Authors: Thomas Aubuchon, MD (EM Intern, NMCP, LT MC USN) and Eric Sulava, MD (EM Chief Resident, NMCP, LT MC USN) // Reviewed by: Brit Long, MD (@long_brit) and Alex Koyfman, MD (@EMHighAK)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 57-year-old male with a history of hypertension, diabetes, gastroesophageal reflux disease, and chronic osteoarthritis presents with several hours of progressively worsening epigastric pain. He noticed a flare of his chronic shoulder pain, for which he has been taking motrin all week. Shortly after dinner he felt a sharp pain in his epigastric region, unlike his previous “heartburn” pains. He tried antacids with no improvement. As the pain worsened, he began to notice lightheadedness and ‘sweating spells’.
Initial Vitals: HR 107, BP 132/86, RR 26, SpO2 95%, Temp 99.3⁰F
Exam: Diaphoretic male who appears to be in mild distress. He is fully oriented and answering all questions in a goal directed manner. Cardiopulmonary exam shows tachycardia and tachypnea, with no other abnormal findings. Abdominal exam shows diffuse tenderness with guarding.
Evaluation: Portable CXR and EKG reveal no acute abnormalities.
What is your diagnosis? What are you most concerned about?
Answer: Peptic ulcer disease with concern for viscus perforation and peritonitis
Background and Epidemiology:
- Peritonitis is an urgent condition that can result from infection, inflammation, vascular occlusion, or obstruction.
- Visceral perforation or trauma is one of the leading causes of peritonitis and sepsis.
- Perforated viscus and peritonitis is life threatening and carries a mortality of up to 30-50% if the patients become septic.
Pathophysiology:
- Perforation requires full thickness injury to the bowel.
- Perforation can be from external causes such as instrumentation and trauma or internal causes such as obstruction, inflammation, ulcerative disease.
- Spillage of intestinal contents into the peritoneum is the ultimate consequence of perforation.
- The peritoneum is a sterile environment that can react to various pathologic insults with an inflammatory response.
- Visceral nerves of the autonomic system are sensitive to mechanical distention, inflammation, ischemia, and intense smooth muscle contraction. These pain sensations often localize to epigastrum or midgut instead of the portion of the abdomen the irritant originated from.
- Parietal nerve fibers are somatic fibers that respond to irritation in specific dermatomes and therefore can be localized.
- Somatic irritation, as it increases, will lead to rigidity and guarding of the abdomen.
Risk Factors:
- Factors that increase the risk for gastrointestinal (GI) perforation are discussed below. Consider the following factors when taking the history of any patient suspected of having GI perforation.

Presentation:
History
- A careful history should be taken with attention to the following:
- History of Present Illness:
- Start with: Onset, Provocation, Quality, Region/Radiation, Severity, Time.
- Refer to Table 1 to assess for high risk etiologies.
- Allow anatomy and location to help narrow the differential.
- See Table 2 for an example on how historical factors can guide your differential and evaluation.
- Careful review of systems (ROS) for associated symptoms
- Past medical/surgical history
- Gynecologic History
- The menstrual history is crucial to the diagnosis of ectopic pregnancy, mittelschmerz, and endometriosis.
- Surgical History
- To assess risk of abdominal scarring, bowel obstruction, post operative complication.
- Clarify anatomic reconstructions.
- Medication History
- Anticoagulants (hematoma), oral contraceptives (benign hepatic adenomas / mesenteric venous infarction), corticosteroids (may mask advanced peritonitis), immune modulators, etc.
- Social Hx:
- Tobacco: delayed wound healing
- Street drugs: increased risk ischemia / perforation
- Family History
- Insight to medical causes of an acute abdomen.
- Travel History
- Location to consider amebic liver abscess / hydatid cyst, malarial spleen, tuberculosis, Salmonella typhi infection, dysentery.
- Gynecologic History
- Start with: Onset, Provocation, Quality, Region/Radiation, Severity, Time.
