Author: Chuck Pilcher, MD, FACEP (Editor, Med Mal Insights) // Editors: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Welcome to this month’s case from Medical Malpractice Insights – Learning from Lawsuits, a monthly email newsletter for ED physicians. The goal of MMI-LFL is to improve patient safety, educate physicians, and reduce the cost and stress of medical malpractice lawsuits. To opt in to the free subscriber list, click here.
Chuck Pilcher, MD, FACEP
Editor, Med Mal Insights
Massive Idiopathic Spontaneous Hemothorax
Sometimes bad things just happen
Facts: A female in her mid 30’s experiences a sudden “pop” in the upper left back progressing quickly to chest pain and syncope. EMS brings her to the local “Level I Cardiac Center”, where a tension hemothorax is found on CXR. A chest tube is placed, and a contrast CT shows a normal aorta. No source can be found, but bright red bleeding is heavy and persistent. The ED physician contacts the on-call cardio-thoracic surgeon, who is busy in the OR repairing an aortic dissection. The only other cardio-thoracic surgeon in the area is unavailable. A full court press is underway in an attempt to stabilize the patient. This includes a second chest tube, 11 units of blood, auto-transfusion, and 5 hours of continuous critical care by the physician and multiple nurses. During this time, the ED physician 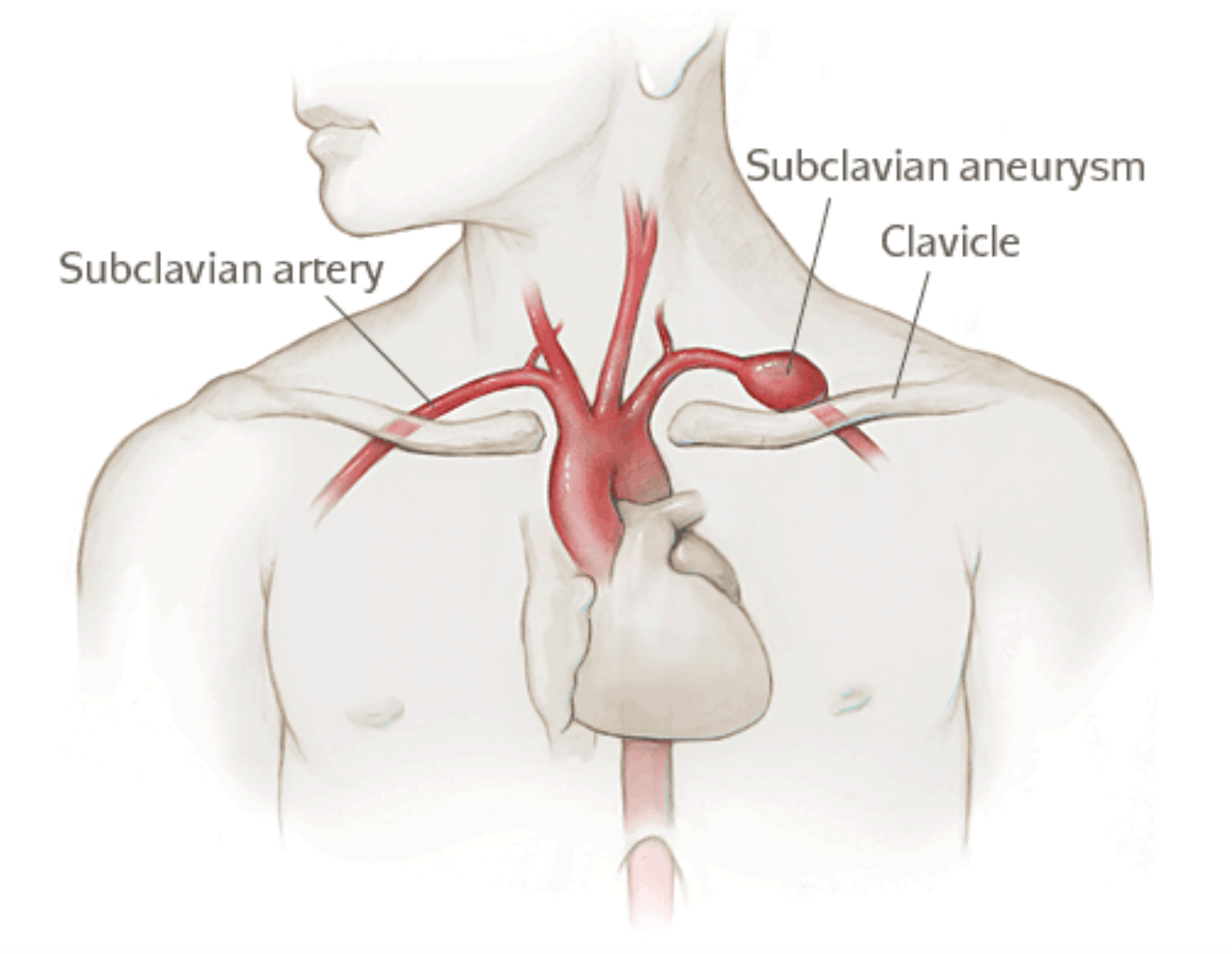 consults the area’s Level 1 Trauma Center which prefers the patient to be stabilized before transfer. During what is perceived as a possible window of opportunity, the patient is transferred by ALS ambulance, arrives at the Trauma Center alive, but dies in the OR. An autopsy is refused, so no source of bleeding is ever proven, but the surgeon completes the death certificate with the words “presumed rupture of subclavian artery aneurysm.” A lawsuit is filed against the hospital and emergency physician.
consults the area’s Level 1 Trauma Center which prefers the patient to be stabilized before transfer. During what is perceived as a possible window of opportunity, the patient is transferred by ALS ambulance, arrives at the Trauma Center alive, but dies in the OR. An autopsy is refused, so no source of bleeding is ever proven, but the surgeon completes the death certificate with the words “presumed rupture of subclavian artery aneurysm.” A lawsuit is filed against the hospital and emergency physician.
