Authors: Simon Sarkisian, DO (EM Attending, Cooper University Hospital/US Army, Camden, NJ) and Zachary Sletten, MD (EM Attending, Brooke Army Medical Center) // Reviewed by: Alexander Y. Sheng, MD, MHPE (@theshenger); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
You are a busy emergency medicine (EM) attending physician, and you hear about a facial laceration that just checked in. The intern asks you for help repairing the laceration, and you eagerly accompany them into the room excited to endow them with your wisdom on laceration repair. After stepping into the room, you realize you might be in over your head (no pun intended). This is not your run of the mill facial laceration.
The series will review the repair of head, eyes, ears, nose, and throat (HEENT) lacerations, with a focus on the areas where emergency physicians tend to struggle. Today we have the last in the series on lip lacerations.
Case
A 21-year-old male was drinking alcohol at a bar when he decided to start a bar fight. In the middle of this fight he sustained a laceration to his lower lip from a beer bottle. In your ED, the patient has a 2 cm laceration to his left lower lip that involves the mucosa and vermillion border. There are no intraoral lacerations.
Lip Lacerations
The lip is composed of three layers: the mucosal layer (within the oral cavity), the middle muscular layer (orbicularis oris muscle), and the outer mucosal layer consisting of the wet vermillion (internal oral) and the dry vermillion (external oral). The cosmetic outline of the lip where the facial skin meets the vermillion is referred to as the vermillion border. Aesthetically, proper alignment of the vermillion border is crucial as misalignment by 1 mm will cause a noticeable scar7. Generally, lip lacerations can be repaired in the ED, however a surgeon should be consulted when:
