Author: Ian Bodford MD (EM Resident Physician, UTSW / Parkland Memorial Hospital) // Edited by: Alex Koyfman MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital) and Stephen Alerhand MD (EM Resident Physician, Icahn School of Medicine at Mount Sinai, @SAlerhand)
Imagine that you are working a clinical shift, and you see the chief complaint of “weakness” pop up on your track board. Instead of avoiding this type of patient like all the other providers are doing, you bite the bullet and assign yourself. You encounter a 35-year-old previously healthy woman who describes vague neurologic symptoms, including progressive numbness that started in both of her feet and has since slowly moved up her legs. It now involves the lower part of her torso up to her navel. She has also been having difficulty walking due to not being able to flex her ankles bilaterally. And she almost forgot to tell you that she has been retaining her urine, as well. Alarm bells start ringing in your head. On physical exam, you confirm her symptoms and also notice that her patellar and Achilles reflexes are absent bilaterally. Your brain travels back to the homunculus and your neurology rotation from your third year of medical school. But now what?
Clinical Features
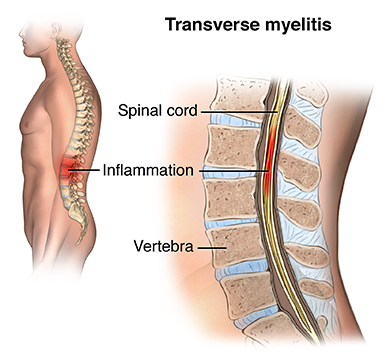
At its core, myelitis is a rare condition that involves inflammation of the spinal cord. The nerve fibers of the spinal cord are damaged and lose their myelin coating. This leads to a decrease in electrical conduction of the central nervous system and a myriad of neurologic issues. The term transverse means that the entire width of the spinal cord is involved. The onset is usually over hours to days with progression of symptoms over days to weeks. It can be acute or subacute. Any and all tracts of the cord can be involved, including motor, sensory, and/or autonomic fibers. Although the entire width of the spinal cord is involved, the symptoms do not necessarily have to be bilateral. Motor symptoms include progression of paraparesis. It is initially characterized by flaccidity, followed by spasticity. The upper extremities can also be involved. Almost all patients with transverse myelitis have a sensory level, usually in the cervical or thoracic area. The sensory symptoms are typically pain, dysesthesia, and paresthesias. The sensory symptoms typically begin in the feet and work their way up to the cervical level. If the autonomic system is involved, the patient may experience urinary and bowel incontinence, urinary retention, constipation, and dysfunction of the sexual organs. Patients can also have dysregulation of their temperature and blood pressure. Transverse myelitis can even lead to spinal shock. If the level is high enough, the patient may also experience difficulty breathing.
In 2002, the Transverse Myelitis Consortium Working Group created diagnostic criteria for transverse myelitis. These include motor, sensory, or autonomic dysfunction that is attributable to the spinal cord. The patient must also have signs and symptoms on both sides of the body, but the symptoms do not have to be symmetric. They must also have a defined sensory level. Inflammatory signs must be present. This can include pleocytosis or elevated IgG in the CSF or lesions on the MRI. Finally, the peak of the patient’s condition must be between 4 hours and 21 days after onset.
Causes
The causes of transverse myelitis are as vast as symptoms that it causes. Although it has several causes, it is deemed idiopathic around 30% of the time. Known causes are demyelinating conditions, viral, parasitic, bacterial, and fungal infections, autoimmune disorders, and paraneoplastic conditions. The most common demyelinating conditions are multiple sclerosis and neuromyelitis optica. The common bacterial infectious causes are Mycoplasma pneumoniae, Lyme disease, and cat scratch fever (Bartonella henselae). Viral infections include HSV, herpes zoster, CMV, EBV, and HIV. Schistosomiasis is the main parasitic infectious cause, and Cryptococcus is the main fungal cause. Lupus and Sjögren syndrome are the two main autoimmune etiologies. No matter the cause, the major theory is that it is an immune-mediated inflammation that causes the demyelination. For a full list of causes see this useful link to Discovery Medicine (http://www.discoverymedicine.com/Timothy-W-West/files/2013/10/discovery_medicine_no_88_timothy_w_west_table_1.png.jhtml?id=2).
