Authors: Simon Sarkisian, DO (EM Attending, Cooper University Hospital/US Army, Camden, NJ) and Zachary Sletten, MD (EM Attending, Brooke Army Medical Center) // Reviewed by: Alexander Y. Sheng, MD, MHPE (@theshenger); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
You are a busy emergency medicine (EM) attending physician, and you hear about a facial laceration that just checked in. The intern asks you for help repairing the laceration, and you eagerly accompany them into the room excited to endow them with your wisdom on laceration repair. After stepping into the room, you realize you might be in over your head (no pun intended). This is not your run of the mill facial laceration.
The series will review the repair of head, eyes, ears, nose, and throat (HEENT) lacerations, with a focus on the areas where emergency physicians tend to struggle. Today we look at tongue lacerations.
Case
A 30-year-old female with a history of epilepsy presents to your ED after having a seizure. She is back to her baseline and reports a recent decrease in her antiepileptic dose that may have contributed to her breakthrough seizure. During your examination you notice a 1 cm laceration of the right lateral border of her tongue.
Tongue Lacerations
Most minor lacerations of the tongue can heal on their own without any intervention. You should repair wounds if they are9:
- Gaping
- Length > 2cm
- Involve lateral border
- Active hemorrhage
- Extend into muscular layer or through-and-through
- Lacerations that may cause dysfunction if healed improperly (such as an anterior split/“serpent” tongue)
Consult a specialist when there is amputation or avulsion of more than 30% because they often require a flap procedure10.
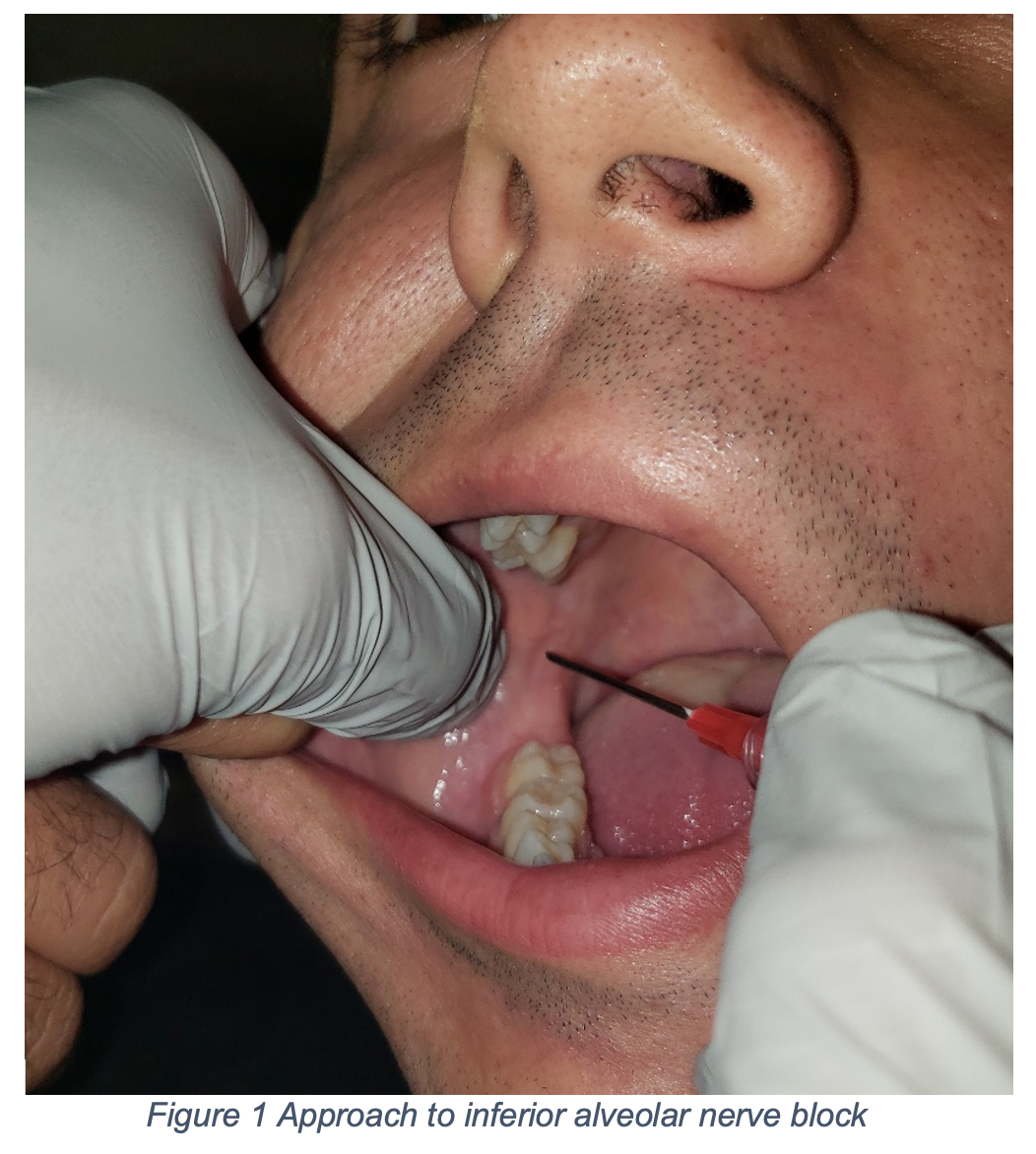
The tongue is innervated bilaterally by the lingual nerve, and anesthesia can be approached with an inferior alveolar nerve block, which provides anesthesia to the anterior 2/3 of the tongue8. If only half the tongue is lacerated, the lingual nerve on that side of the tongue should be blocked. The lingual nerve is slightly anterior and inferior to the inferior alveolar nerve. The target for this block is the inferior alveolar nerve as it passes downward toward the mandibular foramen on the medial aspect of the mandibular ramus. The injection site should be located with the following technique and is depicted in figure 1 below.
