Author: Brian Sumner, MD (EM Resident PGY2, Mount Sinai Morningside-West) // Reviewed by: Anthony DeVivo, DO (EM-Critical Care Fellow, Icahn School of Medicine at Mount Sinai); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Case:
A 25-year-old male without any reported medical history presents to the emergency department with eye pain. He reports that 2 hours prior to arrival he was at his cousin’s house for Thanksgiving and per family tradition, there was a make-shift octagon in the back-yard for some friendly sparring. Despite the face being off-limits, one strike from his brother landed on his right eye. Since then he has had progressive pain and blurring of his vision in that eye. On initial examination, the eye is noted to be proptotic, and he is unable to move it in any of the cardinal directions. His vision is limited to only identifying light vs darkness. There are no obvious signs of globe rupture on initial assessment. Using an intra-ocular pressure meter you measure the intra-ocular pressure on the right to be 52 mm Hg. Given this initial presentation, you are concerned for a retrobulbar hematoma resulting in orbital compartment syndrome. What are your next steps? Is this a procedure you are planning to call in a subspecialist for? What if they are unavailable for emergent intervention?
Background:
A discussion about lateral orbital canthotomy/cantholysis must begin with a clear understanding of terminology. Though commonly used synonymously, canthotomy and cantholysis are two different entities. The former is the procedure wherein one exposes the canthal tendons and the latter is the procedure wherein one incises the tendons themselves. Next, it is important to understand the underlying disease process which results in their indication. Orbital compartment syndrome (OCS) is a condition wherein the pressure within the orbit is above normal levels (10-20 mm Hg). Conceptually, one can group the causes of increased pressure into traumatic and nontraumatic etiologies.1,2 Left untreated there is robust evidence that OCS can result in permanent loss of vision due to the compression of the neurovascular bundle of the eye.3 The increased pressure in the orbit compresses the optic nerve which can cause compressive trauma to the neurons as well as reduced blood supply to the retina as the central retinal artery runs within the nerve bundle.
Assault resulting in facial trauma is a most impetus for retrobulbar hemorrhage, but there are other causes, such as recent surgical intervention, anesthetic procedures, and Valsalva maneuvers in the setting of neoplastic processes within the orbit.1,2 Non-hemorrhagic causes, in contrast, are seen in cases of prolonged recumbent positioning (think long surgeries), facial and periocular burns, third spacing, and orbital emphysema in the setting of orbital trauma.1,2
Physical signs of increased intraocular pressure are often present such as proptosis and conjunctival injection. In other cases, however, having an appropriate index of suspicion and relying on patient symptomatology is key to identifying OCS. Completing a full eye exam including intraocular pressure, using a Snellen chart for visual acuity and fluorescein dye if indicated are all important. If there are no obvious external signs of obvious globe rupture, a thorough fluorescein dye exam to evaluate for subtle signs of rupture, such as the Seidel Sign, is prudent prior to evaluating IOP with a tonometer or other devices.
Normal intraocular pressures are between 10 and 20 mmHg.4 When pressures begin approaching 40 mm Hg the provider should be concerned for ongoing or impending injury to the structures of the eye.1,3,5 In some cases, increased IOP occurs over longer periods of time, such as open angle glaucoma and patients can tolerate higher than normal pressure levels. However, in the setting of acute angle closure glaucoma or a retrobulbar hemorrhage, the rapid rise in pressures, as discussed above, puts the neurovascular bundle of the eye in danger of permanent damage.
