Authors: Jonathan Bornstein, MD (EM Resident Physician, Thomas Jefferson University Hospital); Jennifer Liao, MD (EM Resident Physician, Thomas Jefferson University Hospital); Marzena Sroczynski, RN (Wound Ostomy Care Nurse, Thomas Jefferson University Hospital); Carlos Rodriguez, MD (EM Attending Physician, Thomas Jefferson University Hospital) // Reviewed by: Edward Lew, MD (@elewMD, EM Attending Physician); Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital); Brit Long, MD (@long_brit, EM Attending Physician); and Caitlyn Costanzo, MD (Colorectal Attending Surgeon, Thomas Jefferson University Hospital)
Case:
A 45-year-old male with a history of severe Crohn’s disease on chronic steroids presents to your emergency department complaining of fatigue, dizziness, muscle cramps, paresthesias, and nonspecific abdominal pain. His vitals are Temp 99.4°F, BP 110/77, HR 121, RR 22, SpO2 100% on RA. He tells you he had surgery a week ago for his Crohn’s disease, but can’t relate the details. No outside hospital records are available. You notice he has a right-sided ostomy that is filled with liquid stool and is also leaking outside the bag. On removing the bag, you notice what appear to be two stomas with healthy appearing bowel visible. He is overall cachectic, with dry mucous membranes, and diffusely tender on abdominal exam.
Introduction:
An ostomy is an opening of the gastrointestinal and/or genitourinary tract outside of the abdominal wall that is created to facilitate the excretion of bodily waste. About 100,000 ostomies are performed every year and approximately 750,000-1 million people in the US have ostomies.1 Patients receive ostomies for a variety of indications, generally involving compromise of healthy bowel in the case of GI ostomies and bladder malignancy in the case of GU ostomies. Indications for different types of ostomies will be discussed in detail below.
Gastrointestinal Ostomies
General Anatomy and Indications
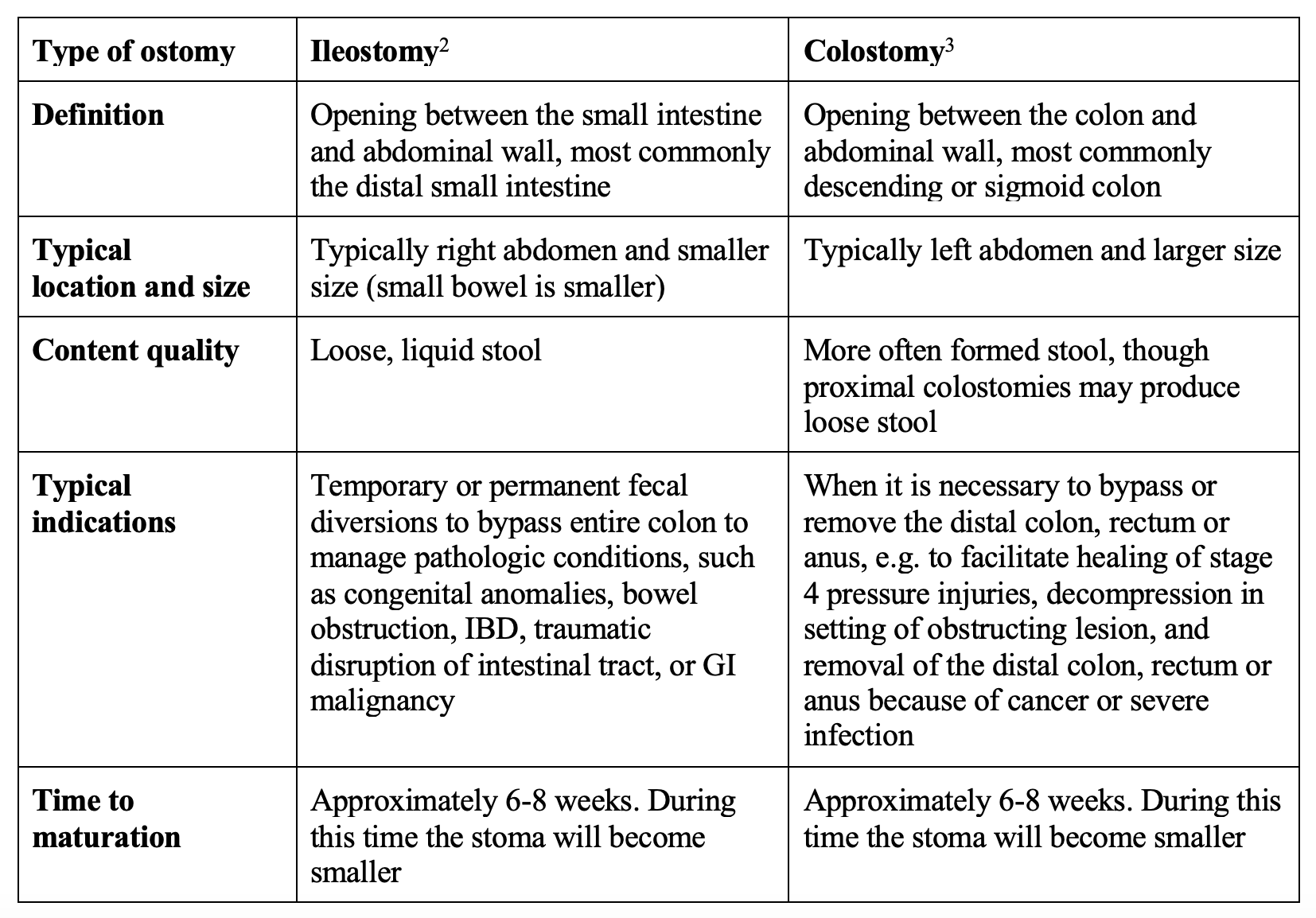
Ostomy Sub-Types
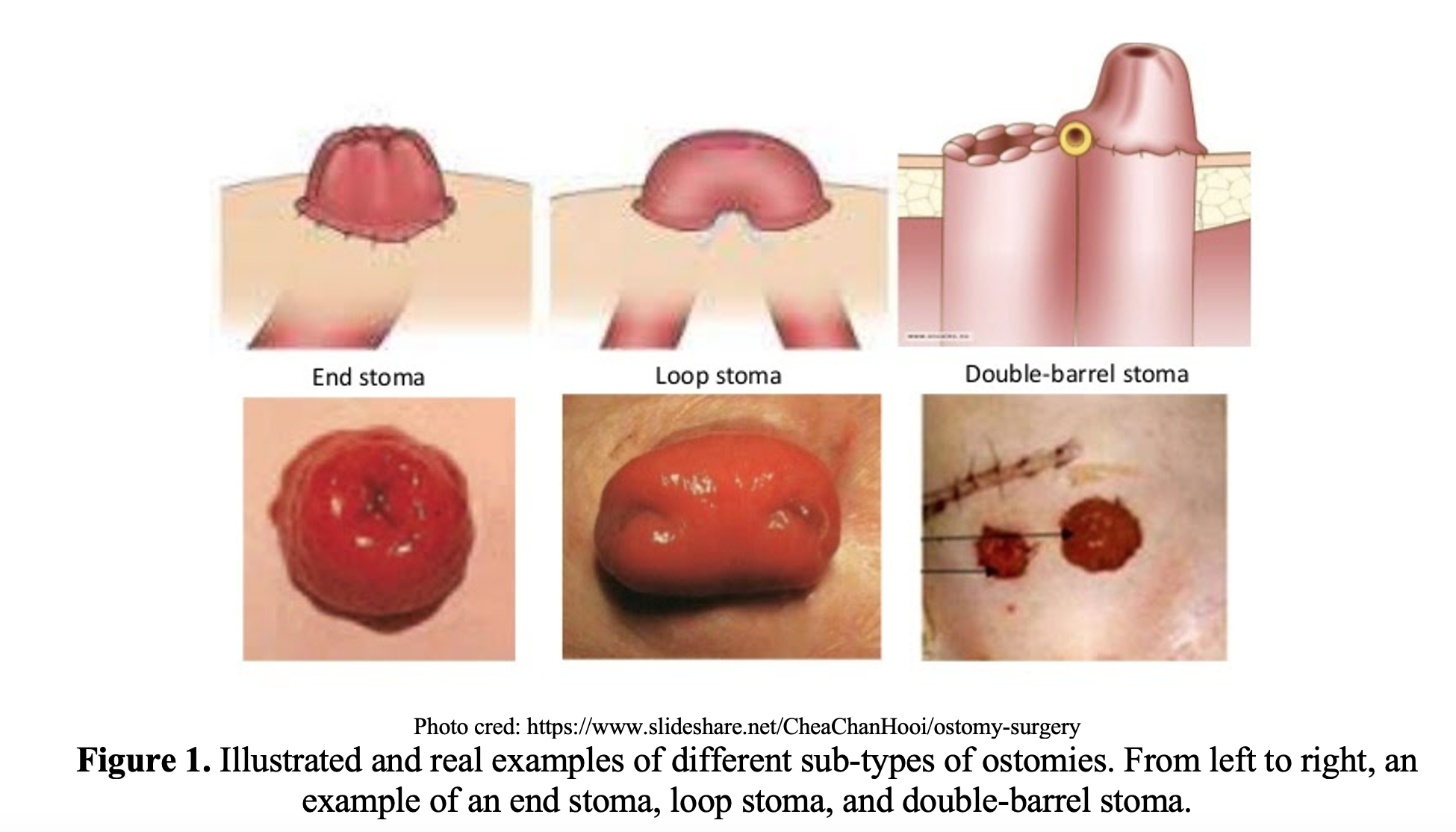
Within ileostomies and colostomies, there are different methods and indications for creating specific types of ostomies. Recognition of these sub-types will aid in management of their complications.
