Author: Ronnie Barakat, MD (EM Resident Physician, Parkland Memorial Hospital/UT Southwestern) // Editors: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
You’re nearing the end of your shift in a busy county emergency department. You go to see a new patient who has a history of HIV diagnosed in Mexico who presents with a chief complaint of “difficulty walking.” During the interview, the patient states he is having difficulty keeping his balance. Your neurology exam is normal with the exception of a positive Romberg’s sign. The patient has otherwise been feeling well but has poor compliance with his anti-retrovirals. He has been followed in your hospital system for the past year, but upon chart review you notice the patient does not have an RPR on file. Your mind turns to syphilis…
Background
The word “syphilis” derives from the Latin poem Syphilis, sive morbus gallicus, which translates into “Syphilis, or the French disease.” The poem, originally published in 1530, describes the first recorded syphilis epidemic in the Western world, which coincided with the French invasion of Italy. (1) Today, syphilis incidence rates in the U.S. are 5.3 per 100,000 population. Furthermore, trends from 2000 to 2013 showed an increase in incidence over that time period. This disease predominantly affects males, with African-Americans and men who have sex with men at greatest risk. (2) Syphilis is a manifestation of infection by the spirochete Treponema pallidum and can be transmitted sexually or vertically (maternal-fetal). Humans are the only reservoir for syphilis, and it cannot be spread from non-living reservoirs such as toilet seats or eating utensils. (13)(14) Syphilis can affect almost any organ of the body, particularly in its secondary and tertiary stages, earning the moniker “the Great Imitator.”
Clinical Manifestations
Primary Syphilis
Classically, the first manifestation of syphilis is a single, painless, sharply-demarcated chancre (ulcer) with a clean base and localized painless lymphadenopathy. However, this is not always reliable for definitive diagnosis. This classic presentation has a low sensitivity of 31% but high specificity of 98%. The most sensitive finding is purulence involving <30% of the base. (3) It is important to note that on occasion more than one chancre may be present, and up to 25% may be painful. This may occur on the penis, vulva, cervix, anus, or oral cavity depending on the point of sexual contact. The chancre usually occurs 9-90 days after inoculation and resolves without scarring within 6 weeks. (4)
Secondary Syphilis
Secondary syphilis begins approximately 3-5 months after initial infection, during which time bacteria move from the initial chancre to the bloodstream via the lymphatic system. This stage is characterized by generalized lymphadenopathy and non-pruritic maculopapular rash that involves the palms and soles that is classically “copper colored.” This rash is usually diffuse, and up to 80% of patients report involvement of palms and soles. Patients also often present with oral and/or genital mucus lesions. Mucus lesions in the mouth are usually painless with central erosion which may cause sore throat. Genital mucus lesions typically occur in women and present as condylomata, ulcerations, or papules. Patients may also present with various constitutional symptoms such as headache, fever, malaise, nausea, anorexia, and low-grade fever. (5)(14)(15)

Circulating immune complexes contain treponemal antigen and antibody which can deposit in various organs of the body, leading to less common manifestations of secondary syphilis such as:
- Ocular complications such as scleritis, keratitis, or posterior uveitis
- Sensorineural deafness or tinnitus
- Proteinuria, nephrotic, or nephritic syndrome
- Syphilitic hepatitis leading to jaundice
- The classic “moth eaten appearance” of alopecia in secondary syphilis only occurs in 7% of patients. (5)(15)
Latent Syphilis
This is the period in which secondary presentations disappear until tertiary symptoms develop. During this time, patients are asymptomatic before the serious complications of tertiary syphilis develop.
