Author: Abdullah Bakhsh, MBBS (EM Resident Physician, Emory Emergency Medicine) // Editor: Justin Bright, MD (@JBright2021)
Definition:
The ACEP Crowding Resources Task Force adopted the following definition of ED crowding: “A situation in which the identified need for emergency services outstrips available resources in the ED. This situation occurs in hospital EDs when there are more patients than staffed ED treatment beds and wait times exceed a reasonable period [80]. Crowding involves an inability to appropriately triage patients, with large numbers of patients accumulating in the ED waiting area of any triage assessment category.” This crowding causes patients to be evaluated and monitored in less than ideal settings – such as in the ED waiting room or hallways – as they await an ED treatment bed.
Clinical Scenario:
A 62 year-old male presents to the emergency department (ED) with low back pain after a mechanical fall as he slipped on a puddle of water. After a 14 hour wait, he finally gets moved to an exam room. Upon examination you notice lumbar spine tenderness with inability to flex his left thigh. A CT of his lumbar spine demonstrates a L2 vertebral body fracture with retropulsion. The patient has to be transferred to another hospital due to unavailability of neurosurgical services. Delays in care were mostly due to boarding patients and lack of staff.
Dangers of ED Crowding:
Emergency department crowding threatens quality and access to health care [1]. Delays to analgesia, antibiotic therapy, thrombolysis, or percutaneous coronary intervention as a result of ED crowding are all well described [2-5]. Intensive Care Unit (ICU) patients boarding in the ED subjected to a delay of more than 6 hours in transfer to an ICU had increased hospital length of stay (7 versus 6 days), and higher mortality rates (10.7% versus 8.4%) [6]. Crowding also impairs dignity, privacy, and completeness of care. Errors are increased with ED crowding. Many of these are errors of omission rather than errors of commission since the emergency staff must simultaneously care for inpatients and focus on the new emergencies coming in the door [7,8].
What Causes ED Crowding:
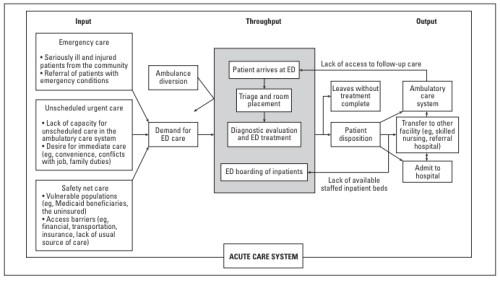
The number of patients in the emergency department at any given time is a function of three variables: input, throughput, and output. This can be explained by Asplin’s model of acute care (figure 1). Before interventions are instituted, it is critical to identify what the main causes of crowding are in an individual emergency department. Researchers initially focused on input factors such as use of the ED for non-emergent complaints. Their data ultimately showed that their reasons for doing so included insufficient or untimely access to primary care [23,24]. More recent research, however, strongly suggests that these input factors are not the root cause of the problem [25,26,27,28]. Inadequate staffing is a commonly studied throughput factor that may cause crowding. Lower staffing levels of physicians and triage nurses predisposed patients to wait longer for care [34]. The use of ancillary services, including computed tomographic (CT) scanning and other procedures, prolonged the ED length of stay among surgical critical care patients [36]. The most common cause of ED crowding is thought to be access block (output). Patients experiencing access block, defined by boarding time exceeding 8 hours, was associated with increased diversion, waiting times, and occupancy level in an Australian ED [35]. Length of stay in one ED increased substantially when the hospital occupancy levels exceeded 90% [37].
