Pelvic fractures: ED presentations and management
- May 29th, 2017
- Katie Lupez
- categories:
Authors: Katie Lupez, MD (@KatieLupez, EM Resident Physician, Carolinas Medical Center) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital) and Brit Long, MD (@long_brit, EM Attending Physician, SAUSHEC)
Case
A 50-year-old male presents to the ED via EMS after being a restrained driver in a head on high speed MVC. He is currently hemodynamically unstable with a BP of 87/45 and HR of 130. On primary survey, airway is intact, breath sounds are equal bilaterally, there is no obvious external hemorrhage, and his GCS is 15. Secondary survey is notable for a soft and non-tender abdomen, no extremity deformities, and no shortening or rotation noted on bilateral lower extremity exam. However, pain is elicited and instability is noted on gentle downward and medial compression of the pelvis over the iliac wings.
Pelvic Fractures
- The bony pelvis is composed of the ilium, ischium, pubis, sacrum, and coccyx bones held together by strong ligamentous connections.
- When the pelvis is disrupted, it implies a high mechanism of energy transfer and can lead to high morbidity and mortality. Overall, there is 10% mortality for pelvic fractures and up to 50% mortality for pelvic fractures in the unstable patient.1
- Pelvic fractures can be classified in three different ways: acetabular fractures, single bone fractures, and pelvic ring fractures.

Acetabulum fractures
- Anatomy: The acetabulum is where the ilium, ischium, and pubis fuse and is divided into anterior and posterior columns.
- The anterior column consists of the anterior iliac wing, superior pubic ramus, and anterior wall of the acetabulum.
- The posterior column consists of the ischium, ischial tuberosity, and posterior wall of the acetabulum.

- Anatomical Classification:
- Posterior wall of the acetabulum
- The posterior wall is the most common location for acetabular fractures to occur.
- The most common cause of a posterior wall fracture is an MVC in which hitting the knee against the dashboard causes a posteriorly directed force vector through the femur impacting the posterior acetabulum.
- Posterior wall acetabular fractures can be associated with posterior dislocation of the hip.
- Be aware of this on your physical exam and look for shortening, flexion, and internal rotation of the affected lower extremity.
- Be cautious and note any evidence of dislocation when reviewing your radiographic images.
- Reduction of dislocation, if present, must occur within 6 hours of injury.
- Epidemiology: There is a bimodal distribution of acetabular fractures affecting both the young and elderly most frequently.1
- In the young, the mechanism is typically major blunt trauma.
- In the elderly, the mechanism is often simply a minor blunt trauma given their baseline boney fragility.
- Treatment: Definitive treatment of acetabular fractures most commonly requires surgical open reduction and internal fixation given the joint instability this injury causes. Yet, there are some special considerations in which your orthopedic colleagues may opt for non-operative measures and may solely recommend weight-bearing restrictions.
- Posterior wall of the acetabulum
Single bone fractures
- Anatomy: Single bone fractures of the pelvis are the most frequently encountered pelvic fractures in the emergency department and can involve any part of the boney pelvis including the sacrum, coccyx, pubis, ischium, or ilium.
- Anatomical Classification:
- Pubic Rami Fracture
- Account for greater than 50% of pelvis fractures.
- Usually simple breaks in the pelvic rim or avulsion fractures.
- Sacral fractures are classified by the Denis classification
- Zones 1, 2, and 3 fractures are characterized by being lateral to, through, or medial to the foramina respectively.
- There is a higher incidence of nerve injury the closer the sacral fracture is to the foramina given the nerve roots’ anatomical exit through the sacral foramina.
- Make sure to do a detailed neurologic exam in patients with concerns for sacral fractures.
- Sacral stress fractures are rare but can occur with repetitive injury to the area or due to insufficiency in the elderly osteoporotic population.
- Coccygeal fractures
- Usual are transverse fractures with the inferior segment pushed inward.
- Ilium fractures
- The anterior and posterior iliac spine prominences (ASIS, AIIS, PSIS, PIIS) are origins for large muscle groups and often can suffer avulsion fractions from forceful contractions of theses muscle groups.
- Fracture of the iliac wing is also known as the Duverney fracture.4
- It is a stable fracture and often heals well given the stability from the surrounding musculature.
- Given the force necessary to disrupt the iliac wing the internal iliac vasculature can sometimes be disrupted.
- Epidemiology: Single bone fractures occur in a bimodal in distribution.
- Commonly caused by high mechanism blunt trauma in the young.
- More commonly occurring in low energy falls in the elderly.
- Treatment: Most single bone fractures are treated non-operatively but will need orthopedic follow up.
- Despite non-operative management, single bone fractures can still lead to significant morbidity for patients given intensity of pain and decreased mobility.
- These fractures can often lead to long term nursing assistance needs for the elderly.
- Pubic Rami Fracture

