Author: D. Heath Garner, MD (EM Resident Physician, UT Southwestern, Dallas, TX) // Reviewed by: Brit Long, MD (@long_brit) and Cynthia Santos, MD
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 22-year-old female presents to the ED after taking an entire bottle of unknown medication approximately an hour and a half ago. She states her boyfriend broke up with her, and she wanted to end her life. She describes a ringing sensation in her ears and mild nausea with no vomiting. She endorses taking a bottle of pills but refuses to say of what. She denies co-ingesting any other medication, drug, or alcohol.
Triage vital signs (VS): BP 122/75, HR 115, T 99.8 Oral, RR 32, SpO2 99% on RA.
The patient appears well and non-toxic. She is tachypneic with no increased work of breathing. She is tearful when being questioned but does not have any further complaints at this time.
What is the most likely medication overdose? What’s the next step in your evaluation and treatment? What lab tests would you like to order?
Answer: Aspirin (Acetylsalicylic Acid )
Background
- Aspirin is widely available over the counter and found in many medications and formulations
- Examples: Oil of Wintergreen, Bismuth Subsalicylate, BC Powder, Goody’s
- Easy overdose potential due to its availability
Mechanism of Action
- Analgesic, antipyretic, anti-inflammatory properties due to inhibition of cyclooxygenase enzyme (COX)
- Salicylates cause inhibition of oxidative phosphorylation, increased renal bicarbonate excretion, lipolysis, leading to metabolic acidosis
- Activation of the medulla within the brainstem results in hyperventilation (tachypnea) resulting in respiratory alkalosis
- It is these two mechanisms that lead to the mixed respiratory alkalosis/metabolic acidosis
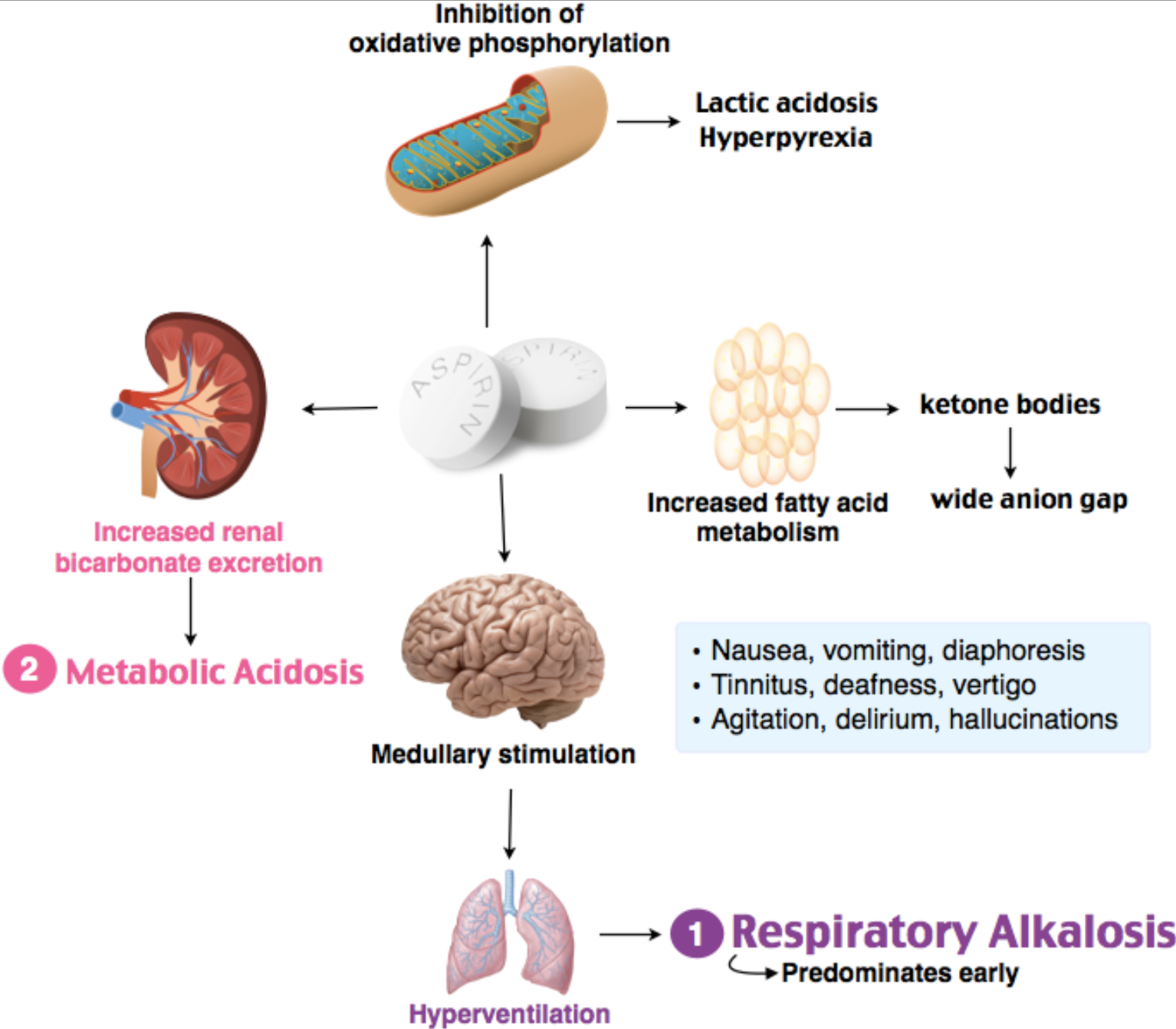
Image Reproduced with permission from Rosh Review
History/Exam
- Consider co-ingestions, and ask patient about any other pills/drugs taken
- Approximately 1/3 of adults who intentionally overdose of aspirin also ingest other substances
- Ask about source and quantity as salicylate concentrations vary widely depending on the formulation
