Authors: Suresh K. Pavuluri, MD, MPH (EM Resident, The Mount Sinai Hospital, Icahn School of Medicine at Mount Sinai); Benjamin Laraway, MD (EM Resident, The Mount Sinai Hospital, Icahn School of Medicine at Mount Sinai); and Kaushal Shah, MD (Vice Chair of Education, New York Presbyterian Hospital, Weill Cornell Medical College) // Edited by Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
A 56-year-old Taiwanese male with a past medical history of type II diabetes on metformin, hypertension, and hyperlipidemia presents to the ED with right upper quadrant (RUQ) pain for the past two days. He complains of fever, chills, and nausea, but no vomiting. He has no past surgical history. Currently, he denies any vomiting, diarrhea, dysuria, or hematuria. He’s a social drinker, but has never smoked.
Vitals: T 38.8 C, HR 103, BP 110/80, RR 20, SpO2 96% RA, and POC glucose 154
Physical exam reveals a middle-aged male who appears uncomfortable, with localized tenderness to the RUQ. Exam is otherwise normal.
Point-of-care ultrasound of the RUQ reveals the following:

Figure 1: sonographic finding of the RUQ shows anechoic regions separated by a hyperechoic border1. From Fernandez, L. Figure 3, Hepatic Amebic Abscess. Sonoworld. https://sonoworld.com/CaseDetails/Hepatic_Amebic_Abscess.aspx?ModuleCategoryId=643
Based on the patient’s presentation, history of diabetes, immigration from an endemic region, and your POCUS, you place hepatic abscess high on your differential. Given that the patient meets SIRS criteria, you decide to immediately draw labs, blood cultures, start fluids, and order antibiotics. After these interventions, you send out consults to Surgery and Interventional Radiology.
History & Risk Factors
In the ED, RUQ pain has almost become pathognomonic for biliary pathology. Unlike the more common biliary processes, hepatic abscess can be an insidious cause of a patient’s presentation. Among all intraabdominal abscesses, hepatic abscesses account for merely 13%2. Despite their low prevalence of 2.3 cases per 100,000 in North America3, liver abscesses are associated with a 10-40% mortality rate4; therefore, it is imperative to diagnose and to treat the condition promptly. Though different pathophysiological mechanisms underlie their formation, certain patient risk factors should alert a clinician to consider hepatic abscess.
The average age of presentation for pyogenic hepatic abscess is >57 years6, with males affected at twice the rate as females7. Immunocompromised patients such as diabetics, cirrhotics, patients undergoing chemotherapy, patients who have received transplants, patients on immunosuppression therapy, or patients with immunological deficiencies are at a higher risk for developing hepatic abscesses6-9. In addition, patients with recent abdominal surgery; penetrating wounds to the abdomen; or recent traveled to or emigrated from certain parts of Asia (e.g., India, Taiwan), Africa, Central or South America are also at an increased risk for hepatic abscesses10,11.
Pathophysiology
To better conceptualize the pathophysiology of hepatic abscesses, hepatic abscesses can be classified into infectious, iatrogenic, or malignancy-associated12. Infectious liver abscesses can form via direct spread of infection from adjacent abdominal pathologies13-15, via hematogenous seeding from systemic or intra-abdominal infections, or by spread of infection through the portal venous system from intra-abdominal infections such as diverticulitis or appendicitis. Amongst the different pathophysiological mechanisms, the most common way of forming hepatic abscesses is through direct spread from the biliary tree12, resulting in pyogenic infection. Gallstone disease, strictures, or malignancy can lead to obstruction, bacterial proliferation through the biliary tract (a cause of ascending cholangitis), and eventual hepatic abscess formation12.
Most infectious causes of hepatic abscesses involve a mixed group of microorganisms. Escherichia coli, Klebsiella pneumoniae, Bacteroides, enterococci, anaerobic streptococci, or microaerophilic streptococci are typically the most common organisms13,16. The three most common causative organisms of hepatic abscesses via hematogenous spread are Staphylococci, hemolytic streptococci, and Streptococcus milleri16.
