Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 43-year-old male right hand dominant man presents with pain and swelling of his left index finger. He is a professional painter and was using an industrial pain sprayer when he injected his left index finger. His finger was not hurting at first, but it now is exquisitely painful, with a large degree of swelling. His VS are normal except for a HR of 102. His finger is swollen, and you notice a small open injury on the tip of the finger. Your neurovascular exam of the finger is normal.
What’s the diagnosis, and what’s your next step in your evaluation and treatment?
Answer: High-pressure injection injury of the finger
- Background:
- This injury is a surgical emergency, with amputation rates as high as 50% for organic solvents.
- It occurs most commonly in laborers who use paint, grease, solvents, and oil.
- Injury usually occurs to the nondominant hand/fingers from injection with grease, paint, or fuel.
- Injection results in a force of 3,000-10,000 PSI, up to 400 mph. A force of > 100 PSI is needed to break skin.
- Even small amounts of injected material may result in compartment syndrome.
- The type of material injected is the most important consideration. Other factors include time from injury to treatment, injection force, injected volume, and material composition.
- As a general rule, water-based solvents are less destructive, while oil-based and industrial solvents are more destructive.
- Air and water, if clean, are lower risk for poor outcomes. Grease results in a small inflammatory response and low rate of amputation. However, paint causes severe inflammation and high rates of amputation.
- Injected material can track up the arm, dissecting planes of least resistance along neurovascular bundles, and result in vascular occlusion and severe soft tissue necrosis.
- History and Exam:
- The hand/fingers are most commonly affected, especially the nondominant extremity index finger (second digit).
- Three phases of injury may occur: Acute (< 6 hours, with symptoms beginning with pain and swelling; at 12 hours, necrosis begins to occur), intermediate (lipogranuloma formation in affected tissues as a result of foreign material), late (breakdown of tissue and skin forming ulcers).
- The actual site of injury typically appears benign at first, but this is misleading.
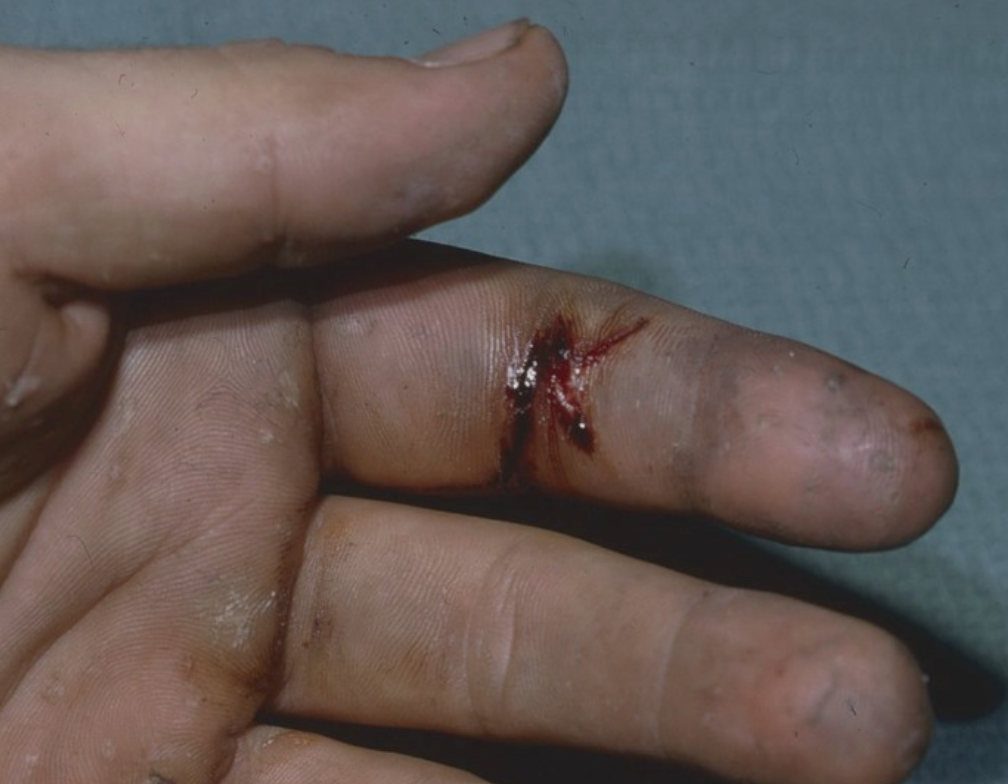
- Later in the course of disease, the affected digit and extremity becomes edematous, tender, and pale.
