Author: Jamie Santistevan, MD (@jamie_rae_EMDoc, Senior EM Resident Physician, University of Wisconsin) // Edited by: Alex Koyfman, MD (EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital, @EMHighAK) & Justin Bright, MD (EM Attending, Henry Ford Hospital, @JBright2021)
Introduction
Look at these two snakes: One is a deadly coral snake, the other a friendly harmless mimic. I learned to tell them apart in the 5th grade using this rhyme: “Red next to black, you’re alright Jack. Red next to yellow, you’re a dead fellow.”

You may be wondering what reptiles have to do with ECGs. Well, welcome to the third blog post in a series on subtle ECG findings in ACS. This post about mimics: benign early repolarization (BER) and the anterior STEMI. Each of these can mimic the other. The problem is that one of these diagnoses is deadly and the other is a normal variant. Today I am going to discuss the key differences between benign ST-segment elevation, also known as J-point elevation or benign early repolarization (BER), and the subtle ST-segment elevation seen occasionally in acute LAD occlusion.
In the previous post concerning hyperacute T-waves, I said that the STEMI criteria are poorly sensitive for diagnosing vessel occlusion. This means that some patients with acute coronary occlusion may not meet criteria for STEMI. In fact, about one quarter of NSTEMI patients have complete vessel occlusion on angiogram [1]. Wang and colleagues studied 1,957 NSTEMI patients and compared baseline characteristics, ECG findings, and long term outcomes, between patients with and without occluded arteries. The group of researchers found that 27% had an occluded culprit artery and those patients had larger infarcts and higher six-month mortality compared to NSTEMI patients without an occluded artery [1].
Remember, the STEMI criteria are arbitrary, based solely on the size (in millimeters) of ST-segment elevation and are only guidelines for reperfusion therapy. We typically use the term “STEMI” to mean complete coronary artery occlusion. “NSTEMI” traditionally means that the patient has had an MI (elevated troponin), but without complete coronary artery occlusion. However, as Wang and colleagues data shows us, some patients have an occluded vessel but do not develop diagnostic ST-segment elevation. These patients, therefore, have a “STEMI-equivalent”, or may be described as having a “subtle-STEMI”.
The subtle STEMI, as defined by 0.1-1mm of ST-segment elevation, occurs in about 18% of patients with an occluded coronary artery [2]. These patients have smaller infarcts compared to patients with obvious STEMI, however subtle STEMI patients are more likely to experience greater delays to reperfusion [2, 3]. Interestingly, subtle STEMI patients do not have better outcomes than those with obvious STEMI [2]. Marti and colleagues studied 504 patients who were taken to the cardiac cath lab for suspected coronary artery occlusion. Patients with subtle and obvious ST-elevation MI had similar rates of pre-interventional TIMI flow of 0/1 (86% of the patients in the subtle STE group and in 87% of the patients in the marked STE group). Among patients with coronary artery occlusion, 18.3% did not have any lead with at least 1 full millimeter of ST-segment elevation. Subtle STEMI patients were more likely to have multi-vessel disease and experienced greater delays to reperfusion. Comparing the subtle-STEMI patients to those with obvious STEMI, the authors found that the rate of reinfarction or death were similar between the two groups (10.0% vs 12.6%, P = .467) [2].
Therefore, recognizing the subtle findings of coronary artery occlusion and taking the next steps to rapidly evaluate for ACS may allow us to recognize these subtle-STEMI patients early and provide timely revascularization. Anterior MI carries the worst prognosis compared to other anatomic areas; it has the highest mortality and rates of complications [4,5]. Early anterior MI can have less than 1mm of ST-segment elevation and can mimic benign early repolarization. So today I will discuss the findings that differentiate BER and LAD occlusion by exploring 5 different ECG features.
Benign early repolarization
The ST segment represents the period between ventricular depolarization and repolarization. In a normal ECG the ST-segment is isoelectric, meaning neither elevated nor depressed relative to the TP-segment [6]. Benign early repolarization is the most common normal ECG variant. It has been reported in both men and women of all age groups and various ethnicities [6] and occurs in about 1% of the population [7] with higher occurrence in black males 20-40 years old [8].
