Authors: Alexander X. Lo, MD, PhD (Department of Emergency Medicine, University of Alabama at Birmingham), Katrina A. Booth, MD (Department of Medicine, Division of Gerontology, Geriatrics, and Palliative Care, University of Alabama at Birmingham), Ula Y. Hwang, MD, MPH (Departments of Emergency Medicine and Geriatrics, Mount Sinai School of Medicine and the Geriatrics Research, Education and Clinical Center (GRECC) at the James J. Peters VAMC, Bronx, NY) // Edited by: Alex Koyfman, MD (EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital, @EMHighAK) & Justin Bright, MD (@JBright2021)
Facts about ED visits by older adults
- “Geriatric patients” have traditionally been referred to as adults >65 years
- >40 million U.S. adults >65 years (2010 census), represent 13% of the U.S. population(1). By 2030, 69 million persons or 19% of the U.S. population will be >65 years, and their healthcare utilization, particularly hospitalizations and ED visits, will continue to increase and exceed the ability of the U.S. healthcare system to meet these needs(2, 3).
- 20 million ED visits in 2010 with continuous rising trend in visit numbers from previous 10 years (16 million visits in 2001)(4)
- 5 mil visits by 65-79y, 7 mil visits by >80y, 50,000 visits by >100y
- >2 million visits for falls related conditions; >800,000 for pneumonia
- Hospital admissions rates for older adults to the inpatient setting or ICU from the ED also increased 2001 and 2010 (4)
- Hospital admissions for those >65y represent 36% of all hospitalizations for all adults >18 years
- Higher % of ED visits result in admissions (33-50%) for adults >65y than for adults <65y (15-20%)
- Top five reasons (2001 to 2009) for ED visit were (1) Chest pain; (2) SOB; (3) Abdominal pain; (4) Accident NOS; (5) General weakness (4)
- Returns to the ED after an ED visit (“ED recidivism”) range from 24% to 38% (5) (see below under Disposition)
Preliminary Steps (Before you walk into the room)
- Acuity increases with age (6), so beware of the under-triaged older adult based on
- Atypical presentations of common complaints
- Stoicism or minimization of problem
- Review medical records (if available)
- Does the patient have a history of dementia, delirium or other cognitive deficit? If so, verify (corroborate) any history
- Is there a pattern of ED visits to suggest unmet social needs (e.g. caregiver fatigue; unsafe home environment; poor access to care)
- Are there patterns of injuries to raise suspicion of elder abuse?
- Code status and goals of care
- If unclear, ask for this information and find out sooner than later
Recommended Approach and Assessment: A few pearls
Subjective Assessment:
- Older adults may minimize complaints, conditions, and symptoms
- Over 40% of older adults in ED have a cognitive deficit which may affect history-taking (37% dementia; 5% delirium)(7); corroborate history with family/caregiver/companion whenever feasible to not miss anything
- Atypical chief complaints are common (8)
- “Confusion” – Is it dementia, delirium or an intracranial lesion?
- If they have dementia, how is this episode DIFFERENT FROM BASELINE?
- A “new” psychiatric problem (e.g. “psychosis” or “mania” or “aggressive behavior” is RARELY a de novo psychiatric problem – think medical (organic) etiology first, then think medications, then think something else OTHER than.
- Common medical problems can cause change in mentation: UTI; AMI; pain; thyroid dysfunction
Objective Assessment:
- Mental Status or “Confusion” – Is it dementia, delirium or an intracranial lesion?
- Not everyone needs a head CT; anyone on anticoagulants MUST get a head CT, EVERYTIME (also see Intracranial section below regarding delayed intracranial hemorrhage)
- If they have dementia, how is this episode DIFFERENT FROM BASELINE?