Tertiary syphilis
After the latent phase, tertiary syphilis occurs in 1/3 of untreated individuals 5-25 years after initial infection and manifests as gummatous (benign) syphilis, cardiovascular syphilis, or neurosyphilis. Tertiary syphilis has a mortality rate of 20%. (13)
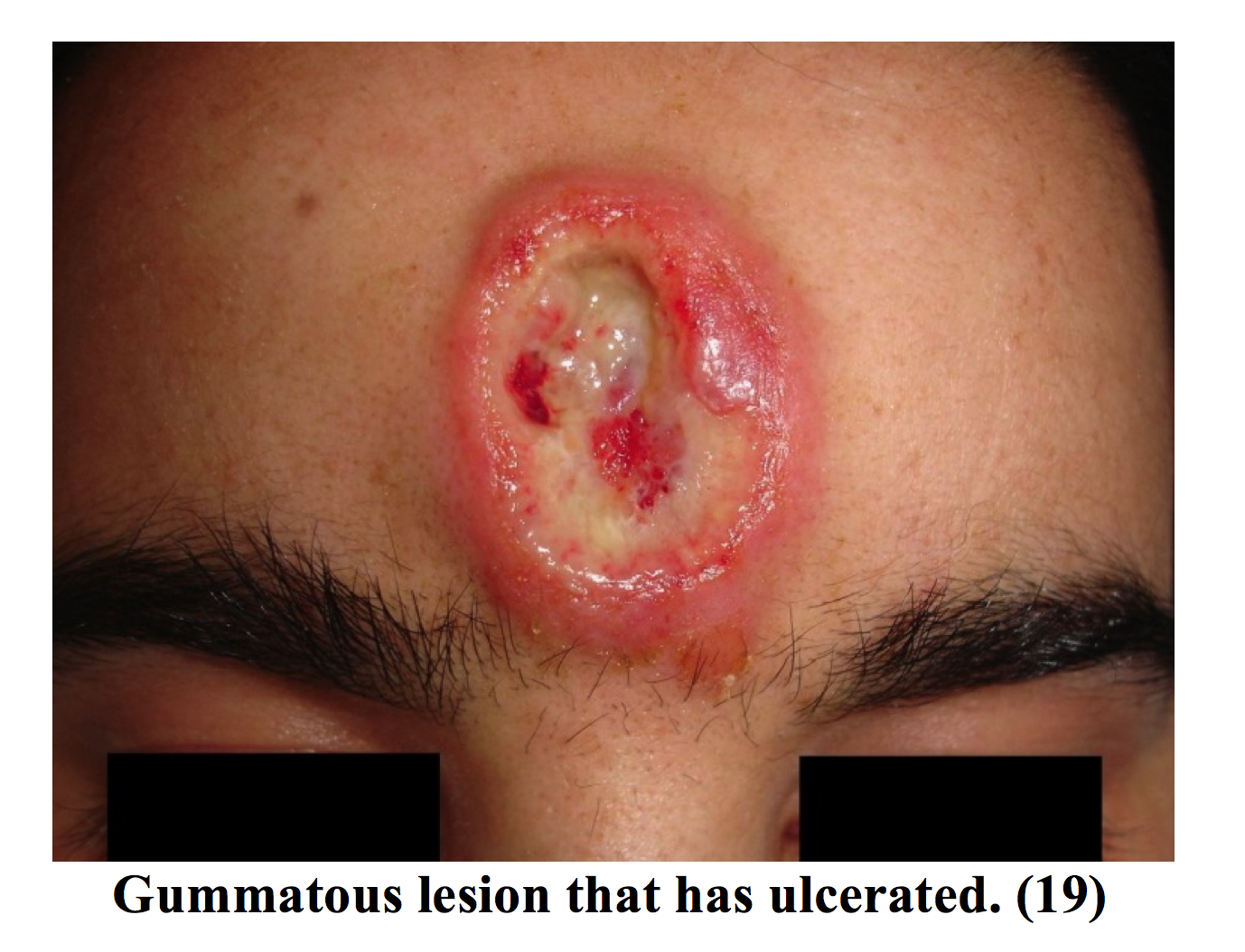
Gummas occur as painless indurated nodules over the skin and can occur on other organs such as liver, spleen, and bone. These are granulomatous lesions that ulcerate and scar. While this is a “benign” manifestation, it can have serious social implications for the patient as it may lead to disfigurement. Gummas resolve promptly with anti-microbial treatment, discussed later. (16)
Tertiary Syphilis – Cardiovascular Manifestations
Cardiovascular syphilis occurs when the spirochete invades the aortic wall. The subsequent endarteritis of the vasa vasorum causes necrosis and weakening of muscular and collagen fibers in the media of the ascending aorta. Its most common manifestation is syphilitic aortitis. It is usually asymptomatic, though 20-25% of patients may present with anginal-type symptoms or heart failure. If aortitis remains untreated, the most common complication is aortic regurgitation. (7)(5) Ascending aortic aneurysm is the least common presentation. The most feared complication of cardiovascular syphilis is aortic dissection or ruptured thoracic aneurysm. (5)
Tertiary Syphilis – Neurologic Manifestations
In the tertiary stage, neurologic manifestations of syphilis vary. Early neurologic manifestations include asymptomatic meningitis, or acute syphilitic meningitis. Patients may be asymptomatic but have an elevated CSF white count or positive CSF VDRL test. Syphilitic meningitis presents with the same CSF findings, as well as typical meningitic symptoms such as headache, fever, and neck stiffness. (7)(8)(5)
Later neurologic manifestations of the tertiary phase include meningovascular syphilis, tabes dorsalis, and paresis. Ten percent of all neurosyphilis cases manifest as meningovascular syphilis. This occurs 5-7 years after initial infection. These patients typically present with encephalopathic features such as mood changes, seizures, or altered consciousness. Occasionally this