Authors: Brit Long, MD (@long_brit, EM Attending Physician at SAUSHEC), Josh Oliver, MD (EM Resident at SAUSHEC, USA), and Matthew Streitz, MD (EM Chief Resident at SAUSHEC, USAF) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Please see ABEM’s Key Advances Heart Score synopsis for more information. Also be sure to check out the educational video.
Case:
A 52-year-old male presents with 6 hours of chest pain, radiating to the left shoulder and associated with shortness of breath. He has a history of hypertension. His vital signs and ECG are normal. His initial troponin is normal. You consider entering him into your center’s chest pain pathway, with repeat troponin in two hours.
Chest pain is common in the ED; for the majority of physicians not a single shift will go by without managing at least one patient with chest pain. Approximately 10% of visits to an ED are due to chest pain.1,2 Fear of myocardial infarction often predominates for both patients and physicians.1,2 However, acute coronary syndrome (ACS) accounts for a minority of these patients. In fact, less than 1% of acute myocardial infarctions (MI) are missed by emergency physicians.3,4 Historically, physicians admitted patients with obvious disease (such as STEMI or non STEMI), while other patients underwent some form of further stress testing, either as an inpatient, outpatient dedicated clinic, or in an observation unit. We now know this further risk stratification in patients with negative biomarkers and unchanged ECG offers little, if any benefit.5,6 Testing can lead to over-diagnosis and over-treatment.
The majority of physicians feel a rate of < 1% or 1-2% is appropriate for missed major cardiovascular adverse event (MACE).4,7 Investigators have sought a tool to consistently and efficiently risk stratify patients to less than 1% risk of MACE.8-14 Patients in this low risk category could potentially be discharged directly from the ED. Prior risk scores or decision aids include the TIMI risk score and GRACE, for example.8-12 These scores were not derived for use in the undifferentiated chest pain patient in the ED, but rather for high risk patients to evaluate for the need for invasive therapy.8-12 They are also complex and difficult to use.
The HEART score and pathway have revolutionized care of chest pain patients in the ED.13-17 The introduction of the HEART score demonstrated ability to stratify a significant percentage of patients as low risk and appropriate for discharge, and the HEART pathway with the addition of repeat troponin further decreases the risk of missed ACS to less than 1%.13-17
Many centers use this pathway. However, are there potential weaknesses when using this score or pathway? This post will evaluate these potential weaknesses. But to look for weaknesses, first let’s evaluate the HEART score and pathway. The initial HEART score is shown below.13,14

As you can see, the HEART score consists of age, risk factors, history, ECG, and troponin. Low risk patients, defined by points 0-3, demonstrate low rate of major cardiovascular adverse event (MACE). The original study evaluating the HEART score spanned three months in the Netherlands, finding one third of patients to be low risk.13 The MACE rate in the low risk group was 2.5%. Since this initial study, the score has been repeatedly validated using multiple methods, with MACE rate less than 2%.14-16
