Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX)// Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 3-year-old male presents with his mom with chief complaint of recurrent bouts of abdominal pain and vomiting (non-bloody and non-bilious). Mom states a “bug” has been going around his daycare, but what concerns her the most is that her son will intermittently cry and refuse to eat, followed by normal activity. Mom denies fevers, but his appetite has been decreased. He was born at term and has no pertinent medical history. Vaccines are up to date.
Triage vital signs (VS): BP 93/55, HR 117, T 98.9 rectal, RR 28, SpO2 99% RA.
Physical exam reveals a patient who appears stated age, nontoxic, and playful. Your physical exam, including abdomen and GU, is normal. The mom rushes out several minutes later and notifies you that her son is crying and holding his abdomen.
What’s the diagnosis, and what’s your next step in your evaluation and treatment?
Answer: Intussusception
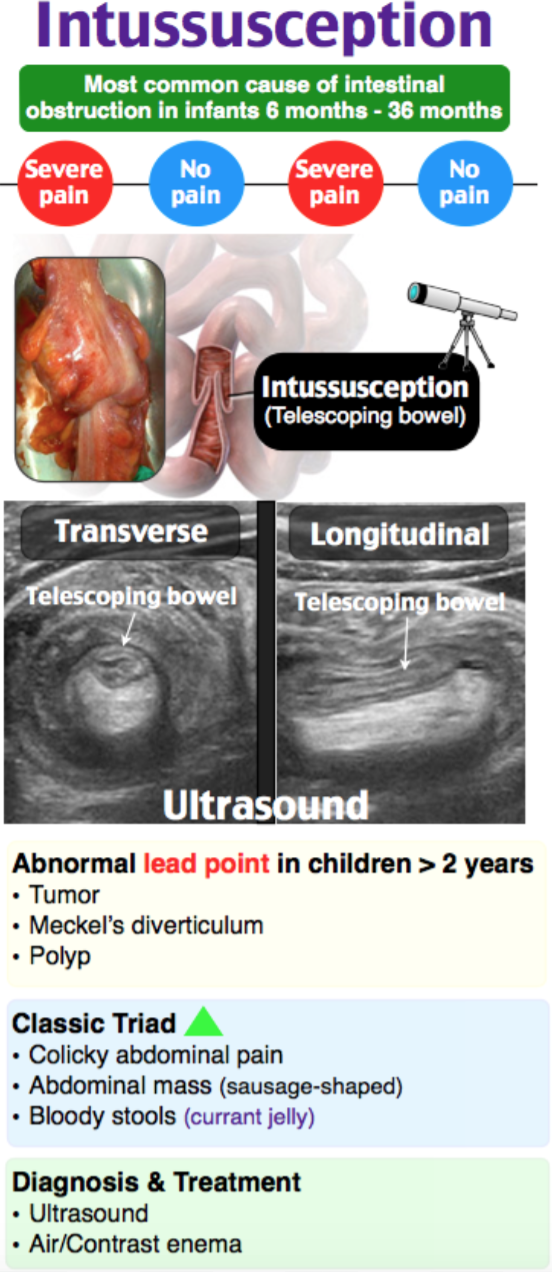
- Background: Defined by telescoping of one part of the intestine into another.
- Most common cause of bowel obstruction in patients ages 6 months to 6 years, but intussusception is most common in those ages 6-36 months.
- If the mesentery is involved, bowel ischemia can occur.
- Pediatric Patients:
-
- There is usually no pathological cause, known as a “lead point”. For patients over 6 years, lead points such as cyst, polyp, tumor, HSP, or Meckel diverticulum are more common.
- The intussusception is most commonly located at the ileocecal junction.
- Males are affected more commonly than females.
- Adults:
- The disease is rare in adults.
- Over 80% involve small bowel, but if this occurs, it is strongly associated with malignancy as a pathological lead point (70%).
- Features:
- In pediatric patients, the classic triad includes sudden colicky pain, a sausage shaped abdominal mass on the right that is palpable, and currant jelly stool. This triad is present in 21% of patients, with currant jelly stool present in 50% of patients.
- Patients commonly present with intermittent episodes of pain and vomiting. They may present in the knee to chest position during episodes of pain.
- There may be asymptomatic periods with no pain. Patients may be playful and appear well. However, recurrent, brief episodes of pain are concerning for the condition.
- Late stages may present with lethargy. Lethargy and decreased activity may be the only signs of the disease.
- Adults more commonly present with signs and symptoms of small bowel obstruction: vomiting, abdominal distension, constipation. Late stages present with severe sepsis.
- Differential: Dependent on age, but consider necrotizing enterocolitis, volvulus, torsion, trauma, pyloric stenosis, Hirschsprung’s Disease, appendicitis, megacolon, vaso-occlusive crisis, UTI, HSP, DKA, toxic ingestion, cyst, pancreatitis, cholecystitis, pneumonia, IBD, pharyngitis, meningitis/encephalitis.
- ED Evaluation:
- The classic triad cannot be relied upon for diagnosis. Consider the disease in patients with vomiting but no diarrhea, intermittent episodes of abdominal pain, or lethargy/altered mental status.
