Authors: Elissabeth Hagler, MD (Emergency Medicine Resident, Carolinas Medical Center, Charlotte, NC); Kathryn T Kopec, DO (Emergency Medicine Attending; Medical Toxicologist, Carolinas Medical Center, Charlotte, NC) // Reviewed by: Cynthia Santos, MD (@Cynthia Santos, MD); Alex Koyfman, MD (@EMHighAK); and Brit Long, MD (@long_brit)

Overview:
Riot control agents are non-lethal chemical compounds that are used to incapacitate exposed individuals via intense irritation of the airway, respiratory tract, eyes, and skin. (1,2,3) These agents have been used as crowd control agents by law enforcement during protests, riots or civil unrest. In general, these compounds are crystallized solids with low vapor pressures that can be aerosolized and released into the air via droplets or small particles. These particles or droplets then cause local irritation to mucosal membranes and skin or the airways/pulmonary system through inhalation. (2,3)
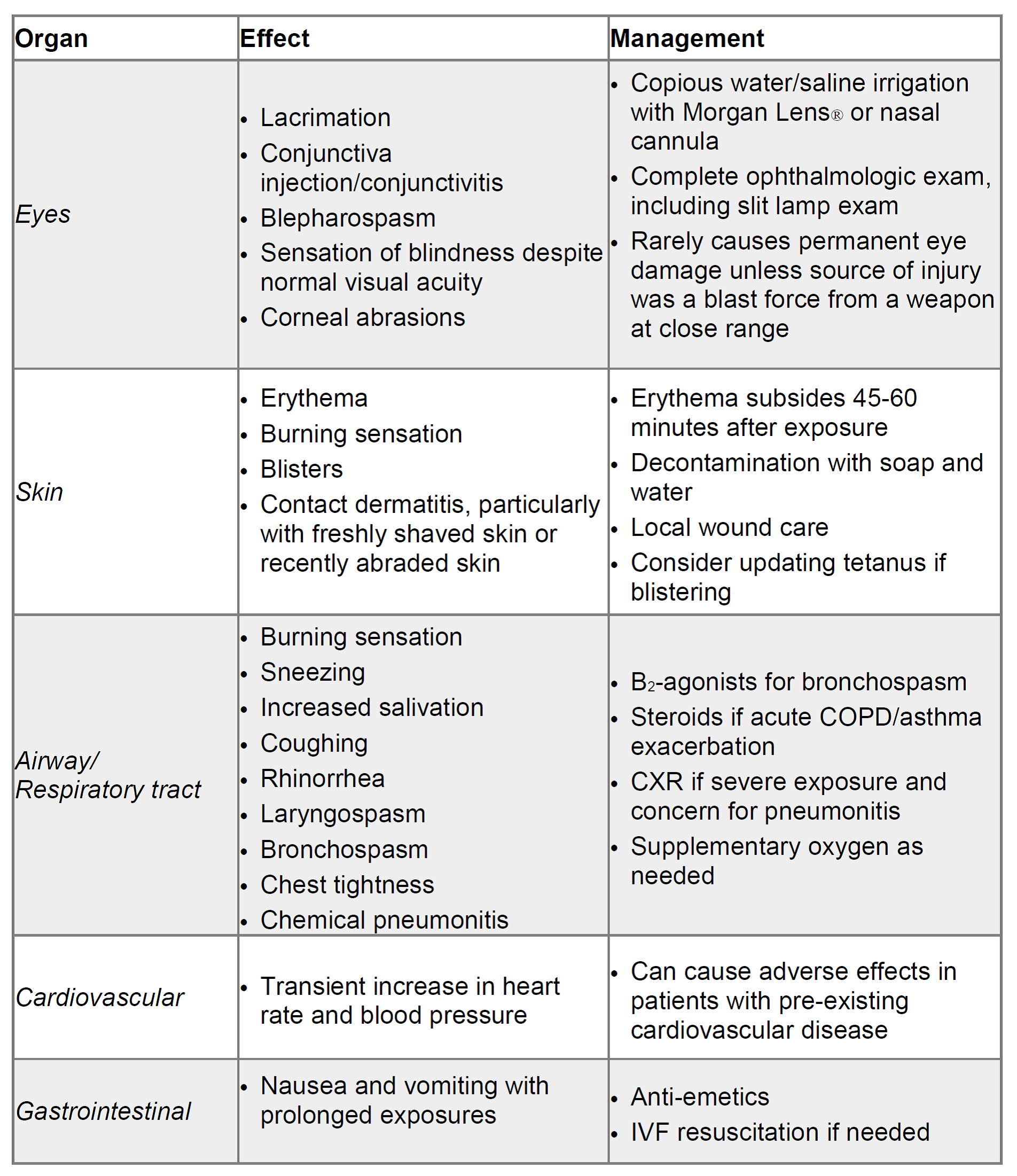
Clinical effects can occur within seconds and are generally transient, resolving within 30 minutes. (3) Prolonged exposure or exposure to a large dose, especially in a closed environment, has been associated with more severe effects, including burns, laryngospasm, and chemical pneumonitis. Death is rare. (2,3) Table 1 provides an overview of the clinical effects and management.