ECG characteristics that are more likely to be seen in BER include:
- ST elevation at the J-point with upward concavity
- Notching of the J-point
- Diffuse ST elevation (typically highest in V3-4)
- Concordant, prominent T-waves with large amplitudes
- Normal R-wave progression
- Relative stability from one ECG to the next
Here is a classic example of benign early repolarization:

The ST-segment elevation is most pronounced in V2-4. There is upsloping ST elevation. The T-waves are asymmetric: they have a concave upslope and a steep downslope. There is good R-wave progression across the precordium with a very tall R-wave in V4. Also, notice the absence of certain features: there is no ST-segment depression and there are no anterior Q-waves.
Acute LAD occlusion will also manifest as anterior ST-segment elevation, often maximal in V2-3. So how does anterior MI differ from BER? To answer this question we are going to discuss 5 ECG features:
- ST-segment morphology
- Reciprocal changes
- Poor R-wave progression
- Anterior Q-waves
- Terminal QRS distortion
ST segment morphology
It is often taught that up-sloping ST segments are benign. However, you should not rely on ST-segment morphology alone to rule out ACS. While convex (“tombstone”) ST-segment elevation is highly specific for AMI [9], it is less common than either straight or upsloping (concave) elevation in acute anterior MI [2, 10]. Straight ST-segment elevation is the most common ST morphology in anterior MI [11]. However, in one retrospective review of patients with LAD occlusion on angiogram, 43% (16/37) had concave morphology [9].
Reciprocal changes
Reciprocal change is ST-segment depression in the leads opposite of the ST-elevation. Occasionally reciprocal ST-segment depression is the first (and rarely, the only) ECG findings in AMI. It is important to look specifically for ST-segment depression because it may be subtle. The absence of ST depression does not rule out AMI, but its presence does make the ST-elevation more specific for coronary artery occlusion [4, 12]. And, the presence of ST depression correlates with a larger infarct area at risk and higher mortality, independent of ST elevation [13].
Reciprocal ST depression can occur in either anterior or lateral MI. An anterior MI will manifest ST-segment depression in the inferior leads when there is a more proximal LAD occlusion (the first diagonal branch is occluded) [4, 14]. If you see ST-depression leads II, III, or aVF, you should carefully scrutinize the ECG for subtle anterior (V1-4) or high lateral (I, aVL) ST-segment elevation or hyperacute T-waves. The bottom line is that in the presence of reciprocal ST-segment depression in the inferior leads, you should be very cautious about diagnosing benign early repolarization.
Poor R-wave progression
Normally, the height of the R-wave increases gradually across the precordial leads to the point where the R-wave is bigger than the S-wave at V3 or V4 and eventually there is only a very small S-wave remaining in V6. One commonly accepted definition of poor R-wave progression is R-wave height ≤ 3 mm in V3. Causes of poor R-wave progression include left ventricular hypertrophy (LVH), inaccurate lead placement, old anterior infarct and acute anterior MI. Remember that BER should always have good R-wave progression.
Here is normal R-wave progression in BER:

Here is a patient who has poor R-wave progression secondary to old anterior infarct:

Notice there are QS-waves in V1-3 and only a very small R-wave in V4.
Q-waves
Pathologic Q-waves result from the absence of electrical myocardial activity secondary to ischemic cell death. The infarcted area of myocardium does not conduct electricity, so the deflection on the ECG paper is negative (downward). Q-waves are classically taught to develop in MI after several hours to days [10]. However, Q-waves can form early in acute MI, as early as less than 1 hour [4, 15].
Pathologic Q-waves in the anterior leads are defined as Q-waves in leads V2–V3 ≥ 20ms [16]. A general rule of thumb is that in acute MI the most common type of Q-wave is a QR-wave. QS-waves may develop later in anterior MI, so they may be suggestive of a subacute presentation, or they can be there from a previous MI. However, when anterior QS-wave are paired with very large, wide and towering T-wave (hyperacute T-waves), this may be a sign of acute LAD occlusion [17].