The HEART pathway can further decrease the miss rate, evaluated by Mahler et al.17 This pathway uses a HEART score of 0-3 and negative troponins. Use of this pathway has repeatedly demonstrated ability to risk stratify a large percentage of patients as low risk appropriate for discharge (some studies 40%), with low rate of MACE (< 1%).17
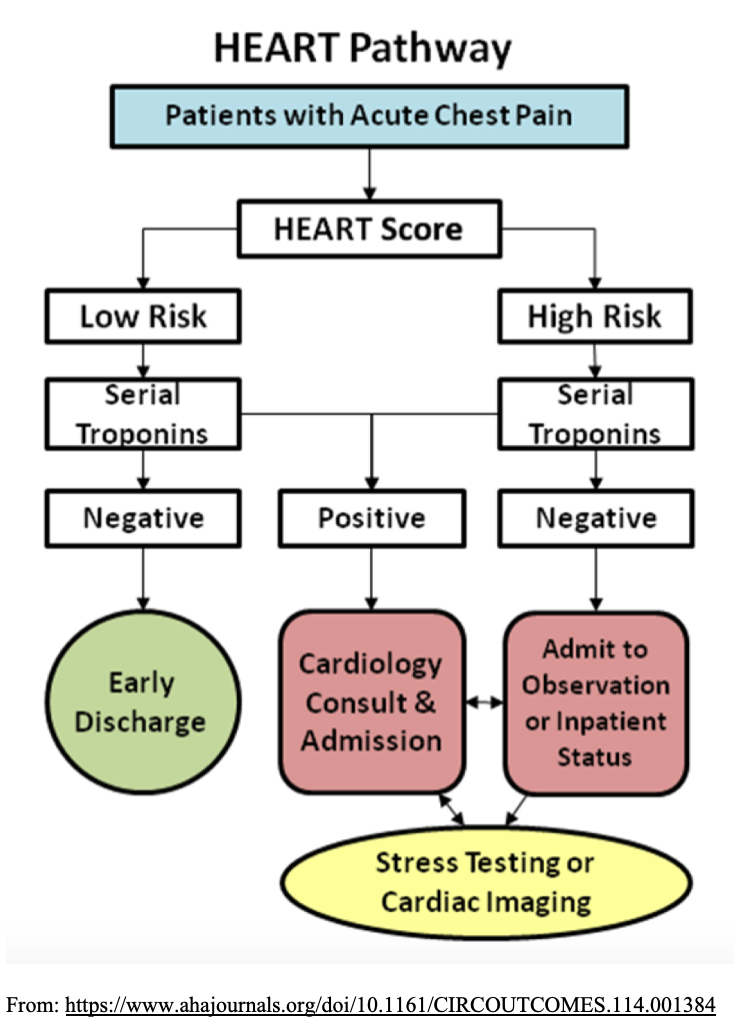
The HEART pathway has demonstrated its utility, but where can it go wrong?
#1: Risk Factors –
Classically, cardiac risk factors (diabetes, hypertension, smoking, hyperlipidemia, family history) have been used to predict the presence or absence of ACS in chest pain. These risk factors were derived in longitudinal studies and likely play little role in the assessment of the patient in front of you.18,19 Jayes et al. finds that no risk factor increases likelihood of ACS in women, while in men, only diabetes and family history increase likelihood.18 A study by Han et al. finds patients over age 65 years overwhelms any other risk factors for predicting ACS, while in patients less than 40, the number of risk factors contributes to risk of ACS.19
The patient may deny medical problems if they never visit a physician or primary care manager. This would potentially give them 0 points, categorized as low risk, no matter the other factors. The patient may not say they have hypertension, hyperlipidemia, or diabetes, but usually when you see an obese patient with BP of 180/90 and blood glucose level of 188, you know better.
Tip: If the patient is hypertensive or has abnormal serum glucose, assume they have these risk factors and score them appropriately. Remember, obesity is a risk factor in the HEART score, and known cardiac disease, cerebrovascular disease, or prior stroke is 2 points on the risk score.13-17
#2: ECG –
Significant ST depressions, nonspecific repolarization abnormalities, and normal define the specific categories on the score. Just like above, dynamic ECG changes with no other points on the HEART score could provide a score of 2, which theoretically would place the patient in the low risk category. Approximately 8-11% of patients will demonstrate normal initial ECGs, and in patients with STEMI, up to one third will demonstrate findings on ECG by 30 minutes.20,21 Another potential weakness is misinterpretation of the ECG.
Tip: The ECG must be viewed systematically and thoroughly. Obtain an old ECG if at all possible to look for changes. Do not dismiss T wave changes (such as hyperacute T waves or inversions). These T wave changes must be taken seriously, and repeat ECGs are a necessity, as changes may not be present on the initial ECG.
#3: Troponin –
An elevated troponin (2 points) with no other points would categorize the patient as low risk on the HEART score. However, troponin elevation should be considered high risk and criteria for admission. The HEART pathway with troponin elevation takes this into account, with positive troponin resulting in admission for the patient.
Tip: Elevated troponin equals admission. The HEART pathway takes this into account.