Specific Agents:
- 1-Chloroacetophenone (CN)
- O-Chlorobenzylidene malononitrile (CS)
- Dibenz [b,f]-1,4-oxazepine (CR)
- Oleoresin capsicum (OC)
- Diphenylaminearsine (DM)
- Chloropicrin (PS)
1-chloroacetophenone (CN), o-chlorobenzilidene malonitrile (CS), & Dibenz [b,f]-1,4-oxazepine (CR):
- 1-chloroacetophenone (CN) = Chemical Mace
- o-chlorobenzilidene malonitrile (CS) = Tear gas
- Mechanism of Action: Alkylating agents that act on nucleophilic sites on sulfhydryl-containing enzymes, transiently inactivating co-enzymes in the pyruvate decarboxylase system, causing tissue injury. (2)
- Pain is generally secondary to bradykinin release rather than tissue injury. (2)
- CS is a more potent lacrimatory than CN and is used more often than CN. (4)
- CN, which contains chlorine in its side chain, is associated with a higher risk of systemic toxicity, including pulmonary injury, second degree burns, and increased risk of death, particularly with high doses used in an enclosed space. (2,5)
- CR is another form of tear gas, but is not used in the United States. It is the most potent lacrimator but the least toxic of these agents. (5)
- Onset of Action: seconds to minutes.
- Duration: Symptoms usually resolve within 30 minutes.
- Initially exposed patients can have elevated blood pressures and irregular respirations. This is thought to be pain related not a pharmacologic effect. (2)
Oleoresin capsicum (Trans-8-methyl-N-vanillyl-6-noneamide) – (OC):
- Common name: Pepper Spray
- Naturally occurring lacrimator, extracted from cayenne pepper plants, Capsicum annum. (3)
- Mechanism of Action: Binds the capsaicin receptor, transient receptor potential vanilloid type-1 ion channel (TRPV1), a heat dependent nociceptor. (3)
- Binds to ion-channel receptors in the nervous system causing cell depolarization and release of substance P, a neuropeptide that acts as a mediator of pain transmission. (2)
- Onset of Action: seconds to minutes.
- Duration: Symptoms usually resolve within 30 minutes.
- Interestingly, people who regularly eat hot peppers or regularly use capsaicin in pain relieving ointments are less susceptible to the pain associated with pepper spray. (2)
Diphenylaminearsine adamsite (DM):
- Odorless, yellow compound that is an aromatic and alkyl derivative of arsenic trichloride.
- Mechanism of Action: may exhibit anticholinesterase activity, but the mechanism is not well understood. (6)
- Onset of Action: 2 – 4 minutes (2)
- Duration: Up to 12 hours (2)
- Because of its slower onset of action, absorption can occur before warning symptoms, and unaware individuals can incidentally absorb a larger dose. (2)
- Causes eye irritation and upper respiratory tract irritation similar to other irritants, but it causes more significant GI effects (abdominal cramps, nausea, vomiting, diarrhea), headaches, and gait instability. (2,6)
- It is no longer used as a riot control agent or chemical warfare agent internationally secondary to serious illness at high concentrations, including death from severe pulmonary damage. (5)
Chloropicrin (trichloronitromethane, or nitrochloroform (PS)):
- Fumigant and soil insecticide that acts as a lacrimator. (2)
- Mechanism of Action: not well understood, but it is thought to inhibit pyruvate dehydrogenase and succinate dehydrogenase. (7,8)
- Onset of action: seconds to minutes.
- Duration: Initial respiratory and ocular symptoms usually resolve within 30 minutes; however, GI symptoms may last for weeks and neurological symptoms can persist up to months after exposure. (9)
- Adverse effects: With moderate/severe exposures, symptoms include pulmonary edema, cyanosis, skin blisters, nausea, vomiting, diarrhea, dizziness, and headaches. (8,9)
- There have been cases of death secondary to pulmonary edema. (8)
- Previously used as a riot control agent and chemical warfare agent; but is no longer authorized for military use. Within the United States, it is authorized as a pesticide. (9)
Table 1: Clinical Effects & Management Overview (2,10,11):
Management Overview:
- There is no antidote for these agents.
