Author: Shelly D. Saha, MD (EM Resident, UTSW / Parkland Memorial Hospital, Dallas, TX) // Reviewed by: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) and Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 28-year-old male presents to the ED with right shoulder pain after falling on an outstretched arm two hours earlier. He denies history of prior shoulder injuries. On exam, he is holding his right upper extremity in adduction and internal rotation at the shoulder. He is unable to externally rotate his shoulder due to pain, and you note prominence to the posterior shoulder on exam.
What is the patient’s diagnosis? What’s the next step in your evaluation and treatment?
Answer: Posterior shoulder dislocation
Background:
- Glenohumeral joint is most frequently dislocated joint.
- Inherently unstable, only 30% of humeral head articulates with glenoid fossa.
- Relies on soft tissues for additional stability.
- Highest incidence in young males, due to trauma.
- Up to 50% of posterior dislocations are misdiagnosed on initial presentation. 1
- Missed due to low clinical suspicion, insufficient imaging, or subtle findings on x-rays.
- Mechanism affects type of dislocation. 2
- Anterior (95-97%):
- Fall onto outstretched hand
- Blow to abducted and externally rotated arm
- Posterior (2-4%):
- Awkward fall with internal rotation
- Direct blow to anterior shoulder
- Less common but exam favorite: 3Es (epilepsy, ethanol, electricity) due to forceful internal rotation and adduction
- Inferior (0.5%):
- Hyperabduction
- High energy axial force from above
- Anterior (95-97%):

Clinical Presentation of Posterior Shoulder Dislocation:
- Arm is internally rotated and adducted with resistance to external rotation.
- May also find flattened anterior shoulder, prominent acromion and coracoid, or palpable posterior humeral head.
- Axillary nerve is most commonly injured in all types of should dislocations as it wraps around surgical neck of humerus.
- Subacromial position is most common; subglenoid and subspinous positions are rare. 3
- X-ray findings:
- Anterior-posterior:
- ‘Light bulb sign’: internally rotated humeral head appears symmetric due to rotation of greater tuberosity
- ‘Empty glenoid sign’: distance between anterior glenoid rim and articular surface of humeral head widened
- ‘Trough line sign’: dense vertical lines indicating impaction fracture of humeral head (reverse Hill-Sachs lesion)
- Anterior-posterior:
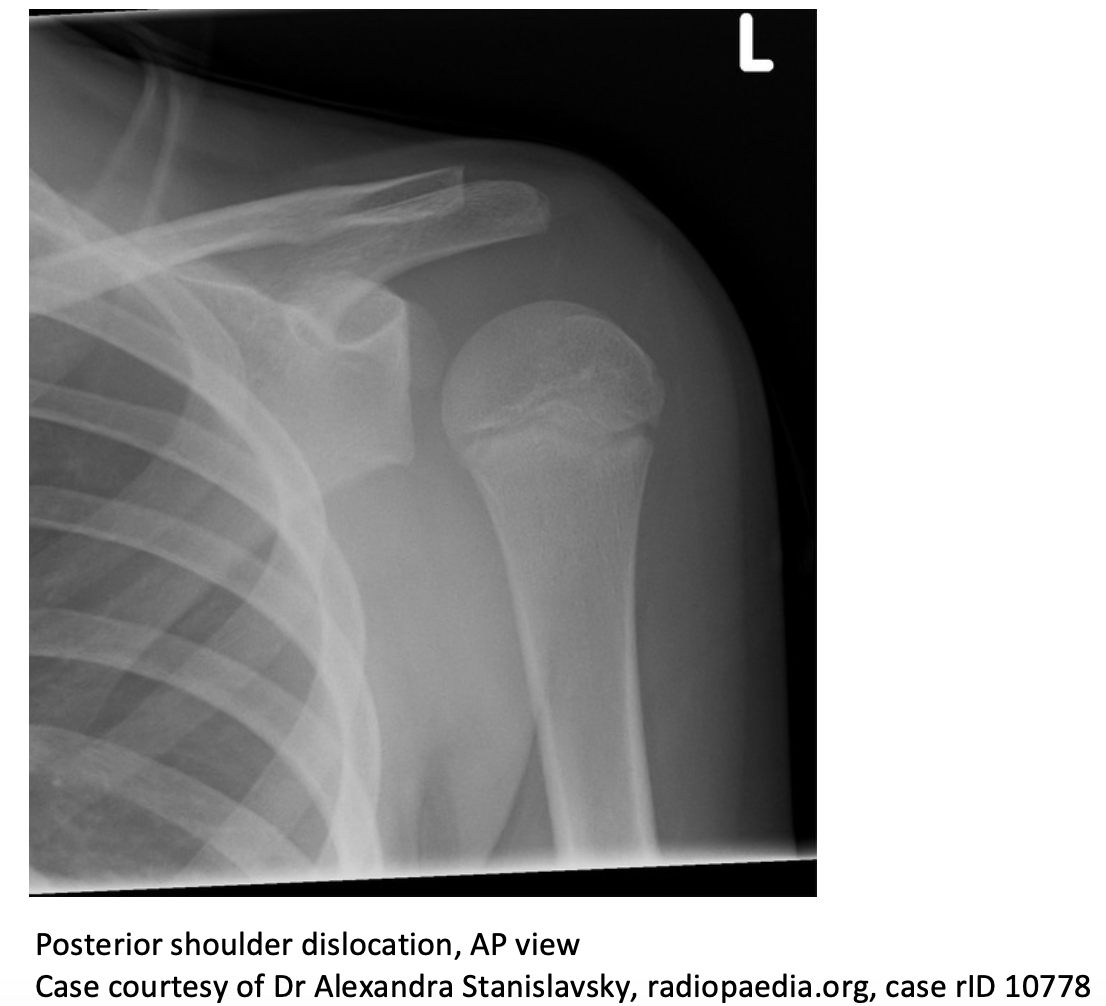
-
- Scapula Y: Humeral head displaced posterior to glenoid fossa and lateral to scapula
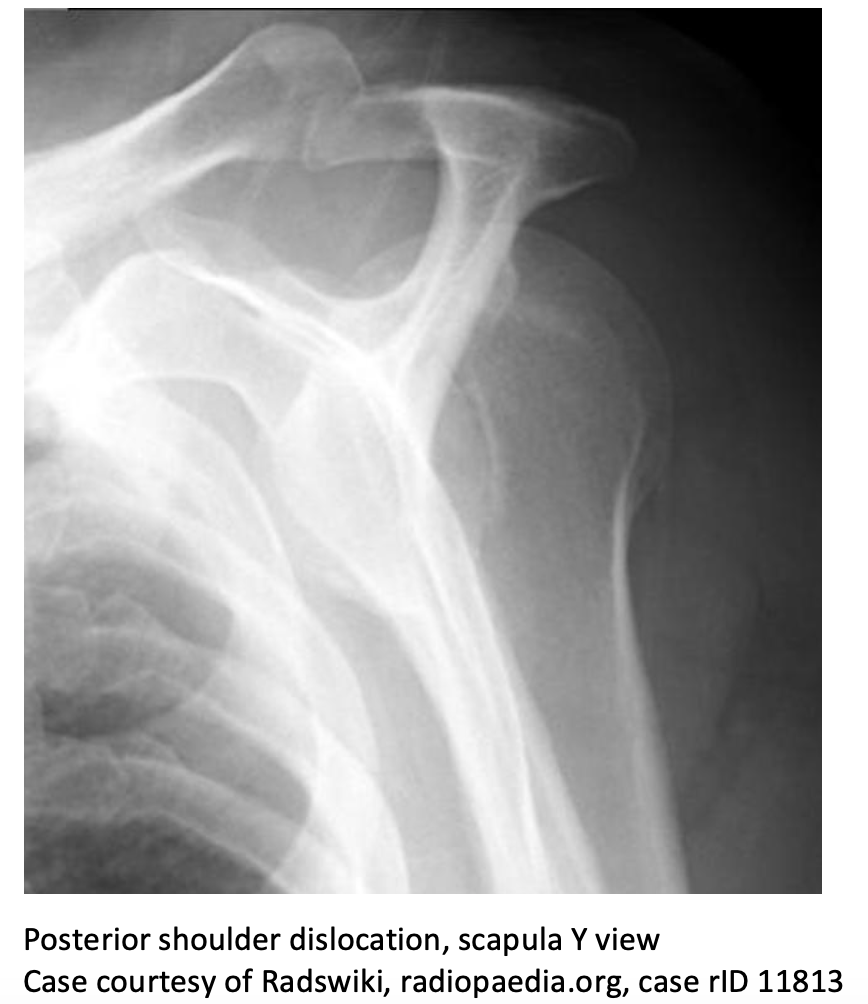
-
- Axillary: Humeral head displaced posterior to coracoid process

- Consider CT if high suspicion for posterior dislocation with equivocal x-rays or to characterize size of reverse Hill-Sachs lesion.