- History of Present Illness:
Physical exam
- Vitals
- Signs of sepsis, SIRS Criteria
- Temperature higher than 38°C (100.4°F) or lower than 36°C (96.8°F)
- Heart rate (HR) higher than 90 beats/min
- Respiratory rate (RR) higher than 20 breaths/min or arterial carbon dioxide tension (PaCO2) lower than 32 mm Hg
- White blood cell (WBC) count higher than 12,000/µL or lower than 4000/µL or with 10% immature (band) forms
- Inspection
- Distension
- Masses
- Surgical scars
- Auscultation
- Decreased sounds can suggest ischemia or peritonitis.
- Increased sounds can suggest obstruction.
- Percusion
- Tympany with distention can suggest obstruction.
- Palpation
- Somatic fibers and localized pain can narrow down to specific organs.
- Guarding and rigidity suggests peritoneal irritation.
- Lower abdominal/pelvic exams can be helpful to recognize pelvic organs as source of perforation and peritonitis.
- GU exam is helpful and necessary for that same reason, to evaluate pelvic organs as source of perforation and peritonitis.
- Palpation of the chest and neck for subcutaneous air.
- Signs of sepsis, SIRS Criteria

Evaluation:
Labs: Evaluation is largely determined on exam. Labs are usually nonspecific in the setting of bowel perforation, but can be helpful if positive
- CBC: Marked leukocytosis/significant left shift can be indicative of serious infection.
- Serum electrolytes, urea nitrogen, and creatinine: will help evaluate for hypovolemia – shock
- ABG / Lactate: can be indicative of sepsis / ischemic bowel / peritonitis; noting lactate elevation / unsuspected metabolic acidosis.
- In suspected hepatobiliary disease, liver function tests are useful to differentiate medical from surgical hepatic disorders.
- Clotting studies can be helpful in possible hematologic abnormality (cirrhosis, DIC, petechiae) if surgical intervention is suspected.
Imaging:
- Plain films: 30% sensitive and 50-70% specific for bowel perforation. Cannot rule-out perforation if negative.
- Highest yield: visible free air under the diaphragm. Most pronounced on upright films. This is an indication for surgical exploration.
- CT: Can diagnose perforation with a sensitivity of 92%, a specificity of 94%, and negative and positive predictive accuracies of 100% and 30%, respectively.
- Findings to suggest perforation on abdominal CT:
- Extraluminal air / oral contrast, free fluid, discontinuity of the intestinal wall, fistula, or intra-abdominal abscess with irregular adjacent bowel wall thickening.
- Other imaging studies:
- Depending on the clinical context advanced imaging studies can be used.
- Other imaging studies include endoscopy (upper, lower), esophagography, upper gastrointestinal series, ultrasound, contrast enema, and dye studies.
- Barium should not be used as the initial oral contrast agent because it can produce granulomas in the tissues if it leaks out.
- Water soluble contrast is preferred if utilized.
- Depending on the clinical context advanced imaging studies can be used.
- Findings to suggest perforation on abdominal CT:
Management & Disposition:
- Early management of the peritoneal focuses on conservative and symptomatic care.
- These patients, especially when showing signs of sepsis, require two large bore IVs, fluid resuscitation, broad spectrum antibiotics, and surgical consideration.
- Broad spectrum antibiotics covering gram negative organisms should be started unless perforation site can be specified by imaging and antibiotics can be better tailored.
- Most patients will require surgical intervention, if truly peritoneal.
- Non-operative care can be considered if there is a contained perforation, enteric fistula formation, or non-septic patient.
- Surgical consultation to assist in the decision for surgical intervention is warranted.
Pearls:
- Early resuscitation with fluids and antibiotics in any suspected perforation.
- Allow your risk factors guide your differential! (Table 1).
- Early surgical consult in any suspected perforation.
- This is often a clinical diagnosis. The abdominal exam can be helpful, but be wary in immunocompromised and elderly patients.
- Imaging can help; however, do not rely on radiographs (especially plain films). CT may be needed for definitive diagnosis.