encephalopathy is accompanied by a focal neurologic deficit. Tabes dorsalis occurs 5-25 years after initial infection. Up to 64% of patients may present with the Argyll-Robertson pupil, which constricts with accommodation but not with reaction to light. The dorsal column of the spinal cord is also affected, presenting as a wide-based gait due to sensory ataxia, positive Romberg’s sign, and loss of temperature sensation. Less specific signs of tabes dorsalis are distal extremity neuropathies and areflexia or hyperreflexia. Paresis occurs 5-25 years after initial infection, similar to tabes dorsalis. This presents initially as dementia and later progresses to psychotic symptoms. (5)
HIV and Syphilis
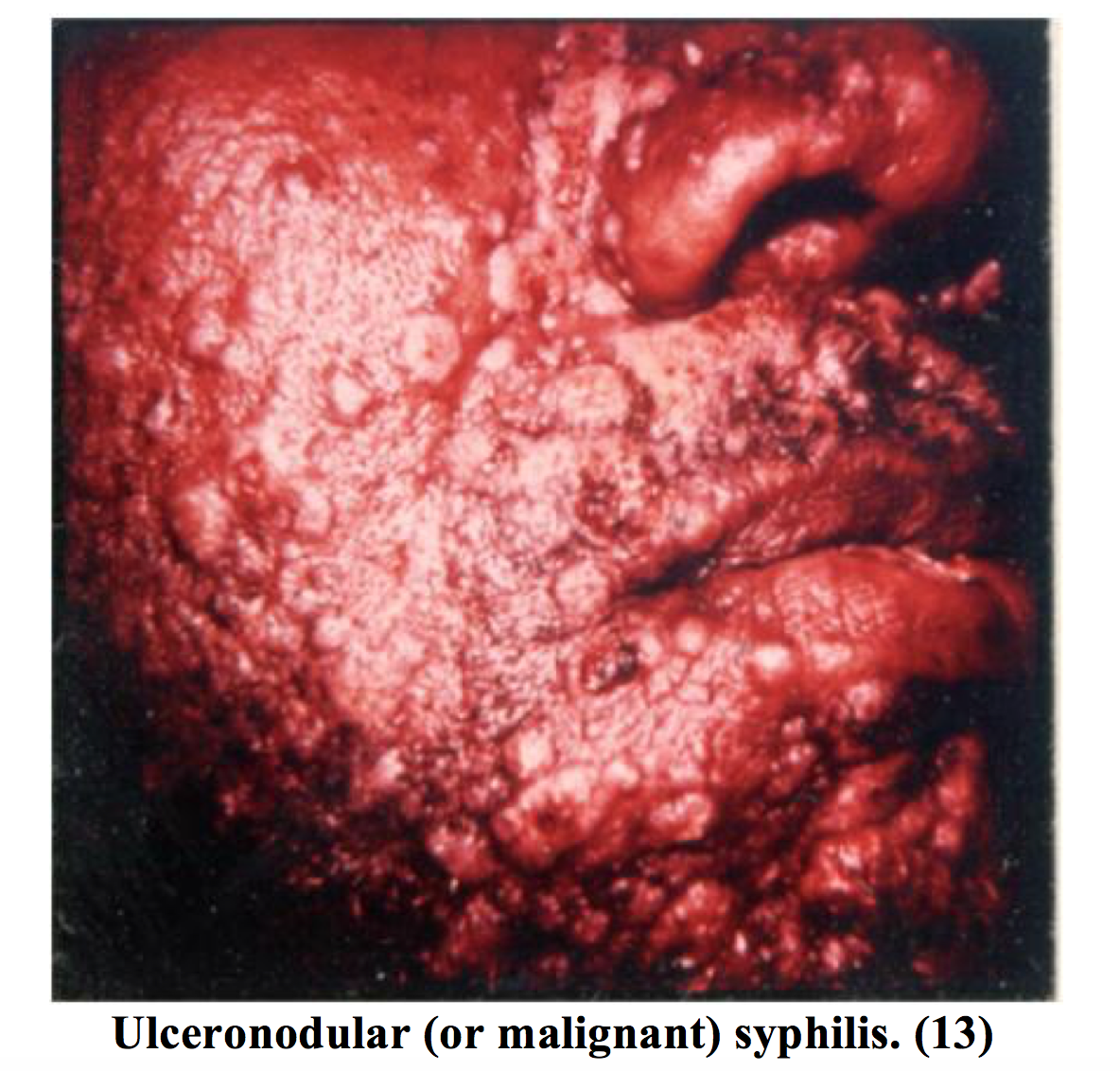
The rate of coinfection of HIV and syphilis ranges from one-third to two-thirds of patients diagnosed with syphilis. HIV-positive patients can present with unusual variations of this disease. Infection with HIV may lead to more rapid progression of syphilis to both secondary and tertiary stages, particularly to neurosyphilis. In this patient, population primary and secondary syphilis are more likely to overlap. (6) Patients may also present with ulceronodular or malignant syphilis during the secondary stage. This is a rare skin variation that is characterized by pustules with ulcerated necrotic centers. (5)(18)(19)
Diagnosis
In any case where syphilis is suspected, a sexual history is paramount. In a patient with prior history of STDs or history of new sexual partners, specific laboratory tests can help confirm your suspicion. Venereal Disease Research Laboratory (VDRL) test and rapid plasma reagin (RPR) test are useful screening tests. It takes 1-4 weeks for these tests to become positive, so within the context of the ED, clinical suspicion should guide treatment early in the disease course. Because these tests detect antibodies against cardiolipin, they may be falsely positive in increased age, pregnancy, SLE, malignancy, or other infectious processes. It is important to note that once a patient tests positive for RPR/VDRL they will remain positive for life, making screening for reinfection difficult. (9) (11) (5) The confirmatory tests include serum fluorescent treponemal antibody absorption test (FTA-ABS) and darkfield microscopy; however, these are usually unavailable in the ED. (11)