Absolute Indications (when retrobulbar hemorrhage is suspected/confirmed):5
- Acute vision loss
- Intraocular pressure >40mmHg
- Persistent proptosis that cannot be reduced
Contraindications:5
- Globe rupture
- Suspected globe rupture: hyphema, irregular shape of pupil, exposed uveal tissue, marked reduction in extraocular range of motion
Anatomy:1-2
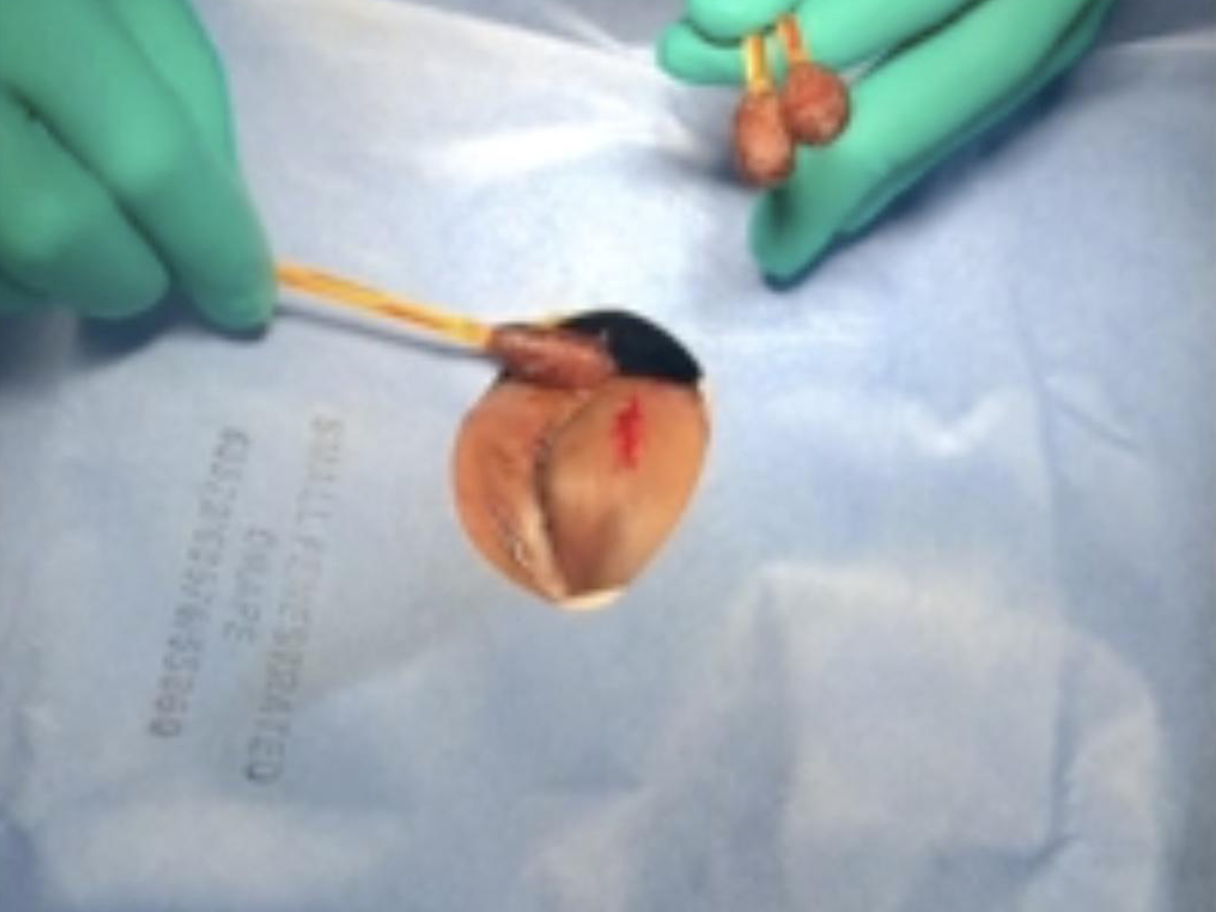
Both the medial and lateral corners of the eye are called a ‘canthus’. The canthus on either side consists of the terminal portions of the upper and lower eyelid. When performing a canthotomy, the inferior limb of the lateral canthal tendon is the first target.
While difficult to find clear data on the reasoning of targeting the inferior limb of the lateral canthus, anatomically it likely provides more latitude for the globe to protrude, permitting more ability to relieve pressure than the superior limb alone.

Procedure:1,3,5,7
- First and foremost, this is an emergent procedure. While ophthalmology should be called, it should not delay management – they can be called after the procedure is completed.
- Explain the procedure to the patient and why it is necessary. If time permits, obtain formal written consent.
- Even the most stoic of patients can become unnerved with the concept of this procedure – consider anxiolysis with a benzodiazepine or other anxiolytic agents, if clinically appropriate.
- Keep them supine with their head turned away from the affected side.
- Clean the external aspect of the canthus taking care to not get the cleaning solution in the eye.
- Clean the soft tissue around the eye to ensure a wide sterile field.
- Drape the area and don sterile gloves.
- Consider placing a morgan lens to protect the aperture of the eye throughout the procedure (utilize ophthalmic anesthesia for this).
