Authors: Jacob Ernst, DO, MS (EM Resident at Madigan Army Medical Center) and Jason Bothwell, MD (Staff physician, Madigan Army Medical Center) // Edited by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
A 60-year-old male with history of ischemic cardiomyopathy with last documented LVEF of 38% presents to your ED with chief complaint of ‘passing out.’ He was sitting at his kitchen table reading the newspaper and recalls a sensation of warmth and flushing with tunnel vision. He awoke an unknown amount of time later in a seated position at the table. His wife found him confused and called EMS. He denies chest pain, shortness of breath, or blood in stools and is asymptomatic at this time. Medications include lisinopril and metoprolol succinate. Vital signs on presentation include T 37 deg C, HR 68 bpm, BP 128/72, RR 16, and SPO2 98% on room air. Physical exam is remarkable for a regularly regular rhythm, no murmurs, and occasional rales in the lung bases bilaterally. There is mild bilateral lower extremity pitting edema to the mid-tibial shaft and no obvious JVD. He is otherwise A&O x 4, with no focal neurologic deficits. ECG is notable for non-specific ST segment and T wave abnormalities, but no STE/STD.
Diagnosis: Syncope
Definition:
Syncope is defined as a symptom complex composed of an abrupt, brief loss of consciousness with inability to maintain postural tone that spontaneously and completely resolves without medical intervention.1,2
Importance:
- Syncope represents approximately 1-1.5% of all ED visits nationwide.1,2
- Up to 6% of hospital admission are for a diagnosis of syncope.
- Up to 30% of unexplained falls in elderly patients may be due to syncope.
- 1 in 5 people experience syncope in their lifetime.
- Up to 10% of cases of Thoracic Aortic Dissection, Acute Coronary Syndrome, Subarachnoid Hemorrhage, or Pulmonary Embolus present with syncope.1,2
Pathophysiology:
All types of syncope are resultant of the same general underlying pathophysiologic process, either:1-3
- Complete disruption of cerebral blood flow for > 10 seconds or,
- A sustained drop in cerebral perfusion by 35-50%.
Categories:
Syncope can be broadly categorized into either Cardiac, Neural/Reflex-Mediated, or Other predefined causes:1-3
1. Cardiac causes can be further simplified into either structural or arrhythmogenic causes:
Examples of structural causes include: Severe aortic stenosis and other valvular heart disease, Pericardial disease, Aortic dissection, Pulmonary embolus, Myocardial ischemia or infarction
Examples of dysrhythmia include: Bradydysrhythmias (short or long QT syndrome, sinus node disease or pacemaker malfunction), Tachydysrhythmia (ventricular tachycardia, torsades de pointes, SVT or atrial fibrillation)
2. Neural or Reflex-mediated causes: Vasovagal (the most common cause; usually associated with a specific trigger), Situational (micturition or swallowing, for example), Carotid sinus syndrome (potentially the most common in elderly populations, can be triggered by something as simple as wearing a tight collared shirt)
3. Other causes: Orthostatic hypotension, Neurologic (TIA, migraines or subclavian steal syndrome), Medications, Psychiatric Conditions
AHA/ACC/HRS 2017 Recommendations
History and Physical Examination:1,2,4
Class I /Level B: A detailed history and physical should be performed in patients with syncope.
Importance historical features to consider include any history of congestive heart failure (either current or in the past); known coronary artery disease or structural heart disease; or any symptoms that could represents PE, ACS, aortic dissection or SAH.
Risk factors to consider include age > 60, exertional syncope, family history of early cardiac death, abnormal cardiac exam, male sex, or presence of known structural or ischemic heart disease.
ED Evaluation
Recommended diagnostic testing:
Class I, Level B: Obtain a 12 lead ECG.2,5
- A 12-lead ECG is inexpensive, widely available, and will often times help elucidate an active underlying arrhythmia or arrhythmogenic condition (for example, Brugada Syndrome or WPW) which contributed to the syncopal event.
