Author: Brit Long, MD (@long_brit, EM Resident at SAUSHEC, USAF) // Edited by: Alex Koyfman, MD (@EMHighAK) & Justin Bright, MD (@JBright2021)
Case 1: A 73 year-old male presents with several weeks of cough, facial swelling, and shortness of breath. He has a history of lung cancer, actively being treated with radiation and chemotherapy. On exam, his vital signs are normal, but he has swelling of the face with a violaceous hue and elevated JVD.
Case 2: A 22 year-old female with a history of B cell lymphoma presents with nausea, vomiting, fatigue, decreased urine output, and palpitations. She has not been attending her normally scheduled cancer treatments. She is tachycardic in the 110s, and the rest of the exam is normal. Laboratory results reveal elevated phosphorus, potassium, and uric acid, with decreased calcium.
These two patients present with an emergency related to malignancy. How should you manage these patients, and what are your next steps?
With the aging population in the U.S., the incidence of malignancy is increasing. Many patients with cancer present to EDs, and some of these presentations are uniquely related to the respective malignancy. These oncologic emergencies can be broken into four categories: local physical effects, biochemical effects, hematologic effects, and therapy effects.
This post will provide a brief overview of the local physical and biochemical oncologic emergencies. Please stay tuned for hematologic and therapy oncologic emergencies in a future post!
Local Tumor Effects:
A) Superior vena cava (SVC) syndrome, B) Malignant pericardial effusion, C) Malignant spinal cord compression
A) SVC syndrome is due to obstruction of blood through the SVC, caused by internal vascular invasion or external compression. Malignancy such as lung cancer is most common (60%), whereas intravascular catheters account for 40% of presentations. External compression can be due to the right lung/mass, lymph nodes, or other mediastinal structures. Malignancy is the predominant cause, commonly non-small cell and small cell lung cancer, followed by lymphoma. Thrombosis of the SVC accounts for the majority of nonmalignant causes of SVC syndrome, usually a result of an indwelling intravascular device. Post-radiation fibrosis and fibrosing mediastinitis are other causes.1-4 The time of symptom onset depends on the rate of obstruction and venous collateral formation. Dyspnea is the most common symptom, with patients also complaining of face fullness/swelling. Cough, chest pain, and dysphagia are other symptoms. Unfortunately if rapid onset of symptoms occurs and no collateral flow is present, rapid onset of airway edema may present necessitating intubation. Facial edema and distension of neck and chest wall veins are commonly seen, though facial plethora and arm edema are rare. Usually symptoms are gradual over weeks with increase in venous pressure, and then improve with collateral vessel formation.1,2,5 Chest xray is abnormal in 84% of patients, often demonstrating widening of the mediastinum and pleural effusion. The optimal imaging is CT of the chest with contrast, which shows venous drainage, point of blockage, and identifies the cause of obstruction. Collateral vessel presence on CT has a specificity of 96% and sensitivity of 92%. MRV, US, and cavogram are other imaging options. Biopsies are often taken of the mass if cancer is found. Treatment involves symptom relief and disease management. If a malignancy is chemotherapy sensitive, systemic chemotherapy is warranted. A stent can be placed by interventional radiology for severe symptoms. Radiotherapy is done for non-small cell lung cancer following stent placement. If thrombus is present, systemic anticoagulation with heparin is needed. If airway edema is present, emergent stenting with radiation is necessary, with high-dose steroids. Though classically included in the treatment in boards review, diuretics are not supported in the literature. Unfortunately survival is around six months on average once the diagnosis is made. 1-6
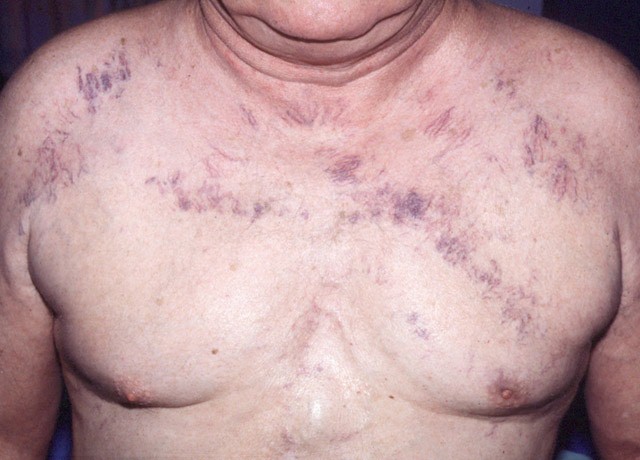