#4: Age –
Patients greater than 65 years receive two points. However, if they receive 0 points in other categories, this results in a score of 2, which is low risk based on scoring. Progressing age has consistently proven to be a risk factor for ACS, and these patients may not present with chest pain.22 Be wary of the patient with dyspnea, nausea/vomiting, and fatigue who is older.22-27 Also be concerned about the younger patient (such as a 35-year-old) with no risk factors and a story strongly suggestive of ACS.
Tip: Older patients warrant caution. Many do not present typically with chest pain, diaphoresis, and vomiting. Dyspnea is more common. The key for older patients is atypical equals typical.22,27
#5: History –
The original HEART score study by Six et al. utilized two investigators to classify patient history.13 Literature demonstrates the most predictive factors of ACS include diaphoresis with chest pain, nausea and vomiting, pain radiation to both arms or right shoulder, and exertional pain.23-26 Chest wall tenderness, pleuritic chest pain, sharp/stabbing chest pain, positional chest pain, and reproducible chest pain decrease the likelihood.23-26 Carefully take a history, and evaluate for these factors.
Tip: Though the prior factors (diaphoresis, vomiting, exertional pain, radiation to both arms/right shoulder) increase the likelihood of ACS, up to 1/3 of patients will present with dyspnea, fatigue, or nausea.27,28 Pay close attention to diabetics, older patients, women, and heart failure patients, as these groups can present atypically.22,27 Atypical presentations are associated with increased mortality.
#6: Gestalt –
EM physicians go through extensive training, resulting in tremendous clinical experience and gestalt. How does gestalt compare to the HEART score? Mahler et al. in 2013 compared unstructured physician assessment, HEART score, and North American Chest Pain Rule, each with serial troponins (0 and 3 hrs).17 The HEART score classified 20% of patients as low risk (with 99% sensitivity) compared to gestalt categorizing 13.5% of patients as suitable for discharge (98% sensitivity).17 However, many institutions that utilize the HEART pathway incorporate clinical gestalt.
Tip: Your experience evaluating these patients is invaluable.7 If the HEART score says the patient is low risk but your gestalt says something different, discuss this with your admitting team and the patient. Many missed cases of ACS are associated with younger patients with no risk factors but a concerning story for cardiac etiology of their chest pain. The patient likely warrants admission in this setting.
#7: Follow up –
Some institutions that utilize the HEART pathway and discharge patients with scores 0-3 attempt to have patients follow up with their primary care physician. Mahler et al.’s HEART pathway study encouraged follow up, but did not mandate it.17 As many know, follow up isn’t always possible. Patients with borderline scores (such as a score of 3), may not be able to see a primary care physician for another visit. However, the AHA/ACC recommend further stratification within 72 hours of discharge, though many are moving from this.29
Tip: Advise your patient to follow up, and document the discussion. Ensure return precautions are provided, and more importantly, that the patient verbalizes and understands these precautions.
#8: Points 3 or 4 –
The dividing line for low risk is 3, while a score above 3 is moderate or high.13-17 The line between 3 or 4 points can be gray, dependent on which areas receive points. A history given 1 point may be 2 points based on the assessment of another physician. A study evaluating MACE rate for each number of points on HEART would provide valuable information on the score and pathway.
#9: Research Design –
This post will not delve into the design of the HEART score/pathway trials, but several items should be considered. First is pathway adherence in the studies, as some nonadherence was observed. Another component is potential physician disagreement on scoring. Some studies do not list HEART interobserver agreement, while others state that physicians were notified if any disagreement occurred.
How can we improve on the HEART score?
The risk of ACS in patients admitted with chest pain, normal ECG, and negative troponin is close to 0.2%.3 The HEART pathway provides support for discharging patients with scores 0-3. Some have sought means of improving the score. One study modified the score by weighing male gender separately, as well as obtaining serial troponins and ECGs over 2 hours.30 This is known as the HEARTS(3) score. The S(3) correlates to sex, serial 2-hour ECG, and serial 2 hour delta troponin. Investigators also find that history highly suspicious of ACS (+LR 13) is much stronger than 3 or more CAD risk factors or age over 65 (+LR 1.4).30 Serial troponins and serial ECGs may improve miss rates, but most providers obtain serial ECG and troponins in patients with chest pain.