- There is crushed or devitalized tissue
- Over 25% of the lip is missing6
Contamination can be considerable, so thoroughly irrigate once nonviable tissue and foreign bodies are removed.
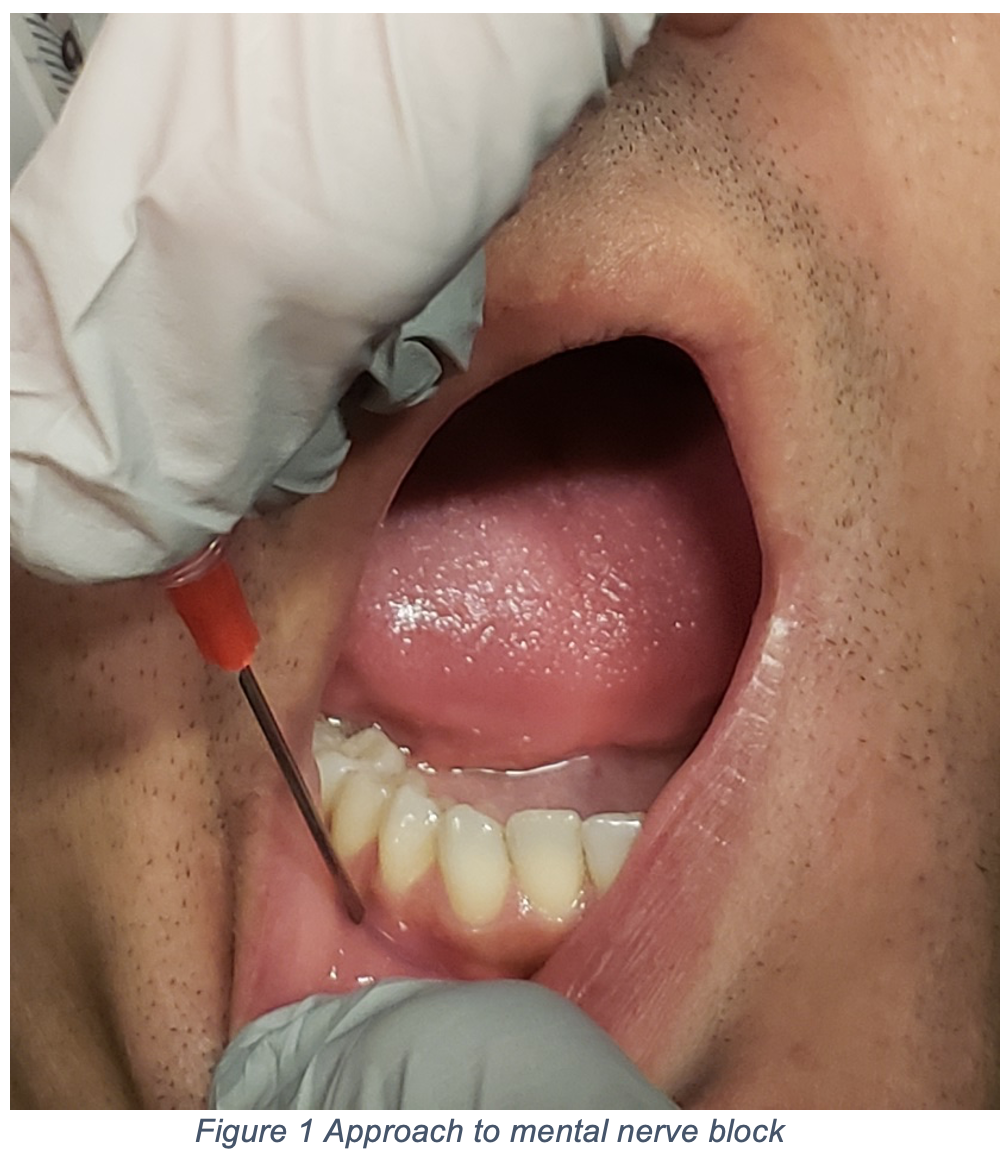
The key to repair of the lip is approximation of the vermillion border. For this reason, a mental nerve block or infraorbital nerve block is an outstanding block for lip lacerations because it avoids tissue distortion though local anesthesia. To perform the mental nerve block, first identify the mental foramen via extraoral palpation (it is usually located just medial to the pupil of the eye when the patient has a forward gaze). Approach the mental foramen intraorally at the mucobuccal fold adjacent to the canine or first premolar at a 45° angle with a 25- or 27-gauge needle and infiltrate adjacent to (not directly in) the foramen as depicted in figures 1 and 2 8,9.

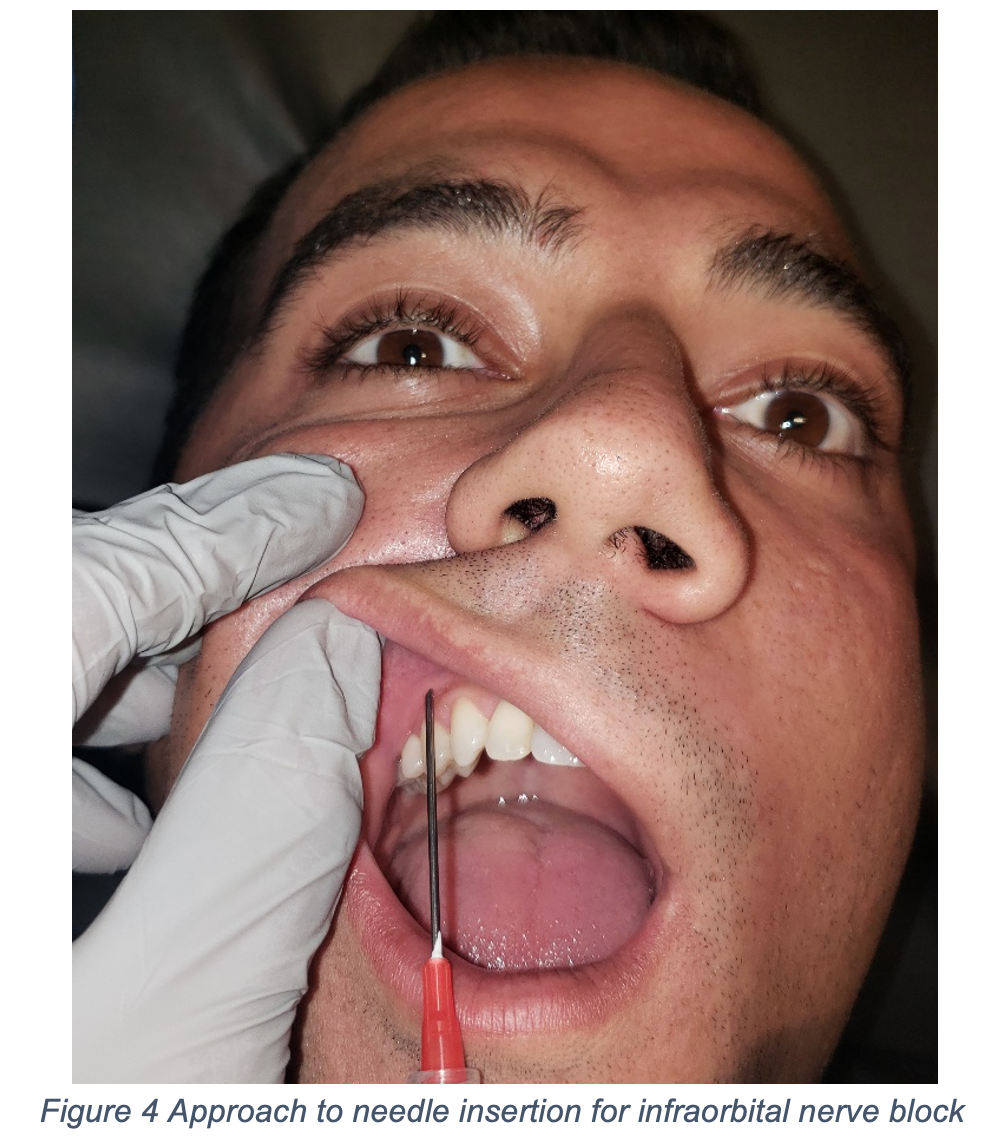
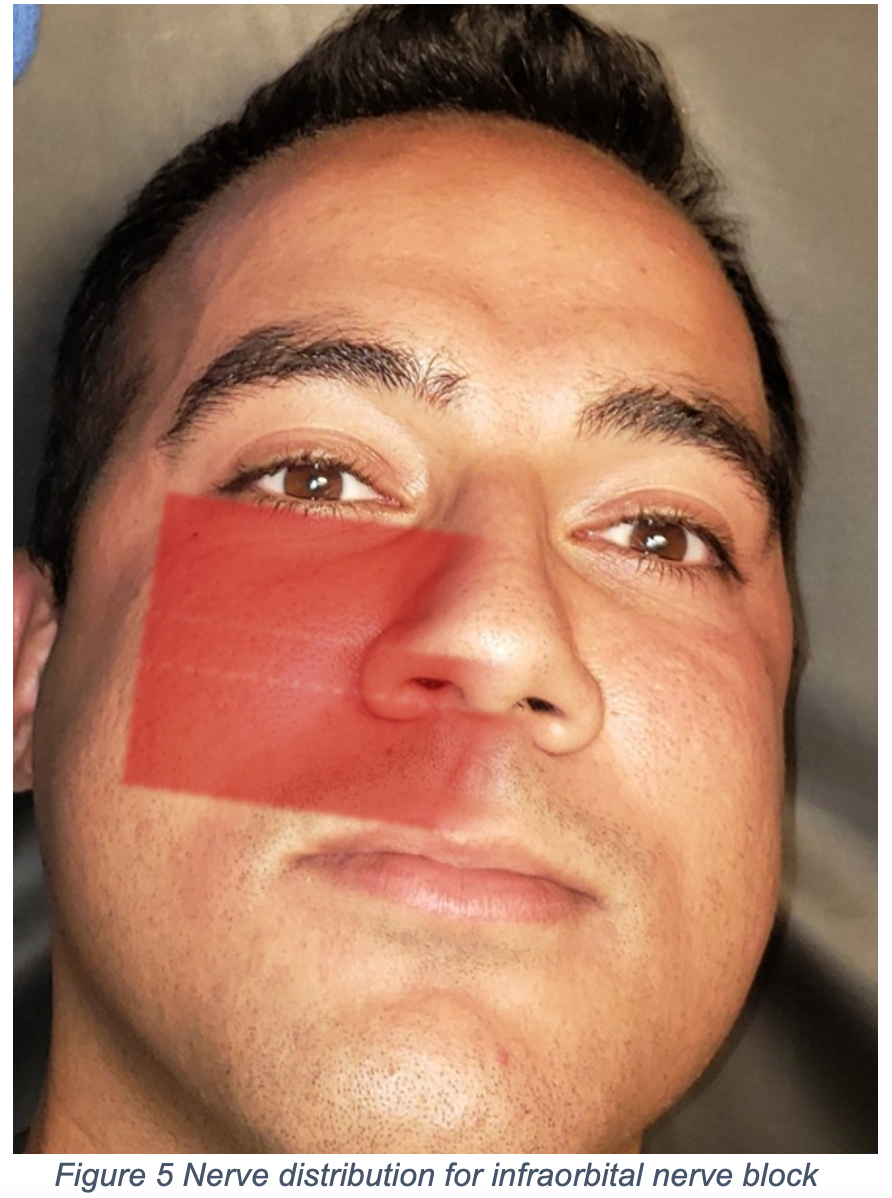
An infraorbital nerve block is the preferred anesthetic modality for upper-lip lacerations because it provides ipsilateral upper-lip anesthesia similar to the mental nerve block for lower-lip lacerations. Typically, the infraorbital foramen is in line with the pupil when the patient has a forward gaze, and although the foramen may not be palpable, it is present immediately under the easily palpated infraorbital ridge. The 25- or 27-gauge needle is inserted parallel to and at the level of