- Mainstay of treatment is aimed at symptomatic relief and supportive care.
- Initial management involves decontamination by removing the patient’s clothing and copious irrigation of the affected area with soap and water to remove irritants.
- Ophthalmologic irrigation with saline/water. Ophthalmology follow up for any abnormalities on examination.
- Healthcare providers should wear PPE when caring for these patients to avoid secondary contamination and exposure.
- Limited evidence for decontamination with milk, aluminum hydroxide-magnesium hydroxide (Maalox®), lidocaine gel, or baby shampoo.
- No significant pain difference among these decontamination techniques versus water. (12)
- Consider projectile or blunt trauma injuries upon patient presentation and manage accordingly.
Safety Considerations to Provide for Patients Involved in Protests:
- Avoid wearing contacts if possible, glasses are preferred in the event of chemical exposure.
- Consider wearing goggles or a facemask for protection from chemical exposures.
- Long sleeve shirts/pants are encouraged to limit sun/chemical exposures.
- Bring a change of clothes; if exposed to riot control chemicals, remove initial clothing and place inside sealed plastic bag.
- Decontaminate chemical agents from your skin with large amounts of soap and water.
- Remember to stay hydrated and use sunscreen.
References:
- Schep, L., Slaughter, R., & McBride, D. (2013). Riot control agents: the tear gases CN, CS and OC—a medical review. Journal Of The Royal Army Medical Corps, 161(2), 94-99. https://doi.org/10.1136/jramc-2013-000165.
- US Army Medical Research Institute of Chemical Defense, Chemical Casualty Care Division. (2007). Medical Management of Chemical Casualties Handbook.4th Aberdeen Proving Ground, MD; 194-211. http://www.globalsecurity.org/wmd/library/policy/army/other/mmcc-hbk_4th-ed.pdf.
- Suchard, J.R. (2019) Chemical Weapons. Nelson LS, Howland M, Lewin NA, Smith, SW, Goldfrank LR, Hoffman, RS. Eds.’ Goldfrank’s Toxicologic Emergencies, 11th Ed. New York, NY: McGraw-Hill. 1741 – 1752.
- Blain, P.G. (2003). Tear gases and Irritant Incapacitants. Toxicol Rev., 22(2):103‐110. https://doi.org/10.2165/00139709-200322020-00005
- Malhotra, R.C., Kumar, P. (1987). Chemistry and Toxicity of Tear Gases. Defence Science J., 37(2): 281-296. https://doi.org/10.14429/dsj.37.5910
- Acute Exposure Guideline Levels: Chloroarsenicals. (2007) US. Environmental Protection Agency. Retrieved 10 June 2020, from https://www.epa.gov/sites/production/files/2014-09/documents/chloroarsenicals_interim_11_2007.v1.pdf.pdf
- Sparks, S.E., Quistad, G. B., & Casida, J. E. (1997). Chloropicrin: reactions with biological thiols and metabolism in mice. Res. Toxicol., 10: 1001–1007.
- Acute Exposure Guideline Levels: Chloropicrin. (2008). US. Environmental Protection Agency. Retrieved 10 June 2020, from https://www.epa.gov/sites/production/files/2014-08/documents/chloropicrin_interim_0.pdf
- Chloropicrin (PS): Lung Damaging Agent. (2011). National Institute for Occupational Safety and Health. Emergency Response Safety and Health Database. Retrieved 9 June 2020 from https://www.cdc.gov/NIOSH/ershdb/EmergencyResponseCard_29750034.html
- Fisher, W. (2020). com. Retrieved 4 June 2020, from https://www.procedurettes.com/eye-irrigation.
- The Morgan Lens for emergency eye irrigation. Youtube. (2020). Retrieved 4 June 2020, from https://www.youtube.com/watch?v=ig_W9tkH5Bw.
- Barry, J.D., Hennessy, R., & McManus, J. (2008). A Randomized Controlled Trial Comparing Treatment Regimens for Acute Pain for Topical Oleoresin Capsaicin (Pepper Spray) Exposure in Adult Volunteers. Prehospital Emergency Care, 12(4): 432-437. https://doi.org/10.1080/10903120802290786
- Danoff, J, Kim, H. (2020). UMEM Educational Pearls: Riot Control Agents. Retrieved 4 June 2020, from https://em.umaryland.edu/educational_pearls/3764/.