- If you suspect undocumented dementia, the Short Blessed Test is a good cognitive function screen for ED use that is most sensitive/specific(7)
- A “new” psychiatric problem (e.g. “psychosis” or “mania” or “aggressive behavior” is RARELY a de novo psychiatric problem – think medical (organic) etiology first, then think medications, then think something else OTHER than psychiatric
- Delirium
- Richmond Agitation Sedation Scale (RASS) is a quick delirium screen for ED use with very good sensitivity/specificity; RASS >+1 or <-1 is nearly diagnostic(9)
- Intracranial
- Older adults, particularly those on anticoagulants, may be at higher risk for delayed bleeds. However, there is NO widely accepted consensus guidelines on screening for delayed bleeds if the initial CT is negative(10-13)
- A compromise strategy may be to screen (e.g. by telephone follow-up for signs/symptoms within 24 hours) to decide need for repeat head CT within 24 hours of a negative study; if follow-up cannot be guaranteed, admission for observation may be necessary(11)
- Dizziness
- 15% of older adults presenting to ED for dizziness have serious etiologies; 4-6% are stroke-related and sensitivity of CT for identifying stroke or intracranial lesion in dizziness is poor (16%), so if CNS etiology suspected, seek neuro consult or MRI (83% sensitivity)(14)
- Skeletal Injury
- C-spine injuries may result from seemingly benign trauma/falls
- Compression fractures of vertebral column can result from relatively little trauma
- Given high prevalence of osteopenia/osteoporosis, X-ray imaging can have reduced sensitivity, consider CT studies for fractures, especially vertebral fractures (15)
- Knee pain? May be referred pain from occult hip fracture
- Cardiopulmonary
- AMI presents with atypical complaints in older adults (e.g., “indigestion”, “dizziness”, “tired”)
- Heart failure (HF): ~70% of patients >65y with HF have normal EF of >50%(18), and BNP underestimates degree of decompensation due to thicker heart (thicker heart, less stretch, smaller rise in BNP)(19); consider BNP difference from last hospital discharge to help determine severity and disposition
- Abdominal pain
- Visceral pain is modified in older adult; exam can underestimate severity (8)
- Constipation and urinary retention are common but often overlooked causes of abdominal pain
- Risk of ischemic bowel is higher in older adults
- Acute abdominal series provides quick screen for perforation or SBO and balances benefit of CT against higher risk of contrast-induced nephropathy in older adults(20)
- Falls
- Rule-out medical/surgical or medication-related reasons for the fall; check orthostatic vital signs
- One mechanical fall in a given year –no unequivocal need for further ED testing unless clinical suspicion
- Two falls in a given year is a red flag and requires a comprehensive evaluation (in the outpatient setting; ideally by a geriatrician)(21)
Clinical Decision Making and ED Management:
- Screening for geriatric syndromes is critical (22)
- polypharmacy
- delirium/dementia
- fall risk
- function (independence) and mobility
- abuse and neglect
