Authors: Daniel Bak, MD and Matthew Siket, MD, MSc, FACEP (Division of Emergency Medicine, Department of Surgery, Robert Larner College of Medicine at the University of Vermont) // Reviewed by: Andrew Grock, MD (Greater LA VA Hospital Center and David Geffen School of Medicine at UCLA); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Case
A 79-year-old woman with a past medical history of hypertension and atrial fibrillation, on apixaban, is brought in by ambulance for sudden onset headache with right-sided hemiparesis beginning 1 hour prior to arrival. She denies a history of similar symptoms and family members, who witnessed symptom onset, deny trauma or seizure activity.
Vitals: BP 210/100, HR100, RR 18, Temp 37.6, SpO2 98%
On exam, she is awake, protecting her airway, confused with a Glasgow Coma Scale (GCS) of 13 (E4, V4, M5), and had a NIH Stroke Scale of 10. Initial labs (CBC, electrolytes, creatinine, glucose and coagulation studies) are drawn, fingerstick glucose is 110 mg/dl, and the patient is sent for an emergent non-contrast computed tomography (NCCT) of the brain.
The CT scan unfortunately reveals a hemorrhage in the region of left putamen, approximately <30 cc by volume, without evidence of intra-ventricular hemorrhage (IVH).
Background
Intracerebral hemorrhage (ICH), also known as hemorrhagic stroke, is both common and deadly. ICH accounts for only one fifth of all strokes but has a mortality rate approaching 50% and an even higher rate of permanent disability. As such, ICH can be an intimidating disease process even for the most experienced clinicians. This article seeks to clarify the approach to diagnosis, emphasize the key points of clinical management, and improve disease-specific communication with patients and families.
Presentation, Initial Evaluation, and Diagnosis
Historical clues for ICH include focal neurologic deficits or stroke-like symptoms. Compared to ischemic strokes, ICH is more likely to present with vomiting, elevated blood pressure, severe headache, and decreased consciousness, though none of these clinical findings are specific1. Examination commonly reveals a focal neuro deficit in a stroke-like distribution. Patients may also present with decreased level of consciousness, obtundation and coma.
ICH risk factors include advanced age, hypertension, alcohol, smoking, vascular malformations, anticoagulant use and cerebral amyloid angiopathy (CAA). The heritability of ICH is estimated to be 44%, though few genes have been identified. Apolipoprotein E is one known genetic risk factor associated with CAA2.
As usual, the evaluation begins with the primary survey – evaluating the ABCs and GCS, obtaining intravenous access, placing the patient on a monitor, and adding exogenous oxygen if indicated. Next, is the more detailed secondary survey which includes a thorough neurological examination. ICH patients require careful airway assessment, as their changing mental status may result in coma, obtundation, or loss of airway protective reflexes. As a general guide, intubation should be considered in any ICH patient with a GCS < 8.
For suspected ICH, neuroimaging should be obtained as quickly as possible with NCCT being the diagnostic gold standard. Initial labs typically include a complete blood count (CBC), basic or complete metabolic panel (BMP/CMP), a rapid fingerstick glucose, coagulation studies, and a type and screen. The NIHSS may be helpful in grading symptom severity and prognostic tools such as the ICH score provide valuable prognostic information3.
Pearl – In cases of deep ICH – think Hypertension
Hypertension can lead to rupture of small penetrating arterioles, often in the brainstem, cerebellum, basal ganglia and thalamus. Markedly elevated Mean Arterial Pressure (MAP) leads to failure of the protective cerebral autoregulatory mechanisms. Recent trials have investigated early aggressive blood pressure reduction (ATACH I and II, INTERACT I and II) have not consistently demonstrated superiority of targeting a goal SBP<140 mmHg compared to <180 mmHg4,5. Current consensus suggests a reasonable approach of aiming for an SBP<160 mmHg. First-line agents are Labetalol (10-20mg IVP) and Nicardipine (5mg/hr titrated to goal).