EMERGENCY DEPARTMENT INTERVENTIONS
Hallways:
As crowding increased, the inflow of patients exceeded outflow for extended hours each day, resulting in the need to place patients somewhere [9]. For a growing number of EDs the solution was to move both stable and semi-stable patients from licensed ED beds into adjacent ED hallways, thus freeing up the official ED bed for another patient [10]. If the chief reason for overcrowding is “exit block,” then simply building a larger ED to increase capacitance may not solve the problem [11,12]. Emergency and inpatient physicians at the Stony Brook University Hospital in New York collaborated and developed a program whereby admitted hallway patients are transferred out of the ED to inpatient hallways [13]. Patients receive more attention in a quieter and more private environment. This transfer of patient care has been shown to be safe, and patients prefer being boarded in inpatient hallways [14-16]. In some academic centers “door to floor” time exceeds 21 hours for 90% of admitted patients. It would make sense then to move admitted patients from ED hallways up to the hallways of the inpatient areas when the hospital is full. Such a proposal is not novel and, in fact, is used extensively on the East Coast [17].
INCREASING EMERGENCY DEPARTMENT PERSONNEL
One study concluded that the addition of a physician during a busy shift decreased the length of stay from 176 minutes to 141 minutes for patients discharged after evaluation in the emergency department [18]. One hospital activated reserve personnel as needed during the viral epidemic season, reducing the waiting time by 15 minutes and the rate of patients leaving without being seen by 37%.[20]. For each additional triage nurse per ED patient, waiting times for all other patients were reduced by an average of 28.8 minutes and for each additional physician per ED patient waiting, waiting times were reduced by 82 minutes [34].
TRIAGE BASED CARE PROTOCOL AND NURSE INITIATED WORKUPS
In the literature, advanced triage protocols have been reported to decrease patient length of stay,[38,39] decrease the time to pain treatment,[40,41] increase patient comfort,[40,42] decrease time to antibiotics in patients admitted with pneumonia,[43] decrease delays in performing ECGs and administering thrombolytic agents for myocardial infarction,[44] and decrease costs associated with patients requiring one-to-one monitoring[45]. It has also been shown to improve throughput and employee satisfaction, and decrease medical errors. Training nursing staff to order X-rays at triage is helpful and cuts the patient’s stay by around 20 minutes [21]. In another study, triage nurse initiated radiography using OAR leads to a statistically significant decrease of 20 minutes in the median ED LOS at a tertiary care center [33].
IMPLEMENTING ED FAST TRACK
Establishment of an effective fast track service line decreased patient wait times,[47-51] increased throughput of lower-acuity patients,[47-49,52-54] and reduced LWBS rates[47-49]. It also decreased hospital admissions,[53] decreased testing and costs,[53] and increased available provider time for higher- acuity patients [52]. Overall ED length of stay was shortened,[47-49, 51-52, 54] patient satisfaction was improved, [55,56] and did not negatively affect clinical outcomes (unscheduled ED return visits or mortality rate) [49,53,56]. The success of fast-track systems is dependent on the availability of dedicated medical and nursing staff while adhering to rigid protocols of what patients can appropriately be placed in that treatment area [58,59]. Failure to staff fast-track areas with appropriate medical staff results in interruptions to fast-track programs [58]. This usually arises when fast-track staff offers their attention to patients in other more acute ED treatment areas [59].
A compilation of fast-track guidelines can be found here:
http://www.triagefirst.com/wp-content/uploads/2015/10/Triage-First_Fast-Track-Guidelines-2.pdf
OBSERVATION UNITS
Traditionally, patients who require care beyond the first hours in the emergency department (ED) have been admitted to the hospital. Economic pressures for efficiency in health care have led to the need for new strategies for those with difficult to rapidly diagnose ED presentations. Thus, observation units are increasingly becoming an important component of the modern ED. The average ED length of stay for an admitted ED patient is 5.5 hours while the average length of stay of an inpatient is 5 days [60]. Hospitals are increasingly being scrutinized for inpatients whose length of stay is one day or less [61]. This length of stay defines a subset of patients whose clinical needs exceed what can realistically be achieved within the 6 hours of an ED visit, but if managed actively will require less than 24 hours of hospitalization. These “6-24 hour” patients are often eligible for a dedicated observation unit. An ED-managed observation care unit decreased ambulance diversion by 40% and halved the rate of patients leaving without being seen [22]. Specific conditions appropriate for observation are:
Chest Pain
Studies have indicated that roughly 4% of patients with acute coronary syndromes are inadvertently discharged from the ED, often due to diagnostic uncertainty[62]. Four prospective randomized studies have shown that relative to inpatient admission, chest pain protocols are associated with lower cost, shorter length of stays, and improved resource utilization[63-66].