B) Malignant pericardial disease is present in up to one third of cancer patients and is most commonly due to metastases from lung or breast cancer. The majority of pericardial effusions (90%) are not malignancy-related. Most patients will present with exertional dyspnea (80%). A slow accumulation of fluid can allow up to 2L in the pericardial sac to collect with no change in hemodynamics. The acute accumulation of fluid causes decompensation. Ultrasound is the key to diagnosis and allows evaluation for tamponade (right atrial collapse in late diastole and right ventricular collapse in early diastole). Pericardiocentesis is often the necessary treatment, with ultrasound guidance preferred. Unfortunately up to 60% of patients will have recurrent pericardial effusions after drainage.1,7-9 Most patients have a poor prognosis following diagnosis, with median survival two to four months.1,10
C) Malignant spinal cord compression is a common cancer complication resulting from thecal sac compression, usually from local disease progression from vertebral body metastases from lung, kidney, or breast cancer, as well as multiple myeloma. There are three types of compression: intramedullary (metastasis in the dura mater), leptomeningeal (metastasis on top of the dura mater), and external compression (90% of cases). The thoracic spine has the most blood supply and greatest number of vertebrae, so it is most susceptible (60-70% of cases). Unfortunately it also possesses the least amount of space in the spinal canal. Prostate cancer will often metastasize to the lumbar region, breast to the thoracic, lung to the thoracic, and kidney to thoracic or lumbar. Median survival is six months. Back pain is the most common complaint found in 80-95% of patients, which often precedes other symptoms by two months.1 Half of patients will have bowel/bladder dysfunction at presentation, so obtaining a post-void residual or ultrasound can be helpful in the evaluation. The most important aspect is diagnosis, and the best prognostic factor, is pretreatment ambulation and neurologic status. MRI of the whole spine is needed for adequate visualization, as one third of patients will have multiple sites of metastasis and/or compression.1,11-15 Pain management is the first item of treatment, with opiate analgesics and glucocorticoids both supported by literature. If severe neurologic deficits such as paraparesis or paraplegia is present, then some recommend using high-dose steroids (dexamethasone 96mg IV), though risk of side effects is increased with greater steroid doses. With minimal symptoms, dexamethasone 10mg IV can be given. If no neurologic symptoms are present, no steroids are needed. As in common back pain, bedrest is not recommended. Definitive treatment involves surgery, external beam radiotherapy, or stereotactic body radiotherapy. If the spine is unstable, surgery is usually needed. Ultimately the course of treatment will be up to your spine surgeon and oncologic specialist.1,15-17
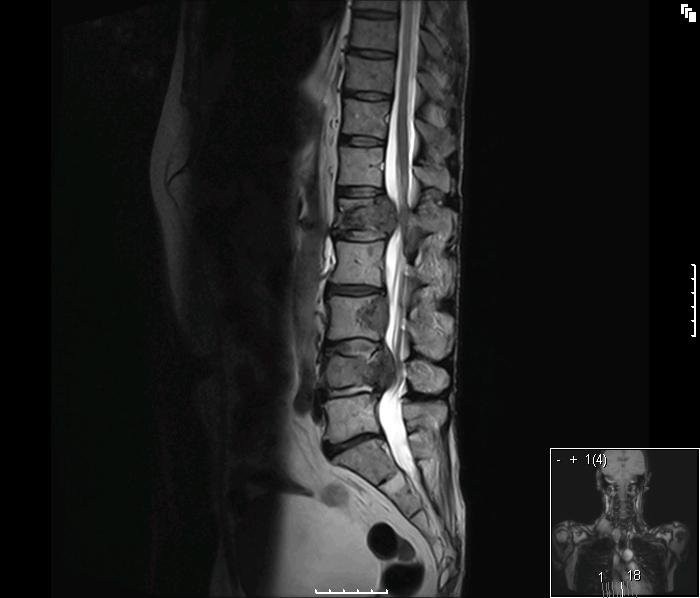
Biochemical Effects:
A) Hypercalcemia, B) Tumor lysis syndrome (TLS)
A) Hypercalcemia of malignancy occurs in 20 to 30% of cancers and is due to three different mechanisms: parathyroid-related protein (PTHrP) production seen in squamous cell carcinoma and lymphoma (80%), osteoclast activating factor seen in multiple myeloma or metastases causing osteolysis (20%), and endogenous calcitriol (1,25-dihydroxyvitamin D) production seen in lymphomas (<1%). Unfortunately hypercalcemia of malignancy is associated with poor prognosis. The most common cancers with bone involvement are breast and lung cancer and multiple myeloma. Patients will present with dehydration, polydipsia, fatigue, confusion, nausea/vomiting, constipation, decreased urine output, and ECG changes (bradycardia, prolonged PR, widened QRS, short QT).1,18,-21 Management includes obtaining an ionized calcium and electrolyte panel with ECG. Patients with mild hypercalcemia (<12mg/dL) with no symptoms do not need immediate treatment, but need adequate fluid intake. Mild symptoms with levels of 12-14mg/dL is often chronic, and treatment should be aimed at rehydration and finding the cause.