Pearl – In cases of superficial/peripheral ICH – think Cerebral Amyloid Angiopathy
Cerebral amyloid angiopathy related ICH accounts for 5–20% of all spontaneous ICH. CAA is caused by the deposition of amyloid-β (Aβ) in small to medium sized cortical and leptomeningeal arteries. Destruction of the vessel wall over time increases risk of hemorrhage, which is most often superficial. CAA typically affects people 60-90 years of age. While hypertension does not increase the risk of CAA, it does increase the risk of CAA related ICH6.
Additional Imaging
Once ICH is diagnosed, the vasculature can be evaluated by CT angiography or digital subtraction angiography. While not routinely necessary in the ED, these imaging studies may be of diagnostic utility to neurologists and neurosurgeons on a case-by-case basis. The location, size and characteristics of a bleed may be used to estimate the likelihood of hematoma expansion, surgical complications, and poor outcome3.
Prognosis Features
ICH Score
The ICH score can grade severity and predict 30-day mortality. The score is easy to use and based on: GCS, age, ICH volume, IVH and hemorrhage origin. The ICH score can aid in communication and standardization of care, however, creators warn against its use in precisely predicting outcome, as early withdrawal of care for severe ICH can serve as a self-fulfilling prophecy7.
Hematoma Volume
Hematoma volume can be calculated from CT imaging using the ABC/2 technique8.
A: Largest diameter of hematoma in CT slice where hematoma is largest
B: Largest diameter perpendicular to “A” in same CT slice
C: (Number of CT slices that include hematoma) X (thickness of CT slice)
2: Factor to approximate ellipsoid shape of hematoma

Hematoma volume, when combined with GCS, is a strong predictor of 30-day mortality. Parenchymal hemorrhage volume ≥60 cm3 and GCS 8 or less predicted a 30-day mortality of 91%. Alternatively, hemorrhage volume <30 cm3 and a GCS 9 or more predicted a 30-day mortality of 19%10.
Hematoma Expansion
Hematoma expansion from baseline is of particular concern because it is associated with early clinical deterioration. The risk of hematoma expansion is greatest immediately following the onset of symptoms. Other predictors of hematoma expansion are large hemorrhage volume on initial imaging and use of anticoagulants or antiplatelets11.