- Loop ileostomies or colostomies have two stomas; one proximal bowel and one distal bowel. Only the proximal stoma will produce stool, while the distal stoma may secrete mucus. Loop ostomies are temporary diversions used to protect distal bowel. For example, this may be used to protect a newly formed bowel-bowel anastomosis. They are designed to be reversed.1,2,4
- Double barrel ostomies are created when the surgeon divides the bowel completely and two adjacent, separate stomas are created. Similar to loop ileostomies, one stoma will put out stool (active side) and the other will put out mucus which protects the colon’s lining (inactive side).5 These are also typically temporary diversions.
- End ileostomies or colostomies will have one stoma and can be permanent or reversible (e.g. Hartmann’s). These are indicated when the distal bowel is compromised, for example rectal cancer where the rectum and anorectal sphincter are resected.2
- Continent diversion is an internal reservoir created from the bowel, most often part of the ileum. Can be used in both GI ostomies and urostomies. Some are created to allow for intermittent catheterization to control urination or bowel movements.
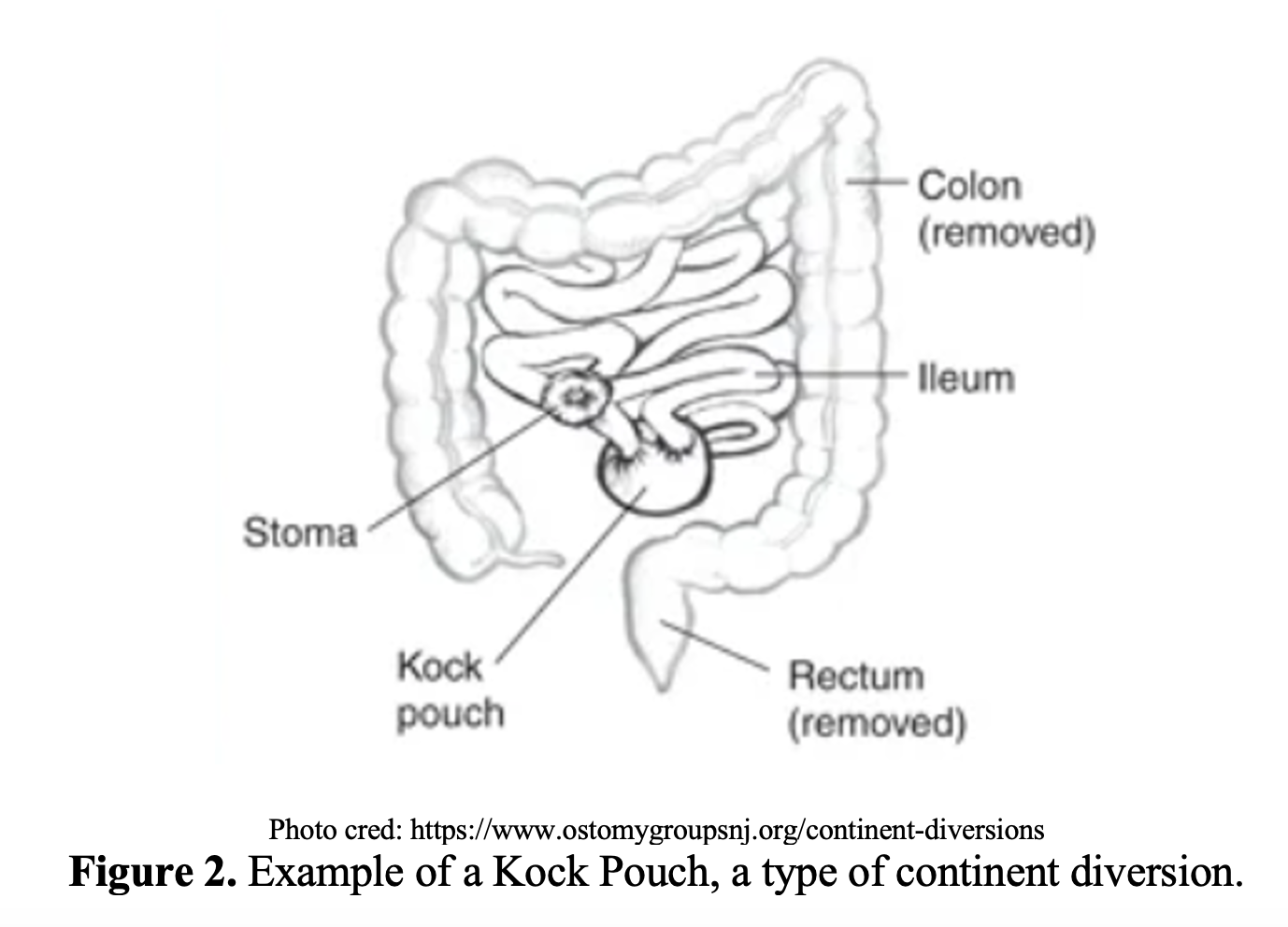
General Gastrointestinal Ostomy Parts and Care
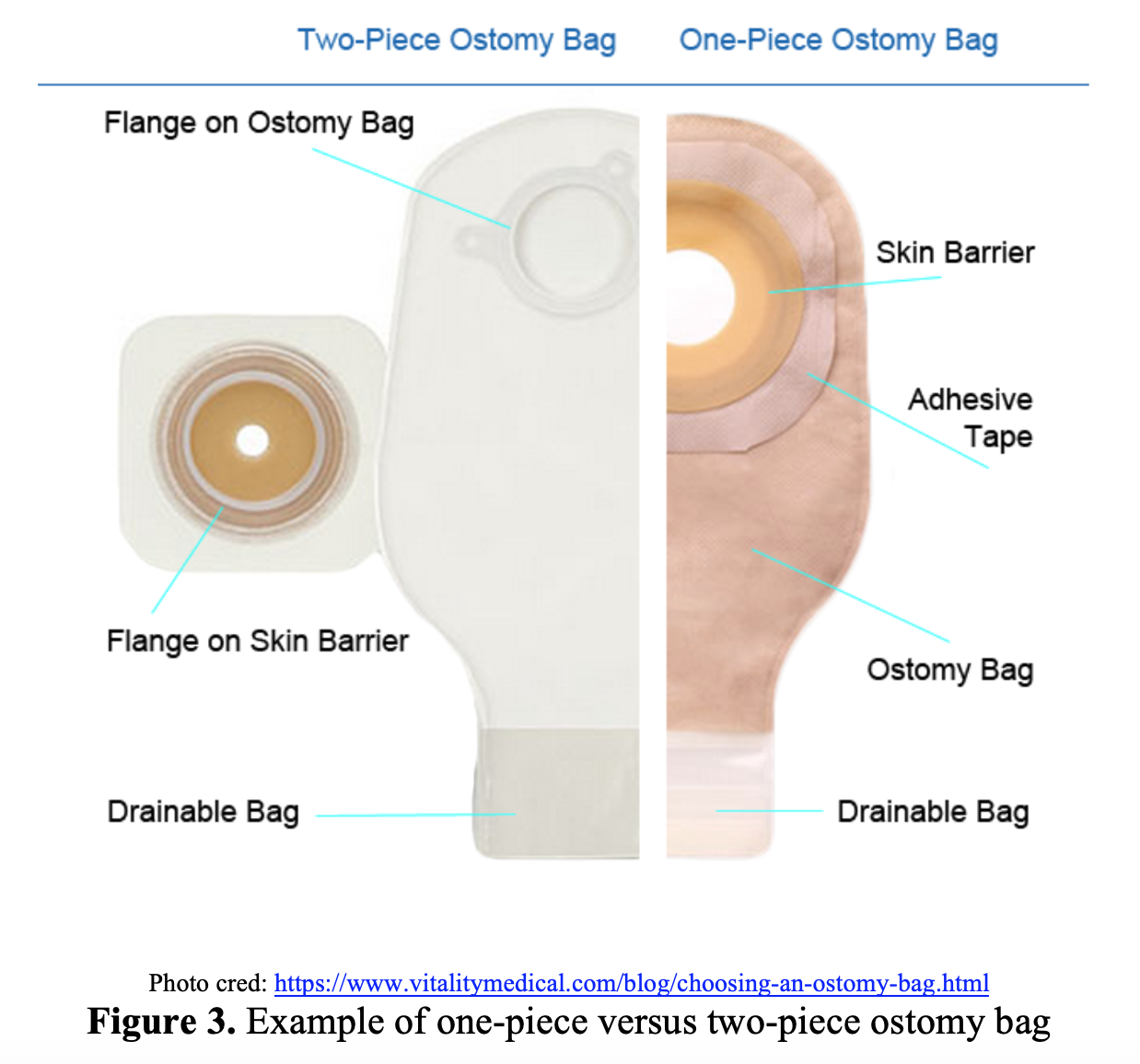