This post will focus on severe hypercalcemia, defined by levels > 14mg/dL with severe symptoms. Initial treatment is with crystalloids, crystalloids, and more crystalloids at 200-300ml/hr.1,18-21 Loop diuretics are not recommended in the absence of renal or heart failure because of potential complications.1,22 Calcitonin is the fastest acting medication, given at 4 international units/kg IM or subcutaneously, but unfortunately tachyphylaxis is common after the first dose. Bisphosphonates such as pamidronic acid (60-90mg IV over 2 hours) and zoledronic acid (4mg IV over 15 minutes) are the mainstays of therapy after adequate rehydration. Hydration and calcitonin will lower levels by 12 hours, with bisphosphonates working within 24 to 72 hours. These patients should be admitted. If neurologic deficits are found with a level of 18mg/dL or greater, then dialysis is warranted. Glucocorticoids are also commonly quoted as treatment, but this is only warranted if mechanism of hypercalcemia is due to calcitriol overproduction (lymphoma, sarcoidosis).1,18-22
B) TLS is due to massive tumor cell lysis with release of potassium, phosphorus, and uric acid into the body. TLS occurs after treatment initiation for high grade lymphomas and ALL, but any malignancy with aggressive therapy or high tumor burden can result in TLS. Treatment with radiation, chemotherapy, and/or steroids is the instigating factor. Patients often present with nausea/vomiting, diarrhea, anorexia, lethargy, low urine output, cramps, and dysrrhythmias.1,23-25 Low calcium is the most common electrolyte abnormality, usually due to release of phosphorus from dying cells binding free calcium. Hyperkalemia can result in arrhythmias, phosphorus elevation can cause calcium phosphate deposits in the kidneys, and high uric acid can lead to uric acid precipitation in the renal tubules, renal vasoconstriction, and acute kidney injury.1 Hyperuricemia is due to the breakdown of purine nucleic acids via xanthine oxidase. Uric acid is not very soluble in water, resulting in crystal formation. Phosphorus is produced in tumor cells at four times the amount of normal tissue cells. Secondary hypocalcemia results, and calcium phosphate deposits will develop when calcium times phosphate is greater than 60mg2/dL2.1,23-27
Two classifications exist via the Cairo-Bishop definition. The first is laboratory TLS (two or more laboratory abnormalities) and the second is clinical TLS (one laboratory abnormality plus increased creatinine, cardiac arrhythmia, or seizure).27 Patients at risk for TLS are followed closely by oncologists, who usually place them on allopurinol for prophylaxis. The most important aspect of this disease is avoiding it! Adequate hydration and allopurinol are essential in prevention. Allopurinol only prevents the formation of uric acid, but does not improve metabolism of the already present uric acid. For treatment of established TLS, there are several avenues to address. First is hydration. IV hydration is vital to maintain the glomerular filtration rate of the kidneys. These patients are often dehydrated, so several boluses of IV fluids (normal saline works well) are usually necessary to correct the dehydration. Next is electrolyte management, especially hyperkalemia (calcium for cardiac membrane stabilization, beta agonists and insulin/glucose for shift) and hyperphosphatemia (restrict intake and use phosphate binders such as calcium carbonate or sevelamer). Renal protection is the next step, which is assisted with your fluid boluses and electrolyte monitoring/management. Rasburicase is vital in this step, which oxidizes uric acid to allantoin. This metabolite is ten times more soluble than uric acid. Unfortunately this does not prevent renal failure or lower mortality! Rasburicase is dosed at 0.2mg/kg one time per day. Urinary alkalinization using sodium bicarbonate is controversial, with no data to support this, and this has been shown to increase formation of calcium phosphate crystals in the kidneys!1,23-30 These patients require admission, often to the ICU for monitoring.