Here are QR-waves accompanied by ST-segment elevation:
Contrast that to these QS-waves paired with a hyperacute T-wave:
In summary, in the presence of anterior Q-waves, anterior ST-segment elevation cannot be considered benign early repolarization. The ST segment elevation may be due to:
- Acute anterior MI
- Subacute anterior MI
- Old anterior infarct with persistent ST-segment elevation (possibly due to LV aneurysm formation)
This is an example of a patient with LAD occlusion who’s ECG demonstrates all 4 ECG criteria discussed here:

This ECG shows upsloping anterior ST-segment elevation. Although this may be confused for normal variant ST-elevation, there are four concerning features make this ECG diagnostic for LAD occlusion. There is a QS-wave in V1-V2 paired with hyperacute anterior T-waves. There is reciprocal ST-segment depression in lead III and poor R wave progression across the precordium.
Dr. Smith’s ECG formula
I would like to make special mention of a mathematical formula developed specifically to differentiate BER and acute LAD occlusion [18]. Smith and colleagues conducted a retrospective study comparing patients with subtle anterior STEMI to those with proven early repolarization. They found that several ECG measurements were independently predictive of STEMI versus BER:
- Greater height of ST-segment elevation (measured at 60ms after the J point)
- Longer QTc interval
- Lower R-wave amplitude
- Higher T-wave/R-wave amplitude ratio in leads V2-V4
Using logistic regression, they derived and validated an ECG-based formula using the first three measurements as follows:
[1.196 x ST-segment elevation 60 ms after the J point in lead V3 in mm]+[0.059 x QTc in ms]-[0.326 x R-wave amplitude in lead V4 in mm]
A value of >23.4 was found to predict STEMI, and </= 23.4 predicted early repolarization with an overall sensitivity and specificity of 86%, 91% respectively [18]. A calculator for this formula and further explanation can be found at http://hqmeded-ecg.blogspot.com/2013/06/here-is-link-to-full-text-of-article-in.html.
Before applying the formula there are some things you must consider:
The equation only applies when trying to distinguish between subtle LAD occlusion and early repolarization. The rule does not apply if there is left ventricular hypertrophy (LVH). Most importantly, if there are other findings on the ECG that support the diagnosis of LAD occlusion such as inferior ST depression, ST-segment convexity, terminal QRS distortion, or Q-waves, then the equation does NOT apply because these kinds of cases were excluded from the study as representing an obvious STEMI.
Terminal QRS distortion
Terminal QRS distortion is defined as emergence of the J point ≥50% of the R wave in leads with QR-wave, or disappearance of the S wave in leads with an RS-wave. [19] In acute MI, terminal QRS distortion predicts greater size of infarct and higher mortality [20].