Plaintiff: I was bleeding to death and needed my chest opened immediately. The hospital failed to provide the “24/7 cardiovascular care” that you advertise as a “Level I Cardiac Center.” You should have had a backup surgeon for the on-call cardio-thoracic surgeon. Because you had no one to help me, you should have transferred me sooner.
Defense: Our call schedule is no different than any other hospital like ours. We cannot double-cover every specialty for a rare event like yours. Your problem was very unusual. You received heroic care. You were too unstable to transfer. You could have died in the ambulance had we not tried to stabilize you with transfusions. And we can only speculate where your bleeding was coming from and if it could have been fixed.
Result: The plaintiff’s expert believed that the ED physician had rendered exemplary care under difficult circumstances and was dropped from the suit. Despite the hospital’s backup cardio-thoracic surgery coverage being the same as other hospitals in the region, the hospital agreed to a “not large” pre-trial settlement. While the hospital likely would have prevailed at trial, the settlement avoided the risk of a plaintiff verdict and potential negative publicity.
Takeaways:
- Although rare, keep this possibility in mind. An aortic dissection is the go-to diagnosis here, and the CTA done as part of that workup will reveal the extra-aortic source in most cases (renal and subclavian arteries being most common.)
- Doing the best we can and doing the same thing we would do for any other patient and the same thing other doctors would do if presented with the same situation is the “standard of care.”
- Sometimes we are “damned if we do and damned if we don’t”; medicine is both art and science – and sometimes more luck than skill.
- Sometimes bad things happen over which we have no control. Practical issues assure that perfection and guaranteed survival will always be beyond our reach.
Reference: Endovascular treatment of ruptured subclavian artery aneurysm presented with hemoptysis. Kim S et al. Journal of Cardiology Cases, May 2015. Vol. 11:5, pp. 129-131.