Pelvic ring fractures
- Anatomy:
- Pelvic ring fractures are the most severe fracture type with two breaks in the circular pelvic ring, often leading to an unstable pelvis that can easily result in an unstable patient.
- Pelvic ring fractures have the highest rate of major hemorrhage given the proximity of these fractures to prominent arteries and veins and the severity of the mechanism necessary for them to occur.
- Pelvic ring fractures often involve damage to the posterior sacroiliac ligament, which is the strongest ligamentous connection in the body. Therefore, if disrupted, have high suspicion for other high mechanism injuries.
- Mechanistic Classification: The Young-Burgess Classification system defines three types of pelvic ring fractures based on the mechanism of injury and force vector pattern.
-
Lateral compression fracture:
- This occurs when a lateral force vector causes an anterior ring disruption and sacral fracture as depicted below.
- This is the most common of the pelvic ring fractures.
- Most commonly occurring after a “t-bone” MVC.
-

-
Anterior Posterior (AP) compression fracture:
- This occurs when a midline force vector causes disruption at the pubic symphysis anteriorly and disruption of the sacral ligaments posteriorly as depicted below.
- The majority of these fractures are what is commonly referred to as an “open book pelvic fracture” given the opening of the pubic symphysis anteriorly.
- Diastasis (widening of the pubic symphysis) greater than 1 cm can represent instability with diastasis greater than 2.5 cm representing posterior sacral ligamentous damage.7
- Special consideration: Female patients who have had children may have a diastasis of 1 cm at baseline.8
- In one study, pelvic diastasis of 5cm resulted in a 20% increase in pelvic volume, with a high association of venous injury.9
- Increasing the pelvic volumes can lead to a greater area for blood to accumulate.
- Diastasis (widening of the pubic symphysis) greater than 1 cm can represent instability with diastasis greater than 2.5 cm representing posterior sacral ligamentous damage.7

-
Vertical shear fracture:
- This occurs when a vertical force vector causes an anterior ring fracture and disruption of the posterior sacral ligaments as depicted below.
- This most commonly occurs in an MVC in which the force vector runs through the gas pedal through the femur up to through the pelvis displacing it as depicted below.

- Straddle Fractures can be caused by AP compression or Vertical shear force vectors.7
- Fracture occurs at the bilateral inferior and superior pubic rami and can also involve the posterior ligaments.
- Associated with 40% chance of GU injury.
- 33% of patients require laparotomy for intraperitoneal injuries.

