Welcome back to Small Talk. Every first Wednesday of the month we will release high yield PEM content written by PEM talent from around the country. We hope you enjoy these reviews. Comments, questions, accolades or concerns: feel free to reach out to Joe Ravera, MD (pemgemspod@gmail.com).

Authors: Joe Ravera, MD (@pemuvm1, Director of Pediatric Emergency Medicine, Assistant Professor of Surgery, Division of Emergency Medicine, University of Vermont Medical Center) and Skyler Lentz, MD (@skylerlentz, Assistant Professor in the Departments of Surgery and Medicine, Divisions of Emergency Medicine and Pulmonary & Critical Care, University of Vermont Medical Center) // Reviewed by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Background
A critically ill child, particularly one requiring endotracheal intubation and mechanical ventilation, quickly raises the anxiety in the ED. For starters, there can be confusion about the appropriately sized equipment. Although there is some concern about accuracy of weight for medication dosing, a length-based resuscitation tape (such as a Broselow™ tape) can provide a quick estimation of appropriately sized equipment (1). There are also numerous apps that can assist with determining appropriate equipment and medication doses. If unavailable, the mnemonic “Miller 2 at age 2” should be helpful as a ballpark for DL blade size, and the formula (Age/4) + 3.5 = cuffed endotracheal tube size can be a quick estimate of the appropriately sized ET tube. It should be noted that cuffed ET tubes are now preferred in all ages whenever available.
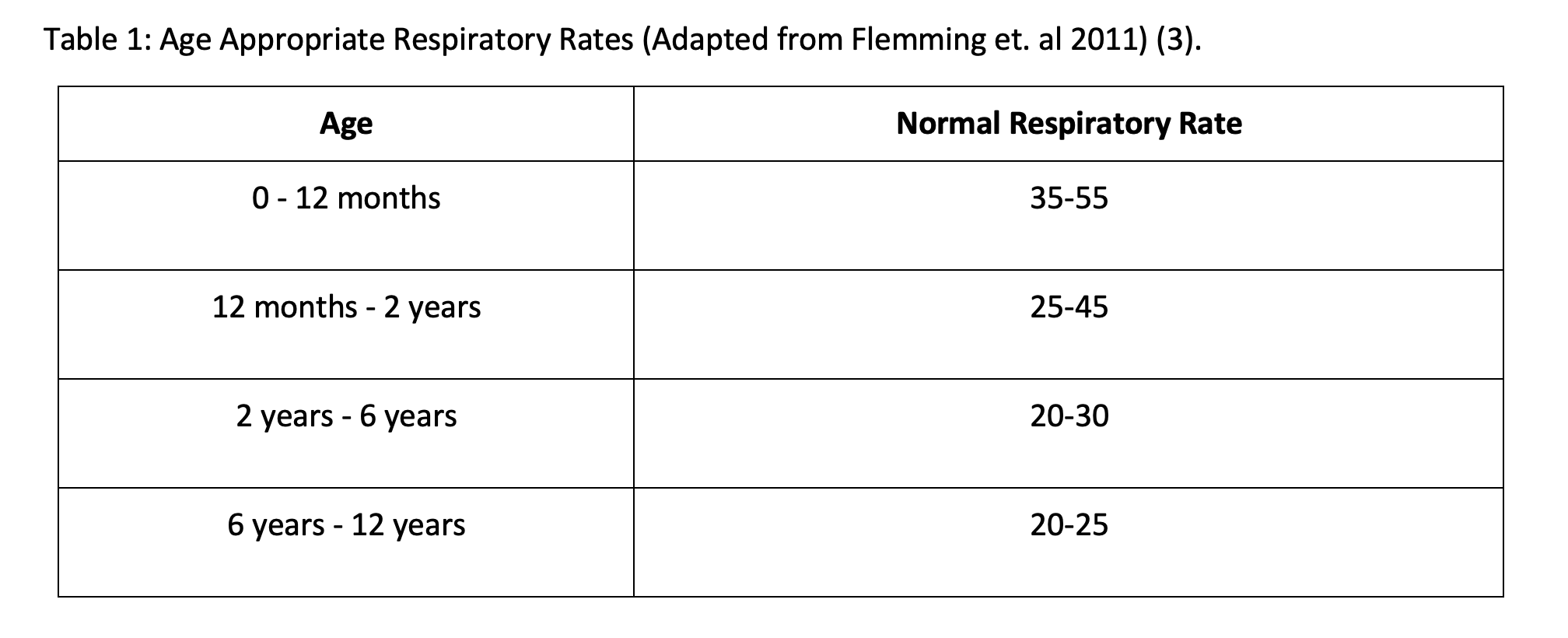
There is often a moment of relief after an endotracheal tube is successfully placed and a feeling of the hard part being over. However, selecting appropriate mechanical ventilation settings is arguably more important than placing the tube. Pediatric patients, similar to adults, can be intubated for pulmonary pathology (pneumonia, bronchiolitis, asthma, etc.) or non-pulmonary, typically CNS pathology, (seizures, trauma, etc.). Fortunately, the starting weight-based tidal volume settings, ventilator modes, ventilator strategies in challenging cases, and PEEP settings are similar in children and adults. As a general rule, children intubated for non-pulmonary indications are not challenging to ventilate, and a simple strategy of a volume control mode at a tidal volume (Vt) of 8 cc/kg of ideal body weight, an age-appropriate respiratory rate (Table 1), and a PEEP of 5 cmH2O will suffice for almost all patients (2). Please note the child intubated for severe metabolic acidosis will need much higher respiratory rates in order to compensate.