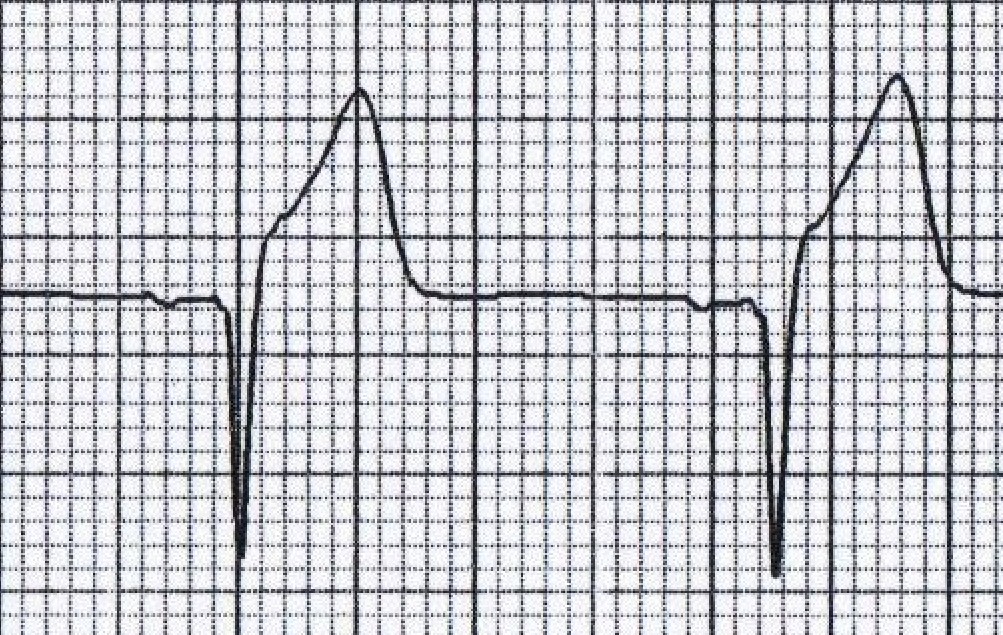
Here are two examples of terminal QRS distortion:
This is the more obvious, with emergence of the J point ≥50% of the R wave in leads with QR-wave

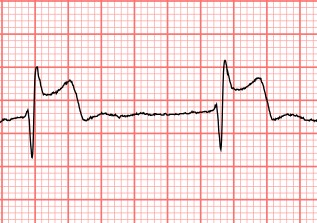
This is more subtle terminal QRS distortion. Notice how the S-wave does not extend below the isoelectric line.
Summary:
As always, it is important to correlate the ECG findings with the clinical picture. You should be incredibly cautious diagnosing BER in a patient over 55 years old, or anyone with concerning symptoms or history. If the ECG is subtle and you are concerned about ACS, get serial ECGs (every 15 minutes) and use adjunctive information such as comparison to an old ECG or obtain echocardiogram. Remember that ACS is a dynamic process and can present subtly. The ECG is a cheap, noninvasive and fast tool, which can provide valuable diagnostic and prognostic information. Missing subtle presentation of ACS can have dire consequences for our patients who may be inappropriately discharged or experience significant delays to reperfusion. As emergency physicians, it is our job to own the ECG and we should strive for mastery to recognize even the subtlest cases.
TAKE-AWAY POINTS
- Anterior STEMI can be subtle and present with less than 1mm ST-segment elevation anteriorly and can mimic benign early repolarization.
- Do not rely on ST-segment morphology alone to rule out AMI because about 40% of patients with anterior MI have upsloping (concave) ST-segment elevation.
- Be very cautious about diagnosing BER when there is poor R-wave progression, anterior Q-waves, inferior ST depression, or terminal QRS-distortion.
- Be cautious diagnosing BER in patients older than 55 years old or anyone with concerning symptoms.
- When concerned for subtle STEMI, use adjunctive information such as serial ECGs, comparison to prior ECGs, and/or echocardiogram.
References / Further Reading
- Wang TY et al. Incidence, distribution, and prognostic impact of occluded culprit arteries among patients with non-ST-elevation acute coronary syndromes undergoing diagnostic angiography. Am Heart J. Apr 2009;157(4):716-23.
- Martí D et al. Incidence, angiographic features and outcomes of patients presenting with subtle ST-elevation myocardial infarction. Am Heart J. Dec 2014;168(6):884-90.
- Sharkey SW et al. Impact of the electrocardiogram on the delivery of thrombolytic therapy for acute myocardial infarction. Am J Cardiol. Mar 1994;15;73(8):550-3.
- Smith SW. The ECG in Acute MI: An evidence-based manual of reperfusion therapy. Lippincott Williams & Wilkins 2002.
- Lee KL et al. Predictors of 30-day mortality in the era of reperfusion for acute myocardial infarction. Results from an international trial of 41,021 patients. GUSTO-I Investigators. Circulation. 1995 Mar;91(6):1659-68.
- Somers, MP et al. The prominent T wave: electrocardiographic differential diagnosis. Am J Emerg Med. 2002 May;20(3):243-51.
