Today on the emDOCs cast with Brit Long, MD (@long_brit), we discuss a challenging case of an upper airway obstruction with Jess Pelletier, MD.
Episode 73: Upper Airway Obstruction Part 1
Case:
60-year-old male who is tachypneic, tripoding, and unable to finish sentences. He has clear lungs with inspiratory and expiratory stridor. His O2 saturation is 100% on 15 L NRB.
Jess was concerned for upper airway obstruction.
What should you look for on exam?
- Supraglottic obstruction causes inspiratory stridor, while narrowing of subglottic structures causes expiratory stridor.
- If stridor is both inspiratory and expiratory, obstruction is likely glottic (Sasidaran, Cohen).
- Other possible symptoms of upper airway obstruction include nasal flaring, tachypnea, hoarseness, and accessory muscle use.
- There may be swelling or erythema of the oropharyngeal structures, or neck masses may be noted on exam.
What are potential etiologies?
- Supraglottic: angioedema or lesions of the tongue, elevation of the tongue due to Ludwig’s angina, neck abscesses (including retropharyngeal abscess), masses, foreign bodies, tonsillar masses, peritonsillar abscesses, masses or edema of the uvula
- Glottic obstruction: epiglottitis, masses, or paralysis of the vocal cords (Eskander).
- Subglottic obstruction: bacterial tracheitis, masses, or subglottic stenosis.
Back to the case…
Jess recommends that he undergo intubation for transfer given how unstable he is. He declines intubation, stating he doesn’t want to be on a ventilator unless he’s “about to die.” She administered methylprednisolone IV, racemic and IM epinephrine, but no improvement. He is able to lie flat for about 30 seconds, enough time to obtain a CT showing a 5 cm mass sitting above his epiglottis.
RSI is chosen as flexible intubating endoscopy was not feasible. Patient preoxygenated and etomidate and rocuronium administered for intubation, but there was a rapid desaturation.
BVM utilized and saturation of 90% obtained. Video laryngoscopy visualized a friable mass completely obstructing the view of the airway. The patient’s saturations dropped.
BVM was again attempted, but saturations drop and patient enters PEA. High-quality CPR started.
Cricothyrotomy performed using a scalpel, bougie, and 6-0 endotracheal tube. Compressions continued and oxygen saturation increased to 80%, followed by ROSC.
Patient underwent tracheostomy, was transferred, and survived neurologically intact. He is undergoing radiation therapy for squamous cell carcinoma.
Jess’s thoughts:
Paralysis and subsequent relaxation of the parapharyngeal tissues caused the mass to completely obstruct this patient’s airway. Supine positioning for RSI likely made this worse. The patient had little to no reserves; his incredible work of breathing was the only thing maintaining his oxygen saturation at 100%. Once paralysis was induced, any semblance of preoxygenation performed with the NRB was lost.
Temporizing with BPAP or HFNC is possible in some patients, but in this case probably wound’t have worked since it was an upper airway obstruction. Transport would have been difficult with this, and he needed a definitive airway.