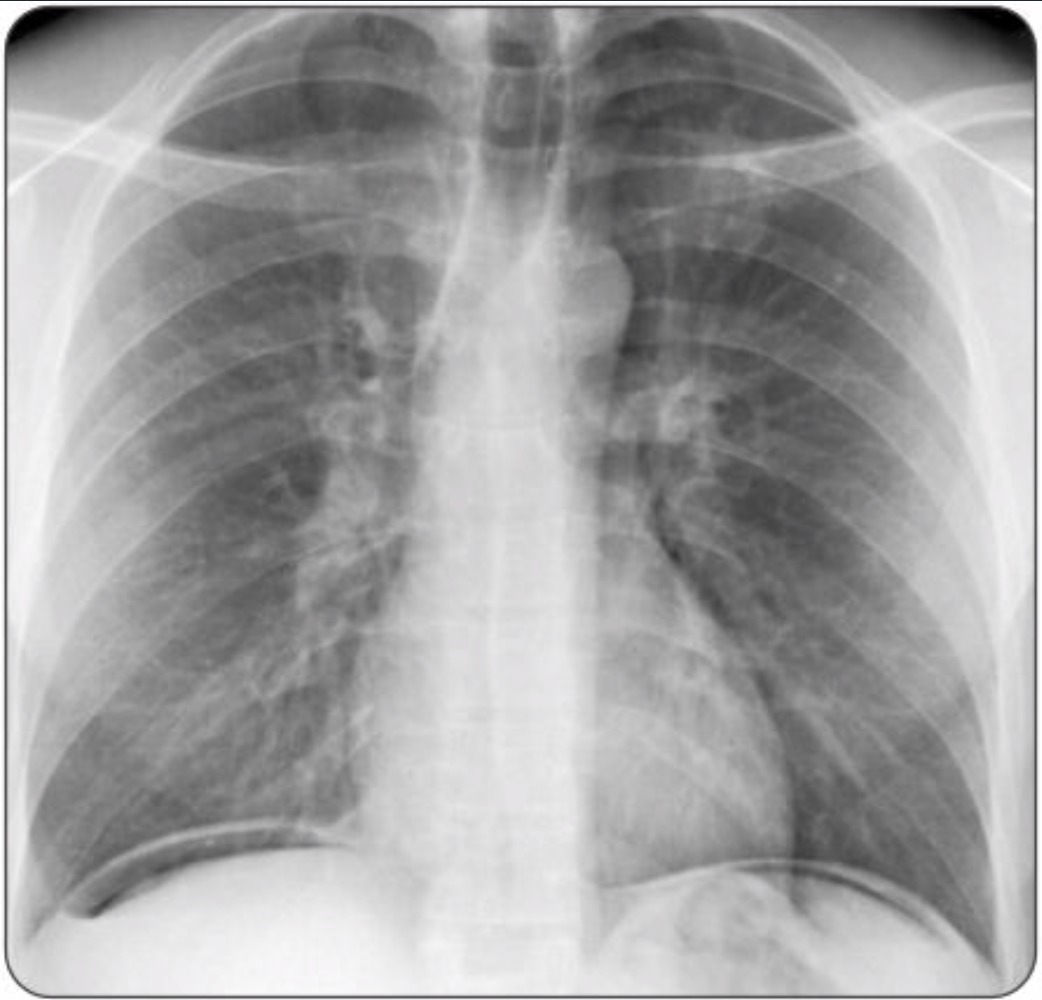
A 75-year-old man presents to the emergency department with sudden and severe abdominal pain. The patient has a past medical history of osteoarthritis and peptic ulcer disease and is currently taking ibuprofen and acetaminophen. A chest radiograph is performed, as seen above. Which of the following is the best next step in management?