Extraintestinal liver manifestations of amebiasis, caused by the protozoan Entamoeba histolytica, are also common. It is theorized that the protozoan ascends through the portal venous system to establish an infection in the liver17. Though the factors that result in invasive amebiasis are not fully understood, patients with compromised cell-mediated immunity are more susceptible to invasive amebiasis18.
Hepatic abscesses can be formed via secondary infection of a primary liver tumor or from liver metastases12. Procedures such as transarterial chemoembolization (TACE) or radiofrequency ablation (RFA) used in cases of inoperable hepatocellular carcinoma can also result in hepatic abscesses19-23. TACE induces an area of necrosis within a tumor, which can serve as a nidus for an infection. Other procedures such as biliary stenting have also been shown to cause hepatic abscesses24,25. In about 15% of hepatic abscesses, no identifiable cause is found40.
Clinical Presentation
Patient presentation may vary based on the age of the patient and the underlying etiology of the hepatic abscess. With amebic liver abscesses, patients may have symptoms for days or weeks and may or may not appear chronically ill42-45. Patients with multiple liver abscesses may have acute and more pronounced systematic symptoms compared to those with a single abscess40. Moreover, elderly patients typically present with more occult symptoms than younger patients40.
Most liver abscess patients typically present with fever (seen in 90%-92% patients) and/or abdominal symptoms such as RUQ pain, tenderness, or guarding (seen in ~50%-75% of patients)13,14,25-27. Patients with amebic liver abscesses tend to present more with abdominal pain than those with bacterial liver abscesses51. Fevers tend to be waxing and waning in nature and may be accompanied with nocturnal sweating. About 50% of patients with liver abscesses may have hepatomegaly or jaundice,27 with the latter more common in bacterial liver abscesses51. Moreover, some patients may experience constitutional symptoms of nausea, vomiting, fatigue, malaise, and anorexia or weight loss, whereas others may not even have any abdominal pain.
Because the symptoms of a liver abscess can be non-specific in nature, it is important to obtain detailed medical and surgical histories. Inevitably, having a high-index of suspicion while risk stratifying a patient based on their history and physical exam findings is critical for diagnosis.
Evaluation
Laboratory Studies
For hepatic abscesses, laboratory tests are neither specific nor diagnostic. As per routine management, blood cultures should be obtained in all patients in whom hepatic abscess is considered. Though they are positive in only half of the patients, they may help guide antibiotic therapy13,28. Normocytic, normochromic anemia, leukocytosis, elevated erythrocyte sedimentation rate (ESR), and hyperbilirubinemia with or without jaundice may also be noted. Serum transaminases may be elevated, but to a lesser extent than serum alkaline phosphatase (seen in 90% of patients)13,14,27. Though bacterial and amebic causes of hepatic abscesses may have similar findings, there are certain markers that point toward an amebic abscess. Lodhi, et al found that mean albumin level was lower in bacterial liver abscesses than in amebic ones51. Unlike most other parasitic infections, eosinophilia is characteristically absent in amebiasis, so it should not be used as a diagnostic marker to exclude amebic abscess49. If a patient is at high-risk for amebiasis, stool cultures and/or serologic testing such as indirect hemagglutination (IHA) for Entamoeba histolytica may be diagnostic46-48,50,51. IHA titers may remain positive several years after infection. In Lodhi, et al IHA titers of 1:32 were found in patients with pyogenic abscesses indicating prior amebiasis whereas titers of 1:256 pointed toward pyogenic abscesses.51
Imaging
For liver abscesses, ultrasound of the RUQ is typically the first diagnostic modality, given its convenience, lack of exposure to radiation, and cost-effectiveness in most EDs29. However, CT scan of abdomen with IV contrast (preferably) confers greater sensitivity (85% vs. 95%) and can be utilized if ultrasound is non-diagnostic30,31. An MRI may also be utilized in certain populations (i.e., pregnant patients), but its relative high cost and lack of access make it a less-utilized option32. Though there are different imaging modalities to diagnose hepatic abscesses, it is not possible to distinguish between the different types (i.e., bacterial vs amebic) on imaging alone33. Having a high-index of suspicion, risk stratifying a patient based on history, and/or serological testing may help distinguish bacterial hepatic abscesses from amebic ones.