Guidelines:
2015 Difficult Airway Society (DAS) Guidelines
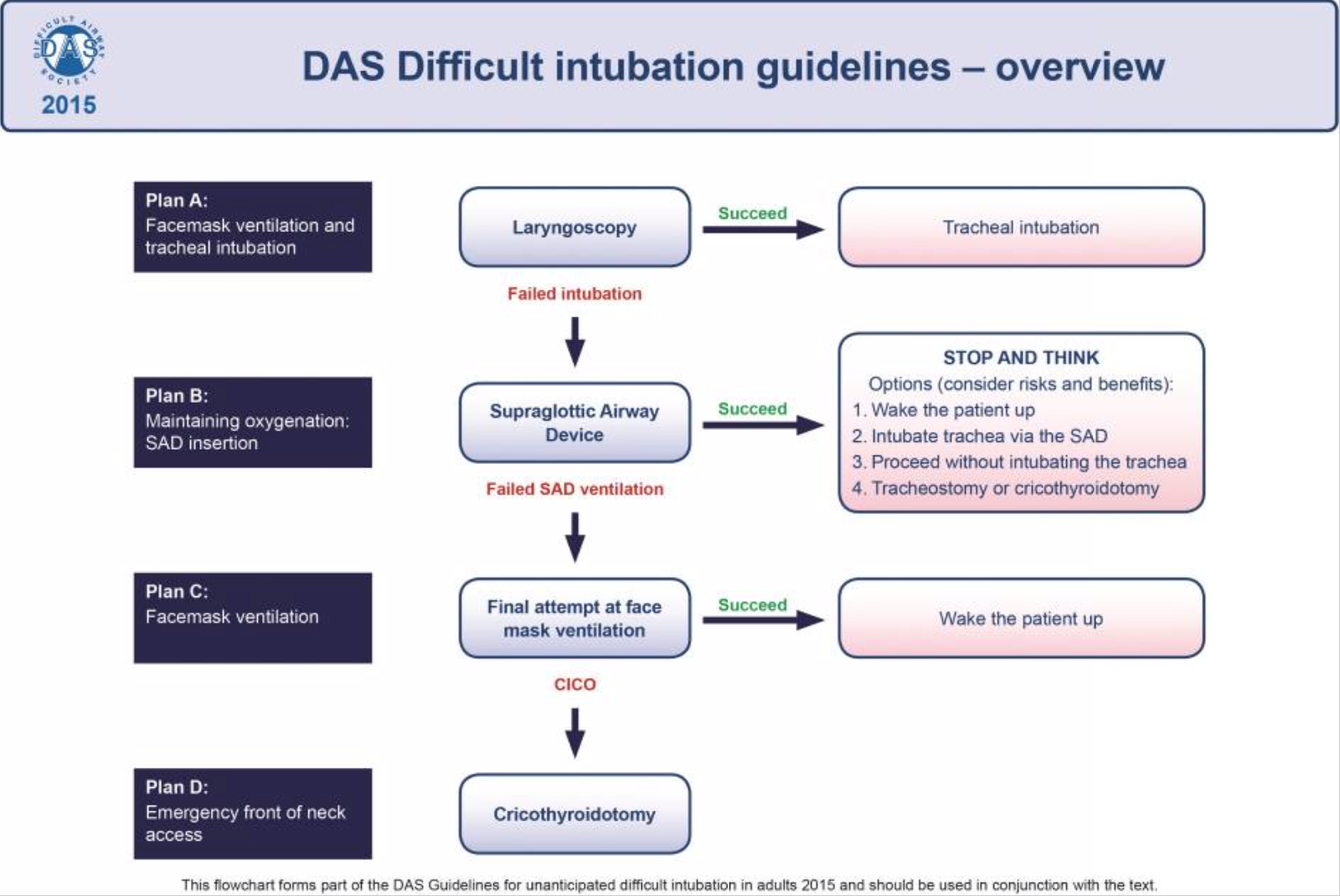
2022 American Society of Anesthesiologists (ASA) Practice Guidelines
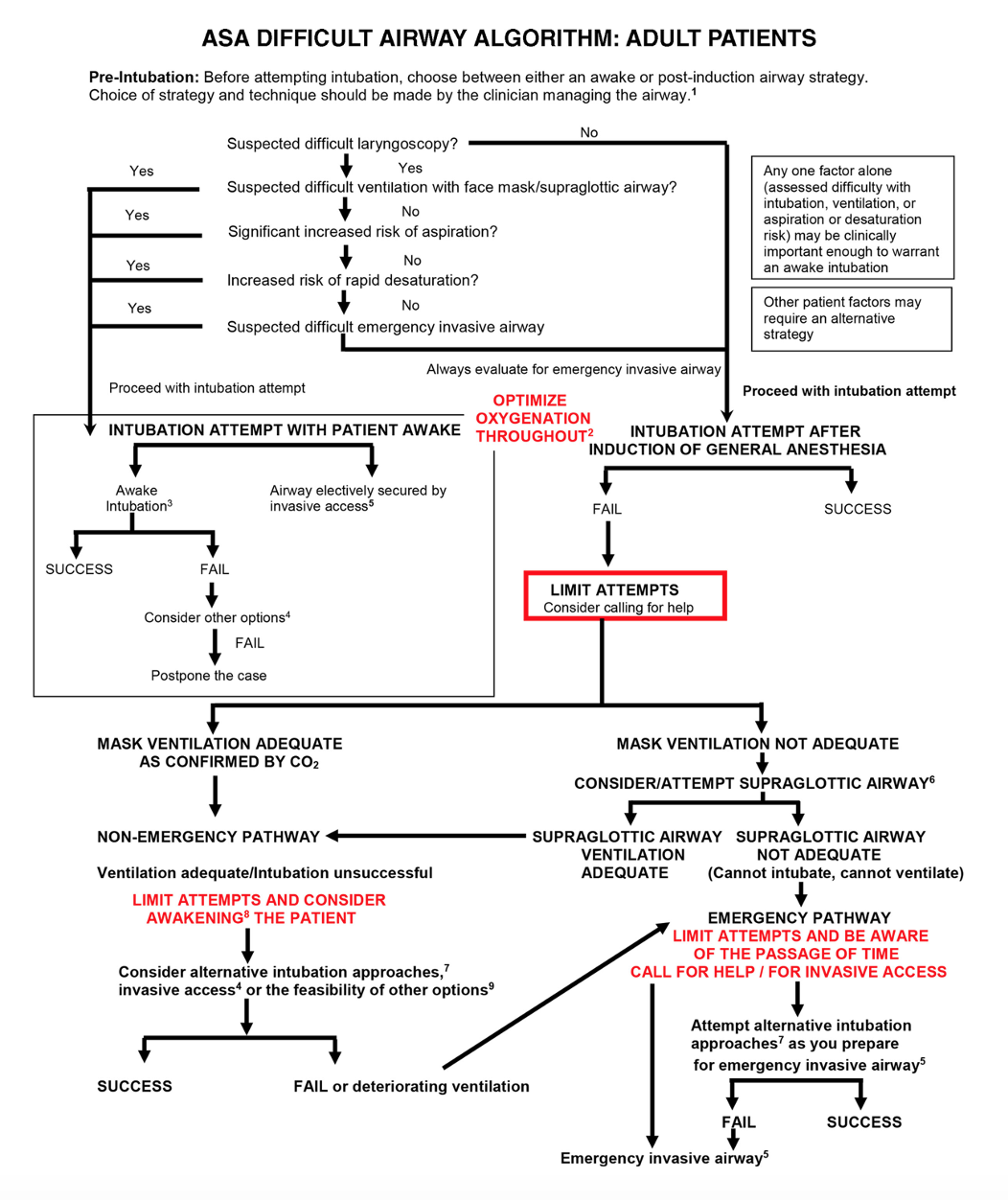
Predicting THE CANNOT INTUBATE, CANNOT VENTILATE (CICV) Scenario
- Physical exam features that can raise concern for a difficult airway: chronic systemic disease, high Mallampati score, male gender, large chest, or neck circumference, head or neck radiation, limited neck range of motion.
- Features associated with difficult face mask ventilation: prior difficult intubation, obesity, presence of facial hair, short neck or large neck circumference.
- Assessments you can perform at bedside: mouth opening, sternomental distance, thyromental distance, upper lip bite test.
- There is no single test that can accurately predict a difficult airway. Always assume the airway will be difficult.
Approach
1. Premark the neck
- Preps team, reduces anxiety
- Use “laryngeal handshake” and identify cricothyroid membrane
- May use POCUS to assist in identifying anatomy
2. Preoxygenation
- Oxygen saturation alone is a poor predictor of the degree of upper airway obstruction; it’s better characterized by respiratory rate and degree of subjective dyspnea.
- Consider BPAP, HFNC for preoxygenation if there is not a complete airway obstruction. Several studies/meta-analyses suggest these improve oxygenation.
- HFNC may have been useful in Jess’s patient.
- Pre-oxygenation could have been optimized by eliminating more dead space with the assistance of positive end expiratory pressure. However, the fact that paralysis caused complete airway obstruction made it impossible to use BVM/face mask ventilation between intubation attempts.