- In acute ingestions early symptoms of toxicity include: tinnitus, tachypnea, hearing loss, dizziness, and nausea/vomiting,
- Usually within 1-2 hours of acute ingestion
- Subsequent symptoms that occur at a higher serum salicylate concentration include: hyperpyrexia, diaphoresis, altered mental status (seizure, agitation, lethargy), hypoglycemia, noncardiogenic pulmonary edema, and shock
- Serum concentrations >150 mg/kg
- Acute Kidney Injury (AKI) can lead to salicylate overdose even with therapeutic doses; this is especially true with the elderly
- Chronic Toxicity
- Important to ask patients (especially elderly) about chronic/repeated salicylate ingestion as this is more serious and associated with higher mortality than acute overdoses; these patients tend to have multiple medical problems
- Toxicity occurs at lower doses than acute toxicity and symptoms may be prolonged
- Duration of symptoms can be prolonged and mimic infection
- Fever, tachypnea, acid-base disturbance, noncardiogenic pulmonary edema
Differential
- Consider toxicologic and non-toxicologic causes
- Infection/Sepsis, renal failure, liver disease, carbon monoxide toxicity, cyanide toxicity, metformin toxicity, iron toxicity, INH, DKA, Alcoholic Ketoacidosis, Reye’s syndrome, beta-agonist toxicity
Diagnostics
- Labs/Imaging: CBC, renal and liver function, electrolytes, VBG, Salicylate Serum Concentration, APAP Level, EtOH level, Chest X-Ray
- Salicylate Serum Concentration
- Acute Ingestion:
- >30 mg/dl = Tinnitus
- > 90-100 mg/dl = Significant Toxicity
- Chronic Ingestion:
- 40-60 mg/dl = Significant Toxicity
- VBG/ABG
- Respiratory alkalosis occurs early
- Metabolic acidosis occurs later
- BMP
- Assess K+, glucose, Mg, and Phos
- Creatinine: Assess renal function
- Chest X-Ray
- Obtain if any clinical signs pulmonary edema
- Head CT
- Depends on clinical picture; should be considered if AMS or focal neurologic defect can not be attributed to noncerebral cause (ie. hypoglycemia)
- Acute Ingestion:
Treatment
- ABCD
- Airway/Breathing
- Avoid intubation unless clear signs of respiratory failure. Sedation causes blunting of compensatory respiratory drive which can worsen acidosis and lead to clinical decompensation.