Further areas of study include disposition and medical decision making in patients with scores 4-6, or intermediate risk patients. These patients have approximately 12-16% risk of MACE.13-17 Does stress testing add to this population? The benefits of stress testing are controversial, and further risk stratification with these tests is difficult.
What about the use of coronary CTA in moderate risk patients? If this test demonstrates no disease (or less than 50%), the risk of ACS is very low.31-37 However, the majority of the literature has evaluated the use of CCTA in patients already at low risk for ACS.33-37 Perhaps a pathway using CCTA for patients with scores 4-6 may allow discharge and further risk stratification, but this requires more study.
Summary and Takeaways:
– The risk of ACS in patients with negative biomarkers and normal ECGs approaches 0.2%.
– Prior risk scores, such as TIMI and GRACE, provide little, if any benefit, in risk stratification for ED chest pain patients.
– The HEART score and pathway can risk stratify patients into three separate categories: low (0-3), moderate (4-6), and high score (> 7).
– Low risk patients on the HEART pathway demonstrate likelihood of ACS that approaches < 1%, and it is easy to use in the ED.
– Risk factors, history, ECG, troponin, follow up, gestalt, patients with points 3 or 4, and research design are areas of potential weakness.
– Further improvement of the HEART pathway at this time is difficult, but in patients at moderate risk, CCTA may hold promise for evaluation of risk. This requires further study.
References/Further Reading
- Bhuiya FA, Pitts SR, McCaig LF. Emergency department visits for chest pain and abdominal pain: United States, 1999–2008. NCHS Data Brief. 2010;(43):1–8.
- Pope JH, Aufderheide TP, Ruthazer R, et al. Missed diagnoses of acute cardiac ischemia in the emergency department. N Engl J Med. 2000;342(16):1163–1170.
- Weinstock MB, Weingart S, Orth F, et al. Risk for clinically relevant adverse cardiac events in patients with chest pain at hospital admission. JAMA Intern Med 2015;175: 1207-1212.
- Than M, Herbert M, Flaws D, et al. What is an acceptable risk of major adverse cardiac event in chest pain patients soon after discharge from the Emergency Department? A clinical survey. Int J Cardiol 2013;166:752-754.
- Kosowsky JM. Approach to the ED patient with ‘‘low-risk’’ chest pain. Emerg Med Clin North Am 2011;29:721–7.
- Lai C, Noeller TP, Schmidt K, King P, Emerman CL. Short-term risk after initial observation for chest pain. J Emerg Med 2003;25: 357–62.
- Kline J.A., Johnson C.L., Pollack C.V., et al: Pretest probability assessment derived from attribute matching. BMC Med Inform Decis Mak 2005; 5: pp. 26.
- Antman EM, Cohen M, Bernink PM, et al. The TIMI risk score for unstable angina/non-ST elevation MI: a method for prognostication and therapeutic decision making. JAMA. 2000;284(7):835–842.
- Cohen M, Demers C, Gurfinkel EP, et al. A comparison of low- molecular-weight heparin with unfractionated heparin for unstable coronary artery disease. N Engl J Med. 1997;337:447–452.
- Eagle KA, Lim MJ, Dabbous OH, et al. A validated prediction model for all forms of acute coronary syndrome: estimating the risk of 6-month postdischarge death in an international registry. JAMA. 2004;291(22):2727–2733.
- Lyon R, Morris AC, Caesar D, et al. Chest pain presenting to the Emergency Department – to stratify risk with GRACE or TIMI? Resuscitation. 2007;74(1):90–93.
- GRACE Investigators. Rationale and design of the GRACE (Global Registry of Acute Coronary Events) project: a multinational registry of patients hospitalized with acute coronary syndromes. Am Heart J. 2001;141:190–199.
- Six AJ, Backus BE, Kelder JC. Chest pain in the emergency room: value of the heart score. Neth Heart J 2008;16:191-6.