On ultrasound of the RUQ, abscesses can look hypoechoic or hyperechoic and may have septations or debris (see Figure 2).
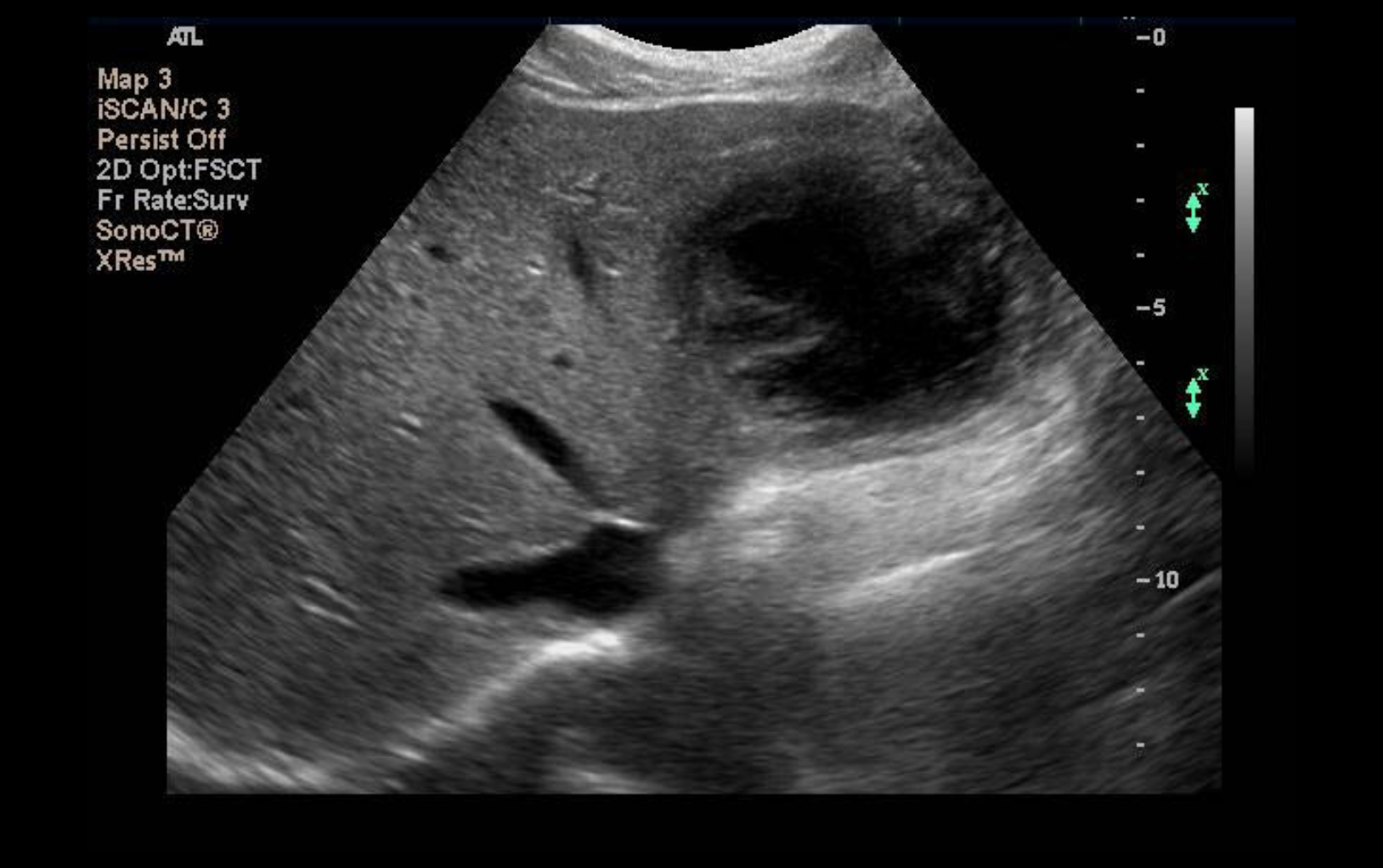
Figure 2: A rounded lesion is seen on the left lobe of the liver with an anechoic center and a hazy, irregular border. This particular patient was diagnosed with amebiasis, but there is no definitive way distinguishing amebiasis vs. other causes of hepatic abscess1. From Fernandez, L. Figure 3, Hepatic Amebic Abscess. Sonoworld. https://sonoworld.com/CaseDetails/Hepatic_Amebic_Abscess.aspx?ModuleCategoryId=643
On contrast-enhanced CT scan, a “double target sign” where a low-attenuation fluid area is surrounded by high-attenuation inner ring and a low-attenuation outer ring can be seen32,34,35. The inner ring contains the fluid-filled contents of the abscess, and the outer ring encompasses the parenchymal edema32. Sometimes a “cluster sign” where a hepatic abscess is surrounded by other small abscesses may also be seen (see Figure 3)36-38. Once a pyogenic liver abscess is confirmed on imaging, prompt treatment with broad-spectrum antibiotics is needed, as well as consultation with IR and surgery.