Asthma
In a study by McDermott acute asthmatics were randomized to either aggressive emergency department observation unit (EDOU) care for an additional 9 hours or to routine inpatient care following standard ED treatment. They found that 59% of EDOU asthmatics were discharged home compared with control groups where all were admitted. There were no differences in the two groups during the follow-up period in terms of relapse rates or subsequent morbidities. However there were significant differences in their length of stays (8.8 hr vs 59 hr), costs ($1202 vs $2247), and quality of life [67].
CHF
Diercks reported that heart failure patients with a systolic blood pressure under 160 mm Hg on ED presentation and a normal initial cardiac Troponin I were significantly more likely to be discharged from the EDOU and not experience a 30-day adverse events (death, readmission, myocardial infarction, arrhythmias) [68].
Dehydration
In a small retrospective observational study the diagnosis of dehydration was identified as the highest risk for early return visit to the ED and subsequent admission to the hospital on early return [69]. Hence, these patients are ideal for further management in the EDOU after initial resuscitation in the ED.
Transient Ischemic Attack
Ross reported a prospective study of 149 patients with transient ischemic attack who were randomized to either inpatient admission (control group) or ED observation unit admission for management using an accelerated diagnostic protocol [70]. All patients with transient ischemic attack had normal findings on computed tomography (CT) of the head, electrocardiography, laboratory studies and no known embolic source. Both groups had orders for serial clinical examinations, a neurology consultation, carotid duplex ultrasonography, echocardiography, and cardiac monitoring. Accelerated diagnostic protocol patients with positive testing results were admitted. Compared with the inpatient control group, patients in the accelerated diagnostic protocol group had total lengths of stay that were half as long (26 versus 61 hours), lower 90-day total direct costs ($890 versus $1,547), and comparable 90-day clinical outcomes. Accelerated diagnostic protocol patients were more likely to undergo carotid imaging (97% versus 90%) and echocardiography (97% versus 73%). Both groups had comparable rates of related return visits, subsequent strokes, and major clinical events.
Atrial Fibrillation
During the past 20 years, hospital admissions for atrial fibrillation have increased by 66% [71]. A subset of patients, those with uncomplicated acute onset (<48 hours) atrial fibrillation, may be eligible for treatment in an EDOU based on prospective studies as well as current American Heart Association practice guideline.
Deep Venous Thrombosis
Recommendations for treatment of DVT by ACP and ACCP state that outpatient treatment should be provided whenever possible [72,73]. This approach has been found to be cost effective, reducing both healthcare costs and hospital length of stay [74-76]. Compared with inpatients, those treated for DVT at home have greater levels of physical activity and social functioning, and demonstrate a more rapid return to pre-morbid levels of activity [77-79]. Integrating the many necessary steps that contribute to successful outpatient DVT management often requires the coordination of multiple therapies and services.
Syncope
Shen performed a prospective randomized control study of intermediate risk syncope patients who were randomized to a designated syncope unit or an inpatient admission following initial ED management which included an ECG and cardiac monitoring [82]. The syncope unit protocol included serial vital signs, continuous cardiac monitoring for up to 6 hours. The results of this study showed that at the time of dismissal from the ED, the presumptive cause of syncope was established for 67% of patients in the syncope unit group compared to 10% in the standard care group. The total hospital bed days were reduced by 54% for patients in the syncope unit group and 2-year clinical outcomes, including all-cause mortality and recurrent syncope, were similar between EDOU and admitted control groups [82].