- Backus BE, Six AJ, Kelder JC, et al. Chest pain in the emergency room. A multicenter validation of the HEART score. Crit Pathw Cardiol 2010;9:164–9.
- Backus BE, Six AJ, Kelder JC, Bosschaert MA, Mast EG, Mosterd A, et al. A prospective validation of the HEART score for chest pain patients at the emergency department. Int J Cardiol 2013 Oct 3;168(3):2153-8.
- Mahler SA, Hiestand BC, Goff DC Jr, Hoekstra JW, Miller CD. Can the HEART score safely reduce stress testing and cardiac imaging in patients at low risk for major adverse cardiac events? Crit Pathw Cardiol 2011;10:128–133.
- Mahler SA, Riley RF, Hiestand BC, Russell GB, Hoekstra JW, Lefebvre CW. The HEART Pathway randomized trial: identifying emergency department patients with acute chest pain for early discharge. Circ Cardiovasc Qual Outcomes 2015 Mar;8(2):195-203.
- Jayes RL Jr, Beshansky JR, D’Agostino RB, Selker HP. Do patients’ coronary risk factor reports predict acute cardiac ischemia in the emergency department? A multicenter study. J Clin Epidemiol. 1992 Jun;45(6):621-6.
- Hans JH, et al. The role of cardiac risk factor burden in diagnosing acute coronary syndromes in the emergency department setting. Ann Emerg Med 2007;49(2):145.
- Welch RD, Zalenski RJ, et al. Prognostic Value of a Normal or Nonspecific Initial Electrocardiogram in Acute Myocardial Infarction. JAMA 2001;286(16):1977-1984.
- Riley RF, et al. Diagnostic time course, treatment, and in- hospital outcomes for patients with ST-segment elevation myocardial infarction presenting with nondiagnostic initial electrocardiogram: a report from the American Heart Association Mission: Lifeline program. Am Heart J 2013 Jan;165(1):50-6.
- Alexander KP, et al. Acute coronary care in the elderly, part I: Non-ST-segment elevation acute coronary syndromes. Circulation 2007;115:2549-2569.
- Body R, Carley S, Wibberley C, McDowell G, Ferguson J, Mackway-Jones K. The value of symptoms and signs in the emergent diagnosis of acute coronary syndromes. Resuscitation. 2010 Mar;81(3):281-6.
- Edwards M, Chang AM, Matsuura AC, Green M, Robey JM, Hollander JE. Relationship between pain severity and outcomes in patients presenting with potential acute coronary syndromes. Ann Emerg Med. 2011 Dec;58(6):501-7.
- Goodacre S, Locker T, Morris F, Campbell S. How useful are clinical features in the diagnosis of acute, undifferentiated chest pain? Acad Emerg Med. 2002 Mar;9(3):203-8.
- Panju AA, Hemmelgarn BR, Guyatt GH, Simel DL. The rational clinical examination. Is this patient having a myocardial infarction? JAMA. 1998 Oct 14;280(14):1256-63.
- Brieger D, et al. Acute coronary syndromes without chest pain, an underdiagnosed and undertreated high-risk group. Insights from the Global Registry of Acute Coronary Events. Chest 2004;126(2):461-9.
- Dorsh MF, et al. Poor prognosis of patients presenting with symptomatic myocardial infarction but without chest pain. Heart 2001;86(5):494-8.
- Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ACC Guideline for the Management of Patients With Non–ST-Elevation Acute Coronary Syndromes: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;64(24):e139-e228.
- Fesmire FM, Martin EJ, Cao Y, Heath GW. Improving risk stratification in patients with chest pain: the Erlanger HEARTS3 score. Am J Emerg Med. 2012 Nov;30(9):1829-37.
- Montalescot G, Sechtem U, Achenbach S, et al. 2013 ESC guidelines on the management of stable coronary artery disease: the Task Force on the Management of Stable Coronary Artery Disease of the European Society of Cardiology. Eur Heart J 2013;34:2949–3003.