A) Obtain a serum lipase
B) Perform a right upper quadrant ultrasound
C) Perform an exploratory laparotomy
D) Perform endoscopic retrograde cholangiopancreatography
Answer: C
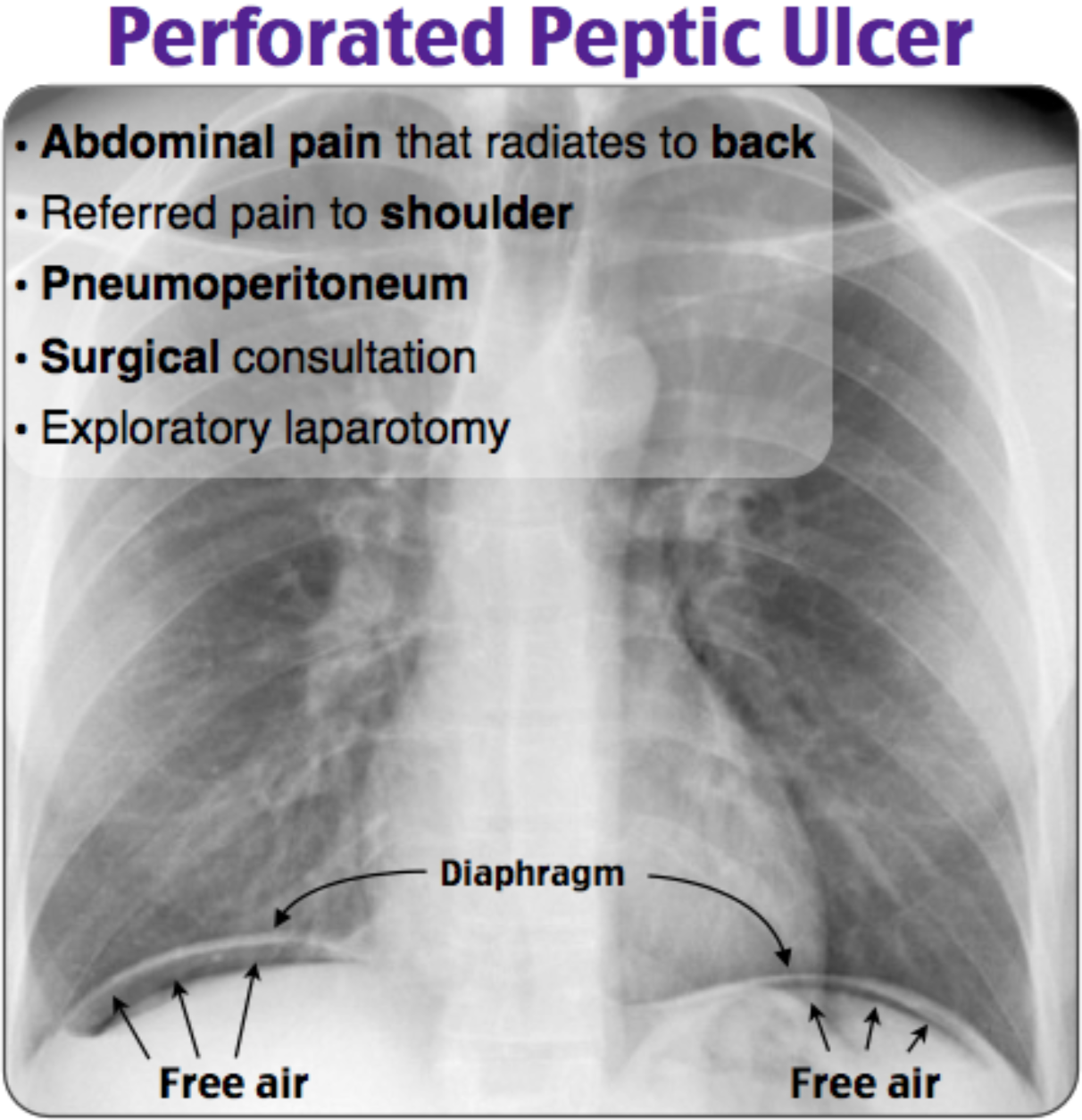
This patient is presenting with severe abdominal pain and a radiograph demonstrating free air under the diaphragm, suggesting a diagnosis of a perforated viscus, which warrants an emergency exploratory laparotomy. A perforated viscus presents with severe and sudden abdominal pain that is typically generalized. The patient will typically remain in an antalgic position and will refuse to move. Abdominal pain that radiates to the back and referred shoulder pain are additional findings that could support the diagnosis of a perforated viscus. Risk factors for a perforated viscus include a history of diagnoses such as peptic ulcer disease, diverticulitis, and trauma. The diagnosis can be supported with free air under the diaphragm on upright chest radiograph (pneumoperitoneum). Any patient presenting with free air under the diaphragm on chest radiography should be emergently evaluated with an exploratory laparotomy. Fluid resuscitation and broad-spectrum antibiotics are also indicated.