IMAGING IN THE ED
The use of IV-contrast only for the evaluation of patients presenting to the ED with abdominal pain has been shown to have a high sensitivity and specificity for the diagnosis of common causes of acute abdominal pain, such as acute appendicitis, diverticulitis, and SBO [29,30]. The impact of limiting PO contrast in such patients not only decreased ED LOS, but also allowed for earlier consultation and definitive treatment for patients with identified pathology, with over 2 hours in time saved for patients requiring operative interventions. The time test ordered to time test completed was a median of 72 minutes shorter for patients undergoing the IV-contrast only protocol. It would be expected that the decrease in ED LOS would approximate the time saved by not using oral contrast [31]. The immediate use of whole body CT scans in trauma patients reduces median time in the ED by 8-35 minutes and time to the operating room but does not reduce mortality compared with selective imaging [32].
CARING FOR HALLWAY PATIENTS
For a growing number of EDs the solution had been to move both stable and semi-stable patients from licensed ED beds into adjacent ED hallways, thus freeing up the official ED bed for another patient [46]. In these circumstances ED physicians face a difficult challenge. They must provide care to patients in the hallway with suboptimal nursing support and lack of privacy, which precludes a full history and physical examination. Patients may not be able to be appropriately monitored. Returning newly triaged patients back to the waiting room until a licensed ED bed becomes available poses a similar risk, as there is no way to directly observe or monitor patients. The type of patient that is placed on a gurney in the ED hallway varies by institution and may vary within the same institution depending on who is in charge during times of crowding. Groups placed in hallways include (1) patients awaiting care but considered too unstable or ill to remain in the waiting room, (2) patients undergoing active medical and trauma care, but no vacant ED bed is available, (3) patients who are being “boarded” while awaiting transfer to an inpatient bed or transfer to another institution, (4) patients who arrive by ambulance but do not require immediate emergency care, and (5) patients awaiting transfer to a psychiatric facility [46].
OVERCAPACITY PROTOCOL
The concept originated in 2001 in the overcrowded emergency department at Stony Brook University Medical Center in Long Island, where patients piled up in the ED due to no available beds upstairs. This led to boarding patients, which in turn made the ED even more crowded and less efficient. Dr. Peter Vicellio, a practicing emergency physician and the clinical director of the emergency department at Stony Brook on Long Island, recognized that placing certain patients in inpatient hallways, would make beds available more quickly. Grant Innes and his group did a fantastic study on the overcapacity protocol, a true “before and after” study, at his institution [81]. “The protocol reduced the length of stay for admitted patients in the emergency department by about 5 hours, and with more than 8,000 admissions annually, this frees up about 41,000 hours of ED stretcher time,” said Dr. Grant Innes, chairman of the emergency department at St. Paul’s Hospital. [57] Mean ED length of stay for all admitted patients fell from 19 to 14 hours, a statistically significant decline. ED length of stay fell by 9 hours, 1.6 hours, and 9.2 hours for admitted medical, surgical, and mental health patients, respectively, changes that also were statistically significant. And hospital length of stay dropped by about 1 day for typical medical, surgical, and mental health patients, Dr. Innes said [57]. After OCP, arriving patients who were rated 1-3 (emergent-urgent) on the Canadian Triage and Acuity Scale rarely were left in ED waiting areas, and ambulance off-load delays dropped by 26%, he said[57].
The overcapacity protocol at Stony Brook can be found at: http://www.hospitalovercrowding.com/fullcapacity.htm
References / Further Reading
- Zoë Slote Morris, Adrian Boyle, Kathleen Beniuk, and Susan Robinson. Emergency department crowding: towards an agenda for evidence-based intervention. Emerg Med J. 2012 Jun;29(6):460-6. doi: 10.1136/emj.2010.107078. Epub 2011 Jun 7.
- J. Schull, M. Vermeulen, G. Slaughter, L. Morrison, and P. Daly, “Emergency department crowding and thrombolysis delays in acute myocardial infarction,” Annals of Emergency Medicine, vol. 44, no. 6, pp. 577–585, 2004.
- Hwang, L. D. Richardson, T. O. Sonuyi, and R. S. Morrison, “The effect of emergency department crowding on the management of pain in older adults with hip fracture,” Journal of the American Geriatrics Society, vol. 54, no. 2, pp. 270–275, 2006.