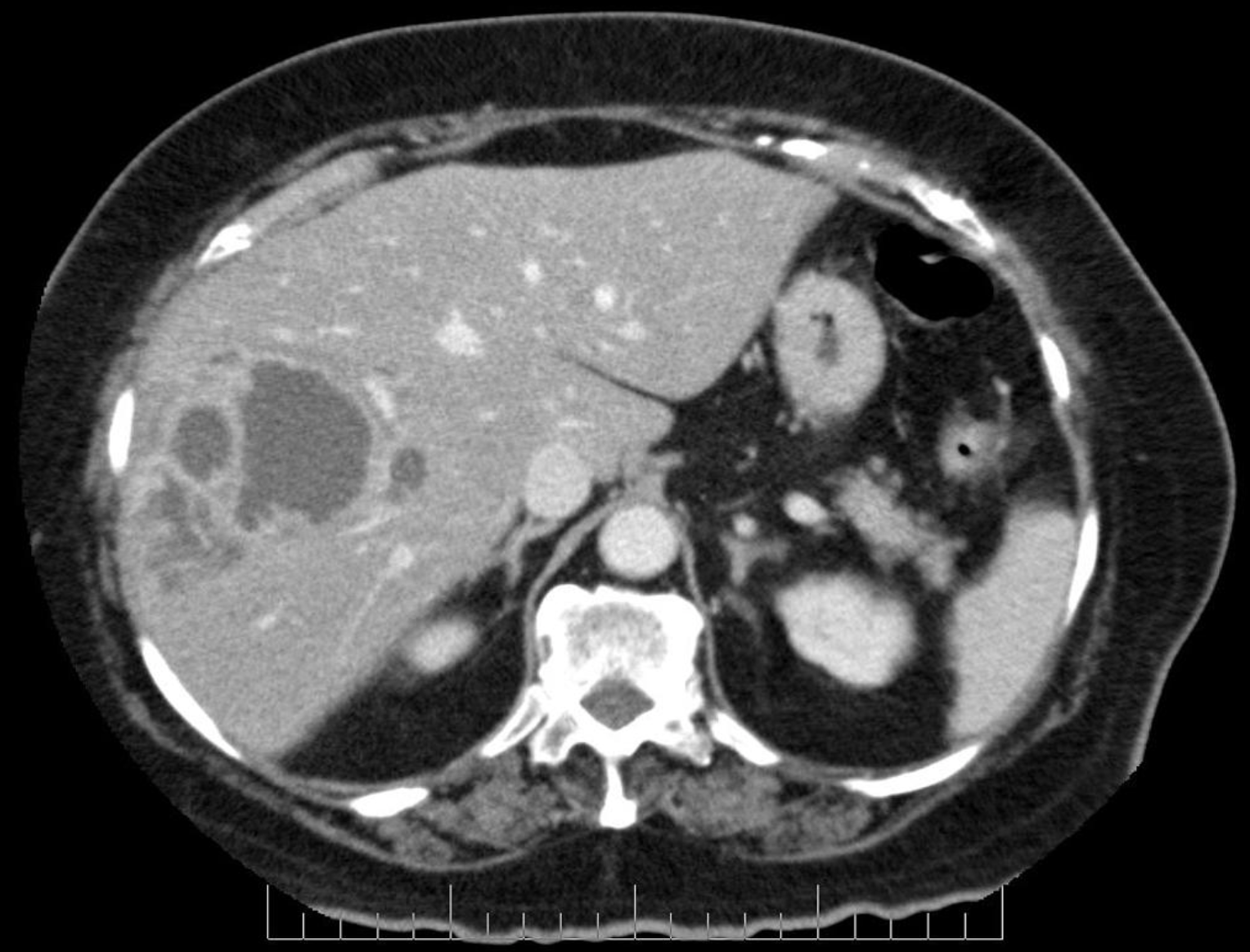
Figure 3: hepatic abscess with a double target sign, where abscesses are separated by inner ring of fluid-filled content and an outer ring encompassing the parenchymal edema. Case courtesy of Dr Laughlin Dawes, Radiopaedia.org, rID: 35962
Treatment
In the ED, patients with hepatic abscesses may present with a wide-range in acuity: some may be acutely septic, and others may have a more sub-acute presentation. Treatment is based on the size of the abscess, whether it has ruptured, underlying etiology, and whether the abscess is multi-loculated or uni-loculated. Generally, for all patients with hepatic abscesses, broad-spectrum antibiotic therapy should be initiated as soon as blood cultures are drawn37.
For abscesses < 3 cm, antibiotic therapy alone may be sufficient38. However, the gold standard treatment for hepatic abscesses is percutaneous drainage37,38. For unilocular abscesses measuring > 3-5 cm, percutaneous drainage is the first treatment of choice. If the first attempt at percutaneous drainage fails to resolve the abscess, a second attempt is reasonable, but surgical resection is also an option38. For multilocular abscesses measuring > 3-5 cm, surgical drainage or resection has been found to be the most effective treatment modality38. For ruptured abscesses, surgical treatment is recommended38,39.
As most hepatic abscesses are polymicrobial in nature, broad-spectrum coverage that includes gram-positive, gram-negative, and anaerobes should be initiated. Zosyn, metronidazole, and/or clindamycin is recommended12,51. For highly-resistant organisms, carbapenems can be used as a monotherapy