- Epidemiology: Pelvic ring fractures are often caused by major blunt trauma and can occur in all age groups with high velocity MVCs being the most common mechanism.11
- Treatment: Definitive treatment for these severe fractures often requires multiple orthopedic operations.
Radiographic Considerations
- Standard AP pelvis
- Most commonly utilized as part of trauma evaluation (ATLS).
- Anterior ring fractures are most often identified with this view yet it may be difficult to visualize posterior structures.
- Inlet and outlet views
- Ideal for further visualization of the individual hemipelvis and sacrum.
- Judet views (oblique views)
- Should be performed for acetabular fractures.
- CT Pelvis
- Helps further characterize pelvic fractures particularly with better identification of posterior portion of the pelvic ring.7
- MRI of the Pelvis may eventually be used by the orthopedic surgery team yet will not be something ED providers are expected to order from the ED.
- What about in the trauma patient?
- If your patient is hemodynamically stable with clinically stable pelvis and negative fast, a plain film of the pelvis in ED can be omitted if plan is to proceed to pelvic CT.12
Emergency Department Management
-
Resuscitate the patient
- Patients with pelvic fractures are at risk of massive hemorrhage given possible disruption of pelvic vasculature.
- Implement damage control resuscitation.13
- Give blood products in a 1:1:1 ratio of pRBCs, plasma, and platelets.
- Permissive hypotension to limit amount of blood exsanguinated.
- Check out more FOAMed for further information on the damage control resuscitation:
- http://rebelem.com/proppr-randomized-clinical-trial/#ITEM-3085-0
- If your patient is unstable and you are giving blood => give TXA.
- TXA prevents clot breakdown and can reduce bleeding.
- Load with 1g IV bolus.
- http://www.emdocs.net/ed-crash-course-txa-matters/
- Avoid resuscitation through lower limb sites as it may drain into retroperitoneal space.
-
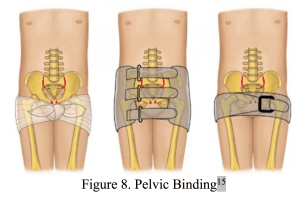
If a pelvic ring fracture => bind the pelvis
- Binding the pelvis has been shown to decrease the available space in the pelvis for hemorrhage to accumulate and ideally helps creates a faster tamponade effect to stop any active vascular bleeds.
- Although the evidence is controversial, binding has been proven to increase MAP pressures in the short term until patient’s reach definitive management of their injuries.14
- Binding can be performed with commercial products or simply with a bed sheet as shown below.
- Common pitfalls in binding the pelvis is placing the binder too high with no true closure of the pelvic ring.
- Make sure your device of choice lays over the bilateral greater trochanters with proper amount of pressure to close the pelvic ring.
- Additionally, binding the pelvis has been theorized to help keep all the sharp boney fragments from moving and causing more damage in and out of transport.
- Special consideration should be had for vertical shear pelvic ring fractures where the effected side of the pelvis may be displaced anteriorly and the lower extremity should be reduced inferiorly before closure of the pelvic can be performed with a binder.
-
Consider resuscitative endovascular balloon occlusion of the aorta (REBOA)
- Endovascular occlusion of the distal aorta (Zone 3) has been shown to assist in control of hemorrhage until definitive management can be obtain.
- The above statement is based on preliminary evidence and more clinical trials are currently underway.
- Check out more FOAMed for further information on the REBOA for severe hemorrhage from pelvic fractures:
- Endovascular occlusion of the distal aorta (Zone 3) has been shown to assist in control of hemorrhage until definitive management can be obtain.
-
Rule out other sources of hemorrhage (especially intraperitoneal bleeding)
- If intraperitoneal bleeding is identified in an unstable patient => they should be taken to the OR immediately.
- While addressing the intraperitoneal injuries, the surgeons can pack the retroperitoneum to tamponade any bleeding from the pelvic vasculature caused by the pelvic fracture.
- If intraperitoneal bleeding is identified in an unstable patient => they should be taken to the OR immediately.
-
Do a FAST exam
- The FAST is highly specific for intraperitoneal bleeding but has low sensitivity, particularly in pelvic fractures.16
- In an unstable pelvic fracture patient that is also hemodynamically unstable:17
- If FAST is positive => Patient goes to OR for exploratory laparotomy.
- If FAST is negative or indeterminate => consider diagnostic peritoneal tap/lavage to assess for intraperitoneal bleeding.
- If DPT positive => proceed to OR.
- If DPT negative => proceed to pelvic angiography and embolization.
-
Pelvic embolization
- Hemodynamic instability associated with a pelvic fracture without any other source of bleeding is an indication for pelvic angiography and subsequent embolization.
- The interventional radiologist will observe for contrast extravasation from damaged vessels and intentionally occlude the damaged vessels in order to control hemorrhage.18
- It is important to note that pelvic embolization solely occludes arterial hemorrhage and continual blood loss from the venous system can still occur.
-
Do not miss associated injuries
- Pelvic ring fractures are most commonly associated with chest trauma > head trauma > intraperitoneal trauma > long bone injuries.19
- Make sure to do a complete trauma assessment because the force created to cause pelvic fractures is usually indicative of other serious pathology.
- GU Injuries
- Physical exam: evaluate for blood at the urethral meatus, high riding prostate, scrotal ecchymosis, inability of patient to void, and a thorough vaginal and rectal exam.
- Hematuria is the most important sign of GU trauma.
- Vaginal and rectal injuries can occur with the sharp fragments of the fracture.
- Urethral injuries are common in anteriorly disrupted pelvic fractures.
- Perform a bedside retrograde urethrogram (RUG) for further evaluation of urethral injury.
- For more information on how to perform the RUG:
- Bladder rupture occurs in 5-10% of patient’s suffering from pelvic fractures.
- Perform a bedside cystogram for further evaluation of bladder injury.
- For more information on how to perform a cystogram:
- Intraperitoneal bladder injury often requires operative fixation.
- Extraperitoneal bladder injury can often be managed non-operatively with a suprapubic catheter.
- Neurologic injuries
- There is a high incidence of sacral nerve injury associated with acetabular fractures.20
- The L5 nerve root runs over the sacral ala and can be damaged in pelvic ring fractures’ posterior disruption.
- Ensure a good distal extremity neurologic exam.
- Pelvic ring fractures are most commonly associated with chest trauma > head trauma > intraperitoneal trauma > long bone injuries.19
-
Treat the pain
- Any fracture involving the pelvis inflicts a lot of pain on our patient’s and we must be cognizant of treating their pain appropriately and in a timely fashion.
-
Stabilize as above and transfer those who will need operative fixation to the appropriate center
Case Resolution
Given your exam, you call for x-ray to come to the trauma bay. The patient’s chest x-ray is within normal limits and his pelvic x-ray is shown below. You place the patient in a pelvic binder.
Simultaneously, you resuscitate the patient with 1:1:1 blood products and ask for TXA to be given. You consider performing a REBOA. You perform a FAST exam, which is negative. The patient is persistently hemodynamically unstable, and you perform a DPT at the bedside (given your knowledge of the low sensitivity of the FAST exam for intraperitoneal injuries particularly in the setting of severe pelvic fractures). The DPT is negative. You call for pelvic embolization to be performed as soon as possible. Active contrast extravasation was identified from the internal iliac and was subsequently embolized. On return of the patient to the ED, you continue to resuscitate your patient and examine him for associated injuries.