the second maxillary premolar and advanced approximately 2.5 cm; injection is adjacent to the foramen8,9. and is depicted in Figures 3, 4, and 5 below. As stated above, direct infiltration of local anesthetic into lip lacerations should be avoided as this can distort the lip tissue, making it more difficult to complete an optimal cosmetic repair.

When repairing the vermillion border, the clinician should first place a single interrupted suture at the vermillion border to ensure proper alignment using a 6-0 nonabsorbable suture. Consider 5-0 or 6-0 nonabsorbable for outer skin closure (Absorbable 6-0 is preferred for children). Consider 5-0 or 6-0 absorbable sutures for mucosal layer (although most small mucosal lacerations do not need to be repaired)
Nonabsorbable sutures should be removed by a health care provider in three to five days, as should any simple interrupted absorbable sutures of the wet or dry vermillion that have not dissolved by five days7.
Other Considerations
How do I dress the wound?
For wounds repaired with simple interrupted sutures, the patient can keep the area moist with a petroleum based jelly (i.e. Vaseline). A nonadherent dressing can be placed for 48 hours with daily dressing changes after that until follow up10,11.
When can the wound get wet?
Daily gentle washing with mild soap and water to remove dried blood and exudate is probably beneficial, especially in areas such as the face or the scalp, but vigorous scrubbing of wounds should be discouraged. Patients may bathe with sutures in place but should not immerse the wound for a prolonged time10.
So I’m good after the sutures are removed, right?