Stay tuned for Part 2, where we cover flexible intubating endoscopy, ramped positioning, seated intubation, supraglottic devices, cricothyrotomy, retrograde intubation, and pearls/pitfalls.
References:
- Sasidaran K, Bansal A, Singhi S. Acute upper airway obstruction. Indian J Pediatr. 2011;78(10):1256-1261.
- Cohen LF. Stridor and Upper Airway Obstruction in Children. Pediatrics In Review. 2000;21(1):4-5.
- Eskander A, de Almeida JR, Irish JC. Acute Upper Airway Obstruction. Longo DL, ed. N Engl J Med. 2019;381(20):1940-1949.
- Frerk C, Mitchell VS, McNarry AF, et al. Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. British Journal of Anaesthesia. 2015;115(6):827-848.
- Apfelbaum JL, Hagberg CA, Connis RT, et al. 2022 American Society of Anesthesiologists Practice Guidelines for Management of the Difficult Airway. Anesthesiology. 2022;136(1):31-81.
- Kristensen MS. Airway management and morbid obesity: European Journal of Anaesthesiology. 2010;27(11):923-927.
- Wong DT, Mehta A, Tam AD, et al. A survey of Canadian anesthesiologists’ preferences in difficult intubation and “cannot intubate, cannot ventilate” situations. Can J Anesth/J Can Anesth. 2014;61(8):717-726.
- Cattano D, Killoran PV, Cai C, et al. Difficult mask ventilation in general surgical population: observation of risk factors and predictors. F1000Res. 2014;3:204.
- Shiga T, Wajima Z, Inoue T, Sakamoto A. Predicting Difficult Intubation in Apparently Normal Patients. Anesthesiology. 2005;103(2):429-437.
- Detsky ME, Jivraj N, Adhikari NK, et al. Will This Patient Be Difficult to Intubate?: The Rational Clinical Examination Systematic Review. JAMA. 2019;321(5):493.
- Shah P, Dubey K, Yadav J. Predictive value of upper lip bite test and ratio of height to thyromental distance compared to other multivariate airway assessment tests for difficult laryngoscopy in apparently normal patients. J Anaesthesiol Clin Pharmacol. 2013;29(2):191.
- Drew T, McCaul CL. Laryngeal handshake technique in locating the cricothyroid membrane: a non-randomised comparative study. British Journal of Anaesthesia. 2018;121(5):1173-1178.
- Campbell M, Shanahan H, Ash S, et al. The accuracy of locating the cricothyroid membrane by palpation – an intergender study. BMC Anesthesiol. 2014;14(1):108.
- Kristensen MS, Teoh WH, Rudolph SS, et al. Structured approach to ultrasound-guided identification of the cricothyroid membrane: a randomized comparison with the palpation method in the morbidly obese. British Journal of Anaesthesia. 2015;114(6):1003-1004.
- Mallin M, Curtis K, Dawson M, et al. Accuracy of ultrasound-guided marking of the cricothyroid membrane before simulated failed intubation. The American Journal of Emergency Medicine. 2014;32(1):61-63.
- Dinsmore J, Heard AM, Green RJ. The use of ultrasound to guide time-critical cannula tracheotomy when anterior neck airway anatomy is unidentifiable: European Journal of Anaesthesiology. 2011;28(7):506-510.
- Malagutti N, Di Laora A, Barbetta C, et al. Is Peripheral Oxygen Saturation a Reliable Predictor of Upper Airways Air-Flow Limitation? J Emerg Med. 2018;55(5):627-634.
- Song J li, Sun Y, Shi Y bo, et al. Comparison of the effectiveness of high-flow nasal oxygen vs. standard facemask oxygenation for pre- and apneic oxygenation during anesthesia induction: a systematic review and meta-analysis. BMC Anesthesiol. 2022;22(1):100.
- Kuo HC, Liu WC, Li CC, et al. A comparison of high-flow nasal cannula and standard facemask as pre-oxygenation technique for general anesthesia: A PRISMA-compliant systemic review and meta-analysis. Medicine. 2022;101(10):e28903.