- B. Kulstad and K. M. Kelley, “Overcrowding is associated with delays in percutaneous coronary intervention for acute myocardial infarction,” International Journal of Emergency Medicine, vol. 2, no. 3, pp. 149–154, 2009.
- C. Moskop, D. P. Sklar, J. M. Geiderman, R. M. Schears, and K. J. Bookman, “Emergency department crowding, part 1-concept, causes, and moral consequences,” Annals of Emergency Medicine, vol. 53, no. 5, pp. 605–611, 2009.
- Chaflin DB, Treciak S, Likourezos A, et al. Impact of delayed transfer of critically ill patients from the emergency department to the intensive care unit. Crit Care Med. 2007;35(6):1477-1483.
- Weissman JS, Rothschild JM, Bendavid E, et al. Hospital workload and adverse events. Med Care. 2007;45(5):448-455.
- Cowan RM, Trzeciak S. Clinical review: emergency department overcrowding and potential impact on the critically ill. Crit Care. 2005;9(3):291-295.
- McNaughton, W. H. Self, I. D. Jones et al. “ED crowding and the use of nontraditional beds,” American Journal of Emergency Medicine, vol. 30, no. 8, pp. 1474–1480, 2012.
- Freeman, “The emerging subspecialty of Hallway Medicine,” Canadian Journal of Emergency Medicine, vol. 5, pp. 283–285, 2003.
- E. Mumma, J. Y. McCue, C.-S. Li, and J. F. Holmes, “Effects of emergency department expansion on emergency department patient flow,” Academic Emergency Medicine, vol. 21, no. 5, pp. 504–509, 2014.
- G. Campbell and D. E. Sinclair, “Strategies for managing a busy emergency department,” Canadian Journal of Emergency Medicine, vol. 6, no. 4, pp. 271–276, 2004.
- Viccellio, C. Santora, A. J. Singer, H. C. Thode Jr., and M. C. Henry, “The association between transfer of emergency department boarders to inpatient hallways and mortality: a 4-year experience,” Annals of Emergency Medicine, vol. 54, no. 4, pp. 487–491, 2009.
- Viccellio, J. A. Zito, V. Sayage et al. “Patients overwhelmingly prefer inpatient boarding to emergency department boarding,” Journal of Emergency Medicine, vol. 45, no. 6, pp. 942–946, 2013.
- R. Richards, G. Ozery, M. Notash, P. E. Sokolove, R. W. Derlet, and E. A. Panacek, “Patients prefer boarding in inpatient hallways: correlation with the national emergency department overcrowding score,” Emergency Medicine International, vol. 2011, Article ID 840459, 4 pages, 2011.
- Walsh, V. Cortez, and H. Bhakta, “Patients would prefer ward to emergency department boarding while awaiting an inpatient bed,” Journal of Emergency Medicine, vol. 34, no. 2, pp. 221–226, 2008.
- Derlet RW, Richards JR. Ten Solutions for Emergency Department Crowding. Western Journal of Emergency Medicine. 2008;9(1):24-27.
- Bucheli B, Martina B. Reduced length of stay in medical emergency department patients: a prospective controlled study on emergency physician staffing. Eur J Emerg Med. 2004;11:29- 34.
- Donald KJ, Smith AN, Doherty S, et al. Effect of an on-site emergency physician in a rural emergency department at night. Rural Remote Health. 2005;5:380.
- Shaw KN, Lavelle JM. VESAS: a solution to seasonal fluctuations in emergency department census. Ann Emerg Med. 1998;32:698-702.
- Lindley-Jones and B. J. Finlayson, “Triage nurse requested x rays—are they worthwhile?” Journal of Accident and Emergency Medicine, vol. 17, no. 2, pp. 103–107, 2000.
- Kelen GD, Scheulen JJ, Hill PM. Effect of an emergency department (ED) managed acute care unit on ED overcrowding and emergency medical services diversion. Acad Emerg Med. 2001 Nov;8(11):1095-100.