This post is sponsored by www.ERdocFinder.com, a supporter of FOAM and medical education, who with their sponsorship are making FOAM material more accessible to ER physicians around the world.

References / Further Reading:
- Orthopaedic Review – Orthobullets.com. Available at: http://www.orthobullets.com/.
- Pelvis Anatomy, Artifacts and Variants – wikiRadiography. Available at: http://www.wikiradiography.net/page/Pelvis+Anatomy%2C+Artifacts+and+Variants.
- Mosby’s Medical Dictionary. 8th Ed. 2009. Available at: http://medical-dictionary.thefreedictionary.com/acetabulum.
- Iliac wing fractures – OrthopaedicsOne Articles – OrthopaedicsOne. Available at: http://www.orthopaedicsone.com/display/Main/Iliac+wing+fractures.
- Cwinn SBC, Adam A. Pelvic Trauma | Clinical Gate. Available at: https://clinicalgate.com/pelvic-trauma/.
- Tibbles CD, Gibbs M. Pelvic Fractures | Anesthesia Key. Available at: https://aneskey.com/pelvic-fractures-3/.
- Khurana B, Sheehan SE, Sodickson AD, Weaver MJ. Pelvic Ring Fractures: What the Orthopedic Surgeon Wants to Know. RadioGraphics. 2014;34(5):1317-1333. doi:10.1148/rg.345135113.
- Wheeless CR, Patzkowski J, Krueger C. Wheeless’ Textbook of Orthopaedics. Available at: http://www.wheelessonline.com/ortho/12813.
- Baqué P, Trojani C, Delotte J, et al. Anatomical consequences of "open-book" pelvic ring disruption: a cadaver experimental study. Surg Radiol Anat. 2005;27(6):487-90. doi:10.1007/s00276-005-0027-2.
- Straddle fracture | Radiology Case | Radiopaedia.org. Available at: https://radiopaedia.org/cases/straddle-fracture.
- Balogh Z, King KL, Mackay P, et al. The epidemiology of pelvic ring fractures: a population-based study. J Trauma. 2007;63(5):1066-73; discussion 1072-3. doi:10.1097/TA.0b013e3181589fa4.
- DUNN EL, BERRY PH, CONNALLY JD, et al. Computed Tomography of the Pelvis in Patients with Multiple Injuries. J Trauma Inj Infect Crit Care. 1983;23(5):378-383. doi:10.1097/00005373-198305000-00004.
- Pohlman TH, Walsh M, Aversa J, Hutchison EM, Olsen KP, Lawrence Reed R. Damage control resuscitation. Blood Rev. 2015;29(4):251-262. doi:10.1016/j.blre.2014.12.006.
- Bakhshayesh P, Boutefnouchet T, Tötterman A. Effectiveness of non invasive external pelvic compression: a systematic review of the literature. Scand J Trauma Resusc Emerg Med. 2016;24:73. doi:10.1186/s13049-016-0259-7.
- Nutbeam T BC. Episode 2: The Pelvic Binder | phemcast. Available at: https://phemcast.co.uk/2015/11/05/podcast-episode-2-the-pelvic-binder/.
- Friese RS, Malekzadeh S, Shafi S, Gentilello LM, Starr A. Abdominal Ultrasound is an Unreliable Modality for the Detection of Hemoperitoneum in Patients With Pelvic Fracture. J Trauma Inj Infect Crit Care. 2007;63(1):97-102. doi:10.1097/TA.0b013e31805f6ffb.
- Cullinane DC, Schiller HJ, Zielinski MD, et al. Eastern Association for the Surgery of Trauma Practice Management Guidelines for Hemorrhage in Pelvic Fracture—Update and Systematic Review. J Trauma Inj Infect Crit Care. 2011;71(6):1850-1868. doi:10.1097/TA.0b013e31823dca9a.
- Lopera JE. Embolization in trauma: principles and techniques. Semin Intervent Radiol. 2010;27(1):14-28. doi:10.1055/s-0030-1247885.
- Giannoudis P V., Grotz MRW, Tzioupis C, et al. Prevalence of Pelvic Fractures, Associated Injuries, and Mortality: The United Kingdom Perspective. J Trauma Inj Infect Crit Care. 2007;63(4):875-883. doi:10.1097/01.ta.0000242259.67486.15.
- Issack PS, Helfet DL. Sciatic nerve injury associated with acetabular fractures. HSS J. 2009;5(1):12-8. doi:10.1007/s11420-008-9099-y.