followed by fluoroquinolones for long-term parenteral therapy. Treatment duration is based on clinical picture, response to treatment, as well as serial US examination of the size of abscess(es). Typically, IV antibiotics are used for 1-3 weeks followed by PO antibiotics for 2-3 months until the resolution of the fever, leukocytosis, and documented evidence of resolution of abscesses via ultrasound12. For amebic abscesses, 10-day antiprotozoal therapy alone may be sufficient52-54. Typically, therapeutic aspiration is reserved for large abscesses, those that are non-responsive to pharmacological therapy, enlarging abscesses, or those at high-risk for rupture55.
Take Home Points
- Hepatic abscesses are associated with a high-mortality rate. Prompt recognition and resuscitation are paramount in successfully treating this disease entity.
- CT with contrast is the diagnostic modality of choice, but abscesses may also be seen on ultrasound.
- Broad-spectrum antibiotic coverage that includes gram-positives, gram-negatives, and anaerobes as well as anti-protozoal therapy for suspected amebic abscesses is important.
- Ultimately, percutaneous drainage or surgical drainage may be needed along with IV antibiotics for 1-3 weeks and PO antibiotics for 1-2 months or until resolution of clinical symptoms such as fever and resolution of abscess(es) on repeat ultrasound.
References/Further Reading
- Fernandez, L. Figure 3, Hepatic Amebic Abscess. Sonoworld. https://sonoworld.com/CaseDetails/Hepatic_Amebic_Abscess.aspx?ModuleCategoryId=643
- Altemeier WA, Culbertson WR, Fullen WD, Shook CD. Intra-abdominal abscesses. Am J Surg 1973; 125:70.