The wound is not totally healed the day the sutures are removed. The recommended time of suture removal is a delicate balance between achieving tensile strength and the foreign body effect and the consequent risk of granuloma and scarring. The most dangerous time of wound dehiscence is the day the sutures are removed. After suture removal, advise the patient to not stretch or pull with shaving, and advise the patient to minimize activity increasing tension across the wound for at least 2 weeks11
Which anesthetic should I use?
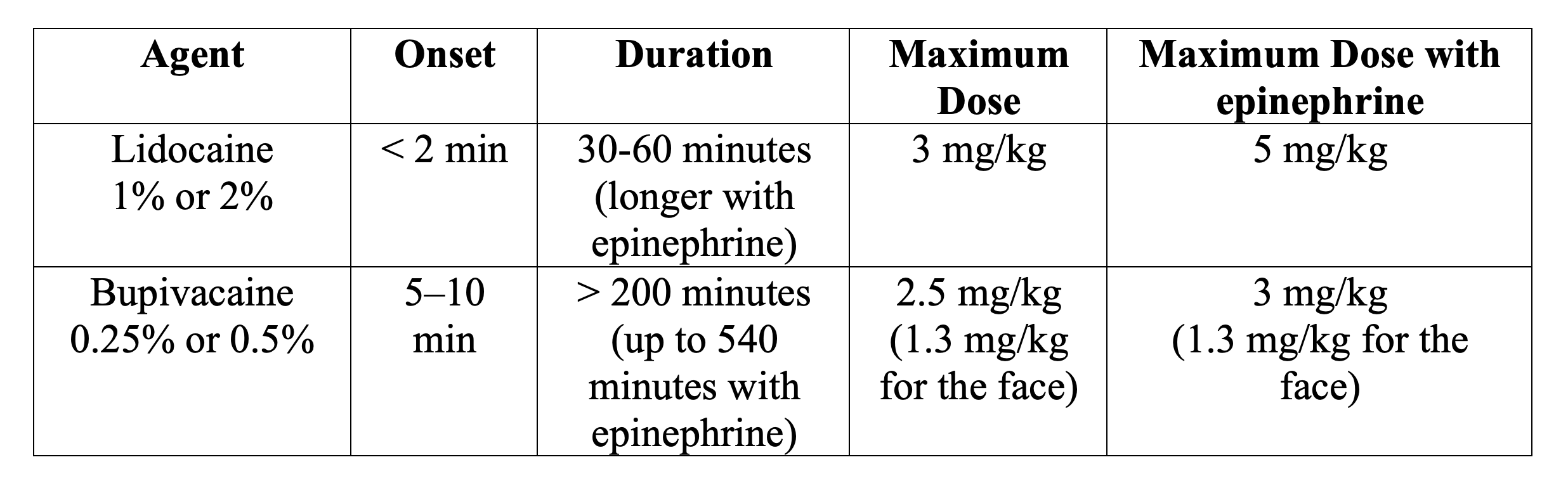
Bupivacaine is a good choice for lengthy procedures such as cleaning and suturing complex forehead lacerations. Lidocaine is better for lip lacerations, so the patient does not accidentally bite the lip and unknowingly mutilate the repair8.
Thanks for joining us on the HEENT laceration series!
References/Further Reading
1. Tintinalli JE, Ma OJ, Yealy DM, et al. Tintinalli’s emergency medicine: a comprehensive study guide. 2020.
2. Hollander JE, Richman PB, Werblud M, Miller T, Huggler J, Singer AJ. Irrigation in facial and scalp lacerations: does it alter outcome? Ann Emerg Med 1998;31:73-7.
3. Singer AJ, Gulla J, Hein M, Marchini S, Chale S, Arora BP. Single-layer versus double-layer closure of facial lacerations: a randomized controlled trial. Plast Reconstr Surg 2005;116:363-8; discussion 9-70.
4. Farion KJ, Russell KF, Osmond MH, et al. Tissue adhesives for traumatic lacerations in children and adults. Cochrane Database of Systematic Reviews 2002.
5. Holger JS, Wandersee SC, Hale DB. Cosmetic outcomes of facial lacerations repaired with tissue-adhesive, absorbable, and nonabsorbable sutures. Am J Emerg Med 2004;22:254-7.