- One-piece versus two-piece pouch systems: One-piece and two-piece pouch systems are available to contain the output of ostomies. Either the wafer and pouch are separate (two piece) or joined (one piece). If there is a rigid plastic ring, this is a two-piece pouch system with a detachable pouch that will snap on and off.1,6 One-piece systems have a flatter profile, but stomas are more difficult to visualize and the whole system has to be replaced if there is a pouch issue, compared to simply replacing the pouch component in a two-piece system.7 Two-piece pouch systems are generally easier to manipulate and used in older populations.
- Ostomy Wafer: An adhesive that will attach directly to the skin around the stoma. The barrier should be slightly larger than the stoma. There are supplemental materials that you may come across to improve adhesion (ostomy ring, powders, strips, paste, liquid adhesive).

- Cleaning and evaluating the ostomy: After removing the ostomy, use soap and water to clean the area, examine the skin for signs of infection, and inspect the stoma. Make sure to dry completely before reattaching.
Gastrointestinal Ostomy Complications and Emergency Management
Early complications (hours to weeks)
- High output, fluid losses, dehydration
- Etiology: Most common early complication as the remaining bowel takes time to adapt. A high-output ostomy (>1.5-2 L/day) is the most common reason for hospital readmission. Normal output is typically 200ml-700ml per day. Can be due to extensive bowel resection, chronic impairment of bowel function, steroid withdrawal, or Clostridium difficile 2,8,9
- Clinical presentation: Hypokalemic with a non-anion gap metabolic acidosis (similar mechanism as profuse diarrhea). Ileostomy fluid is also highly concentrated with sodium so these patients are often severely hyponatremic and exhibit signs of this, including confusion and lethargy.1,2
- ED Management: Fluid resuscitation and electrolyte management. Consider CT imaging if ostomy was created within the last 6-8 weeks and there is diffuse abdominal tenderness and distention to evaluate for anastomotic leak and bowel obstruction. If the ostomy is more than hours to weeks old, suspect an alternative underlying cause such as gastroenteritis, IBD flare, Clostridium difficile infection, and/or short gut syndrome. For patients who are clinically stable and do not have severe electrolyte derangements, you can start these patients on a fiber supplement and Loperamide, counsel them that they should have a goal output of less than one liter per day and haver them follow-up closely with their colorectal surgeon.