Complications:3, 4
- Reverse Bankart lesion – tear of posterolateral labrum
- Reverse Hill-Sachs deformity – impaction fracture of anteromedial aspect of humeral head
- Fracture of humeral shaft
- Fracture of lesser tuberosity
- Neurovascular injury and rotator cuff tears are less common than in anterior dislocation
- Adequate anesthesia is vital.
- Muscle tension from pain will make reduction more difficult.
- Consider intraarticular anesthetic, systemic analgesia, or both
- Can also use procedural sedation
- Consider an ortho consult for operative management if: 5
- Reverse Hill Sachs deformity > 25% of humeral head, may need open reduction internal fixation
- Bankart fracture causing glenohumeral instability
- Chronic dislocation, >3 weeks
- Irreducible dislocation
- Reduction (helpful to have 1-2 assistants)
- Mechanics are similar to traction-countertraction technique used in anterior dislocation
- With patient supine, apply inferior and posterior traction to long axis of humerus. Have an assistant applying direct pressure to posterior humeral head and another providing countertraction.
- Obtain post-reduction x-rays.
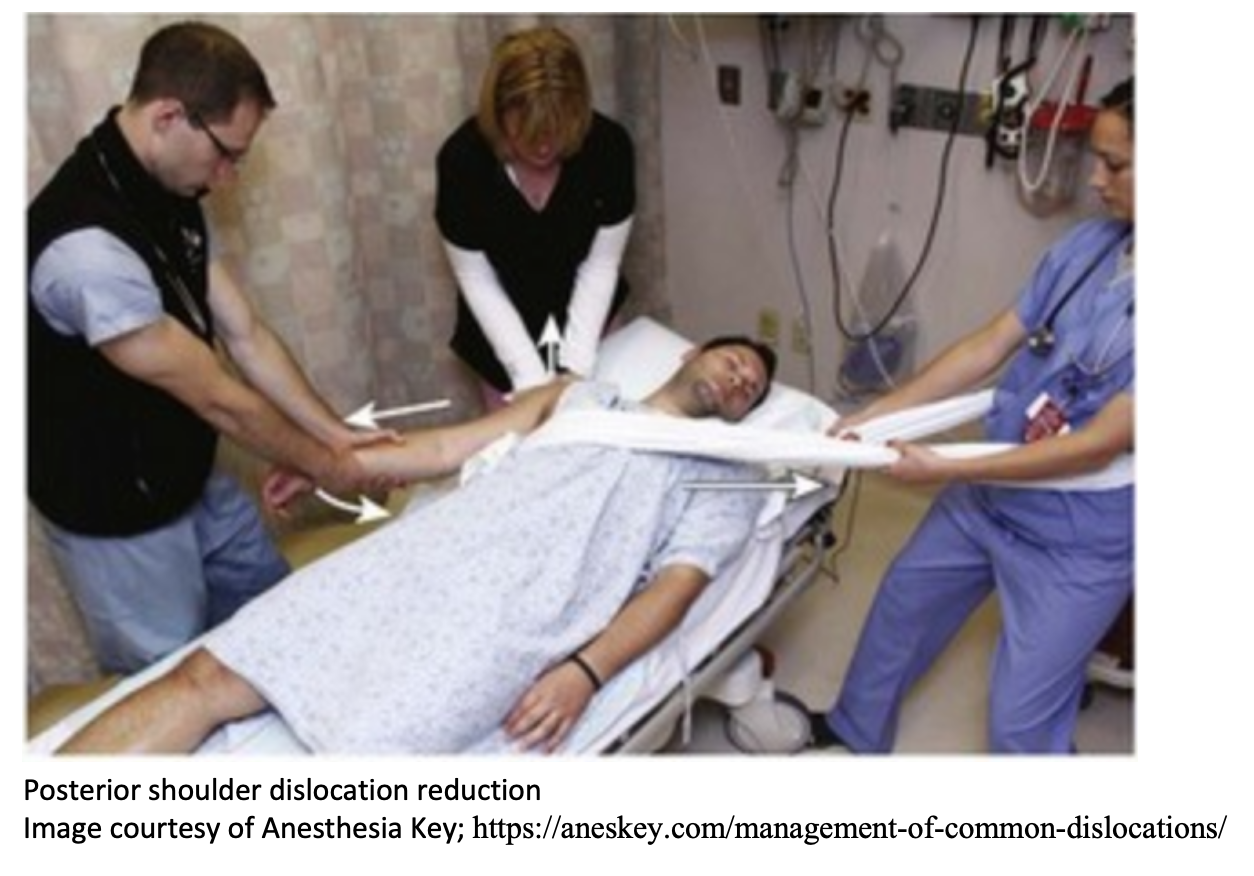
Disposition:
- Discharge if reduced successfully and pain controlled.
- Place in shoulder immobilizer at 10-20 degrees of external rotation for 4-6 weeks.
- Referral to orthopedics and physical therapy for follow-up.

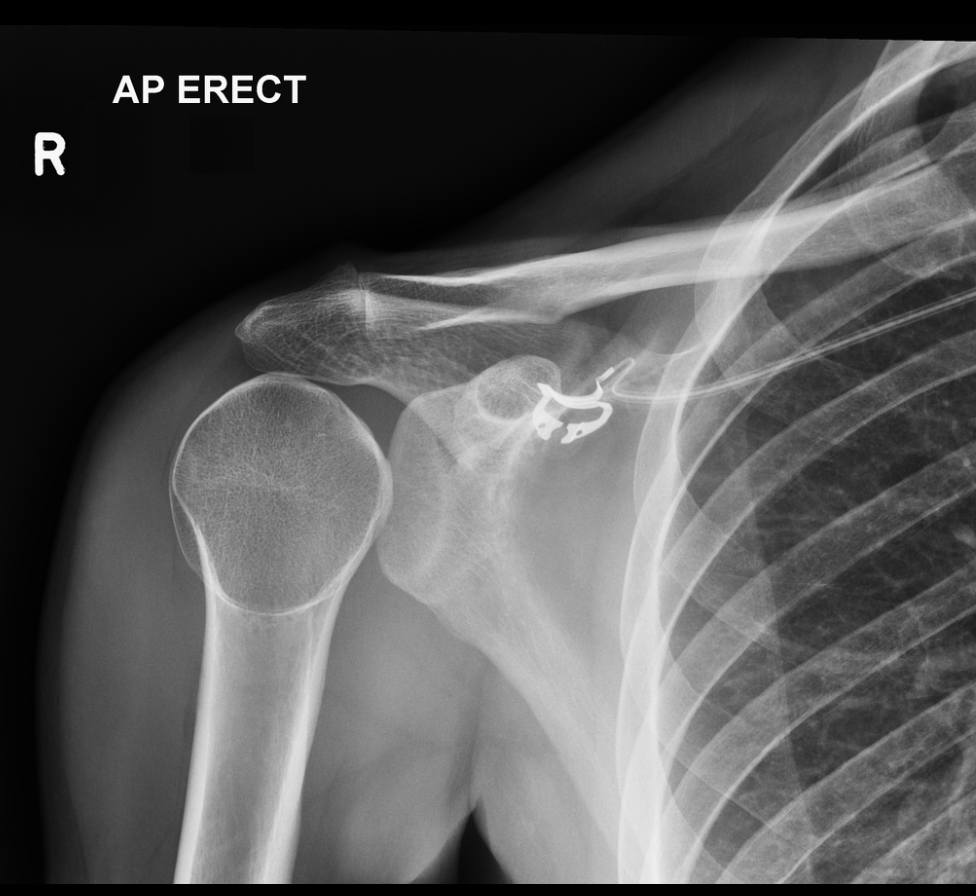
A 28-year-old man presents to the emergency department after a fall while riding his mountain bike. The patient states he went off a six-foot ramp and landed on his right shoulder. On physical exam, he is unable to move his right shoulder, and he holds the right upper extremity in internal rotation. An X-ray of the right shoulder is obtained, as seen above. Which of the following is the most likely diagnosis?