If a patient has a positive RPR and there is a suspicion for cardiovascular syphilis, CT angiography of the aorta should be performed if the patient is stable. If the patient is unstable bedside TEE is the study of choice. Cardiothoracic or vascular surgery should be consulted. Lumbar puncture with CSF VDRL with associated elevated CSF lymphocyte count is diagnostic for neurosyphilis. However, if a patient exhibits signs of increased intracranial pressure, a CT brain should be obtained first. (5)
All newly diagnosed patients with syphilis should be screened for HIV, gonorrhea, chlamydia, and hepatitis B. (11)
Treatment
There are several nuances to treatment of syphilis. Please see the 2015 CDC recommendations and the CDC website for detailed information. Primary and secondary syphilis are treated with a single dose of penicillin G benzathine, 2.4 million units IM. If a patient has a penicillin allergy they may be treated with doxycycline BID for 2 weeks. Pregnant women with a penicillin allergy must be desensitized and treated with oral penicillin G. Tertiary syphilis is treated with penicillin G benzathine, 2.4 million units IM once weekly for three weeks. Patients should follow up for repeat testing in 6-12 months. Sexual partners in the past 90 days should also be treated. (11) (12)
The Jarisch-Herxheimer reaction occurs due to release of T. pallidum lipoproteins from dying organisms. It is most common in treatment of early syphilis. It occurs within 12 hours of treatment and ends within 24 hours of beginning treatment. It presents as low-grade fever, secondary rash, and other constitutional symptoms such as headache, pharyngitis, and malaise. This is not an allergic reaction, and symptomatic management with acetaminophen is the treatment of choice. (5)
Case Conclusion:
You perform an RPR on your patient, which is positive. You then perform a lumbar puncture and admit the patient. While admitted the CSF VDRL is positive, and there is a mononuclear pleocytosis consistent with neurologic tertiary syphilis. The patient is treated with IM penicillin and later discharged from the hospital.