- The thumb of the non-injecting hand is placed in the coronoid notch of the mandibular ramus while simultaneously retracting the soft tissues of the buccal mucosa and lip.
- An imaginary line extends from the thumbnail posteriorly toward the pterygomandibular raphe, a mucosal deflection running vertically along the ramus of the mandible.
- The intersection of the imaginary line and the raphe is the injection point. Keep the needle parallel to the occlusal surface of the lower molars
- Advance the needle slowly until contact is made with the mandibular sulcus. Then retract slightly and inject 1-3cc.
- Approach the injection point from the opposite premolar to facilitate contact with the ramus.
- If the laceration is in the midline or the posterior 1/3 of the tongue, direct infiltration is likely necessary.
- Bilateral lingual nerve blocks are not recommended because of a loss of sensation in the entire tongue and choking sensation experienced by the patient.
- Have the patient protrude their tongue and hold it with gauze. Or, put a silk suture through the tongue and use that to pull it out (after proper sedation). Use absorbable 3-0 or 4-0 suture material.
A layered approach for deep lacerations will help prevent the collection of a hematoma. Careful re-approximation is recommended because the suture line can involute and look like a bifid tongue/cleft. Close wounds loosely to allow for swelling. Tie sutures with at least 4 knots. If possible, bury the knot into the wound1.
Within the first 48 hours, complications of tongue laceration can include edema, hemorrhage, and aspiration of saliva and blood. Mild lingual edema may be controlled by application of cold (ie, ice chips, Popsicles). A single dose of intravenous steroids (eg, dexamethasone 0.6 mg/kg) may be considered in more severe cases if no contraindications are present. Hospitalization may be warranted until airway patency is ensured. Other complications of tongue laceration include dehiscence and infection. There is no convincing evidence to guide decisions regarding prophylactic antibiotics6,11. Prevention of dehiscence entails placing sutures loose enough to permit swelling12.
Patients should be advised to avoid eating or drinking until anesthetic wears off. They should eat a soft diet, suck on ice chips or popsicles to prevent tongue swelling, and follow up in 48 hours for re-evaluation of sutures (checking for dehiscence). Whether or not any intraoral laceration is repaired, discharge the patient with chlorhexidine 0.12% oral rinse, 15 mL, swish and spit for 30 seconds every 12 hours7.
Stay tuned for our next piece in the series on repair of oral mucosa lacerations.
References/Further Reading
1. Tintinalli JE, Ma OJ, Yealy DM, et al. Tintinalli’s emergency medicine: a comprehensive study guide. 2020.
2. Hollander JE, Richman PB, Werblud M, Miller T, Huggler J, Singer AJ. Irrigation in facial and scalp lacerations: does it alter outcome? Ann Emerg Med 1998;31:73-7.
3. Singer AJ, Gulla J, Hein M, Marchini S, Chale S, Arora BP. Single-layer versus double-layer closure of facial lacerations: a randomized controlled trial. Plast Reconstr Surg 2005;116:363-8; discussion 9-70.
4. Farion KJ, Russell KF, Osmond MH, et al. Tissue adhesives for traumatic lacerations in children and adults. Cochrane Database of Systematic Reviews 2002.
5. Holger JS, Wandersee SC, Hale DB. Cosmetic outcomes of facial lacerations repaired with tissue-adhesive, absorbable, and nonabsorbable sutures. Am J Emerg Med 2004;22:254-7.
6. Steele MT, Sainsbury CR, Robinson WA, Salomone JA, 3rd, Elenbaas RM. Prophylactic penicillin for intraoral wounds. Ann Emerg Med 1989;18:847-52.
7. Walls RM, Hockberger RS, Gausche-Hill M. Rosen’s emergency medicine: concepts and clinical practice2018.
8. Benko K. Fixing Faces Painlessly: Facial Anesthesia in Emergency Medicine. Emergency Medicine Practice 2009;11.
9. Wound Magment, Part II. 2018. (Accessed 07 JUL, 2020, at https://www.emrap.org/episode/c3wound1/c3wound.)
10. Egozi E, Faulkner B, Lin KY. Successful revascularization following near-complete amputation of the tongue. Ann Plast Surg 2006;56:190-3.
11. Mark DG, Granquist EJ. Are prophylactic oral antibiotics indicated for the treatment of intraoral wounds? Ann Emerg Med 2008;52:368-72.
12. Evaluation and Repair of Tongue Lacerations. 2020. (Accessed 10 JUL, 2020, at https://www.uptodate.com/contents/evaluation-and-repair-of-tongue-lacerations?search=evaluation%20and%20repair%20of%20tongue%20lacerations&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1.)