Spot Sign
The “spot sign” occurs with contrast extravasation into hematoma resulting in a bright spot within the hematoma on CTA. The spot sign may represent active bleeding and is a predictor of hematoma expansion and poor outcome3. The spot sign is also associated with higher rates of surgical complications like intraoperative bleeding, post-operative rebleeding and residual hematoma12.
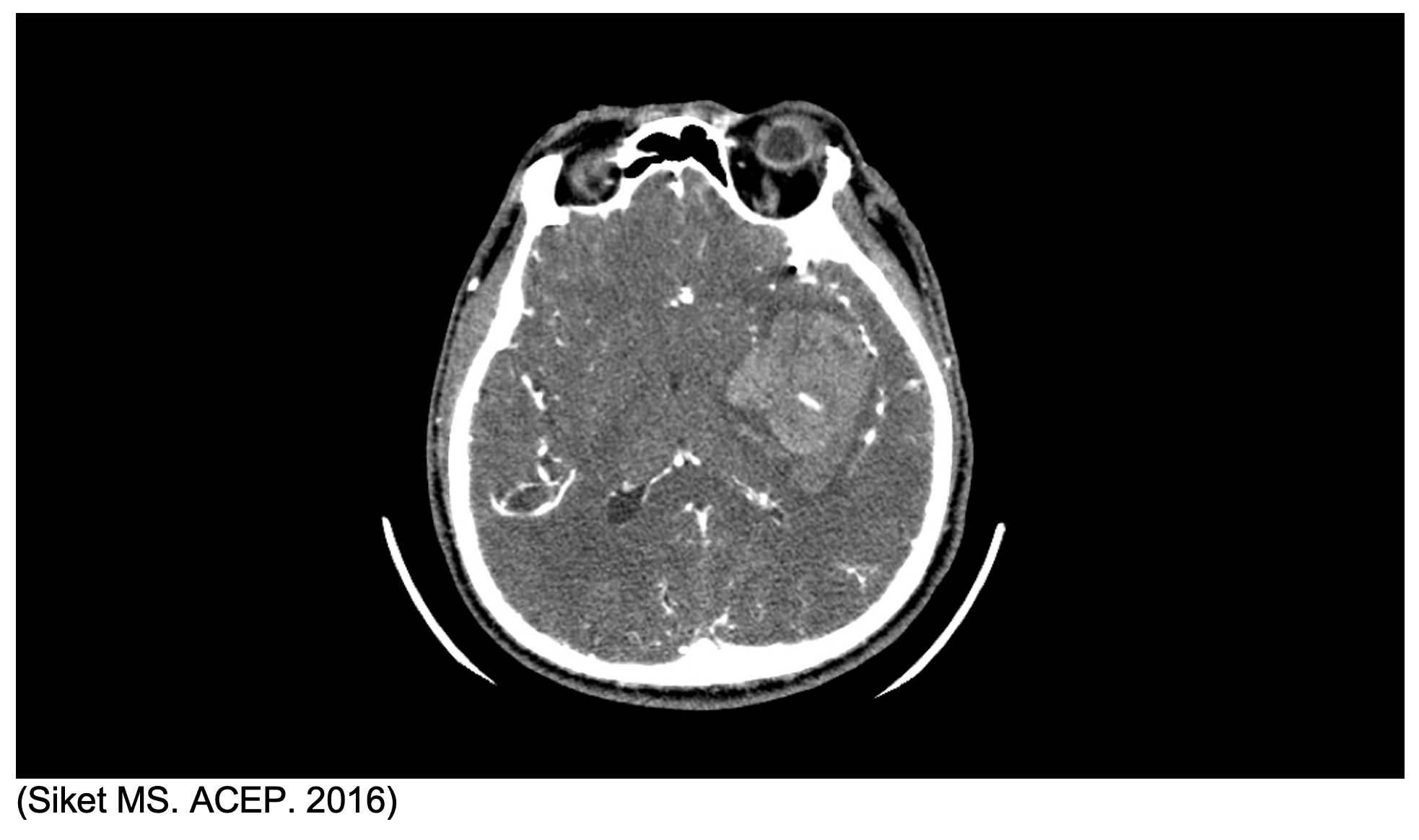
Intraventricular Hemorrhage
Intraventricular hemorrhage (IVH) results from hematoma expansion into ventricles and occurs in half of all cases of ICH. Thalamic and caudate bleeds, as well as larger bleeds, are most likely to result in IVH.Spontaneous decompression of hematoma into ventricles, once hypothesized to improve outcomes, is actually associated with worse clinical outcomes. In fact, patients with IVH were twice as likely to have a poor outcome as those without IVH13.

Management: Doing the Basics Well
Strong evidence supports significant improvement in clinical outcomes with conservative management done well. In the Quality in Acute Stroke Care (QASC) trial, authors demonstrated that improved management of fever, hyperglycemia and swallowing dysfunction improved patient outcomes after discharge14. Guidelines from the AHA and ASA on ICH further emphasize key fundamentals of care.
- Head of the bed should be elevated 30-45º to promote venous drainage of blood.
- Fevers should be treated when present.
- Glucose should be monitored, with care taken to avoid hyperglycemia and hypoglycemia.
- Lowering SBP to 140 mmHg is safe and may improve functional outcomes in patients with an initial SBP 150-220 mmHg, without contraindications to acute BP treatment4. This can be safely achieved with labetalol and nicardipine15.
- Frequent neurological exams, at least every hour, to monitor for deterioration.
- Dysphagia screening should be performed prior to any oral intake.
- Antiplatelet medications should not be reversed with platelet transfusions16.
- Routine use of prophylactic antiepileptics is not recommended. Phenytoin used in this setting was associated with worse clinical outcomes17.
- Clinical seizures should be treated with anticonvulsants and continuous EEG should be considered, as 30% of patients with ICH will demonstrate electrical seizure activity18.