Laboratory evaluation
Class IIa, Level B Recommendations: Targeted blood tests are reasonable in the evaluation of selected patients with syncope identified on the basis of clinical assessment from history, physical exam and ECG:2,6
- For example:
- CBC to evaluate for underlying anemia
- BMP to evaluate for renal disease or elevated BUN suspicious for GI blood loss
- Troponin if concern for acute coronary syndrome
- D- dimer if concern for PE or dissection
Class IIb, Level C: Usefulness of brain natriuretic peptide and high-sensitivity troponin measurement is uncertain in patients for whom a cardiac cause of syncope is suspected.2
Class III, Level B: Routine comprehensive laboratory evaluation in patients with syncope is NOT useful.2,7
Imaging
Class III, Level B Recommendation: MRI and CT of the head are NOT recommended in the routine evaluation of patients with syncope in the absence of focal neurologic findings or head injury.2
Risk Stratification:
Class I, Level B: Evaluation of the cause and assessment for the short and long-term morbidity and mortality risk associated with syncope are recommended.2,8
The table below represents known short and long-term risk factors, reprinted from table 5 in the AHA/ACC/HRS 2017 guidelines.2
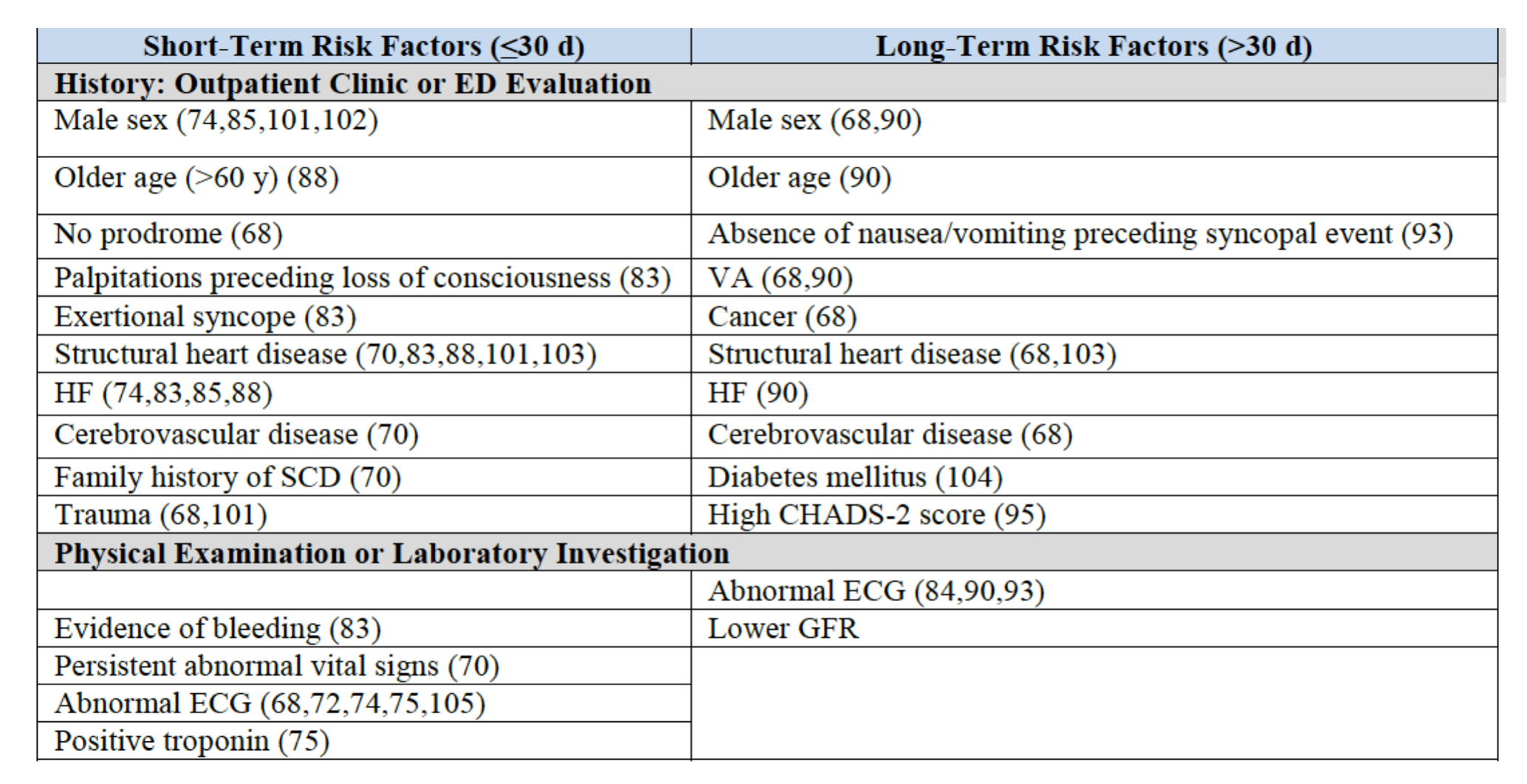
Class IIB, Level B: Use of risk stratification scores may be reasonable in the management of patients with syncope.2
