topical anesthetic agents (i.e. benzocaine)
- Consider the diagnosis in any patient with cyanosis and hypoxia that doesn’t respond to oxygen administration
- Administer methylene blue to any patient with abnormal vital signs, metabolic acidosis, end organ dysfunction or, a serum level > 25%
Read More
Core EM: Episode 97.0 – Methemoglobinemia
Price DP. Chapter 127. Methemoglobin Inducers. In: Nelson LS, Lewin NA, Howland M, Hoffman RS, Goldfrank LR, Flomenbaum NE. eds. Goldfrank’s Toxicologic Emergencies, 9e New York, NY: McGraw-Hill; 2011.. Link