- Remember “TIPS AEIOU” for altered mental status? Keep in mind one of the “I’s” stands for intussusception.
- Lab findings are nonspecific and typically not helpful. Stool may be guaiac positive in up to 75% of patients who do not have visible blood in stools.
- Imaging: Key testing!
- Ultrasound is operator dependent, but sensitivity and specificity approach 100%. For most younger patients, a linear probe applied in graded compression over all quadrants of the abdomen may reveal a bullseye (short axis) or pseudokidney (longitudinal view). Ultrasound will diagnosis ileo-ileal intussusception. However, if US is negative, intermittent intussusception may be present.
- For more US goodness, see https://vimeo.com/37877537and https://www.youtube.com/watch?v=sHVA55BF2qw.
- Abdominal X-ray may demonstrate a mass in the right upper quadrant, but if used alone, they are limited. They can be falsely negative in up to 20% of patients.
- Air contrast enema can diagnose and treat the condition. IV hydration, NG tube, and surgery consult is recommended before enema is completed. A saline or water-soluble enema may also be useful.
- CT abdomen is needed for adult patients due to the common presence of a pathological lead point. Air contrast or barium enemas are not reliable in adults.
- ED Management:
- Stable pediatric patients with high suspicion of or diagnosis of intussusception without perforation can be treated with: air contrast or saline/water-soluble contrast enema. Patients should be NPO.
- Surgery should be consulted if nonoperative therapies do not work, if the patient has evidence of perforation, or if toxic-appearing. If ileo-ileal intussusception is present and the patient is stable without symptoms, expectant management is reasonable, but surgery should be consulted.
- Surgery is recommended for all adults with intussusception.
- Disposition:
- Patients may be discharged after reduction if the patient is pain free, afebrile, stable, PO tolerant, has follow-up, and is able to return quickly to the hospital. However, patients may experience recurrence in 5-15% of cases, though this typically does not occur within the first several days.
- Admission is warranted for all other patients.

An 18-month-old boy presents to the emergency department with his mother for two days of intermittent episodes of inconsolable crying. During these episodes, the child is noted to stop playing, lie down, and draw his legs up to his chest. His mother also notes two grossly bloody bowel movements over the last day. Which of the following is a risk factor for this patient’s condition?
A) Henoch-Schonlein purpura
B) Intestinal malrotation
C) Prematurity
D) Vaccination against
Answer: A
Intussusception is the invagination of a bowel segment into a distal segment of bowel. It is the most common abdominal emergency and cause of intestinal obstruction in early childhood. Intussusception is most common in males and in children six to 36 months of age. The majority of cases of pediatric intussusception are idiopathic, but risk factors include conditions that cause a lead point for intestinal telescoping, including Meckel’s diverticulum, Henoch-Schonlein purpura, intestinal tumors, rotavirus vaccine, and recent viral infection. The classic presentation of intussusception is intermittent abdominal pain, drawing up of the legs towards the abdomen, vomiting, bloody “currant-jelly” stools mixed with mucus, and a right-sided sausage-shaped abdominal mass. In reality, however, the triad of intussusception—pain, bloody stools and abdominal mass—is rarely present. Children may present only with progressive lethargy and altered consciousness, a presentation which is often mistaken for sepsis. In children with uncertain presentations, the diagnosis of intussusception should be confirmed with ultrasonography, which has nearly 100% sensitivity in intussusception and classically shows a “target sign.”
Prematurity (C) and intestinal malrotation (B) are not associated with an increased risk of intussusception. Rotavirus vaccination, rather than H. influenzae vaccination (D), is associated with an increased risk of intussusception.
References:
- Bruce J, Huh YS, Cooney DR, et al. Intussusception: evolution of current management. J Pediatr Gastroenterol Nutr 1987;6:663-674.
- Marinis A et al. Intussusception of the bowel in adults: A review. World J Gastroenterol. 2009 Jan 28; 15(4): 407–411.
- Gray MP, Li SH, Hoffmann RG, Gorelick MH. Recurrence rates after intussusception enema reduction: a meta-analysis. Pediatrics. 2014 Jul;134(1):110-9.
- Mandeville K1, Chien M, Willyerd FA, et al. Intussusception: clinical presentations and imaging characteristics.Pediatr Emerg Care. 2012 Sep;28(9):842-4
- Whitehouse JS, Gourlay DM, Winthrop AL, et al. Is it safe to discharge intussusception patients after successful hydrostatic reduction?J Pediatr Surg. 2010 Jun;45(6):1182-6.
- Beres AL, Baird R, Fung E, Hsieh H, Abou-Khalil M, Ted Gerstle J. Comparative outcome analysis of the management of pediatric intussusception with or without surgical admission. J Pediatr Surg. 2014 May;49(5):750-2.
- Mendez D, Caviness AC, Ma L, Macias CC. The diagnostic accuracy of an abdominal radiograph with signs and symptoms of intussusception. Am J Emerg Med. 2011 Mar 28.
- Little KJ, Danzl DF. Intussusception associated with Henoch-Schonlein Purpura. The Journal of Emergency Medicine: 1991;9(1):29