- If intubation is necessary it is imperative that hyperventilation is maintained
- Circulation
- May be hypotensive due to sensible/insensible fluid losses and inappropriate vasodilation. Give fluids as needed. If blood pressure does not respond to fluids start pressors
- Decontamination
- Activated Charcoal (1g/kg up to 50 g) effectively absorbs aspirin and should be considered within 2 hours of ingestion in patients who have normal mental status, tolerating PO, and have low risk of aspiration
- Can be given via NG/OG tubes in intubated patients
- Call toxicologist/poison control center early in treatment
- Plasma and Urinary Alkalinization
- Primary method of salicylate elimination
- Mechanism of Action
- Acetylsalicylic Acid is a weak acid (pKa 5) and tends to be absorbed in acidic environments
- Sodium Bicarb is utilized to increase the urinary pH (7.5) to decrease renal tubular reabsorption thus renally excreting the toxin
- Only unionized molecules can cross the phospholipid bilayer
- If toxin pKa < pH of the environment, the ionized conjugate base (anion) of aspirin will be trapped in the urine and unable to cross the phospholipid bilayer of renal tubular cells
- Henderson-Hasselbach equation: pH= pKa+ log (A–/HA)
- Check out http://www.emdocs.net/toxcards-absorption-toxicokinetics/ for deeper dive
- IV Sodium Bicarb
- Initial bolus: 1-2 mEq/kg IVP over 1-2 minutes
- Infusion: 3 amps (150 mEq) with 40-50 mEq KCl in 1 L of D5W at 150-200 mL/h (or 2x maintenance in peds)
- “5,4,3,2,1” Pneumonic
- 5- D5W
- 4- 40 mEq KCL
- 3- 3 amps Sodium Bicarb
- 2- 2 x maintenance rate
- 1- Mixed in 1 L bag of D5W
- Goal Serum pH 7.45-7.55
- Goal Urine pH >7.5
- Correct K+ to high normal concentrations. Important for salicylate excretion
- Replete glucose, Mg, and Phos as needed
- Hemodialysis
- Standard of care for those patients who are critically ill, altered mental status, or pulmonary edema
- Aspirin elimination occurs via the kidneys, therefore renal failure is an absolute indication for hemodialysis
- Consider HD in patients who have worsening acid/base dysfunction despite aggressive treatment
- Acute Serum Concentration >90 mg/dl
- Chronic Serum Concentration >60 mg/dl
- Standard of care for those patients who are critically ill, altered mental status, or pulmonary edema
- Check ASA serum levels every 2 hours until concentration decreases, then every 4-6 hours until level is non-toxic
- Airway/Breathing
Disposition
- Continue treatment until salicylate concentration is <30 mg/dL
- Discharge from ED when there has been clinical improvement, no significant acid/base derangements, and down-trending salicylate levels with at least two levels <30 mg/dL
- If despite treatment patient’s symptoms continue to worsen or salicylate concentrations rise, the patient should be admitted
- If overdose was deliberate, obtain psychiatric consultation prior to discharge

A 27-year-old woman with a history of depression presents with abdominal pain and tinnitus. She says she is sad because her husband recently divorced her. She denies homicidal ideations or hallucinations. She intentionally took 18 324 mg aspirin tablets approximately six hours prior to arrival. Her vital signs are T 100.1ºF, BP 125/85 mm Hg, P 104 beats/minute, RR 26 breaths/minute, and oxygen saturation 99% on room air. She has hemoccult negative stool. Her serum salicylate level is 39 mg/dL. Toxicology and psychiatry are consulted. Sodium bicarbonate is administered. What is the endpoint of sodium bicarbonate administration?