Summary
- SVC syndrome occurs predominantly due to malignancy, with thrombosis and intravascular catheter obstruction distant causes (catheters as main cause quickly rising). Symptoms depend on rate of obstruction and collateral formation. CT chest with IV contrast is key to diagnosis. Treatment includes radiotherapy or stent placement.
- Malignant pericardial effusion most commonly presents with dyspnea. Acute accumulation of fluid causes decompensation. Ultrasound is key in diagnosis. Most patients require fluid loading and pericardiocentesis.
- Malignant spinal cord compression most commonly affects the thoracic spine, with back pain the most common complaint. MRI of the whole spine is needed for diagnosis, with steroids and surgery or radiation for treatment. Close to half of patients will have bowel/bladder dysfunction at presentation.
- Hypercalcemia of malignancy has three different mechanisms: PTHrP production, osteoclast activating factor, and calcitriol production. Breast cancer, lung cancer, and multiple myeloma are most common. Patients with severe symptoms and/or calcium >14mg/dL require treatment, predominantly with hydration, calcitonin, and bisphosphonates. Loop diuretics are controversial.
- TLS causes massive electrolyte changes, with increases in potassium, phosphorus, and uric acid. Treat with adequate hydration and rasburicase. Allopurinol is helpful in prevention. Urinary alkalinization with sodium bicarbonate does not have literature support.
- All of these are poor prognostic findings
- These require heme/onc consult when the patient is in the ED.
References/Further Reading:
-
- McCurdy MT, Shanholtz CB. Oncologic emergencies. Crit Care Med. 2012: 40(7); 2212-22.
- Wilson LD, Detterbeck FC, Yahalom J. Clinical practice. Superior vena cava syndrome with malignant causes. N Engl J Med 2007; 356:1862.
- Yellin A, Rosen A, Reichert N, Lieberman Y. Superior vena cava syndrome. The myth–the facts. Am Rev Respir Dis 1990; 141:1114.
- Rice TW, Rodriguez RM, Light RW. The superior vena cava syndrome: clinical characteristics and evolving etiology. Medicine (Baltimore) 2006; 85:37.
- Markman M. Diagnosis and management of superior vena cava syndrome. Cleve Clin J Med 1999; 66:59.
- Rowell NP, Gleeson FV. Steroids, radiotherapy, chemotherapy and stents for superior vena caval obstruction in carcinoma of the bronchus: a systematic review. Clin Oncol (R Coll Radiol) 2002; 14:338.
- Maisch B, Ristic A, Pankuweit S. Evaluation and management of pericardial effusion in patients with neoplastic disease. Prog Cardiovasc Dis 2010; 53:157.
- Klatt EC, Heitz DR. Cardiac metastases. Cancer 1990; 65:1456.
- Laham RJ, Cohen DJ, Kuntz RE, et al. Pericardial effusion in patients with cancer: outcome with contemporary management strategies. Heart 1996; 75:67.
- Tsang TS, Seward JB, Barnes ME, et al. Outcomes of primary and secondary treatment of pericardial effusion in patients with malignancy. Mayo Clin Proc 2000; 75:248.
- Loblaw DA, Laperriere NJ, Mackillop WJ. A population-based study of malignant spinal cord compression in Ontario. Clin Oncol (R Coll Radiol) 2003; 15:211.
- Mak KS, Lee LK, Mak RH, et al. Incidence and treatment patterns in hospitalizations for malignant spinal cord compression in the United States, 1998-2006. Int J Radiat Oncol Biol Phys 2011; 80:824.