- Geriatric syndromes are individually associated with ED returns and adverse outcomes (e.g. hospitalization, death at 30 days) and must be addressed, not necessarily in the ED if prompt and reliable outpatient follow-up with their PCP can be arranged
- Beware that screening for adverse outcomes is complicated by scarcity of reliable instruments (results vary across populations)(23)
- Managing the agitated older adult
- Try to avoid use of restraints (if patient has dementia or is delirious, restraints worsen the situation)
- Is agitation related to pain? Agitation is often secondary to pain: Start with low dose opioid, and titrate up (start low and go slow) – why? You can reverse it
- Avoid benzodiazepines with delirium, they can paradoxically worsen it – UNLESS patient is on chronic benzodiazepines (make sure it’s for a good reason), then consider use as it could be benzo withdrawal
- Avoid Haldol – Haldol can lead to fatal reactions in Parkinson’s disease and prolonged QT interval; if neither condition is present (once you’re sure), then use a LOW dose. AVOID Haldol 5mg in anyone over 55. Use magnesium sulfate to treat long QT intervaL
- Antipsychotics help manage the behavior but will NOT treat the underlying cause – you still need to evaluate for the medical cause(s) of the agitation
- After any diagnostic study with IV contrast, give fluids
- Older adults are at higher risk of contrast-induced nephropathy; IV saline is recommended(20)
- IV fluid resuscitation
- Unless patient is in shock, steady IV infusion is preferred over a rapid bolus, particularly if heart failure present
- Medications
- Do not assume what is listed in the computer accurately reflects the patient’s medication regimen
- Always confirm medication regimen with patient, family, or pharmacy/home health if patient/family not able to tell
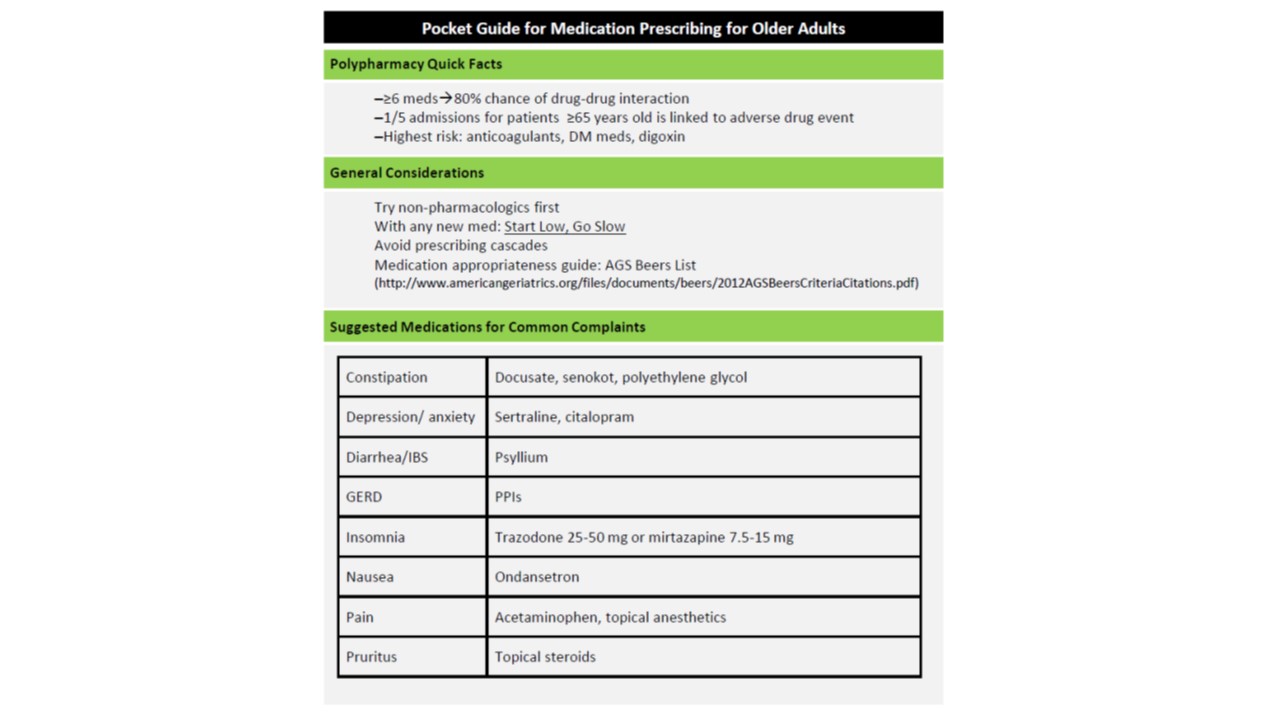
- Potentially Inappropriate Medications (PIM) (24): Older adults have greater susceptibility to adverse effects of particular medications (See Tables 1 and 2)
- New symptoms may be due to a medication side effect (See Tables 1 and 2)
- New medications for common complaints could be a source of adverse outcomes. Tables 1 and 2 provide suggested treatments for common complaints
- PIMs may be indicated and necessary in specific ED situations (e.g. diphenhydramine for acute allergic reactions) but be cautious regarding duration/course when prescribing for post-discharge use
Disposition:
- Precautionary steps at time of discharge
- Ability to understand and follow discharge instructions (consider degree of patient and caregiver health literacy, low vision, cognitive impairment, logistics of clinician follow-up)
- If all work-ups are negative but clinical suspicion persists
- Pursue rapid (24-48 hours) outpatient follow-up with PCP (if available and if patient logistically can go to PCP)
- Consider the 48-hour ED return
- CAUTION: Hospitalization worsens function, mobility, and morbidity(25, 26), which in turn lead to ED returns(5) and hospitalization(27)
- Hospitalize only if clinically indicated (ideally)
- If social issues exist – can ED social worker or case manager find a sufficiently safe disposition for patient and avoid hospitalization?