6. Wedmore I. Wound Care: Modern Evidence In The Treatment Of Man’s Age-Old Injuries. Emergency Medicine Practice 2005;7.
7. Assessment and Management of Intra-Oral Lacerations. 2020. (Accessed 25 JUL, 2020, at https://www.uptodate.com/contents/assessment-and-management-of-intra-oral-lacerations?search=Assessment%20and%20Management%20of%20Intraoral%20Lacerations&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1.)
8. Benko K. Fixing Faces Painlessly: Facial Anesthesia in Emergency Medicine. Emergency Medicine Practice 2009;11.
9. Pedigo RA, Zaurova M. Dental Emergencies: Management Strategies That Improve Outcomes [Digest]. Emerg Med Pract 2017;19:S1-S2.
10. Walls RM, Hockberger RS, Gausche-Hill M. Rosen’s emergency medicine : concepts and clinical practice. 2018.
11. Brian Lin ZS. Red, Hot, and Shot, Wound Repair Part 3-Delayed Presentation. EM:RAP. 2017









1 thought on “Preventing Scarface: Pearls for Complicated Facial Lacerations – Lip Laceration”
For the upper lip a full infraorbital block is not needed. A less painful and easier method is to deposit anesthetic adjacent to the ala nasi, usually 1.5 to 2 cc is all you need. Go intraoral, pull the lip up and enter at the junction of the lip and maxillary mucosa and deposit the anesthetic next to the ala nasi. You can palpate externally to feel the area getting full. This gets the branches of the IO nerve going to the upper lip, you can call it a partial IO block or a lip block. If the lac is near the midline sometimes you need to do both sides. Quick, easy, effective. I learned this on an OMFS rotation as a resident 35 years ago and it works every time.