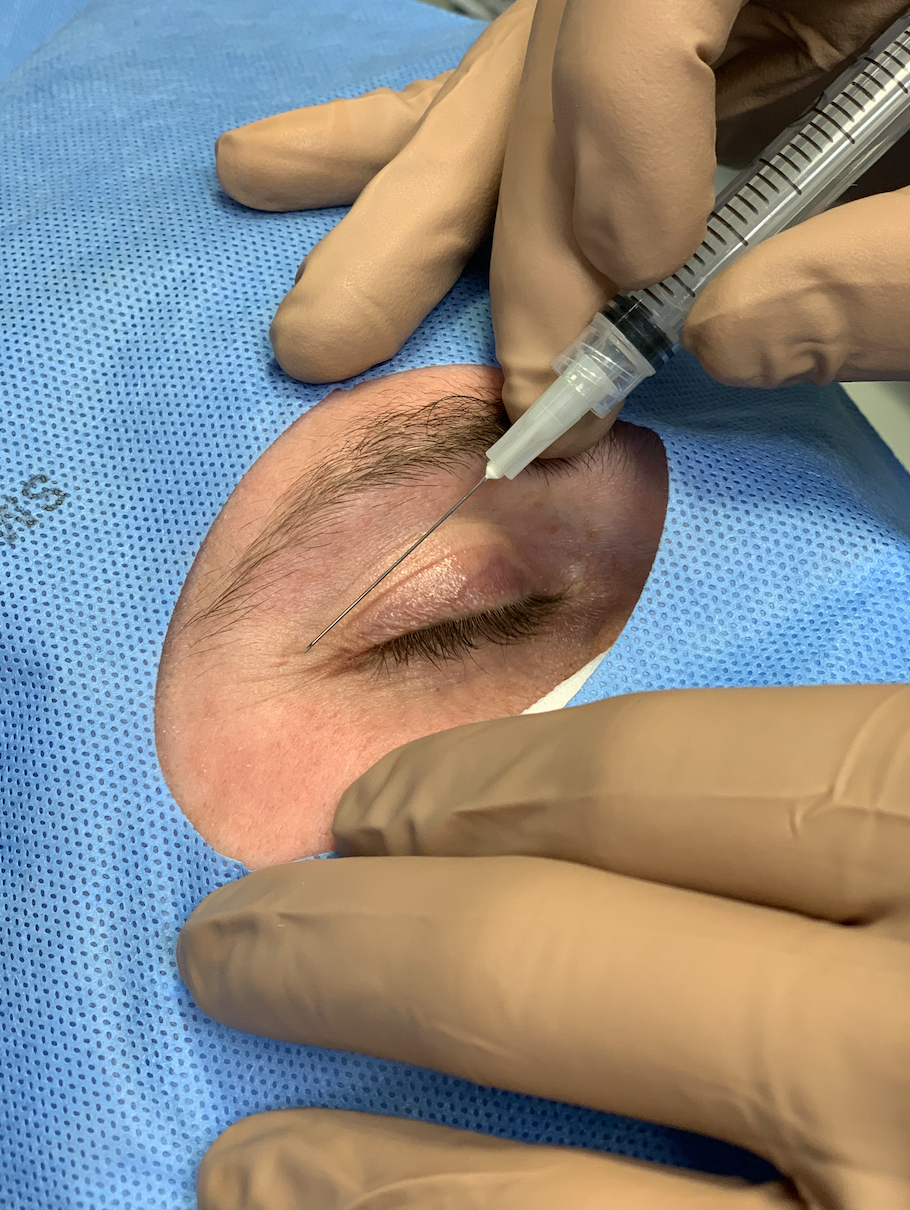
- Inject 2-3cc lidocaine with epinephrine into the canthus. For this step and all to come, point any instruments away from the eye itself, toward the lateral edge and the orbital rim.
- Using a hemostat, clamp the lateral canthus and let stand for 1 minute.