- Lin YT, Liu CJ, Chen TJ, Chen TL, Yeh YC, Wu HS, et al. Pyogenic liver abscess as the initial manifestation of underlying hepatocellular carcinoma. Am J Med. 2011;124:1158–1164. doi: 10.1016/j.amjmed.2011.08.012
- Law ST, Li KK. Is hepatic neoplasm-related pyogenic liver abscess a distinct clinical entity? World J Gastroenterol. 2012;18:1110–1116. doi: 10.3748/wjg.v18.i10.1110.
- Lee KT, Wong SR, Sheen PC. Pyogenic liver abscess: an audit of 10 years’ experience and analysis of risk factors.Dig Surg. 2001; 18(6):459-65; discussion 465-6.
- Tian LT, Yao K, Zhang XY, Zhang ZD, Liang YJ, Yin DL, et al. Liver abscesses in adult patients with and without diabetes mellitus: an analysis of the clinical characteristics, features of the causative pathogens, outcomes and predictors of fatality: a report based on a large population, retrospective study in China. Clin Microbiol Infect. 2012;18:E314–E330. doi: 10.1111/j.1469-0691.2012.03912.x.
- Lee KT, Wong SR, Sheen PC. Pyogenic liver abscess: an audit of 10 years’ experience and analysis of risk factors. Dig Surg. 2001;18:459–465. discussion 465-466. doi: 10.1159/000050194.
- Mølle I, Thulstrup AM, Vilstrup H, Sørensen HT. Increased risk and case fatality rate of pyogenic liver abscess in patients with liver cirrhosis: a nationwide study in Denmark. Gut. 2001;48:260–263.doi: 10.1136/gut.48.2.260
- Eltawansy SA, Merchant C, Atluri P, Dwivedi S. Multi-organ failure secondary to a Clostridium perfringens liver abscess following a self-limited episode of acute gastroenteritis. Am J Case Rep. 2015;16:182–186. doi: 10.12659/AJCR.893046.
- Trump DL, Fahnestock R, Cloutier CT, Dickman MD. Anaerobic liver abscess and intrahepatic metastases: a case report and review of the literature. 1978 Feb; 41(2):682-6.
- Jorge JF, Costa AB, Rodrigues JL, Girão ES, Luiz RS, Sousa AQ, Moore SR, Menezes DB, Leitão TM. Salmonella typhi liver abscess overlying a metastatic melanoma. Am J Trop Med Hyg. 2014 Apr; 90(4):716-8
- Mavilia, M. G., Molina, M., & Wu, G. Y. (2016). The Evolving Nature of Hepatic Abscess: A Review. Journal of Clinical and Translational Hepatology,4(2), 158-168. doi:10.14218/JCTH.2016.00004
- Huang CJ, Pitt HA, Lipsett PA, Osterman FA Jr, Lillemoe KD, Cameron JL, Zuidema GD. Pyogenic hepatic abscess. Changing trends over 42 years. Ann Surg. 1996;223(5):600.
- Rahimian J, Wilson T, Oram V, Holzman RS. Pyogenic liver abscess: recent trends in etiology and mortality. Clin Infect Dis. 2004;39(11):1654.
- Lam YH, Wong SK, Lee DW, Lau JY, Chan AC, Yiu RY, Sung JJ, Chung SS. ERCP and pyogenic liver abscess. Gastrointest Endosc. 1999;50(3):340.
- Carpenter, C and Gilpin, N. Hepatic Abscess. POC-IT Guides. John Hopkins ABX, HIV, Diabetes and Psychiatry.
- K. Aikat, S. R. Bhusnurmath, A.K. Pal, P.N. Chhuttani, D.V. Datta. The pathology and pathogenesis of fatal hepatic amoebiasis—a study based on 79 autopsy cases. 1979; 73(2): 188-192. Transactions of the Royal Society of Tropical Medicine and Hygiene. doi.org/10.1016/0035-9203(79)90209-8
- Park WB, Choe PG, Jo JH, Kim SH, Bang JH, Kim HB, Kim NJ, Oh MD, Choe KW. Amebic liver abscess in HIV-infected patients, Republic of Korea. 2007; 13(3): 516-7. Emerging Infectious Diseases. doi: 3201/eid1303.060894.
