Author: Dhara P. Amin (EM Resident Physician, Keck School of Medicine/Department of Emergency Medicine, LAC+USC Medical Center) // Editors: Alex Koyfman, MD (@EMHighAK) and Manpreet Singh, MD (@MPrizzleER)
Case #1:
An 8 week-old male infant brought in by parents for decreased PO intake and increased fussiness x 2 days. He was born at term after an uncomplicated pregnancy, was exclusively breastfed and developing appropriately. Vitals were stable and patient was afebrile. On exam infant had a strong cry but noted to not hold head up well when picked up and eye movements were delayed. Reflexes were intact. He would not feed with breast or formula in the ED with multiple attempts noted to have a weak suck response. Workup was initially targeted to sepsis and dehydration based on the concerning findings. Urinalysis, chest x-ray, and spinal fluid were negative for infectious etiology. IV antibiotics and IV fluids were started and admission to PICU.
Upon consultation with PICU attending and his exam there was immediate concern for infantile botulism. Mother was unemployed and father worked as a construction worker. BIG-IV was ordered and administered within 7 hours of suspicion for infection. Patient within 10 hours of PICU admission was noted to have poor respiratory effort and was intubated for ventilator support. Remained in ICU for 6 days and was extubated on day 4.
Case #2:
A 2-month-old female presented with a 5-day history of lethargy, poor feeding, constipation, and rhinorrhea. Her older siblings had concurrent upper respiratory tract infections. She was born at term, following an uncomplicated pregnancy. She was previously well. She is formula fed.
On examination, she appeared lethargic, had a weak cry and was noted to have droopy eyelids. There were no other significant clinical findings. She was started on intravenous antibiotics for suspected sepsis following a full septic work-up. Due to poor respiratory effort patient was intubated and transferred to a tertiary care hospital with a high concern for infantile botulism. Upon arrival to pediatric intensive care unit patient was continued on IV antibiotics and BIG-IV was given 5 hours after arrival. Patient went on to stay in PICU for 5 days then was extubated and began to have good oral intake. Transferred to ward bed for 3 days and went on to be discharged with full recovery on day 9 of hospitalization.
Most common admitting diagnosis: Bronchiolitis with dehydration and sepsis
Infantile Botulism (Clostridium botulinum)
- Most common form of botulism in the United States (the other forms are wound and foodborne) and most cases are in California.
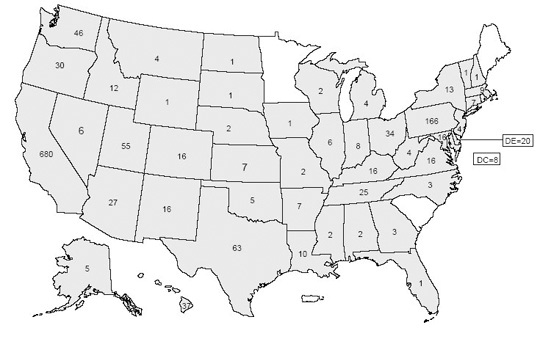
- Centers for Disease Control and Prevention: Annual incidence (2012) of 122 cases in the US, with a mean age of 19 weeks.
| Infant (122 cases) | |
| Median age | 19 weeks (range: 1–53 weeks) |
| Death | 0 confirmed |
| Gender | 73 (60%) male, 49 (40%) female |
| Toxin type | 51 (42%) type A 66 (54%) type B 1 (<1%) type Ba 1 (<1%) type Bf 3 (2%) type F |
| Outbreaks | None |
Centers for Disease Control and Prevention (CDC). Botulism Annual Summary, 2012. Atlanta, Georgia: US Department of Health and Human Services, CDC, 2014.
- Worldwide incidence is rare, 90% of world’s cases in US!
- Acquired by ingesting the spores, which are found in soil or honey products
- Gram positive spore-forming anaerobic organism capable of forming different neurotoxins
- Attacks presynaptic cholinergic receptors leading to lack of acetylcholine available for muscle excitation
Clinical Presentation:
- Constipation!!!