- Bach F, Larsen BH, Rohde K, et al. Metastatic spinal cord compression. Occurrence, symptoms, clinical presentations and prognosis in 398 patients with spinal cord compression. Acta Neurochir (Wien) 1990; 107:37.
- Constans JP, de Divitiis E, Donzelli R, et al. Spinal metastases with neurological manifestations. Review of 600 cases. J Neurosurg 1983; 59:111.
- Cole JS, Patchell RA. Metastatic epidural spinal cord compression. Lancet Neurol 2008; 7:459.
- George R, Jeba J, Ramkumar G, et al. Interventions for the treatment of metastatic extradural spinal cord compression in adults. Cochrane Database Syst Rev 2008;CD006716.
- Loblaw DA, Mitera G, Ford M, Laperriere NJ. A 2011 updated systematic review and clinical practice guideline for the management of malignant extradural spinal cord compression. Int J Radiat Oncol Biol Phys 2012; 84:312.
- Stewart AF. Clinical practice. Hypercalcemia associated with cancer. N Engl J Med 2005; 352:373.
- Horwitz MJ, Stewart AF. Hypercalcemia associated with malignancy. In: Primer on the metabolic bone diseases and disorders of mineral metabolism, 6th ed, Favus MJ (Ed), American Society of Bone and Mineral Research, Washington, D.C. 2006. p.195.
- Bilezikian JP. Clinical review 51: Management of hypercalcemia. J Clin Endocrinol Metab 1993; 77:1445.
- Maier JD, Levine SN. Hypercalcemia in the Intensive Care Unit: A Review of Pathophysiology, Diagnosis, and Modern Therapy. J Intensive Care Med 2015; 30:235.
- LeGrand SB, Leskuski D, Zama I. Narrative review: furosemide for hypercalcemia: an unproven yet common practice. Ann Intern Med 2008; 149:259.
- Coiffier B, Altman A, Pui CH, et al. Guidelines for the management of pediatric and adult tumor lysis syndrome: an evidence-based review. J Clin Oncol 2008; 26:2767.
- Howard SC, Jones DP, Pui CH. The tumor lysis syndrome. N Engl J Med 2011; 364:1844.
- Montesinos P, Lorenzo I, Martin G, et al. Tumor lysis syndrome in patients with acute myeloid leukemia: identification of risk factors and development of a predictive model. Haematologica 2008; 93:67.
- Candrilli S, Bell T, Irish W, et al. A comparison of inpatient length of stay and costs among patients with hematologic malignancies (excluding Hodgkin disease) associated with and without acute renal failure. Clin Lymphoma Myeloma 2008; 8:44.
- Common Terminology Criteria for Adverse Events, version 4.0, June 2010, National Institutes of Health, National Cancer Institute http://evs.nci.nih.gov/ftp1/CTCAE/CTCAE_4.03_2010-06-14_QuickReference_5x7.pdf (Accessed on May 03, 2011).
- Cairo MS, Bishop M. Tumour lysis syndrome: new therapeutic strategies and classification. Br J Haematol 2004; 127:3.
- Goldman SC, Holcenberg JS, Finklestein JZ, et al. A randomized comparison between rasburicase and allopurinol in children with lymphoma or leukemia at high risk for tumor lysis. Blood 2001; 97:2998.
- Lopez-Olivo MA, Pratt G, Palla SL, Salahudeen A. Rasburicase in tumor lysis syndrome of the adult: a systematic review and meta-analysis. Am J Kidney Dis 2013; 62:481.
- http://www.ncbi.nlm.nih.gov/pubmed/22463972
- http://www.ncbi.nlm.nih.gov/pubmed/21277135
- http://www.ncbi.nlm.nih.gov/pubmed/25060247
- http://www.ncbi.nlm.nih.gov/pubmed/23246111
- http://www.ncbi.nlm.nih.gov/pubmed/25060250
- http://www.ncbi.nlm.nih.gov/pubmed/25098804





3 thoughts on “Oncologic Emergencies Part I: Pearls and Pitfalls”
Pingback: An Urgent Care Approach to Malignancy Complications - Journal of Urgent Care Medicine
Pingback: emDOCs.net – Emergency Medicine EducationMultiple Myeloma Emergencies - emDOCs.net - Emergency Medicine Education
Pingback: Oncologic Emergencies – Emergency Medicine Ireland