- J. Gallagher, S.G. Lynn. The etiology of medical gridlock: causes of emergency department overcrowding in New York City. J Emerg Med, 8 (1990), pp. 785–790
- United States General Accounting Office. Emergency departments: unevenly affected by growth and change in patient use: Report to the Chairman, Subcommittee on Health for Families and the Uninsured, Committee on Finance, US Senate, January 1993
- S. Olshaker, N.K. Rathlev. Emergency department overcrowding and ambulance diversion: the impact and potential solutions of extended boarding of admitted patients in the emergency department. J Emerg Med, 30 (2006), pp. 351–356
- Trzeciak, E. Rivers. Emergency department overcrowding in the United States: an emerging threat to patient safety and public health. Emerg Med J, 20 (2003), pp. 402–405
- Espinosa, O. Miro, M. Sanchez, et al. Effects of external and internal factors on emergency department overcrowding [letter]Ann Emerg Med, 39 (2002), pp. 693–695
- J. Schull, A. Kiss, J.-P. Szalai. The effect of low-complexity patients on emergency department waiting times. Ann Emerg Med, 49 (2007), pp. 257–264
- Mun S, Ernst RD, Chen K, et al. Rapid CT diagnosis of acute appendicitis with IV contrast material. Emerg Radiol. 2006;12:99–102.
- Anderson SW, Soto JA, Lucey BC, et al. Abdominal 64-MDCT for Suspected Appendicitis: The Use of Oral and IV Contrast Material Versus IV Contrast Material Only. Am J Roentgenol. 2009;193:1282–1288.
- Hopkins CL, Madsen T, Foy Z, Reina M, Barton E. Does Limiting Oral Contrast Decrease Emergency Department Length of Stay? Western Journal of Emergency Medicine. 2012;13(5):383-387.
- Shah K.H., Guthrie J.M. Does immediate total-body computed tomography reduce mortality and time in the emergency department for trauma patients? Annals of Emergency Medicine. 2014;63(4),pp.465-466.
- Lee WW, Filiatrault L, Abu-Laban RB, et al. Effect of Triage Nurse Initiated Radiography Using the Ottawa Ankle Rules on Emergency Department Length of Stay at a Tertiary Centre. CJEM. 2015;20:1-8.
- Lambe S, Washington DL, Fink A, et al. Waiting times in California’s emergency departments. Ann Emerg Med. 2003;41: 35-44.
- Fatovich DM, Nagree Y, Sprivulis P. Access block causes emergency department overcrowding and ambulance diversion in Perth, Western Australia. Emerg Med J. 2005;22:351-354.
- Davis B, Sullivan S, Levine A, et al. Factors affecting ED length- of-stay in surgical critical care patients. Am J Emerg Med. 1995; 13:495-500.
- Forster AJ, Stiell I, Wells G, et al. The effect of hospital occupancy on emergency department length of stay and patient disposition. Acad Emerg Med. 2003;10:127-133.
- Lee KM, Wong TW, Chan R, et al. Accuracy and efficiency of X-ray requests initiated by triage nurses in an accident and emergency department. Accid Emerg Nurs. 1996;4:179-181.
- Singer AJ, Stark MJ. Pretreatment of lacerations with lidocaine, epinephrine, and tetracaine at triage: a randomized double-blind trial. Acad Emerg Med. 2000;7:751-756.
- Campbell P, Dennie M, Dougherty K, et al. Implementation of an ED protocol for pain management at triage at a busy level I trauma center. J Emerg Nurs. 2004;30:431-438.
- Seguin D. A nurse-initiated pain management advanced triage protocol for ED patients with an extremity injury at a level I trauma center. J Emerg Nurs. 2004;30:330-335.
- Singer AJ, Stark MJ. Pretreatment of lacerations with lidocaine, epinephrine, and tetracaine at triage: a randomized double-blind trial. Acad Emerg Med. 2000;7:751-756.