- If social needs cannot be met, or if safety is a concern, then admit to hospital but ensure that inpatient service understands the problem (and document this need for transitions of care)
Pitfalls
- Look for atypical presentations of common medical conditions (8)
- Avoid admitting to hospital simply because of their age, as unwarranted hospitalization CAN be harmful to the patient’s subsequent function, mobility, and quality of life
- Know your own biases: older adults are a source of stress in EPs; >75% recognize the need to improve quality of care (28)
- Address unmet social needs as these are highly responsible for ED returns (5) – ask ED social worker or case manager for help
- Screen for geriatric syndromes to identify older adults at high risk for adverse events
- Delirium (abnormal RASS score) predicts increased mortality at 6 months (31)
- Dementia is unrecognized in the ED up to 70% of the time
- Elder abuse and neglect may have subtle signs/symptoms
- Two mechanical falls in a given year indicates an increased risk of adverse events
- Declines in mobility (e.g. walking speed) is associated with increased hospitalization or mortality
- Potentially Inappropriate Medications (PIMs)

References / Further Reading
- Steiner C, Elixhauser A, Schnaier J. The healthcare cost and utilization project: an overview. Eff Clin Pract. 2002;5(3):143-51.
- Hwang U, Shah MN, Han JH, Carpenter CR, Siu AL, Adams JG. Transforming emergency care for older adults. Health Aff (Millwood). 2013;32(12):2116-21.
- Halaweish I, Alam HB. Changing demographics of the American population. Surg Clin North Am. 2015;95(1):1-10.
- Pines JM, Mullins PM, Cooper JK, Feng LB, Roth KE. National trends in emergency department use, care patterns, and quality of care of older adults in the United States. J Am Geriatr Soc. 2013;61(1):12-7.
- Deschodt M, Devriendt E, Sabbe M, Knockaert D, Deboutte P, Boonen S, et al. Characteristics of older adults admitted to the emergency department (ED) and their risk factors for ED readmission based on comprehensive geriatric assessment: a prospective cohort study. BMC Geriatr. 2015;15:54.
- Green SM. Emergency department patient acuity varies by age. Ann Emerg Med. 2012;60(2):147-51.
- Carpenter CR, Bassett ER, Fischer GM, Shirshekan J, Galvin JE, Morris JC. Four sensitive screening tools to detect cognitive dysfunction in geriatric emergency department patients: brief Alzheimer’s Screen, Short Blessed Test, Ottawa 3DY, and the caregiver-completed AD8. Acad Emerg Med. 2011;18(4):374-84.
- Peters ML. The older adult in the emergency department: aging and atypical illness presentation. J Emerg Nurs. 2010;36(1):29-34.
- Han JH, Vasilevskis EE, Schnelle JF, Shintani A, Dittus RS, Wilson A, et al. The Diagnostic Performance of the Richmond Agitation Sedation Scale for Detecting Delirium in Older Emergency Department Patients. Acad Emerg Med. 2015;22(7):878-82.
- Goergen N, Cooper JG, Wintour K. The threshold for CT scanning anticoagulated head injury patients is still not yet clear. Ann Emerg Med. 2013;61(4):500-1.
- Li J. Admit all anticoagulated head-injured patients? A million dollars versus your dime. You make the call. Ann Emerg Med. 2012;59(6):457-9.
- Miller J, Lieberman L, Nahab B, Hurst G, Gardner-Gray J, Lewandowski A, et al. Delayed intracranial hemorrhage in the anticoagulated patient: A systematic review. J Trauma Acute Care Surg. 2015;79(2):310-3.
- Shah KH, Newman DH, Raja AS. Repeated CTs-let’s use our heads. Ann Emerg Med. 2012;60(4):537-8; author reply 8.
- Lo AX, Harada CN. Geriatric dizziness: evolving diagnostic and therapeutic approaches for the emergency department. Clin Geriatr Med. 2013;29(1):181-204.
- Parizel PM, van der Zijden T, Gaudino S, Spaepen M, Voormolen MH, Venstermans C, et al. Trauma of the spine and spinal cord: imaging strategies. Eur Spine J. 2010;19 Suppl 1:S8-17.