- Fihn SD, Gardin JM, Abrams J, et al., American College of Cardiology Foundation/American Heart Association Task Force. 2012 ACCF/AHA/ACP/AATS/PCnA/SCAI/STS guideline for the diagnosis and management of patients with stable ischemic heart dis- ease: a report of the American College of Cardiology Foundation/ American Heart Association task force on practice guidelines, and the American College of Physicians, American Association for Thoracic Surgery, Preventive Cardiovascular nurses Association, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Circulation 2012;126:e354–471.
- Achenbach S. Can coronary computed tomography angiography replace invasive angiography? Yes: it is all about finding the right test for the right person at the right time. Circulation 2015;131: 410–6. discussion 417.
- Stefanini GG, Windecker S. Can coronary computed tomography angiography replace invasive angiography? Coronary computed tomography angiography cannot replace invasive angiography. Circulation 2015;131:418–25. discussion 426.
- deFilippi CR, Rosanio S, Tocchi M, et al. Randomized comparison of a strategy of predischarge coronary angiography versus exercise testing in low-risk patients in a chest pain unit: in-hospital and long- term outcomes. J Am Coll Cardiol 2001;37:2042–9.
- Litt HI, Gatsonis C, Snyder B, et al. CT angiography for safe discharge of patients with possible acute coronary syndromes. N Engl J Med 2012;366:1393–403.
- Redberg RF. Coronary CT angiography for acute chest pain. N Engl J Med 2012;367:375–6.









10 thoughts on “The Great and Powerful HEART Score: Does it have a weakness?”
Thanks for this nice review & discussion of pitfalls. Wondering if you meant to say: “Patients greater than 65 years receive two points. However, if they receive 0 points in other categories, this results in a score of 0. ”
Seems these patients would still have a score of 2 not zero, but their true risk would likely be greater than a young patient with a score of 2.
Thanks!
Kevin Kent
@drkevink
Dr. Kent, thank you for your comment and for reading. You are correct in that a patient over 65 years with no other points would result in a score of 2, which is low risk based on scoring. This has been corrected. Thank you!
-Brit
Thanks for this nice review & discussion of pitfalls. Wondering if you meant to say: “Patients greater than 65 years receive two points. However, if they receive 0 points in other categories, this results in a score of 0. ”
Seems these patients would still have a score of 2 not zero, but their true risk would likely be greater than a young patient with a score of 2.
Thanks!
Kevin Kent
@drkevink
Dr. Kent, thank you for your comment and for reading. You are correct in that a patient over 65 years with no other points would result in a score of 2, which is low risk based on scoring. This has been corrected. Thank you!
-Brit
Very well written! I think this sheds light on the importance of understanding decisions rules as opposed to just writ adherence without waffling from them.
The community hospital I work has instituted a discharge policy on intermediate HEART scores (4-6) after discussion with cardiology (who do not come and evaluate the patient). The hospital has a nice follow up system in place to get them appropriate follow up in 3 days. We are discharging LOTS of chest pain patients but I HATE discharging patients with a risk of MACE of ~15%. Our cardiology group argues that MACE was studied over 2 weeks and thus 3 days is adequate to mitigate the 15% risk. In conjunction with the hospital, carrdiology provides three-day follow up for most patients (despite the AHA/ACC recommendation being for LOW risk chest pain). Has anyone seen any literature on this? Does this sound as scary to readers as it is in my head?
Thanks
Very well written! I think this sheds light on the importance of understanding decisions rules as opposed to just writ adherence without waffling from them.
The community hospital I work has instituted a discharge policy on intermediate HEART scores (4-6) after discussion with cardiology (who do not come and evaluate the patient). The hospital has a nice follow up system in place to get them appropriate follow up in 3 days. We are discharging LOTS of chest pain patients but I HATE discharging patients with a risk of MACE of ~15%. Our cardiology group argues that MACE was studied over 2 weeks and thus 3 days is adequate to mitigate the 15% risk. In conjunction with the hospital, carrdiology provides three-day follow up for most patients (despite the AHA/ACC recommendation being for LOW risk chest pain). Has anyone seen any literature on this? Does this sound as scary to readers as it is in my head?