- Cooper JJ, Datner EM, Pines JM. Effect of an automated chest radiograph at triage protocol on time to antibiotics in patients admitted with pneumonia. Am J Emerg Med. 2008;26:264-269.
- Graff L, Palmer AC, Lamonica P, et al. Triage of patients for a rapid (5-minute) electrocardiogram: a rule based on presenting chief complaints. Ann Emerg Med. 2000;36:554-560
- Macy D, Johnston M. Using electronic wristbands and a triage protocol to protect mental health patients in the emergency department. J Nurs Care Qual. 2007;22:180-184.
- John R. Richards, M. Christien van der Linden, and Robert W. Derlet, “Providing Care in Emergency Department Hallways: Demands, Dangers, and Deaths,” Advances in Emergency Medicine, vol. 2014, Article ID 495219, 7 pages, 2014. doi: 10.1155/2014/495219.
- Ieraci S, Digiusto E, Sonntag P, et al. Streaming by case complexity: evaluation of a model for emergency department fast track. Emerg Med Australas. 2008;20:241-249.
- O’Brien D, Williams A, Blondell K, et al. Impact of streaming “fast track” emergency department patients. Australian Health Rev. 2006;30:525-532.
- Sanchez M, Smally AJ, Grant RJ, et al. Effects of a fast-track area on emergency department performance. J Emerg Med. 2006;31; 117-120.
- Kwa P, Blake D. Fast track: has it changed patient care in the emergency department? Emerg Med Australas. 2008;20:10-15.
- Cooke MW, Wilson S, Pearson S. The effect of a separate stream for minor injuries on accident and emergency department waiting times. Emerg Med J. 2002;19:28-30.
- Simon HK, McLario D, Daily R, et al. “Fast tracking” patients in an urban pediatric emergency department. Am J Emerg Med. 1996;14:242-244.
- Hampers LC, Cha S, Gutglass DJ, et al. Fast track and the pediatric emergency department: resource utilization and patient outcomes. Acad Emerg Med. 1999;6:1153-1159.
- Darrab AA, Fan J, Fernandes CM. How does fast track affect quality of care in the emergency department? Eur J Emerg Med. 2006;13:32-35.
- Rodi SW, Grau MV, Orsini CM. Evaluation of a fast track unit: alignment of resources and demand results in improved satisfaction and decreased length of stay for emergency department patients. Q Manage Health Care. 2006;15:163-170.
- Nash K, Zachariah B, Nitschmann J, et al. Evaluation of the fast track unit of a university emergency department. J Emerg Nurs. 2007;33:14-20.
- http://www.acep.org/Clinical—Practice-Management/Overcapacity-Protocol-Cuts-Time-Spent-in-ED/ last accessed November 14, 2015
- Cameron JM. Managing emergency demand in public hospitals. Performance audit report no 71. Melbourne: Office of the Auditor General, 2004. http://www.audit.vic.gov.au/reports_par/medph_report.pdf (Last accessed November 23 2015)
- Meislin HW, Coates SA, Cyr J, et al. Fast track: urgent care within a teaching hospital. Can it work? Ann Emerg Med 1988;17:453–6.
- Pitts SR, Niska RW, Xu J, et al. National Hospital Ambulatory Medical Care Survey: 2006 emergency department summary. Natl Health Stat Report 2008:1-38.
- Program for Evaluating Payment Patterns Electronic Report. (Accessed at http://www.pepperresources.org/).
- Zalenski RJ, Selker HP, Cannon CP, et al. National Heart Attack Alert Program position paper: chest pain centers and programs for the evaluation of acute cardiac ischemia. Ann Emerg Med. 2000;35:462-71.
- Roberts RR, Zalenski RJ, Mensah EK, et al. Costs of an emergency department-based accelerated diagnostic protocol vs hospitalization in patients with chest pain: a randomized controlled trial. JAMA. 1997;278:1670-6.
- Gomez MA, Anderson JL, Karagounis LA, et al. An emergency department-based protocol for rapidly ruling out myocardial ischemia reduces hospital time and expense: results of a randomized study (ROMIO). J Am Coll Cardiol. 1996;28:25-33.