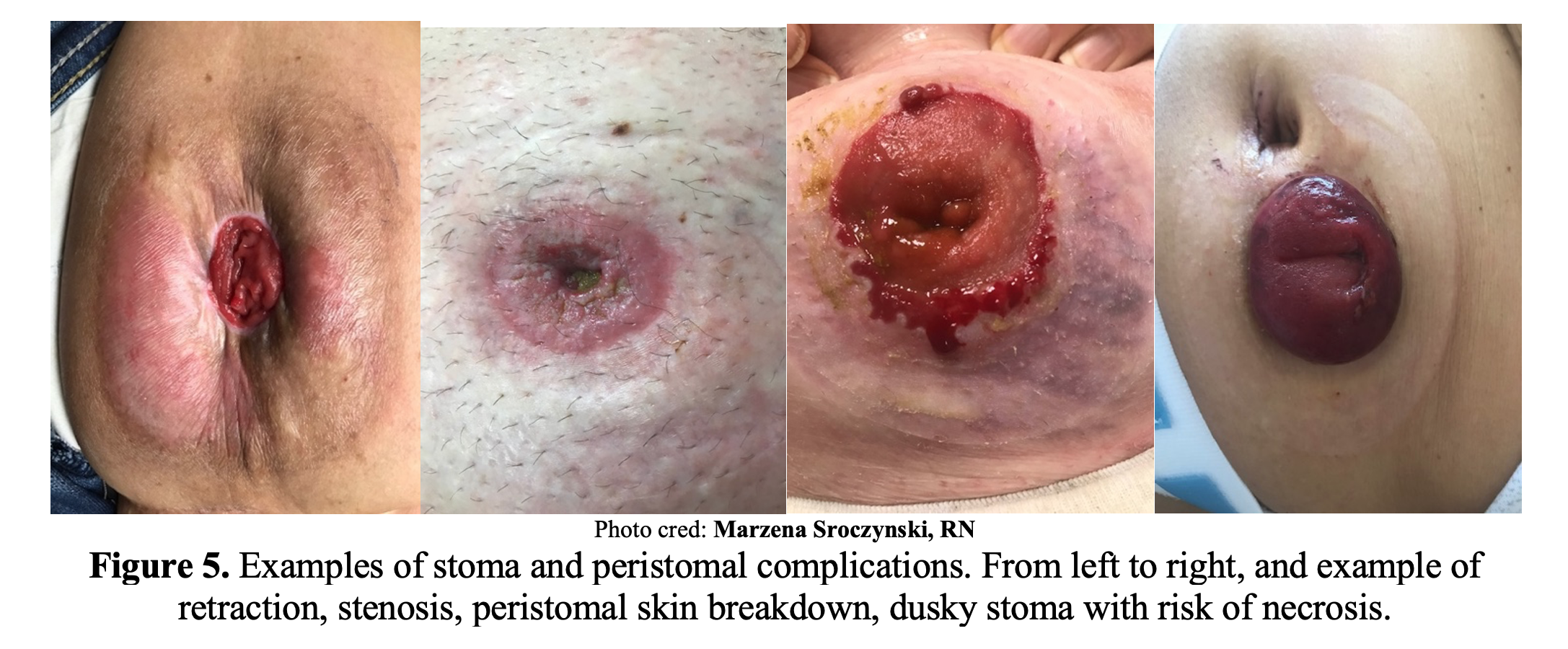
- Stomal necrosis3,6,10
- Etiology: Most often due to a failure to leave adequate perfusion to the stoma during stoma creation.
- Clinical Presentation: Pain around the stoma, abdominal pain, fever, peritonitis, and/or oral intolerance.
- ED management: Stomal tissue can be evaluated at the bedside with a test tube (if you can find one in the department!) and a light source. Stomal tissue will appear dusky and necrotic. Obtain a surgical consult and resuscitate the patient. Often requires surgical revision depending on depth of necrosis.
- Stomal retraction
- Etiology: Defined as stoma more than 0.5 cm below the skin surface.10 This is an early complication of ostomies due to high tension on stomal site. A slight degree of protrusion is desired (>1cm).8
- Clinical Presentation: Often detected during a routine ostomy bag change or due to leakage. More often seen in obese patients. However, this may present as a septic patient with peritoneal findings if there is discharge of fecal contents into the abdomen.3
- ED management: Assess for the degree of retraction. Will require a surgical consult if the patient is septic or peritoneal.
- 5Ws
- Etiology: As with any post-op patient, evaluate for common post-op problems that may be unrelated to the stoma: Wind (atelectasis, pneumonia), Water (UTI), Wound (SSI), Walking (DVT), Wonder (about) drugs.