There are several studies evaluating multiple risk stratification scores; the OESIL, Boston Syncope Rule, and San Francisco syncope rule to name a few. The most commonly deployed and well-validated decision rule in the ED setting is the San Francisco Syncope Rule.9

From https://www.instagram.com/p/BMnB3lGAZGc/
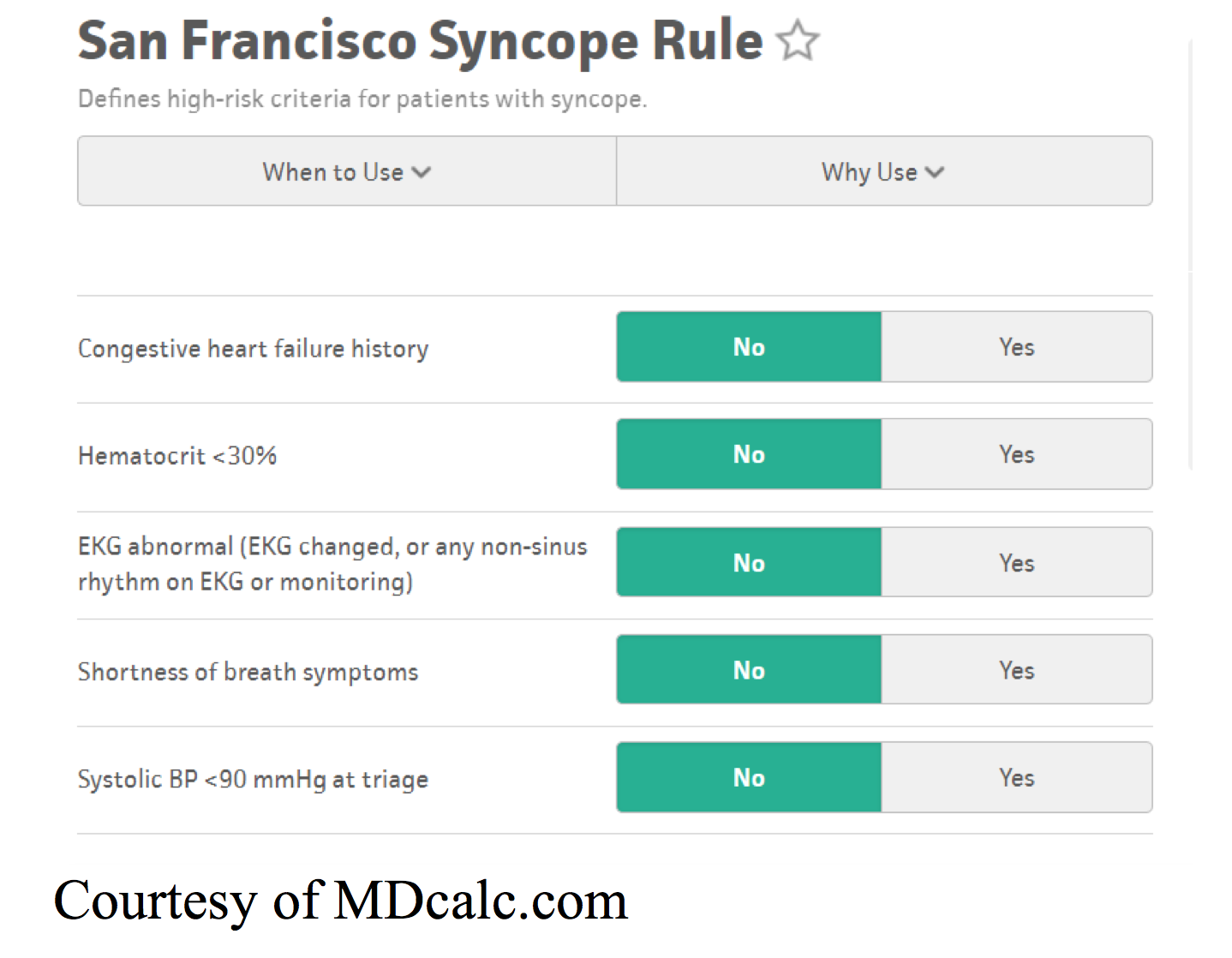

In a meta-analysis by Saccilotto et al (2011), the SFSR was found to have a pooled estimated sensitivity of 0.87 (95% CI 0.79 – 0.93) and pooled estimated specificity 0.52 (95% CI 0.43-0.62).9
- Probability of serious outcome was < 5% with negative (zero out of 5 criteria) SFSR, and less than 2% when applied to patients whom which there was NO obvious cause after initial evaluation.
- Overall negative predictive value was 97%.
Of note, the SFSR strictly predicts the short-term risk of adverse outcomes within 30 days of ED discharge.11
Since the development of the SFSR, several studies have attempted to replicate the sensitivity and specificity of the decision rule and evaluate its utility in ED patients presenting with syncope. For example, a prospective study by Birnbaum et al. noted substantially lower sensitivity and specificity than in previous studies at 74% and 57% respectively.12 Another prospective study by Sun et al reported a sensitivity of 89% and specificity of 42% for the primary outcome of predicting any serious clinical event within 7 days of ED discharge.13 In general, there is conflicting data regarding the true sensitivity and specificity of the SFSR and it has been at the very least difficult to replicate the original study conclusions. Refer to the section at the end of this write-up on the importance of physician gestalt in the disposition of these patients.