- Backus BE, Six AJ, Kelder JC, Bosschaert MA, Mast EG, Mosterd A, et al. A prospective validation of the HEART score for chest pain patients at the emergency department. Int J Cardiol. 2013;168(3):2153-8.
- Six AJ, Backus BE, Kelder JC. Chest pain in the emergency room: value of the HEART score. Neth Heart J. 2008;16(6):191-6.
- Lo AX, Donnelly JP, McGwin G, Jr., Bittner V, Ahmed A, Brown CJ. Impact of Gait Speed and Instrumental Activities of Daily Living on All-Cause Mortality in Adults >/=65 Years With Heart Failure. Am J Cardiol. 2015.
- Collins SP, Storrow AB. Acute heart failure risk stratification: can we define low risk? Heart Fail Clin. 2009;5(1):75-83, vii.
- Detrenis S, Meschi M, Bertolini L, Savazzi G. Contrast medium administration in the elderly patient: is advancing age an independent risk factor for contrast nephropathy after angiographic procedures? J Vasc Interv Radiol. 2007;18(2):177-85; quiz 85.
- Panel on Prevention of Falls in Older Persons AGS, Society BG. Summary of the Updated American Geriatrics Society/British Geriatrics Society clinical practice guideline for prevention of falls in older persons. J Am Geriatr Soc. 2011;59(1):148-57.
- Carpenter CR, Bromley M, Caterino JM, Chun A, Gerson LW, Greenspan J, et al. Optimal older adult emergency care: introducing multidisciplinary geriatric emergency department guidelines from the American College of Emergency Physicians, American Geriatrics Society, Emergency Nurses Association, and Society for Academic Emergency Medicine. Acad Emerg Med. 2014;21(7):806-9.
- Carpenter CR, Shelton E, Fowler S, Suffoletto B, Platts-Mills TF, Rothman RE, et al. Risk factors and screening instruments to predict adverse outcomes for undifferentiated older emergency department patients: a systematic review and meta-analysis. Acad Emerg Med. 2015;22(1):1-21.
- American Geriatrics Society Beers Criteria Update Expert P. American Geriatrics Society updated Beers Criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2012;60(4):616-31.
- Brown CJ, Roth DL, Allman RM, Sawyer P, Ritchie CS, Roseman JM. Trajectories of life-space mobility after hospitalization. Ann Intern Med. 2009;150(6):372-8.
- Covinsky KE, Palmer RM, Fortinsky RH, Counsell SR, Stewart AL, Kresevic D, et al. Loss of independence in activities of daily living in older adults hospitalized with medical illnesses: increased vulnerability with age. J Am Geriatr Soc. 2003;51(4):451-8.
- Cesari M, Kritchevsky SB, Penninx BW, Nicklas BJ, Simonsick EM, Newman AB, et al. Prognostic value of usual gait speed in well-functioning older people–results from the Health, Aging and Body Composition Study. J Am Geriatr Soc. 2005;53(10):1675-80.
- Schumacher JG, Deimling GT, Meldon S, Woolard B. Older adults in the Emergency Department: predicting physicians’ burden levels. J Emerg Med. 2006;30(4):455-60.
- O’Cathain A, Knowles E, Maheswaran R, Pearson T, Turner J, Hirst E, et al. A system-wide approach to explaining variation in potentially avoidable emergency admissions: national ecological study. BMJ Qual Saf. 2014;23(1):47-55.
- Lewis Hunter AE, Spatz ES, Bernstein SL, Rosenthal MS. Factors Influencing Hospital Admission of Non-critically Ill Patients Presenting to the Emergency Department: a Cross-sectional Study. J Gen Intern Med. 2015.
- Han JH, Vasilevskis EE, Shintani A, Graves AJ, Schnelle JF, Dittus RS, et al. Impaired arousal at initial presentation predicts 6-month mortality: an analysis of 1084 acutely ill older patients. J Hosp Med. 2014;9(12):772-8.
- http://www.ncbi.nlm.nih.gov/pubmed/25635203