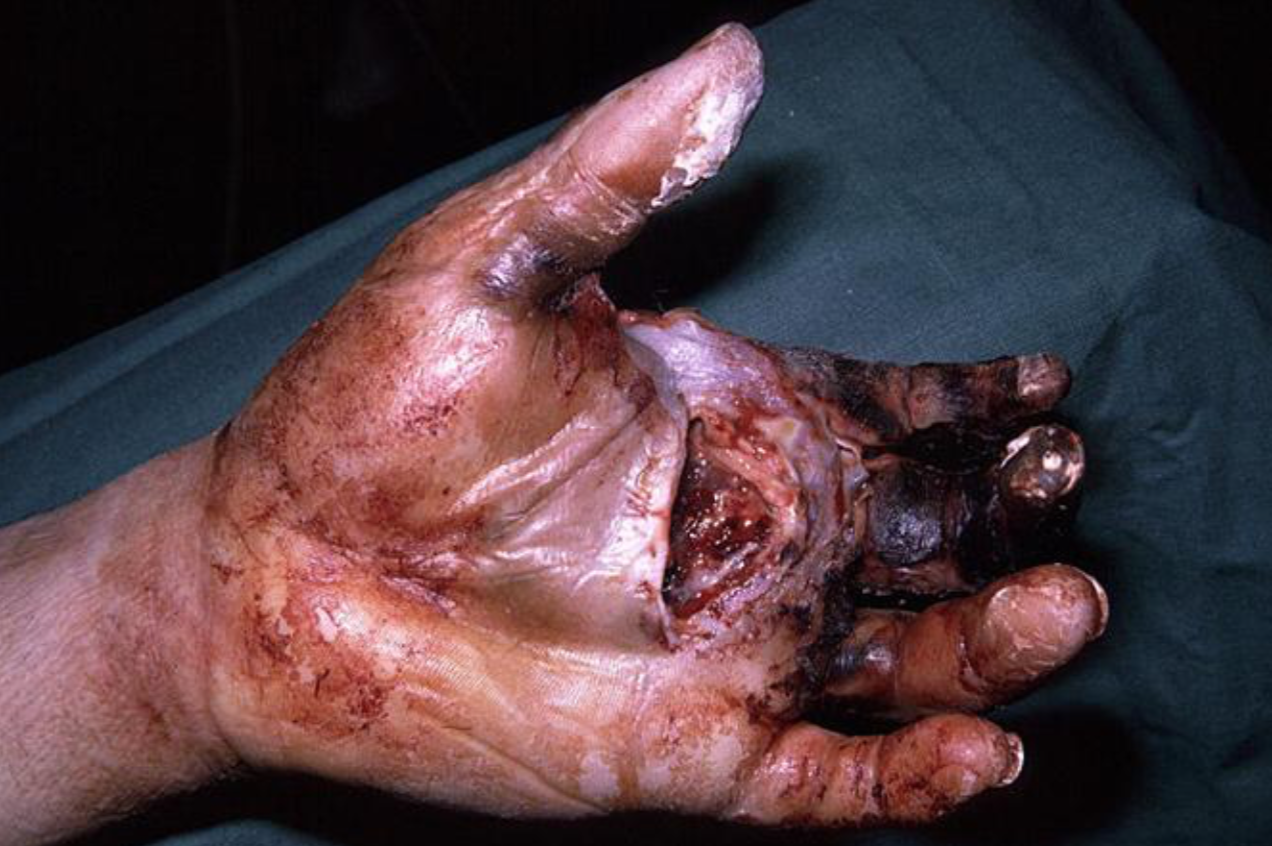
- Systemic absorption may result in generalized toxic reaction to material with fever and flu-like illness.