- Farkouh ME, Smars PA, Reeder GS, et al. A clinical trial of a chest-pain observation unit for patients with unstable angina. Chest Pain Evaluation in the Emergency Room (CHEER) Investigators. N Engl J Med. 1998;339:1882-8.
- Baugh CW, Bohan JS. Estimating observation unit profitability with options modeling. Acad Emerg Med. 2008;15:445-52.
- McDermott MF, Murphy DG, Zalenski RJ, et al. A comparison between emergency diagnostic and treatment unit and inpatient care in the management of acute asthma. Arch Intern Med. 1997;157:2055-62.
- Diercks DB, Peacock WF, Kirk JD, et al. ED patients with heart failure: identification of an observational unit-appropriate cohort. Am J Emerg Med. 2006;24:319-24.
- Johnston SC, Gress DR, Browner WS, et al. Short-term prognosis after emergency department diagnosis of TIA. JAMA. 2000;284:2901-6.
- Ross MA, Compton S, Medado P, et al. An emergency department diagnostic protocol for patients with transient ischemic attack: A randomized controlled trial. Ann Emerg Med. 2007.50(2);109-119.
- Fuster V, Ryden LE, Cannom DS, et al. ACC/AHA/ESC 2006 Guidelines for the Management of Patients with Atrial Fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the Management of Patients With Atrial Fibrillation): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation. 2006;114:e257-354.
- Snow V, Qaseem A, Barry P, et al. Management of venous thromboembolism: a clinical practice guideline from the American College of Physicians and the American Academy of Family Physicians. Ann Fam Med. 2007;5:74-80.
- Estrada CA, Mansfield CJ, Heudebert GR. Cost-effectiveness of low-molecular-weight heparin in the treatment of proximal deep vein thrombosis. J Gen Intern Med. 2000;15:108-15.
- Gould MK, Dembitzer AD, Sanders GD, et al. Low-molecular-weight heparins compared with unfractionated heparin for treatment of acute deep venous thrombosis. A cost-effectiveness analysis. Ann Intern Med. 1999;130:789-99.
- Rodger M, Bredeson C, Wells PS, et al. Cost-effectiveness of low-molecular-weight heparin and unfractionated heparin in treatment of deep vein thrombosis. CMAJ. 1998;159:931-8.
- Koopman MM, Prandoni P, Piovella F, et al. Treatment of venous thrombosis with intravenous unfractionated heparin administered in the hospital as compared with subcutaneous low-molecular-weight heparin administered at home. The Tasman Study Group. N Engl J Med. 1996;334:682-7.
- O’Brien B, Levine M, Willan A, et al. Economic evaluation of outpatient treatment with low-molecular-weight heparin for proximal vein thrombosis. Arch Intern Med. 1999;159:2298-304.
- Bossuyt PM, van den Belt AG, Prins MH. Out-of-Hospital Treatment of Venous Thrombosis: Socioeconomic Aspects and Patients’ Quality of Life. Haemostasis. 1998;28 Suppl S3:100-7.
- Vinson DR, Berman DA. Outpatient treatment of deep venous thrombosis: a clinical care pathway managed by the emergency department. Ann Emerg Med. 2001;37:251-8.
- ACEP Crowding Resources Task Force. Responding to Emergency Department Crowding: A Guidebook for Chapters. Dallas, TX: American College of Emergency Physicians; 2002.
- Innes GD, Grafstein E, Stenstrom R, Harris D, Hunte G, Schwartzman A. IMPACT of an overcapacity care protocol on emergency department overcrowding. Academic Emerg Med. 2007. 14(5 Supplement 1):S85-S85. DOI: 10.1197/j.aem.2007.03.936
- Shen WK, Decker WW, Smars PA, et al. Syncope Evaluation in the Emergency Department Study (SEEDS): a multidisciplinary approach to syncope management. Circulation. 2004;110:3636-45.