Thanks
From Dr. Barbra Backus:
What a beautiful blogpost.
My compliments to the authors of EMdocs on this bright overview with al their helpful tips. I think this blogpost is a must read for everyone who starts using the HEART score in their ED.
As asked on twitter I have some supplemental ideas and evidence.
Jacob Six and I have also asked ourselves if we could improve the HEART score. Was it really so simple that the original HEART score was the final station or could we do better? Based on regression analysis of our prospective validation study we made a modified / adjusted HEART score. As stated by dr Long risk factors and age are the weaker elements of the HEART score, while troponin and history could receive a little bit more weight. We showed that the adjusted HEART score has slightly better calibration and discrimination, but without significant benefit on clinical use. This study supports the use of the original HEART score.
https://www.ncbi.nlm.nih.gov/pubmed/27183254
Follow up remains a point of discussion. Some physicians order every patient back for an outpatient visit, while I think that many patients with a low HEART score could be referred to their general practitioner in case of persistent complaints. I think the most important thing is to reassure your patient to revisit a doctor when their symptoms change.
In this light Amal Mattu has made a beautiful blogpost on shared decision making.
http://blog.ercast.org/amal-mattu-low-risk-chest-pain/ …
In the subheading of “Future studies” Dr. Long discusses the added value of an exercise test in risk stratifying patients with an intermediate HEART score. In one of our observational studies we found that an exercise test does not add a lot to the HEART score, since many of these tests are false positive or inconclusive. Only a negative exercise test in a patient with an intermediate HEART adds diagnostic value.
https://www.ncbi.nlm.nih.gov/pubmed/23283413
The interobserver variability of the HEART score remains a subject of interest. I know two studies who are currently running on interobserver variability of the HEART score. Hopefully we will have some results out of this soon.
A study comparing HEART and CTA would be very interesting.
Again I would like to express my sincere compliments to Dr. Long and his colleagues on this beautiful blogpost.
Barbra Backus
From Dr. Barbra Backus:
What a beautiful blogpost.
My compliments to the authors of EMdocs on this bright overview with al their helpful tips. I think this blogpost is a must read for everyone who starts using the HEART score in their ED.
As asked on twitter I have some supplemental ideas and evidence.
Jacob Six and I have also asked ourselves if we could improve the HEART score. Was it really so simple that the original HEART score was the final station or could we do better? Based on regression analysis of our prospective validation study we made a modified / adjusted HEART score. As stated by dr Long risk factors and age are the weaker elements of the HEART score, while troponin and history could receive a little bit more weight. We showed that the adjusted HEART score has slightly better calibration and discrimination, but without significant benefit on clinical use. This study supports the use of the original HEART score.
https://www.ncbi.nlm.nih.gov/pubmed/27183254
Follow up remains a point of discussion. Some physicians order every patient back for an outpatient visit, while I think that many patients with a low HEART score could be referred to their general practitioner in case of persistent complaints. I think the most important thing is to reassure your patient to revisit a doctor when their symptoms change.
In this light Amal Mattu has made a beautiful blogpost on shared decision making.
http://blog.ercast.org/amal-mattu-low-risk-chest-pain/ …
In the subheading of “Future studies” Dr. Long discusses the added value of an exercise test in risk stratifying patients with an intermediate HEART score. In one of our observational studies we found that an exercise test does not add a lot to the HEART score, since many of these tests are false positive or inconclusive. Only a negative exercise test in a patient with an intermediate HEART adds diagnostic value.
https://www.ncbi.nlm.nih.gov/pubmed/23283413
The interobserver variability of the HEART score remains a subject of interest. I know two studies who are currently running on interobserver variability of the HEART score. Hopefully we will have some results out of this soon.
A study comparing HEART and CTA would be very interesting.
Again I would like to express my sincere compliments to Dr. Long and his colleagues on this beautiful blogpost.
Barbra Backus
Pingback: Moderate Risk Chest Pain in the Emergency Department – MedTx
Pingback: Low Risk Chest Pain and High Sensitivity Troponin | Emergency Medicine Cases