Obtain a serum lipase (A) is a specific diagnostic test for pancreatitis, which presents with epigastric pain that is associated with alcohol consumption or fatty food consumption. Perform a right upper quadrant ultrasound (B) is appropriate management of acute cholcystitis or choledocholithasis. Acute cholecystitis presents with right upper quadrant abdominal pain and tenderness, and is more common in middle-aged and overweight women. Ultrasound would demonstrate an enlarged gallbladder with wall thickening and pericholecystic fluid. Perform endoscopic retrograde cholangiopancreatography (D) is appropriate management of biliary tract pathologies such as ascending cholangitis, which presents with fever, jaundice, and right upper quadrant tenderness. A sphincterotomy and stone removal can be performed with this procedure, thus removing the obstruction.
Further Reading:
References:
- Abid, S., et al. “Pill-Induced Esophageal Injury: Endoscopic Features and Clinical Outcomes.” Endoscopy, vol. 37, no. 8, 2005, pp. 740–744., doi:10.1055/s-2005-870129.
- Furukawa, A., et al. “Gastrointestinal Tract Perforation: CT Diagnosis of Presence, Site, and Cause.” Abdominal Imaging, vol. 30, no. 5, 2005, pp. 524–534., doi:10.1007/s00261-004-0289-x.
- Karanikas, I. D., et al. “Barium Peritonitis: a Rare Complication of Upper Gastrointestinal Contrast Investigation.” Postgraduate Medical Journal, vol. 73, no. 859, 1997, pp. 297–298., doi:10.1136/pgmj.73.859.297.
- Langell, John T., and Sean J. Mulvihill. “Gastrointestinal Perforation and the Acute Abdomen.” Medical Clinics of North America, vol. 92, no. 3, 2008, pp. 599–625., doi:10.1016/j.mcna.2007.12.004.
- Nassour, Ibrahim, and Sandy H. Fang. “Gastrointestinal Perforation.” JAMA Surgery, vol. 150, no. 2, 2015, p. 177., doi:10.1001/jamasurg.2014.358.
- New York: McGraw-Hill Education. Tintinalli, Judith E.,, et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. Eighth edition. New York: McGraw-Hill Education, 2016.
- Nicolaou, Savvas, et al. “Imaging of Acute Small-Bowel Obstruction.” American Journal of Roentgenology, vol. 185, no. 4, 2005, pp. 1036–1044., doi:10.2214/ajr.04.0815.
- Rubesin, Stephen E, and Marc S Levine. “Radiologic Diagnosis of Gastrointestinal Perforation.” Radiologic Clinics of North America, vol. 41, no. 6, 2003, pp. 1095–1115., doi:10.1016/s0033-8389(03)00100-3.
- Wu, James T., et al. “Esophageal Perforations: New Perspectives and Treatment Paradigms.” The Journal of Trauma: Injury, Infection, and Critical Care, vol. 63, no. 5, 2007, pp. 1173–1184., doi:10.1097/ta.0b013e31805c0dd4.
- Zafar, S. Nabeel, et al. “Outcome of Selective Non-Operative Management of Penetrating Abdominal Injuries from the North American National Trauma Database.” British Journal of Surgery, vol. 99, no. S1, 2011, pp. 155–164., doi:10.1002/bjs.7735.
Acknowledgements:
We are military service members. This work was prepared as part of our official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines a United States Government work as a work prepared by a military service member or employee of the United States Government as part of that person’s official duties.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.