- Obtain history of site of injury, time of injury, hand dominance, suspected injected material. Time of injury is essential to obtain, as time to treatment affects outcome.
- Evaluate neurovascular status: resting position, tenderness, passive/active range of motion, radial/median/ulnar nerves, capillary refill, pulses, appearance of skin.
- Diagnostics:
- Laboratory studies typically not required and are often normal.
- Radiographs are important to evaluate for spread of radio-opaque dye. However, images may be normal.
- Keep in mind this is a clinical diagnosis.
- Management
-
- Splint and elevate the affected area.
- Emergently consult orthopedics/hand surgery.
- Nonoperative therapy may be an option for patients with injection of air and water.
- Operative therapy is required in the majority of patients. Immediate debridement is associated with improved outcomes.
- Delay of > 10 hours from time of injection is associated with higher rates of amputation.
- Debridement requires removal of as much foreign material as possible.
- Update tetanus status.
- Provide broad-spectrum antibiotics, as necrotic material acts as a culture medium for bacterial growth. Gram-positive and Gram-negative bacteria result in severe infection.
- Provide systemic analgesia, but avoid digital blocks due to high pressure in the affected extremity.
- Admit all patients with high-pressure injection injury.

-
*All photos and tables credit of orthobullets.*

A 34-year-old, right hand dominant man presents with pain and swelling of his left index finger. The patient works as a painter and was using an industrial paint sprayer and sprayed his left index finger. At first, his finger was not painful but he has developed increasing pain and swelling. The finger is mildly swollen but no laceration, erythema, or warmth is noted. Range of motion is full and sensation and capillary refill are normal. In addition to splinting and elevation, which of the following represents the best management course?
A) Admission to medical service for intravenous antibiotics
B) Discharge with urgent orthopedics follow up within 72 hours
C) Emergent hand surgery consultation
D) Performance of bedside incision and drainage
Answer: C
High pressure injection injuries are associated with high morbidity. Devices which spray liquids at high pressure can inject foreign material deep into soft tissue. This causes an inflammatory response and fibrosis which varies based upon the material injected. Paint and paint thinner cause an earlier, more intense inflammatory response and result in a high number of amputations. Grease injuries, on the other hand, cause a less intense inflammatory response and fewer amputations, but more often cause granuloma and fistula formation with loss of function. Symptoms may be minimal immediately after the injury but swelling, vascular compromise and tissue necrosis develop in a matter of hours. X-rays may reveal the extent of spread of radio-opaque material and can show subcutaneous edema. Patients with these injuries should be splinted, given tetanus prophylaxis and broad spectrum antibiotics. The affected extremity should be elevated. Emergent hand surgery consultation is necessary as most cases require extensive surgical decompression and debridement.

This patient should not be admitted to a medical service for intravenous antibiotics (A) without hand surgery consultation as he will likely require surgical debridement. Discharge with urgent orthopedics follow up within 72 hours (B) is inappropriate, as the inflammatory response is likely to progress in a matter of hours. A delay in treatment would likely lead to significant morbidity. Performance of bedside incision and drainage (D) is inappropriate as this patient will require surgical exposure of the deep tissues of the hand to ensure adequate washout.
FOAMed:
References:
- Gonzalez R, Kasdan ML. High pressure injection injuries of the hand. Clin Occup Environ Med. 2006;5(2):407-11, ix.
- Hogan CJ, Ruland RT. High-pressure injection injuries to the upper extremity: a review of the literature. J Orthop Trauma. 2006 Jul;20(7):503-11.
- Loveday I. High-pressure injection injuries. Emerg Nurse. 2007 Nov;15(7):22-3.