A) Acromioclavicular separation
B) Anterior shoulder dislocation
C) Clavicle fracture
D) Posterior shoulder dislocation
Answer: D
A posterior shoulder dislocation is caused by an axial force applied while the shoulder is internally rotated and abducted or by a direct blow to the anterior shoulder. With this injury, the arm will be held in adduction and internal rotation, and there is mechanical obstruction with active external rotation of the extremity. This injury is frequently missed because it is difficult to identify on radiographs. The subtle “light bulb” sign may be appreciated on the anteroposterior view of the radiograph. The axillary view is most helpful for diagnosis and will show the humeral head posterior to the glenoid fossa. Posterior shoulder dislocations are commonly associated with fractures of the surgical neck of the humerus, reverse Hill–Sachs deformities, and rotator cuff injuries. Procedural sedation should be given for reduction. The technique for reduction includes internal rotation and lateral traction to disimpact the humeral head from the glenoid rim, followed by external rotation. Reduction can be difficult, and orthopedic consultation for operative management may be required. The shoulder should be immobilized in external rotation with slight abduction.

Acromioclavicular separation (A) occurs most commonly from falling directly on the “point” of the shoulder, which causes the clavicle to separate from the scapula. Anterior shoulder dislocation (B) occurs with force on the extremity while in abduction, external rotation, and extension. This is the most common type of shoulder dislocation. The radiograph will show the humeral head anterior, medial, and inferior to the normal location. A clavicle fracture (C)usually occurs from falling onto the lateral shoulder, onto an outstretched arm, or from a direct blow. The majority of fractures occur in the middle third of the clavicle.
Further Reading:
Further FOAMed:
- EM@3AM – Anterior Shoulder Dislocation: http://www.emdocs.net/em3am-anterior-shoulder-dislocation/
- CORE EM – Shoulder Dislocation: https://coreem.net/core/shoulder-dislocation/
- EMRAP – Reduction of Posterior Shoulder Dislocation: https://www.emrap.org/episode/reductionof1/reductionof
References:
- Schwartz, D. T. (2008). Emergency radiology: case studies. New York: McGraw-Hill Medical.
- Grate, I. (2000). Luxatio erecta: A rarely seen, but often missed shoulder dislocation. The American Journal of Emergency Medicine, 18(3), 317–321. doi: 10.1016/s0735-6757(00)90127-x
- Bjoernsen, L., Ebinger, A. (2020). Shoulder and Humerus Injuries. In Tintinalli’s Emergency Medicine: A Comprehensive Study Guide (9th ed.). McGraw-Hill Education.
- McCasey, S. (2019). Rehabilitation of Musculoskeletal Conditions of the Upper Extremity. In Principles of Rehabilitation Medicine. McGraw-Hill Education.
- Perron AD, Jones RL. Posterior shoulder dislocation: avoiding a missed diagnosis. Am J Emerg Med 2000; 18:189.






1 thought on “EM@3AM: Posterior Shoulder Dislocation”
Pingback: Posterior Shoulder Dislocation – EMbeds.co.uk