Summary
- Syphilis is known as the “Great Imitator” and can present as almost any condition.
- The natural history of syphilis in HIV patients is accelerated, and various stages may overlap.
- When exploring the diagnosis, recording a full sexual history is paramount. Patients with positive RPR in the past will have a positive RPR for the rest of their lives.
- Pregnant patients with penicillin allergies should be treated with penicillin desensitization.
- Check the CDC for detailed treatment recommendations. Penicillin is typically the go-to therapy. Tertiary stage syphilis requires IM penicillin weekly for three weeks.
- Jarisch-Herxheimer is not an allergic reaction; the treatment of choice is acetaminophen.
References/Further Reading:
- Frith J. Syphilis – Its early history and Treatment until Penicillin and the Debate on its Origins. Journal of Military and Veterans’ Health. 2012;(20)4.
- Patton ME, Su JR, Nelson R, et al. Primary and Secondary Syphilis–United States, 2005-2013. Morb Mortal Wkly Rep. 2014; (63)18; 402-406.
- DiCarlo RP, Martin DH. The clinical diagnosis of genital ulcer disease in men. Clin Infect Dis. 1997;(25)2; 292-298.
- Read PJ, Donovan B. Clinical aspects of adult syphilis. Internal Medicine Journal. 2012 Jun;42(6):614-20
- Singh AE, Romanowski B. Syphilis: Review with Emphasis on Clinical, Epidemiological, and Some Biologic Features. Clinical Microbiology Review. 1999 Apr;12(2):187-209.
- Drago F, Merlo G, Rebora A, Parodi A. Syphilitic aortitis and its complications in the modern era. G Ital Dermatol Venereol. 2016.
- Holmes MD, Brant-Zawadzski MM, Simon RP. Clinical features of meningovascular syphilis. Neurology. 1984 Apr;34(4):553-6.
- Chesson HW, Heffelfinger JD, Voigt RF, Collins D. Estimates of primary and secondary syphilis rates in persons with HIV in the United States, 2002. Sex Transm Dis. 2005 May;32(5):265-9.
- Hook WE, Marra CM. Acquired syphilis in adults. N Engl J Med. 1992; 326:1060-1069
- JE, Tintinalli. Emergency Medicine: A Comprehensive Study Guide, 8th Edition. McGraw-Hill. 2011. 1012-1013.
- G, Mackay. Current Diagnosis & Treatment: Obstetrics and Gynecology, 11e. Chapter 43 Sexually Transmitted Diseases & Pelvic Infections. New York. McGraw-Hill. 2013.
- Radolph, Justin D. “Chapter 36: Treponema”. Medical Microbiology. 4th edition. Baron S, editor. Galveston (TX): University of Texas Medical Branch at Galveston; 1996. Retrieved August 29, 2017. http://www.ncbi.nlm.nih.gov/books/NBK7716/#A1994
- “Sexually Transmitted Diseases: Syphilis CDC Fact Sheet”. Centers for Disease Control and Prevention. Retrieved August 29, 2017. http://www.cdc.gov/std/syphilis/STDFact-Syphilis.htm
- Baughn RE, Musher DM. Secondary Syphilitic Lesions. Clinical Microbiology Reviews. 2005;18(1); 205-216.
- Zetola NM, Engelman J, Jensen TP, Klausner JD. Syphilis in the United States: an update for clinicians with an emphasis on HIV coinfection. Mayo Clin Proc. 2007 Sep;82(9):1091-102.
- Workowski KA, Berman SM; Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2006. MMWR Recomm Rep 2006; 55:1–94.
- Pereira TM, Fernandes JC, Vieira AP, Basto AS. Tertiary syphilis. Int J Dermatol 2007;46:1192–5.
- Andrade, P; Mariano, A; & Figueiredo. Solitary frontal ulcer: A syphilitic gumma. Dermatology Online Journal. 2010; 16(8). Retrieved from: http://escholarship.org/uc/item/5gs4q6wz
- Salado-Rasmussen K. Syphilis and HIV co-infection. Epidemiology, treatment and molecular typing of Treponema pallidum. Dan Med J. 2015 Dec;62(12):B









1 thought on “Syphilis in the ED: Presentations, Diagnosis, and Management of the Great Imitator”
Pingback: Spot the Diagnosis! The Case of the Dutch Painter - CanadiEM