Disposition:
The AHA/ACC/HRS proposes the following general algorithm:2
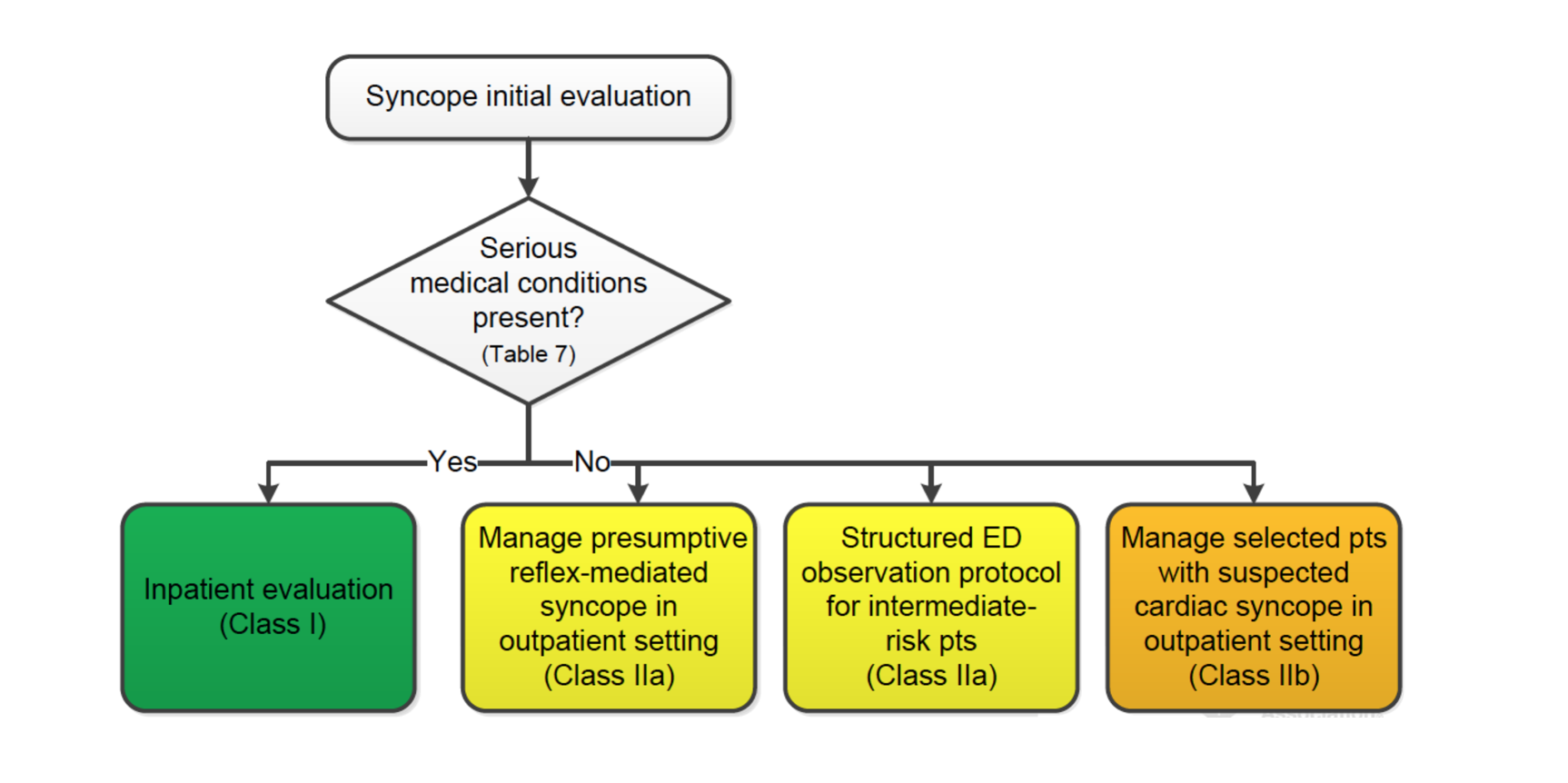
Examples of serious medical conditions potentially warranting inpatient evaluation include (adapted from AHA guidelines):
2007 ACEP Clinical Policy
For the reader’s comparison, the following briefly outlines the 2007 ACEP clinical policy recommendations.1 Similarities to the 2017 AHA/ACC/HRS updates have been bolded for ease of comparison. Of note, the 2017 guidelines are endorsed by and were developed in collaboration with ACEP and SAEM.
- What history and physical exam data help to risk stratify patients with syncope?
- Level A Recommendation: use history and exam features consistent with heart failure to identify patients at higher risk for adverse outcomes.
- Level B Recommendations
- Consider older age, history of structural heart disease or coronary artery disease as risk factors for adverse outcomes.
- Consider younger patients with syncope that is non-exertional, without history or signs of cardiovascular disease, a family history of sudden death, and without comorbidities to be at low risk of adverse events.
- Level C recommendations: none specified
- What diagnostic testing helps risk-stratify patients with syncope?
- Level A Recommendation: Obtain a standard 12 lead ECG in patients with syncope.
- Level B Recommendation: none specified.
- Level C Recommendation: Laboratory testing and advanced investigative testing such as echocardiography or cranial CT scanning need not be routinely performed unless guided by specific findings in the history or physical examination.
- Who should be admitted after an episode of syncope?
- Level A Recommendation: none specified.
- Level B Recommendation:
- Admit patients with syncope and evidence of heart failure or structural heart disease.
- Admit patients with syncope and other factors that lead to stratification as high-risk for adverse outcome.
- Level C Recommendation: none specified.
With respect to the Level B recommendation to admit patients with factors placing them at high risk for adverse outcome, the 2007 ACEP guidelines propose the following table as high-risk factors:1

Conclusions:
Syncope is a common presenting complaint in the ED. A thorough H&P and 12-lead electrocardiogram are the cornerstones of evaluating these patients. Focused laboratory testing can be useful, but routine imaging studies are not recommended. In patients with no obvious cause for their syncope after initial evaluation, it is reasonable to risk-stratify using the San Francisco syncope rule and consider outpatient follow up. Admit patients with high-risk historical features, physical examination findings, past medical history or laboratory findings.