A) Cessation of tinnitus
B) Serum bicarbonate > 25 mmol/L
C) Serum pH 7.45 to 7.55
D) Urine pH 7.45 to 7.55
Answer: C
Clinical signs and symptoms of acute salicylate toxicity are seen at serum salicylate levels above 30 mg/dL (therapeutic range is 10 to 20 mg/dL). This level correlates with an ingestion of > 150 mg/kg of salicylates. Salicylates are found in a variety of medications such as analgesics, antipyretics, antidiarrheal medications, acne treatments, Chinese herbal preparations, oral antiseptic rinses, and topical ointments (e.g., oil of wintergreen). Initial manifestations of toxicity include otic symptoms (e.g., tinnitus), nausea, vomiting, fever, and diarrhea. Other clinical signs can include vertigo, delirium, seizures, lethargy, cerebral edema, and coma. Salicylate toxicity classically causes a mixed acid-base disturbance beginning with primary respiratory alkalosis. This is due to stimulation of the medullary respiratory center, causing hyperventilation. Over time, the uncoupling of oxidative phosphorylation leads to hyperthermia, and elevated anion gap metabolic acidosis develops. Management involves airway management, fluid resuscitation, gastric decontamination, and alkalinization for serum salicylate levels > 40 mg/dL. This is achieved with an initial 1 to 2 mEq/kg sodium bicarbonate bolus followed by an infusion with 3 ampules (150 mEq) of sodium bicarbonate in 1 L of 5% dextrose in water (D5W) at a rate of 1.5 to two times the maintenance rate. This is titrated to a goal serum pH of 7.45 to 7.55 or a urine pH of 7.50 to 8.0. Indications for hemodialysis for salicylate toxicity include pulmonary edema, severe metabolic acidosis, altered mental status, coagulopathy, renal failure, clinical deterioration despite supportive care, and absolute serum salicylate level > 100 mg/dL in acute poisonings and > 60 mg/dL in chronic poisonings.

The clinical endpoint for alkalinization is not cessation of tinnitus (A), serum bicarbonate > 25 mmol/L (B), or urine pH 7.45 to 7.55 (D). It is a serum pH of 7.45 to 7.55 or a urine pH of 7.5 to 7.8.
Further Reading:
References:
Hill JB, Department of Biochemistry. Salicylate Intoxication: NEJM. New England Journal of Medicine. https://www.nejm.org/doi/full/10.1056/NEJM197305242882107. Accessed April 23, 2020.
Katz KD, O’Connor AD. EMRA AND ACMT MEDICAL TOXICOLOGY GUIDE. Irving, Tx: EMRA; 2018.
Cydulka RK, Fitch MT, Nogar JN. et al. Tintinallis Emergency Medicine Manual. 8th ed. New York, NY: McGraw-Hill Education; 2018.
Gabow PA, Anderson RJ, Potts DE, Schrier RW. Acid-base disturbances in the salicylate-intoxicated adult. Archives of internal medicine. https://www.ncbi.nlm.nih.gov/pubmed/?term=708168. Published October 1978. Accessed April 23, 2020.
Boyer EW, Weibrecht KW. Salicylate (Aspirin) Poisoning in Adults. UpToDate. https://www.uptodate.com/contents/salicylate-aspirin-poisoning-in-adults?search=salicylate toxicity&source=search_result&selectedTitle=1~115&usage_type=default&display_rank=1. Published January 14, 2020. Accessed April 23, 2020.
Leatherman JW, Schmitz PG. Fever, hyperdynamic shock, and multiple-system organ failure. A pseudo-sepsis syndrome associated with chronic salicylate intoxication. Chest Jounal. https://www.ncbi.nlm.nih.gov/pubmed/?term=1935299. Published November 1991. Accessed April 23, 2020.
Botma M, Colquhoun-Flannery W, Leighton S. Laryngeal oedema caused by accidental ingestion of Oil of Wintergreen. International Journal of Pediatric Otorhinolaryngology. 2001;58(3):229-232. doi:10.1016/s0165-5876(01)00453-0
Feldman S, Chen S-L, Pickering LK, Cleary TG, Ericsson CD, Hülse M. Salicylate absorption from a bismuth subsalicylate preparation. Clinical Pharmacology and Therapeutics. 1981;29(6):788-792. doi:10.1038/clpt.1981.112







1 thought on “EM@3AM: Salicylate Overdose”
Pingback: Quiz 73, June 26th, 2020 – The FOAMed Quiz