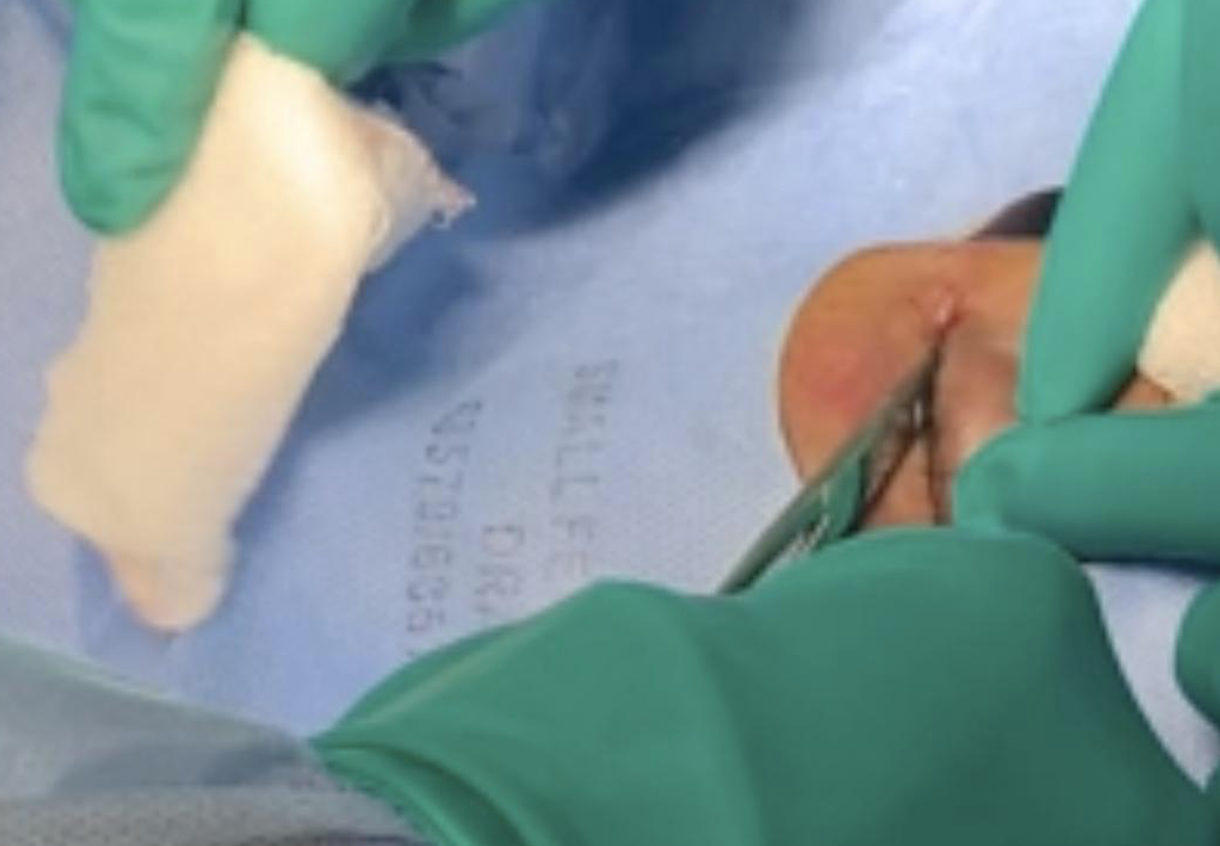
- Canthotomy: Using iris scissors, or other sterile scissors available, cut the canthus laterally by 1-2 cm.
- Cantholysis: Despite hemostat clamping, bleeding may obstruct the visualization of the field and tendon; the clinician can strum the tissue and the tendon should feel like a guitar string. Once the tendon is identified, make the cut
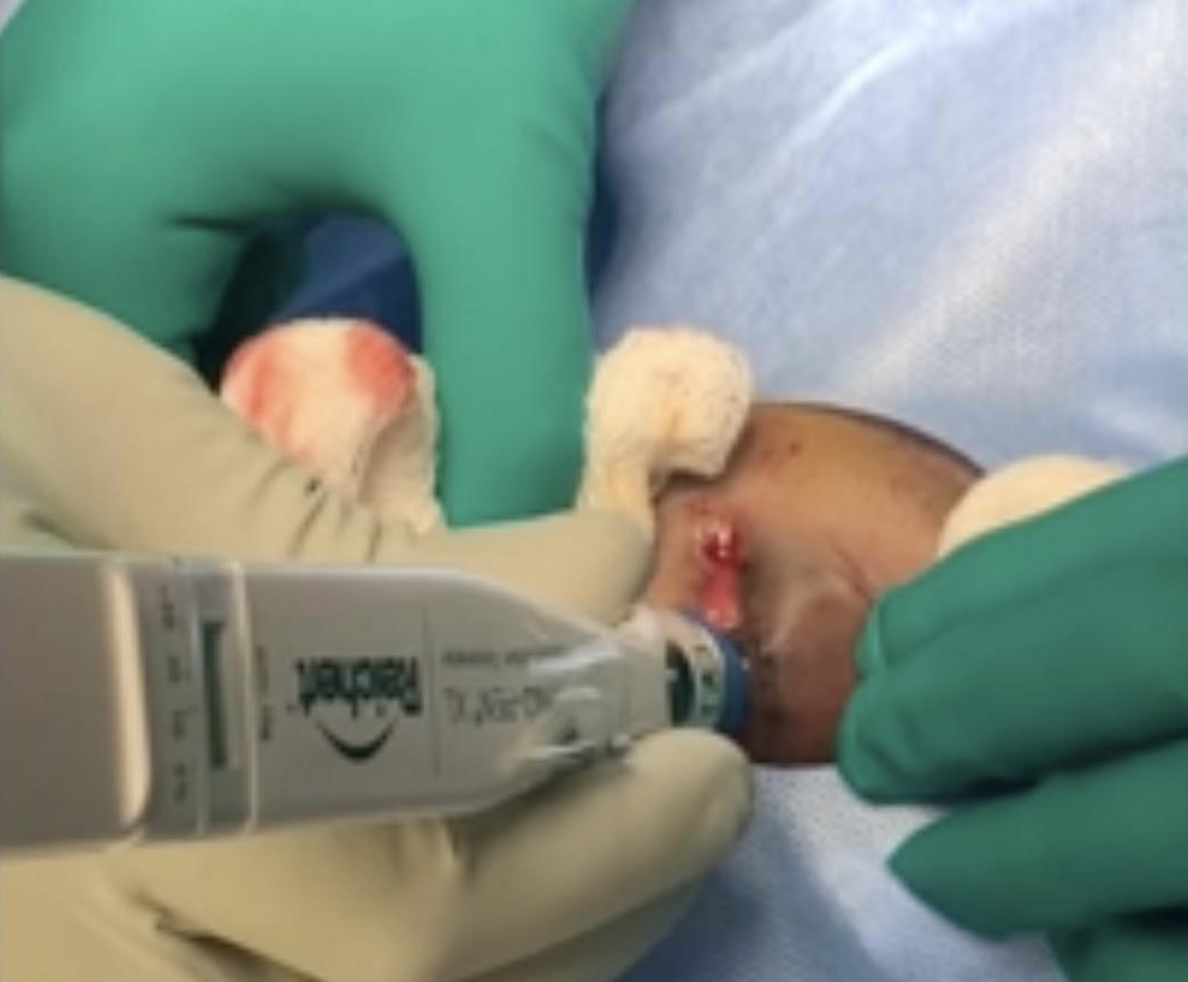
- Recheck ocular pressures – If still above 40mmHg, you may need to proceed with cutting the superior tendon of the canthus.

Post-procedure
- Reevaluate the patient for any signs of globe injury during the procedure.
- Inform the patient of the spontaneous healing process, but also let them know the likelihood of scarring.
- Ensure ophthalmology has been consulted.
Complications
- Bleeding at the site of incision
- Injury to the globe and aperture of the eye
- Pain at the operative site
- Post-procedure infection/adhesions
- Interruption of the lacrimal gland/artery
- Injury to the lateral rectus muscle
- Injury to the levator aponeurosis resulting in ptosis
Rapid Procedure Review
- Premedicate with anxiolytic medications.
- Anesthetize with lidocaine + epinephrine; direct needle and ALL equipment throughout the procedure away from the eye towards lateral margin.
- Clamp the canthus to encourage hemostasis.
- Canthotomy and cantholysis – the tendon should feel like a guitar string if it cannot be visualized directly.