- Clinical Presentation: Variable depending on the etiology.
- ED management: Variable depending on the etiology.
Late complications (months to years)
- Skin Breakdown, peristomal dermatitis, bacterial and/or fungal infection
- Etiology: Common complication and may be due to poor fit, difficulty with adherence, inadequate care, or infection.8 More common with ileostomies as they contain a larger concentration of proteolytic enzymes and alkali.2 The patient may need a new ostomy fitting and should be referred to an ostomy nurse for possible advanced intervention. Peristomal pyoderma gangrenosum, an inflammatory ulcerative skin condition, is a complication specific to patients with autoimmune disorders and often secondary to pathergy. Typically this is treated with topical steroids or tacrolimus; if there is treatment failure with topicals, systemic immunosuppression is considered. Rarely requires immediate treatment unless there is overlying infection.6
- Clinical Presentation: Pain, erythema, leakage and/or excoriation around the stoma site.
- ED management: Remove the ostomy pouch, assess for signs of fungal or bacterial infection and stomal or skin necrosis. See section on “General GI ostomy parts and care” above. Look for signs of fungal infection like satellite lesions. If it is a fungal infection, will need nystatin powder (don’t use creams as the ostomy won’t adhere). Apply the powder then a skin prep, allow to dry and reattach a new ostomy. If the cause is allergic dermatitis, will need to determine the offending allergen and remove/replace. May need to consider antibiotics for overlying bacterial infections.
- Stomal prolapse
- Etiology: High intra-abdominal pressure causing eversion of stoma through the abdominal wall. Occurs most often in transverse loop colostomies.3,8,11
- Clinical Presentation: Generally painless, stoma appears more protruded than normal. Occasionally, prolonged mucosal exposure can lead to ulceration and bleeding.
- ED management: Attempt to reduce. May use granulated sugar for osmotic reduction of edema to help with reduction. Will require surgery consultation if there are signs of ischemia.6,11
Complications that may occur anytime
- Decreased output3
- Etiology: There are several possible underlying reasons. Ileus is common during the first week post-op. Ileostomies are often subject to bezoars as the ileal lumen can narrow in diameter. Volvulus of bowel is another early complication causing decreased output. Stomal stenosis may also occur early post-op due to edema or as a late complication due to infection and retraction.6,11 Later presentations may also be due obstruction from a surgical adhesion or constipation or an incarcerated peristome hernia .
- Clinical Presentation: Abdominal pain, distention, and decreased ostomy output, nausea, and/or vomiting.
- ED management: Inquire about normal output and consistency. Assess the contents in the bag to evaluate for presence of flatus or stool. Assess the stoma for necrosis or signs of vascular compromise. A CT A/P can assist in evaluating for obstruction versus ileus. Requires surgical consult, resuscitation, and possible nasogastric tube placement if obstruction is the underlying etiology. If decreased output is a result of stomal stenosis in the subcutaneous aspect, course of gradual dilation outpatient can be trialed, though this can lead to further trauma and stenosis.11
- Parastomal hernia
- Etiology: Incisional hernia at the site of the stoma. It is more commonly late as the stoma may dilate over time. It occurs in up to 50% of patients. As the abdominal wall is already violated, the location of the hernia may be different than other hernias. Subcutaneous is the most common location. They can also be intramuscular, intrastomal, or peristomal.6,8
- Clinical Presentation: Presents similarly to other hernias.
- ED management: Similar to other hernias. Rule out obstruction, incarceration, or strangulation. CT can be used to evaluate. Managed conservatively unless strangulation, obstruction or incarceration is suspected.
- Leakage
- Etiology: Most often a benign cause such as poor ostomy fit.
- Clinical Presentation: Leakage of ostomy contents.
- ED management: Rule out serious complications such as high output failure, stomal necrosis, or stomal retraction (see discussion above). Assess the fit of the ostomy. Clean and replace the ostomy (see “General GI ostomy parts and care” above).