Infectious Pulmonary Pathology in Children
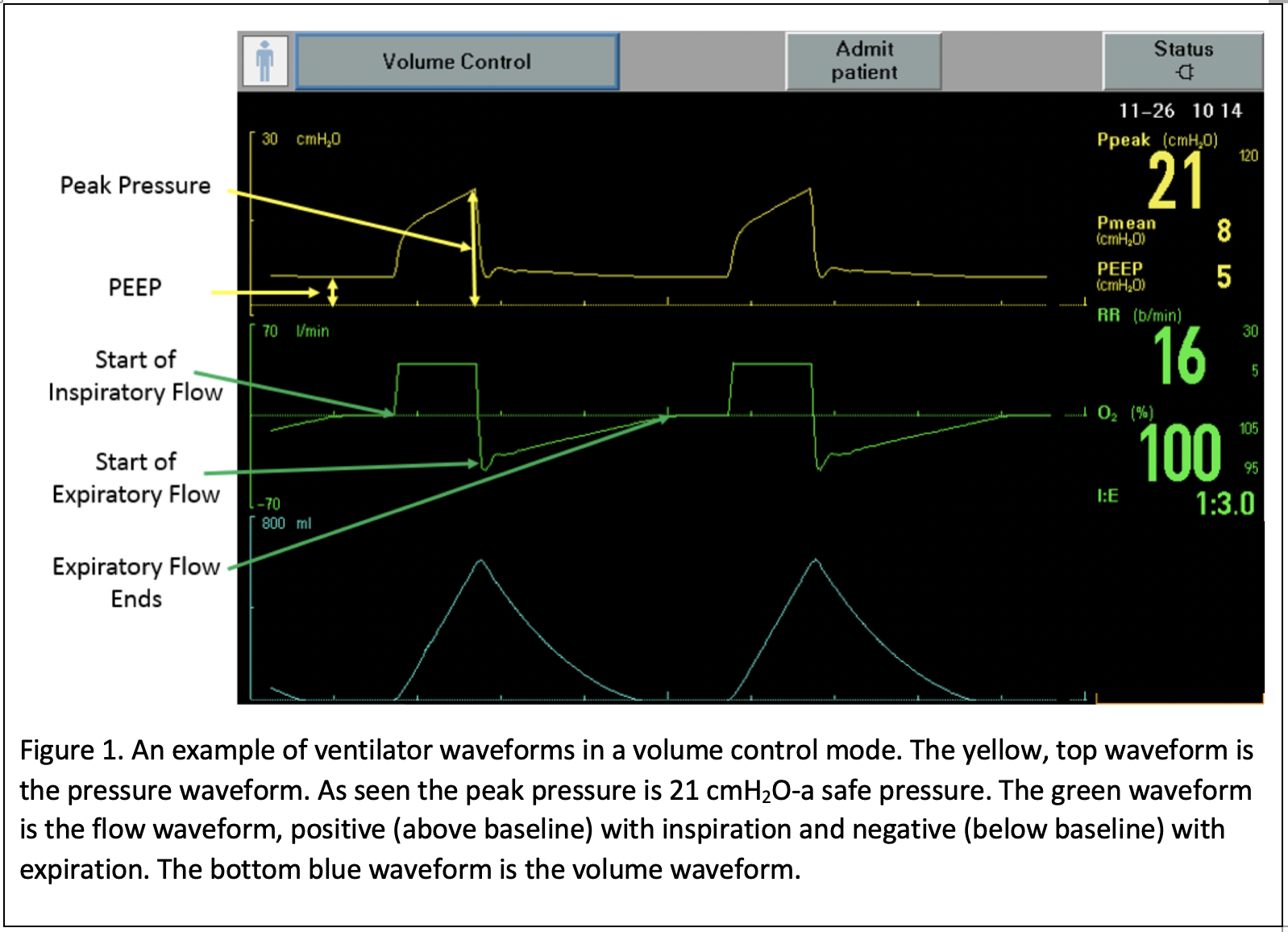
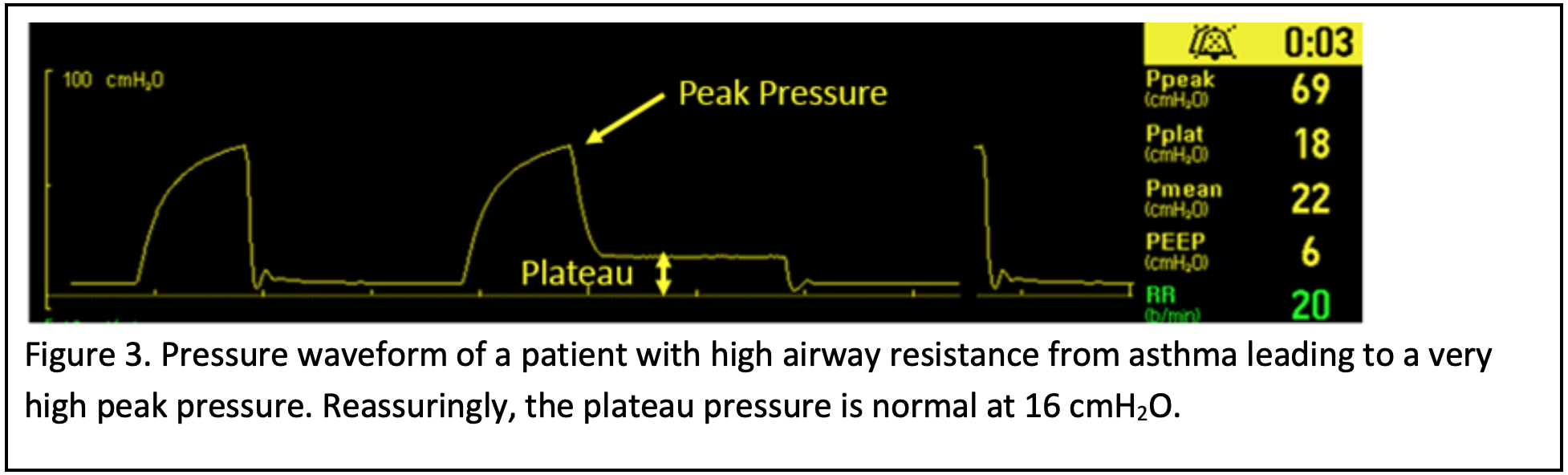
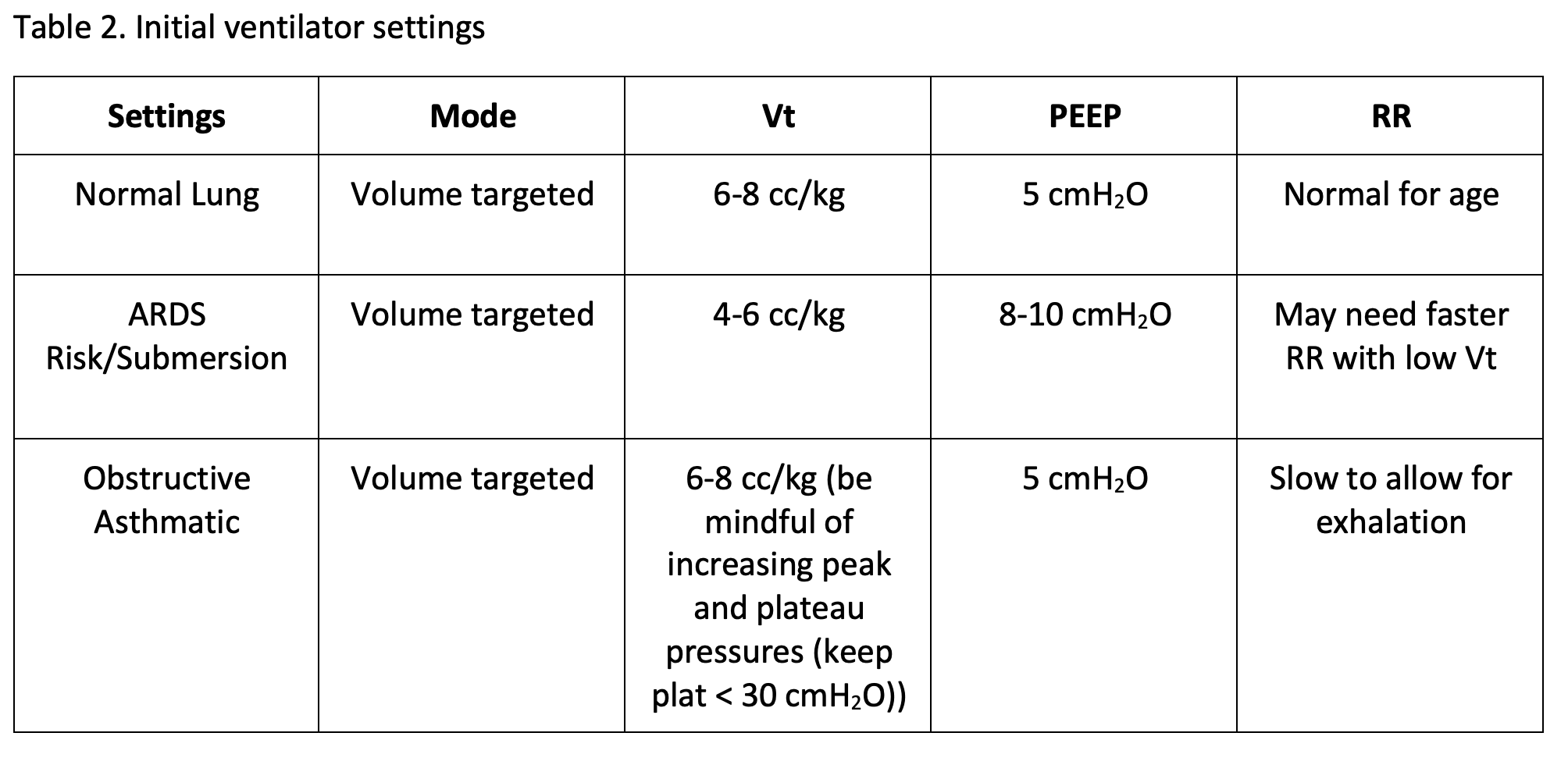
Infectious pulmonary pathology is a common indication for intubation in children. Infectious etiologies such as bacterial pneumonia and viral bronchiolitis are the most common indications. It is important to understand that these children are at risk for subsequent acute respiratory distress syndrome (ARDS) and ventilator associated lung injury. If there are already signs of ARDS with diffuse interstitial infiltrates on a chest x-ray and moderate to severe hypoxia, a lung protective strategy should be considered. Lung protective strategy in children consists of a volume mode with a Vt of 4-6 cc/kg and a PEEP of 8-10 