- Recheck pressures – If no drop, ensure complete incision of the inferior tendon. Proceed with incision of superior tendon if pressure does not reduce.
- Call ophthalmology – definitive care must be decided on by your trusty consultants.
References/Further Reading:
- Desai NM, Shah SU. Lateral Orbital Canthotomy. 2020 Jul 31. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan. PMID: 32491408.
- Rowh AD, Ufberg JW, Chan TC, Vilke GM, Harrigan RA. Lateral canthotomy and cantholysis: emergency management of orbital compartment syndrome. J Emerg Med. 2015 Mar;48(3):325-30. doi: 10.1016/j.jemermed.2014.11.002. Epub 2014 Dec 16. PMID: 25524455.
- Hayreh SS, Kolder HE, Weingeist TA. Central retinal artery occlusion and retinal tolerance time. Ophthalmology. 1980 Jan;87(1):75-8. doi: 10.1016/s0161-6420(80)35283-4. PMID: 6769079.
- Walker RA, Adhikari S. Eye Emergencies. In: Tintinalli JE, Ma O, Yealy DM, Meckler GD, Stapczynski J, Cline DM, Thomas SH. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 9e. McGraw-Hill; Accessed January 05, 2021. https://accessemergencymedicine-mhmedical-com.eresources.mssm.edu/content.aspx?bookid=2353§ionid=222404436
- Mahon BM, Desai BK. Lateral Canthotomy.Atlas of Emergency Medicine Procedures. New York, NY: Springer New York; 2016. p. 305-8.
- McInnes G, Howes DW. Lateral canthotomy and cantholysis: a simple, vision-saving procedure. Cjem. 2002;4(1):49-52.
- Lateral Canthotomy. EM:RAP. https://www.emrap.org/hd/playlist/smartcardsPL/chapter/lateral/lateral