Anticoagulation Reversal
Emergent reversal of anticoagulation, in conjunction with optimal blood pressure management has been shown to prevent hematoma expansion19. Vitamin K antagonists such as warfarin should be reversed to an INR < 1.4. The suggested approach to reversal by the American Society of Hematologists (ASH) is parenteral administration of vitamin K and 4-factor Prothrombin Complex Concentrates (PCCs). PCCs offer advantages over Fresh Frozen Plasma (FFP) by requiring less volume of infusion, not requiring blood typing and thawing, and are without the risk of transfusion reactions. They have been associated with faster normalization of the INR in patients with vitamin K associated ICH, but their effect on clinical outcome is less certain20. The ASH suggests the use of recombinant Xa (Andexxa) or 4-factor PCC for patients on oral direct Xa inhibitors, and idarucizumab for those on dabigatran, but acknowledges low certainty in supporting evidence21. Idarucizumab, an FDA approved antibody reversal agent for dabigatran, reverses its anticoagulant effects and should be considered, when available. Similarly, the factor Xa inhibitors apixaban and rivaroxaban may be reversed with andexanet when available22. Protamine sulfate is the preferred reversal agent for ICH associated with heparin use3. Of note, antiplatelet medications (such as aspirin and clopidogrel) should not be routinely reversed with platelet transfusions, as this was associated with higher mortality for spontaneous supratentorial intracerebral hemorrhages in the PATCH trial16.
Diagnosing and Managing Intracranial Pressure
IVH can obstruct cerebrospinal fluid (CSF) outflow and result in increased intracranial pressure (ICP). Cerebral perfusion pressure (CPP), as calculated by CPP = MAP-ICP, should target 50-70 mmHg. Hyperosmolar therapy with either mannitol or hypertonic saline is equally effective in lowering ICP23. Elevating the head of bed to 30º has been shown to decrease ICP, without adversely affecting cerebral oxygenation24. Hyperventilation for a brief period (<2 hours) to achieve cerebral vasoconstriction may be used as a temporizing measure in emergency settings of impending herniation, but carries risk of brain ischemia23.
Surgical Intervention
Neurosurgery should be emergently consulted in cases of ICH as a subset of patients will benefit from surgical intervention. An external ventricular drain (EVD) should be considered when IVC leads to hydrocephalus, reduced consciousness or evidence of transtentorial herniation. An EVD both measures and modulates ICP by draining CSF. While drainage of blood by EVD would theoretically also be beneficial, it is often difficult via ventricular catheters. Current research is evaluating adjunct thrombolytics to improve drainage of blood1.
More often, however, surgery is reserved for those who fail medical management. Hematoma evacuation is recommended in the management of cerebellar hematomas with evidence of hydrocephalus or brainstem compression. Surgical hematoma evacuation may also be considered in deteriorating patients with supratentorial hematomas as a life-saving measure1. Early surgical intervention did not improve outcomes in superficial ICH without IVH in the STICH I & II trials25.
Pearl – Posterior fossa hemorrhages are at particular risk for early clinical deterioration. ICH affecting the cerebellum often lead to local mass effect since there is little space to adjust to increases in volume. Obstructive hydrocephalus and brainstem compression can occur quickly. It is advised that these patients be considered for early surgical decompression1.
Delay Limitations of Care and DNAR Orders
The majority of mortality from ICH occurs during initial hospitalization. The AHA and ASA have identified withdrawal of medical support and early care limitations as predictors of poor outcome in what they describe as a self-fulfilling prophecy. As such, the AHA and ASA advocate for early aggressive care and recommend postponement of new do-not-attempt-resuscitation (DNAR) orders until at least the second full day of hospitalization1.
Case Resolution
4-factor PCC was given to reverse her apixaban (andexanet alfa unavailable) and her hypertension was treated with Labetalol (20mg IVP) and Nicardipine (5mg/hr) to a target SBP < 160 mmHg. CT angiography confirmed the location of bleed and showed no evidence of hematoma expansion, spot sign, or vascular malformation. Neurosurgery was consulted, but did not recommend emergent surgical intervention given the absence of any signs of obstructive hydrocephalus and the deep location of the hemorrhage. The patient was admitted to the ICU where she received dysphagia screening, continuous EEG monitoring, frequent neuro checks, and head of the bed elevation. Her ICH score of 1 predicted a 30-day mortality of <20%. Prior to admission, the patient was full code and discussion of new care limitations were appropriately delayed. After a week-long hospital admission, she was discharged to neurorehabilitation where she made significant functional gains. She was discharged with mild residual motor deficits.