Physician Judgement – a few brief notes…
There is a growing body of evidence suggesting that physician clinical judgement is at least as good (if not better) in predicting serious outcomes in patients presenting with syncope. In a 2014 meta-analysis by Constantino et al of 3681 patients, physician clinical judgement performed better than any of the evaluated syncope rules in predicting serious outcomes at 10 and 30 days.15 In other words, the best decision rule we have may not outperform a savvy physician’s judgement. Keep this in mind when evaluating patients presenting with syncope!
EM Pearls:
- All patients presenting with syncope should undergo thorough H&P and a 12-lead ECG.
- Up to 10% of subarachnoid hemorrhage, aortic dissection, acute coronary syndrome, and pulmonary embolus present with syncope.
- Beware of features such as known cardiovascular disease, history or evidence of congestive heart failure, age > 60, or an exertional component to presentation.
- Routine neuroimaging is NOT
- Patients with serious medical conditions such as history of cardiac arrhythmias, structural cardiac disease, trauma, or persistent abnormal vital signs should be considered for admission.
- In patients with no known cause for their syncope after initial evaluation, risk stratification with a decision rule such as the San Francisco Syncope Rule is acceptable.
- Patients with zero out of 5 categories positive in the SFSR have a < 2% probability of serious outcome.
- Physician judgement may be just as good as decision rules in predicting serious adverse outcomes in patients presenting with syncope.
References / Further Reading:
- Huff et al. Clinical Policy: Critical Issues in the Evaluation and Management of Adult Patients Presenting to the Emergency Department with Syncope. Ann Emerg Med. 2007; 49: 431-444.
- Shen W-K et al. 2017 ACC/AHA/HRS Guidelines for the Evaluation and Management of Patients With Syncope. Circulation (2017).
- Tintinalli’s Emergency Medicine
- Alboni P, Brignole M, Menozzi C, et al. Diagnostic value of history in patients with syncope with or without heart disease. J Am Coll Cardiol. 2001; 37:1921-8.
- Pérez-_Rodon J, Martinez-Alday J, Baron-Esquivias G, et al. Prognostic value of the electrocardiogram in patients with syncope: data from the group for syncope study in the emergency room (GESINUR). Heart Rhythm. 2014; 11:2035-44.
- Chiu DT, Shapiro NI, Sun BC, et al. Are echocardiography, telemetry, ambulatory electrocardiography monitoring, and cardiac enzymes in emergency department patients presenting with syncope useful tests? A preliminary investigation. J Emerg Med. 2014; 47:113-8.
- Pfister R, Diedrichs H, Larbig R et al. NT-pro-BNP for differential diagnosis in patients with syncope. Int J Cardiol. 2009; 135: 51-4.
- Costantino G, Perego F, Dipaola F, et al. Short- and long-term prognosis of syncope, risk factors, and role of hospital admission: results from the STePS (Short-Term Prognosis of Syncope) study. J Am Coll Cardiol. 2008; 51:276-83.
- Saccilotto RT, Nickel CH, Bucher HC, et al. San Francisco Syncope Rule to predict short-term serious outcomes: a systematic review. CMAJ. 2011; 183:e1116-e26.
- Quinn JV, Stiell IG, McDermott DA, et al. Derivation of the San Francisco Syncope Rule to predict patients with short term serious outcomes. Ann Emerg Med. 2004; 43:224-232.
- Moya A, Sutton R, Ammirati F, et al. Guidelines for the diagnosis and management of syncope (version 2009). Eur Heart J. 2009; 30:2631-71.
- Birnbaum A, Esses D, Bijur P, Wollowitz A, Gallagher EJ. Failure to validate the San Francisco Syncope Rule in an independent emergency department population. Ann Emerg Med. 2008; 52(2): 151-9.
- Sun BC et al. External validation of the San Francisco Syncope Rule. Ann Emerg Med. 2007; 49(4): 420-7.
- MDCalc.com
- Constantino et al. Syncope risk stratification tools vs clinical judgement: an individual patient data meta-analysis. Am J Med. 2014; 127:1126 e13-25.