Epidemiology
Transverse myelitis is considered to be a rare disorder. Estimates are up to 8 cases per million people per year. This is likely an underestimate due to misdiagnosis of other neurologic conditions. This relates to 1,400 new cases per year in the United States and roughly 34,000 chronically affected at a time. It is equal in men and women and does not seem to be hereditary. The bimodal peaks are in the teenage years and in patients’ 30s; however, it can happen at any point during a patient’s life.
Work-Up/Diagnosis
It is our job as emergency physicians to rule out all the life-threatening conditions. Several conditions can mimic transverse myelitis, including extrinsic compression of the cord, vascular disease of the spinal cord, and neoplastic conditions. The work-up for the myelitis can help rule out these conditions. This includes MRI with and without contrast of the brain and spinal cord. The lesions are gadolinium-enhanced on the MRI. MR brain should be normal unless there are multiple sclerosis lesions. A lumbar puncture is also essential to the work up. The CSF will show a pleocytosis, as well as a possible elevated IgG index. The CSF should also be sent for viral PCR and culture. An autoimmune screen can be sent as well, including complement levels, rheumatoid factor, ANA, etc.
 http://www.discoverymedicine.com/Timothy-W-West/2013/09/29/transverse-myelitis-a-review-of-the-presentation-diagnosis-and-initial-management/
http://www.discoverymedicine.com/Timothy-W-West/2013/09/29/transverse-myelitis-a-review-of-the-presentation-diagnosis-and-initial-management/
Management
Our job remains to first and foremost resuscitate the patient. If the involved dermatomal level is high enough and the patient is in respiratory distress, they may require intubation. Also, if the patient is in spinal shock, fluids and vasopressors might be needed. Always involve your neurologists and neurosurgeons as soon as the diagnosis is suspected, as they will be the ones to ultimately guide workup and treatment. Glucocorticoids are the mainstay of treatment; however, randomized controlled trials have never been performed. The preferred regimen is either methylprednisolone 1,000 mg daily or dexamethasone 200 mg daily for three to five days. Plasma exchange can also be considered for transverse myelitis. Keep in mind that it is more effective when used early after the onset of symptoms. Other therapies include immunomodulators, but the decision to initiate these medications are usually made by the admitting consultants.
Disposition/Prognosis
Most patients with severe enough disease will need to be admitted for further workup, usually to a neurologist or neurosurgeon. Around one third of patients fully recover, one third have some residual disability, and one third have severe lasting disability. The recovery usually begins around one to three months after symptom onset and can take years. Around one quarter to one third of patients will have a recurrent episode of transverse myelitis. A poorer prognosis is expected if a patient experiences rapid progression of symptoms, back pain, or spinal shock. All transverse myelitis patients will need long-term follow-up.
Pearls
- Neurologic symptoms include motor, sensory, and autonomic dysfunction. Sensory symptoms typically involve a dermatomal level.
- Causes are broad including demyelinating conditions, infections, and autoimmune disorders.
- Rule out life-threatening disorders, including compression of the cord. Order MRI brain and spinal cord with and without contrast. A lumbar puncture must also be obtained.
- Remember your ABCs! Resuscitate the patient first and foremost.
- Mainstay of therapy is IV steroids +/- plasmapheresis. Get consultants involved early.
- Admit the patient for a full workup.
- Up to one third of transverse myelitis patients will have a recurrence, so if it is in the chart, always keep it on the differential.
References / Further Reading
-Beh, et. al. “Differential Diagnosis of Acute Transverse Myelitis.” Discovery Medicine. Table 1. < http://www.discoverymedicine.com/Timothy-W-West/files/2013/10/discovery_medicine_no_88_timothy_w_west_table_1.png.jhtml?id=2>
-Krishnan, et. al. “Transverse Myelitis.” UpToDate. 19 May 2015. <www.uptodate.com>
-Nickson M.D., Chris. “Transverse Myelitis.” Life in the Fast Lane. 16 January 2014. <http://lifeinthefastlane.com/ccc/transverse-myelitis/>
-Swartz, et. al. “Transverse Myelitis.” WikEM. 27 January 2015. https://www.wikem.org/wiki/Transverse_myelitis
–http://www.ncbi.nlm.nih.gov/pubmed/16126136







1 thought on “Traversing Transverse Myelitis”
Pingback: How These 7 Succulent Doctors Educate Others On Transverse Myelitis