Takeaways
Early and aggressive optimization of care can impact outcomes in ICH despite its intimidating prognosis. Initially, key steps include: a primary and secondary survey, identifying patients with potential ICH, and rapidly performing a NCCT brain. Once diagnosed, immediately elevate the head of the bed, keep SBP < 180 mmHg, reverse any coagulopathy, and consult neurosurgery. Surgical intervention, with a few important exceptions, remains reserved for those who have failed medical management, are rapidly deteriorating, or showing signs of obstructive hydrocephalus. Imaging findings and tools like the ICH scorecan aid in prognostication and communication with patients, family members, and colleagues. Maintenance of euglycemia and normothermia, and prevention of aspiration are basic, but meaningful strategies to optimize functional outcome. While treatment options for ICH remain largely conservative, recognizing that we have the power to affect outcomes is critical to ensuring that patients receive optimal care.
References and Further Reading
- Hemphill JC 3rd, Greenberg SM, Anderson CS, et al. Guidelines for the Management of Spontaneous Intracerebral Hemorrhage: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. 2015;46(7):2032-2060. doi:10.1161/STR.0000000000000069
- Carpenter AM, Singh IP, Gandhi CD, Prestigiacomo CJ. Genetic risk factors for spontaneous intracerebral haemorrhage. Nat Rev Neurol. 2016 Jan;12(1):40-9. doi: 10.1038/nrneurol.2015.226. Epub 2015 Dec 16. PMID: 26670299
- Morotti A, Goldstein JN. Diagnosis and Management of Acute Intracerebral Hemorrhage. Emerg Med Clin North Am. 2016;34(4):883-899. doi:10.1016/j.emc.2016.06.010
- Anderson CS, Heeley E, Huang Y, et al. Rapid blood-pressure lowering in patients with acute intracerebral hemorrhage. N Engl J Med. 2013;368(25):2355-2365. doi:10.1056/NEJMoa1214609
- Qureshi AI, Palesch YY, Barsan WG, et al. Intensive Blood-Pressure Lowering in Patients with Acute Cerebral Hemorrhage. N Engl J Med. 2016;375(11):1033-1043. doi:10.1056/NEJMoa1603460
- Charidimou A, Gang Q, Werring DJ. Sporadic cerebral amyloid angiopathy revisited: recent insights into pathophysiology and clinical spectrum. J Neurol Neurosurg Psychiatry. 2012;83(2):124-137. doi:10.1136/jnnp-2011-301308
- Hemphill JC 3rd, Bonovich DC, Besmertis L, Manley GT, Johnston SC. The ICH score: a simple, reliable grading scale for intracerebral hemorrhage. Stroke. 2001 Apr;32(4):891-7. doi: 10.1161/01.str.32.4.891. PMID: 11283388.
- Kothari RU, Brott T, Broderick JP, Barsan WG, Sauerbeck LR, Zuccarello M, Khoury J. The ABCs of measuring intracerebral hemorrhage volumes. Stroke. 1996 Aug;27(8):1304-5. doi: 10.1161/01.str.27.8.1304. PMID: 8711791.