- Shin JU, Kim KM, Shin SW, Min SY, Park SU, Sinn DH, et al. A prediction model for liver abscess developing after transarterial chemoembolization in patients with hepatocellular carcinoma. Dig Liver Dis. 2014;46:813–817. doi: 10.1016/j.dld.2014.05.003.
- Huang SF, Ko CW, Chang CS, Chen GH. Liver abscess formation after transerterial chemoembolization for malignant hepatic tumor. Hepatogastroenerology. 2003;50:1115–1118.
- Iida H, Aihara T, Ikuta S, Yamanaka N. Risk of abscess formation after liver tumor radiofrequency ablation: A review of 8 cases with a history of enterobiliary anastomosis. Hepatogastroenterology. 2014;61:1867–1870.
- Elias D, Di Pietroantonio D, Gachot B, Menegon P, Hakime A, De Baere T. Liver abscess after radiofrequency ablation of tumors in patients with a biliary tract procedure. Gastreoenterol Clin Biol. 2006;30:823–827. doi: 10.1016/S0399-8320(06)73327-9.
- Hoffmann R, Rempp H, Schmidt D, Pereira PL, Claussen CD, Clasen S. Prolonged antibiotic prophylaxis in patients with bilioenteric anastomosis undergoing percutaneous radiofrequency ablation. J Vasc Interv Radiol. 2012;23:545–551. doi: 10.1016/j.jvir.2011.12.025.
- Montvuagnard T, Thomson V, Durieux M, Mabrut JY, Marion-Audibert AM., Berthezene Y, et al. Superinfection of focal liver lesions after bile duct procedures. Diagn Interv Imaging. 2012;93:e191–e195.doi: 10.1016/j.diii.2012.01.001.
- Huang RJ, Ambrosy AP, Triadafilopoulos G. Hepatic abscess with biliary communication following transarterial chemoembolization of hepatocellular carcinoma. Dig Dis Sci. 2013;58:2463–2465. doi: 10.1007/s10620-013-2593-1.
- Mohsen AH, Green ST, Read RC, McKendrick MW. Liver abscess in adults: ten years experience in a UK centre. QJM 2002; 95:797.
- Rubin RH, Swartz MN, Malt R. Hepatic abscess: changes in clinical, bacteriologic and therapeutic aspects. Am J Med 1974; 57:601.
- Chemaly RF, Hall GS, Keys TF, Procop GW. Microbiology of liver abscesses and the predictive value of abscess gram stain and associated blood cultures. Diagn Microbiol Infect Dis 2003; 46:245.
- Zaleznik, DF, Kasper, DL. Intra-abdominal abscesses. In: Gastrointestinal Infections: Diagnosis and Management, Lamont, JT (Ed), Marcel Dekker, New York 1997. p.397.
- Halvorsen RA, Korobkin M, Foster WL, et al. The variable CT appearance of hepatic abscesses. AJR Am J Roentgenol 1984; 142:941.
- Lin AC, Yeh DY, Hsu YH, et al. Diagnosis of pyogenic liver abscess by abdominal ultrasonography in the emergency department. Emerg Med J 2009; 26:273.
- Bächler P, Baladron MJ, Menias C, et al. Multimodality Imaging of Liver Infections: Differential Diagnosis and Potential Pitfalls. Radiographics 2016; 36:1001.
- Lodhi S, Sarwari AR, Muzammil M, et al. Features distinguishing amoebic from pyogenic liver abscess: a review of 577 adult cases. Trop Med Int Health 2004; 9:718.
- Skucas J. Advanced imaging of the abdomen. Springer Verlag. (2006) ISBN:1852339926.