cmH2O to start (6). PEEP improves oxygenation by recruitment and maintaining lung aeration (4). Target a peak pressure of < 30-35 cmH2O (see figure 1) and/or a plateau pressure < 28 cmH2O (2). Peak pressure is the sum of airway resistance, plateau pressure and PEEP (both applied and auto-PEEP), compared to plateau pressure, a measure of lung compliance. High peak pressures with a normal plateau pressure is indicative of high airway resistance and can be due to several causes: bronchospasm (e.g. asthma, anaphylaxis etc.), kinked tube, small diameter tube, or ventilator circuit obstruction. Plateau pressure elevation can be seen with pneumothorax, ARDS (or other restrictive lung disease), overdistension by excessive Vt, right mainstem intubation, pneumonia, pulmonary edema, and auto-PEEP (5). A high peak pressure with significant difference between the peak and plateau pressures (>5 cmH2O) typically means acute elevation in airway resistance (see figure 3); however, if the difference is low (< 5 cmH2O), decreased lung compliance is likely the etiology. If the peak pressure is > 35 cmH20, decrease the Vt by 1 cc/kg to as low as 3-4 cc/kg until the peak pressure is < 35 cmH2O and/or plateau pressure is < 28 cmH2O (6). As the Vt is decreased, the respiratory rate may need to be increased to maintain a normal minute ventilation. It is important to remember that hypercapnia can be tolerated as long as the pH remains above 7.20 (2). An important caveat is in patients with pulmonary hypertension and head injury, normocapnia (pCO235-45 mmHg) should be targeted (2).