- Siket, M. ICH, Evidence-Based Approach to the “Other” Stroke. ACEP. October 18, 2016. ACEP Scientific Assembly. Las Vegas, NV
- Broderick JP, Brott TG, Duldner JE, Tomsick T, Huster G. Volume of intracerebral hemorrhage. A powerful and easy-to-use predictor of 30-day mortality. Stroke. 1993;24(7):987-993. doi:10.1161/01.str.24.7.987
- Al-Shahi Salman R, Frantzias J, Lee RJ, et al. Absolute risk and predictors of the growth of acute spontaneous intracerebral haemorrhage: a systematic review and meta-analysis of individual patient data [published correction appears in Lancet Neurol. 2018 Sep 19]. Lancet Neurol. 2018;17(10):885-894. doi:10.1016/S1474-4422(18)30253-9
- Brouwers HB, Raffeld MR, van Nieuwenhuizen KM, et al. CT angiography spot sign in intracerebral hemorrhage predicts active bleeding during surgery. Neurology. 2014;83(10):883-889. doi:10.1212/WNL.0000000000000747
- Hallevi H, Albright KC, Aronowski J, et al. Intraventricular hemorrhage: Anatomic relationships and clinical implications. Neurology. 2008;70(11):848-852. doi:10.1212/01.wnl.0000304930.47751.75
- Middleton S, McElduff P, Ward J, et al. Implementation of evidence-based treatment protocols to manage fever, hyperglycaemia, and swallowing dysfunction in acute stroke (QASC): a cluster randomised controlled trial. Lancet. 2011;378(9804):1699-1706. doi:10.1016/S0140-6736(11)61485-2
- Ortega-Gutierrez S, Thomas J, Reccius A, et al. Effectiveness and safety of nicardipine and labetalol infusion for blood pressure management in patients with intracerebral and subarachnoid hemorrhage. Neurocrit Care. 2013;18(1):13-19. doi:10.1007/s12028-012-9782-1
- Baharoglu MI, Cordonnier C, Al-Shahi Salman R, et al. Platelet transfusion versus standard care after acute stroke due to spontaneous cerebral haemorrhage associated with antiplatelet therapy (PATCH): a randomised, open-label, phase 3 trial. Lancet. 2016;387(10038):2605-2613. doi:10.1016/S0140-6736(16)30392-0
- Naidech AM, Garg RK, Liebling S, et al. Anticonvulsant use and outcomes after intracerebral hemorrhage. Stroke. 2009;40(12):3810-3815. doi:10.1161/STROKEAHA.109.559948
- Rymer MM. Hemorrhagic stroke: intracerebral hemorrhage. Mo Med. 2011;108(1):50-54.
- Kuramatsu JB, Gerner ST, Schellinger PD, et al. Anticoagulant reversal, blood pressure levels, and anticoagulant resumption in patients with anticoagulation-related intracerebral hemorrhage. JAMA. 2015;313(8):824-836. doi:10.1001/jama.2015.0846
- Steiner T, Poli S, Griebe M, et al. Fresh frozen plasma versus prothrombin complex concentrate in patients with intracranial haemorrhage related to vitamin k antagonists (INCH): a randomised trial. Lancet Neurol.2016;15(6):566-73
- Witt DM, Nieuwlaat R, Clark NP, et al. American Society of Hematology 2018 guidelines for management of venous thromboembolism: optimal management of anticoagulation therapy. Blood Adv. 2018;2(22):3257-3291. doi:10.1182/bloodadvances.2018024893
- Dabi A, Koutrouvelis AP. Reversal Strategies for Intracranial Hemorrhage Related to Direct Oral Anticoagulant Medications. Crit Care Res Pract. 2018;2018:4907164. Published 2018 Jul 4. doi:10.1155/2018/4907164
- Stevens RD, Shoykhet M, Cadena R. Emergency Neurological Life Support: Intracranial Hypertension and Herniation. Neurocrit Care. 2015;23 Suppl 2(Suppl 2):S76-S82. doi:10.1007/s12028-015-0168-z
- Ng I, Lim J, Wong HB. Effects of head posture on cerebral hemodynamics: its influences on intracranial pressure, cerebral perfusion pressure, and cerebral oxygenation. Neurosurgery. 2004;54(3):593-598. doi:10.1227/01.neu.0000108639.16783.39
- Mendelow AD, Gregson BA, Rowan EN, et al. Early surgery versus initial conservative treatment in patients with spontaneous supratentorial lobar intracerebral haematomas (STICH II): A randomised trial. 2013;382(9890):397–408.