- Mathieu D, Vasile N, Fagniez PL et-al. Dynamic CT features of hepatic abscesses. Radiology. 1985;154 (3): 74-52. doi:10.1148/radiology.154.3.3969480
- Jeffrey RB, Tolentino CS, Chang FC et-al. CT of small pyogenic hepatic abscesses: the cluster sign. AJR Am J Roentgenol. 1988;151 (3): 487-9. doi:10.2214/ajr.151.3.487
- Lardière-Deguelte S, Ragot E, Armoun K, Piardi T, Dokmak S, Bruno O, et al. Hepatic abscess: diagnosis and management. J Visc Surg. 2015;152:231–243. doi: 10.1016/j.jviscsurg.2015.01.013.
- Hope WW, Vrochides DV, Newcomb WL, Mayo-Smith WW, Iannitti DA. Optimal treatment of hepatic abscess. Am Surg. 2008;74:178–182.
- Tan YM, Chung AY, Chow PK, Cheow PC, Wong WK, Ooi LL, et al. An appraisal of surgical and percutaneous drainage for pyogenic liver abscesses larger than 5 cm. Ann Surg. 2005;241:485–490. doi: 10.1097/01.sla.0000154265.14006.47.
- Krige JE, Beckingham IJ. ABC of diseases of liver, pancreas, and biliary system. BMJ 322: 537-540, 2001.
- Knobloch J, Mannweiler E. Development and persistence of antibodies to Entamoeba histolytica in patients with amebic liver abscess. Analysis of 216 cases. Am J Trop Med Hyg 1983; 32:727.
- Peterson KM, Singh U, Petri WA Jr. Enteric Amebiasis. In: Tropical Infectious Diseases: Principles, Pathogens and Practice, 3rd ed, Guerrant R, Walker DH, Weller PF (Eds), Saunders Elsevier, Philadelphia 2011. p.614.
- Nespola B, Betz V, Brunet J, et al. First case of amebic liver abscess 22 years after the first occurrence. Parasite 2015; 22:20.
- Hoffbrand BI. Amoebic liver abscess presenting thirty-two years after acute amoebic dysentery. Proc R Soc Med 1975; 68:593.
- Lachish T, Wieder-Finesod A, Schwartz E. Amebic Liver Abscess in Israeli Travelers: A Retrospective Study. Am J Trop Med Hyg 2016; 94:1015.
- Peterson KM, Singh U, Petri WA Jr. Enteric Amebiasis. In: Tropical Infectious Diseases: Principles, Pathogens and Practice, 3rd ed, Guerrant R, Walker DH, Weller PF (Eds), Saunders Elsevier, Philadelphia 2011. p.614.
- Adams EB, MacLeod IN. Invasive amebiasis. I. Amebic dysentery and its complications. Medicine (Baltimore) 1977; 56:315.
- Katzenstein D, Rickerson V, Braude A. New concepts of amebic liver abscess derived from hepatic imaging, serodiagnosis, and hepatic enzymes in 67 consecutive cases in San Diego. Medicine (Baltimore) 1982; 61:237.
- Leder, K, Weller, PF. Extraintestinal Entamoeba histolytica amebiasis. UpToDate. 2018.
- Pritt BS, Clark CG. Amebiasis. Mayo Clin Proc 2008; 83:1154.
- Lodhi, S, Sarwari, AR, Muzammil, M, Salam, A, Smego, RA. Features distinguishing amoebic from pyogenic liver abscess: a review of adult cases. Tropical Medicine and International Health. 2004.
- Abuabara, SF, Barrett, JA, Hau, T et al.Amebic liver abscess. 1982. Archives of Surgery 117, 239– 244.
- Katzenstein D, Rickerson V & Braude A. New concerpts of amebic liver abscess derived from hepatic imaging, serodiagnosis and hepatic enzymes in 67 consecuitve cases in San Diego. 1982. Medicine 61, 237-246.
- Conter RL, Pitt HA, Tompkins RK et al. Differentiation of pyogenic from amoebic hepatic abscesses. 1986. Surgical Gynecology and Obstetrics 162, 114-120.
- Saraswat VA, Agarwal DK, Baijal SS, Roy S, Choudhuri G, Dhiman RK, Bhandari L, Naik SR. Percutaneous catheter drainage of amoebic liver abscess. Clinical Radiology. 1992 Mar; 45(3): 187-9.