- Poor feeding
- Weak Cry
- Poor muscle tone (hypotonic, hyporeflexic, floppy)
- Lethargy
- Respiratory difficulties
- Seizures
Differential Diagnosis:
- Sepsis
- Meningoencephalitis
- Metabolic (Hyponatremia, Reye’s Syndrome, Hypothyroid)
- Toxins and Poisonings (Heavy metals, alcohols, organophosphates, anticholinergic, narcotics)
- Neuromuscular (Poliomyelitis, Guillain-Barre Syndrome, Congenital myasthenia gravis, muscular dystrophy, tick paralysis)
Diagnosis:
High index of clinical suspicion and stool sample detection of botulinum toxin and electromyogram studies (takes days). Given the delay in completing this analysis, and the characteristic clinical findings, some authors suggest that for treatment purposes, the clinical diagnosis should be considered the gold standard, with laboratory findings being confirmatory.
Treatment:
- Supportive (ICU admission)
- BabyBIG® (BIG-IV)
BACKGROUND: October 2003 the U.S. Food and Drug Administration licensed to the California Department of Public Health its public service orphan drug for the treatment of infant botulism, Human Botulism Immune Globulin, under the proprietary name BabyBIG(R).
Dose: 1mL/kg (50mg/kg), given as a single intravenous infusion
Cost: $45,300 per vial
Prognosis: Excellent! A case-fatality rate of less than 2 percent.
In 2006, Arnon et al[2] reported two large multi-center studies on the efficacy and safety of BIG-IV in a California-based randomized control trial (RCT) and an open-label study that was America wide. In the RCT, BIG-IV was given to infants with suspected botulism within the first 3 days of their hospital admission (59 of the 65 patients who received BIG-IV had confirmed infant botulism). BIG-IV significantly reduced the average length of hospitalization by 3.1 weeks, the length of admission to ICU by 3.2 weeks, the duration of mechanical ventilation by 2.6 weeks, and duration of feeding by a tube or through intravenous means by 6.4 weeks. This corresponded to a gross saving of $US88 600 per patient.
- Consultation or BIG-IV can be obtained from the California Department of Health Services by IMMEDIATELY calling the 24-hour number at 510-231-7600. Also contact department of health to arrange for testing. Additional information about infant botulism is available at: http://www.infantbotulism.org/
- Because CDC, the Alaska Division of Public Health, and the California Department of Public Health (CDPH), are the only sources of botulism antitoxin administered in the United States, nearly all recognized cases of botulism are reported.
Pearls:
- Infant botulism is a rare disease that often presents non-specifically
- Making the diagnosis requires a high index of suspicion and specific confirmatory tests should be arranged
- BIG-IV provides a safe, efficacious and likely cost-effective treatment of infant botulism. However, its use is time sensitive, with its greatest effect occurring before the confirmatory tests may be available.
Questions from “Of war and sausages: A case-directed review of infant botulism”
- Clinical signs consistent with Botulism include all the following except:
a. Hypotonia
b. Hyperreflexia
c. Opthalmoplegia
d. Mydriasis
e. Hypertension
- Botulinum toxin exerts its main disease producing effect via:
a. Blocking noradrenaline release at the neuromuscular junction
b. Blocking acetylcholine binding to receptors at the neuromuscular junction
c. Causing anterior horn nerve cell damage in the spinal cord
d. Blocking acetylcholine release at the neuromuscular junction
e. Blocking noradrenaline release at the neuromuscular junction.
- All of the following tests are important for confirming the diagnosis of botulism in a child except:
a. Stool sample for botulinum toxin identification
b. Electromyogram
c. Mouse bioassay with toxin neutralization
d. Stool sample for culture of Clostridium botulinum.
e. Magnetic resonance imaging of the brain and spinal cord
References:
- Centers for Disease Control and Prevention. (2012). National Botulism Surveillance Overview. Retrieved fromhttp://www.cdc.gov/ncezid/dfwed/PDFs/bot-overview_508c.pdf
- Arnon SS, Schechter R, Maslanka SE, Jewell NP, Hatheway CL. Human botulism immune globulin for the treatment of infant botulism. Engl. J. Med. 2006; 354: 462–471.
- Schmidt RD, Schmidt TW. Infant botulism: a case series and review of the literature. J Emerg Med 1992;10:716.
- Brown N. Desai S. Infantile Botulism: A Case Report and Review. Research Article. J Emerg Med December 2013;45;842-845.
- Cox N, Hinkle. Infant R. Infant botulism. Am Fam Physician 2002;65;1388–1392.
- BarnesM, BrittonP, Singh-Grewal D. Of war and sausages: A case-directed review of infant botulism. Journal of Pediatrics and Child Health. 2013;49, E232–E234.
Answers: B/D/E