Obstructive Pulmonary Pathology in Children
Patients with obstructive pulmonary pathology, asthma in particular, are some of the most challenging and high-risk patients on mechanical ventilation. Often the best care for an asthmatic is to avoid endotracheal intubation and mechanical ventilation if at all possible. Maximal therapy including inhaled bronchodilators, parenteral steroids, magnesium, and even IV/IM beta agonists such as epinephrine or terbutaline should be given in an effort to avoid intubation. In addition, non-invasive mechanical ventilation such as high flow nasal cannula or bi-level non-invasive ventilation (BiPAP™) can be used as a bridge therapy to give medical therapy time to work. Despite maximal therapy, there is a subset of asthmatics that will require mechanical ventilation (7).
The main challenge in these patients is not only are they at risk for ventilator associated lung injury, but due to airway inflammation and bronchoconstriction, they are at high risk for a ventilator associated pneumothorax, breath stacking, and auto-PEEP (a condition where they are not able to completely exhale each breath) (see figure 2). In addition to tidal volumes of 6-8 cc/kg, careful attention must be paid to the respiratory rate (8). One strategy is to observe the flow volume curve on the ventilator to gauge how long it takes the child to exhale one breath (figure 2). Another strategy is to give the child one breath via bag mask through the endotracheal tube and count the seconds it takes for the child to completely exhale. Many need a respiratory rate as low as 10-14/min; the sickest may require even lower.

The first 15 minutes after an asthmatic is intubated are critical, and the physician must pay careful attention to both the patient and the ventilator. These patients typically exhibit a high degree on patient ventilator dyssynchrony due to the stimulating respiratory acidosis. If the asthmatic has a high spontaneous respiratory rate that is difficult to manage, they may require deep sedation and paralysis. If paralyzed, be sure to continue adequate sedation. Furthermore, patients with airway obstruction (i.e. asthma) have very high airway resistance leading to increased peak inspiratory pressures (see figure 3). An elevated peak pressure without a rise in plateau pressure is not generally harmful, as these elevated peak pressures are not transmitted to the alveoli (4). However, a high peak pressure should alert the physician to obtain a plateau pressure, obtained by an end-inspiratory hold in a passive patient. The plateau pressure estimates alveolar pressure, and when severely elevated can lead to barotrauma, pneumothorax and diminished venous return to the heart (9). An elevated plateau pressure in this setting is most likely indicative of auto-PEEP, to directly measure auto-PEEP an end expiratory hold in a passive patient is performed (see figure 2) (8). In obstructive lung disease, the plateau pressure should be kept ≤ 30 cmH2O (2). If the plateau pressure is elevated > 30 cmH2O aggressive efforts should be taken to treat bronchoconstriction and increase the expiratory time such as further decreases in the respiratory rate.
Avoid the urge to increase the respiratory rate to blow down the CO2 – this will lead to breath-stacking. These patients typically tolerate hypercapnia and a pH ≥ 7.20. The pH may take several hours or even days to normalize in the PICU.
Submersion Injury in Children
Submersion injury often involves delayed pulmonary injury 6-12 hours from the initial resuscitation. These patients are at high risk for developing ARDS and should treated with a lung protective strategy (10). In children this consists of a volume targeted mode (i.e. volume control) and a tidal volume of 6 cc/kg, starting with a PEEP of 8 cmH20 and up titrating if oxygenation remains an issue. If the peak pressure is > 35 cmH2O the Vt may need to be as low as 4-5 cc/kg and PEEP as high as 10 cmH2O if oxygenation is an issue from the start. Another common problem in submersion injuries is a large volume of water swallowed in the stomach. Gastric distention is an impediment to ventilation in all pediatric patients. An NG or OG tube placed immediately after intubation and decompression of the stomach is critical to facilitate mechanical ventilation, not only in patients with submersion injury, but almost all pediatric patients.
Prolonged Ventilator Management in the Emergency Department
In many settings a critically ill child may need to be transferred to a tertiary receiving facility. This requires prolonged post intubation care in the ED. Post intubation sedation is critical and must be tailored to the clinical scenario and timing to definitive care. In certain instances IV, pushes of ketamine (1-2 mg/kg) or fentanyl (1 mcg/kg) and midazolam (0.1 mg/kg) may be appropriate as temporizing sedation. If there is prolonged transport, a continuous infusion of ketamine, propofol, fentanyl and versed, or dexmedetomidine are all reasonable choices. These authors would advise that community providers use whatever they are comfortable with and is readily available at their facility. It should be noted that propofol and a benzodiazepine/opiate combination have higher risk for hypotension and should be avoided in certain clinical settings (e.g. severe trauma and hemorrhage). Discussion with the pediatric intensivist can be extremely helpful in choosing appropriate sedation.