- Mehta MC, Jain AC: Early repolarization on scalar electrocardiogram. Am J Med Sci 1995;309:305-311
- Thomas J, Harris E, Lassiter G: Observations on the T wave and S-T segment changes in the precordial electrocardiogram of 320 young Negro adults. Am J Cardiol 1960;5:368-374
- Smith SW. Upwardly concave ST segment morphology is common in acute left anterior descending coronary occlusion. J Emerg Med. Jul 2006;31(1):69-77
- Nable, JV and Brady, W. The evolution of electrocardiographic changes in ST-segment elevation myocardial infarction. Am J Emerg Med. 2009 Jul;27(6):734-46.
- Kosuge et al. Value of ST-segment elevation pattern in predicting infarct size and left ventricular function at discharge in patients with reperfused acute anterior myocardial infarction. Am Heart J. 1999 Mar;137(3):522-7.
- Brady WJ et al. Reciprocal ST segment depression: impact on the electrocardiographic diagnosis of ST segment elevation acute myocardial infarction. Am J Emerg Med. 2002 Jan;20(1):35-8.
- Willems JL et al. Circulation. Significance of initial ST segment elevation and depression for the management of thrombolytic therapy in acute myocardial infarction. European Cooperative Study Group for Recombinant Tissue-Type Plasminogen Activator. 1990 Oct;82(4):1147-58.
- Engelen DJ et al. Value of the electrocardiogram in localizing the occlusion site in the left anterior descending coronary artery in acute anterior myocardial infarction. J Am Coll Cardiol. 1999 Aug;34(2):389-95.
- Raitt, MH, et al. Appearance of abnormal Q waves early in the course of acute myocardial infarction: implications for efficacy of thrombolytic therapy. J Am Coll Cardiol. 1995 Apr;25(5):1084-8.
- Pathologic Q waves. ECGPedia. Web. 12 Dec 2015. http://en.ecgpedia.org/wiki/Pathologic_Q_Waveshttp://en.ecgpedia.org/wiki/Pathologic_Q_Waves
- Left ventricular Aneurysm Morphology Distorted by Right Bundle Branch Block, Mimicking Acute STEMI with RBBB. http://hqmeded-ecg.blogspot.com/2012/01/left-ventricular-aneurysm-morphology.html
- Smith S et al. Electrocardiographic differentiation of early repolarization from subtle anterior ST-segment elevation myocardial infarction. Ann Emerg Med. Jul 2012;60(1):45-56
- Birnbaum Y, et al. Distortion of the terminal portion of the QRS on the admission electrocardiogram in acute myocardial infarction and correlation with infarct size and long-term prognosis (Thrombolysis in Myocardial Infarction 4 Trial).Am J Cardiol. 1996 Aug 15;78(4):396-403.
- Mulay DV, Mukhedkar SM. Prognostic significance of the distortion of terminal portion of QRS complex on admission electrocardiogram in ST segment elevation myocardial infarction. Indian Heart J. 2013 Dec;65(6):671-7.
- Flickr photo. Web. 12. Dec 2015. https://www.flickr.com/photos/paulmarcellini/5598836030
- “Anterior Myocardial Infarction”. Life in the Fast Lane Medical Blog. Web. 12 Dec 2015. http://lifeinthefastlane.com/ecg-library/anterior-stemi/
- ”Conclusin to snapshot case: 44 year old male-chest tightness”. EMS 12 Lead Blog, 2014. Web. 12 Dec 2015. http://www.ems12lead.com/2014/02/10/conclusion-to-snapshot-case-44-year-old-male-chest-tightness/








2 thoughts on “Subtle ECG Findings in ACS: Part III Benign Early Repolarization vs. Anterior STEMI”
Completely unrelated to the post but in relation to the first paragraph. There are multiple coral snake patterns and unless you are a trained herpetologist it would be advisable to stay away from anything that looks like one. The rhyme, unfortunately has been debunked and does not hold true any longer.
Pingback: Länkar v8 | Internmedicin