It is important to follow certain parameters in the first hour after placing a pediatric patient on the ventilator. The pulse oximetry should be followed closely and oxygen should be rapidly titrated down to avoid oxygen toxicity (caution in pediatric head trauma where hypoxia can significantly worsen outcomes). A reasonable target for non-head injury patients, per PARDS protocol, is 92%-97% for patients requiring a PEEP <10 cmH2O (2). A VBG/ABG should be obtained within an hour and correlated with end-tidal CO2to evaluate the patient’s ventilation status. When using a volume targeted mode, the peak pressures should be monitored and ideally be under 30-35 cmH2O and/or plateau pressure < 28 cmH2O. In the asthmatic, keep the plateau pressure < 30 cmH2O. As with sedation, early communication with your pediatric intensivist is extremely helpful in ventilator management.
Case Continued
After successful intubation, the patient was placed on volume control at a rate of 24, a PEEP of 10 cmH2O, and a tidal volume of 100 cc (5 cc/kg). During the hour waiting for the transport team, his oxygen saturation rose to 100%, and FiO2was weaned from 1.0 to 0.6. He was admitted to the pediatric intensive care unit and was extubated 3 days later neurologically intact.
Pearls and Pitfalls:
–Early communication with the accepting pediatric intensivist is extremely helpful in critical pediatric resuscitation and mechanical ventilation.
-When intubating for non-pulmonary pathology indications, it is unlikely that there will be difficulty with ventilation. Remember to set appropriate respiratory rate for age and tidal volume for size. Children with a severe metabolic acidosis, such as DKA, may need an increased respiratory rate with a goal to maintain pre-intubation minute ventilation.
–Lung protective strategy of 4-6 cc/kg should be considered in patients who have signs of or are at risk for ARDS.
-Asthmatics are high risk for immediate complications from the ventilator. Pay careful attention to the respiratory rate and peak and plateau pressures. Very low respiratory rates may be needed. Tolerate hypercapnia; a pH >7.20 is safe.
–NG/OG placement after intubation for gastric decompression particularly in submersion injury patients is recommended.
-For post intubation sedation, the clinical scenario and time of transport to definitive care are factors to consider when choosing a specific agent and bolus versus infusion.
–Follow CBG or VBG as well as ETCO2, pulse oximetry, and peak airway pressures to assess the adequacy and potential complications of mechanical ventilation.
References / Further Reading
- Wells et al. The accuracy of the Broselow tape as a weight estimation tool and a drug-dosing guide – A systematic review and meta-analysis. Resuscitation. 2017 Dec;121:9-33.
- Kneyber et.al. Recommendations for mechanical ventilation of critically ill children from the Paediatric Mechanical Ventilation Consensus Conference (PEMVECC). Intensive Care Med. 2017 Dec;43(12):1764-178.
- Flemming et al. Normal ranges of heart rate and respiratory rate in children from birth to 18 years of age: a systematic review of observational studies. Lancet. 2011 Mar 19;377(9770):1011-8.
- Tobin, Martin. Advances in Mechanical Ventilation. N Engl J Med 2001; 344: 1986-1996.
- Wood, S and Winters, M. Care of the intubated emergency patient. Journ Emerg Med 2011; 40(4):419-427.
- The Pediatric Acute Lung Injury Consensus Conference Group. Pediatric Acute Respiratory Distress Syndrome: Consensus Recommendations from the Pediatric Acute Lung Injury Consensus Conference. Pediatr Crit Care Med 2015; XX:00–00.
- Pardue Jones al. Pediatric acute asthma exacerbations: Evaluation and management from emergency department to intensive care unit. J Asthma. 2016 Aug;53(6):607-17.
- Mechanical ventilation for severe asthma. Chest. 2015 Jun;147(6):1671-1680.
- Tobin, Martin. Mechanical Ventilation. N Engl J Med 1994; 330:1056-1061.
- Semple-Hess, Campwala. Pediatric submersion injuries: emergency care and resuscitation. Pediatr Emerg Med Pract. 2014 Jun;11(6):1-21.