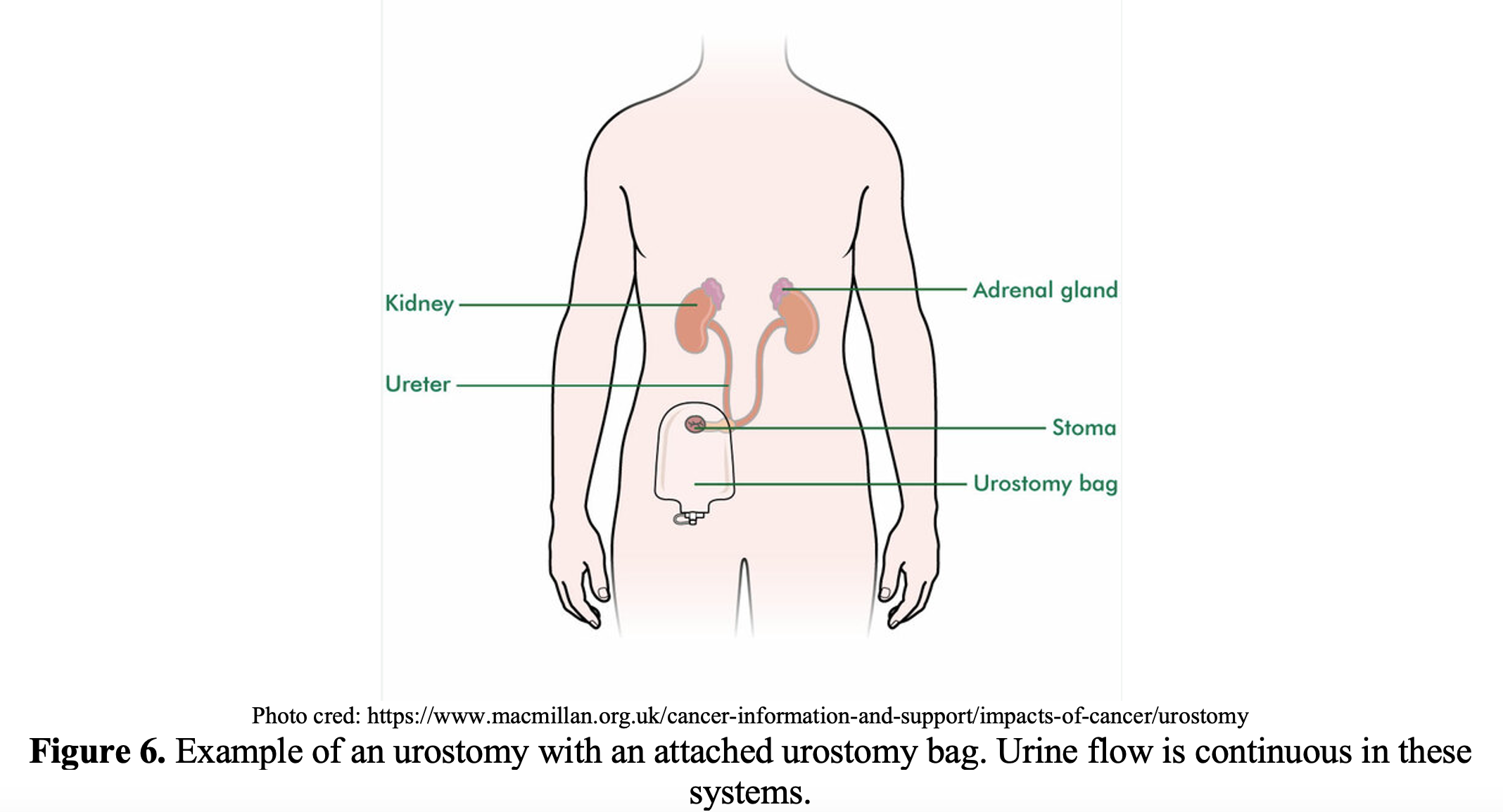
Urostomies
Definition: Opening between the abdominal wall and the urinary system, with the ileum being the most common conduit.
Anatomy
- Urostomies generally use a length of the ileum (ileal conduit) connected to the ureter to carry urine. Output will be continual. Colonic conduits (using a length of colon) are less common.7
- Ileal conduits are generally right sided.7
- Usually in the first weeks to months, stents are left in the ureters to maintain patency while the anastomoses site heals.7
- Some patients will have internal continent urinary pouches, which are also typically constructed from length of ileum, and either reconnected to the urethra or brought to the surface of the abdomen to create an abdominal stoma. In the case of these internal continent diversions with abdominal stoma, patients do not have external urostomy bags and intermittently self-catheterize the stoma to empty urine.7
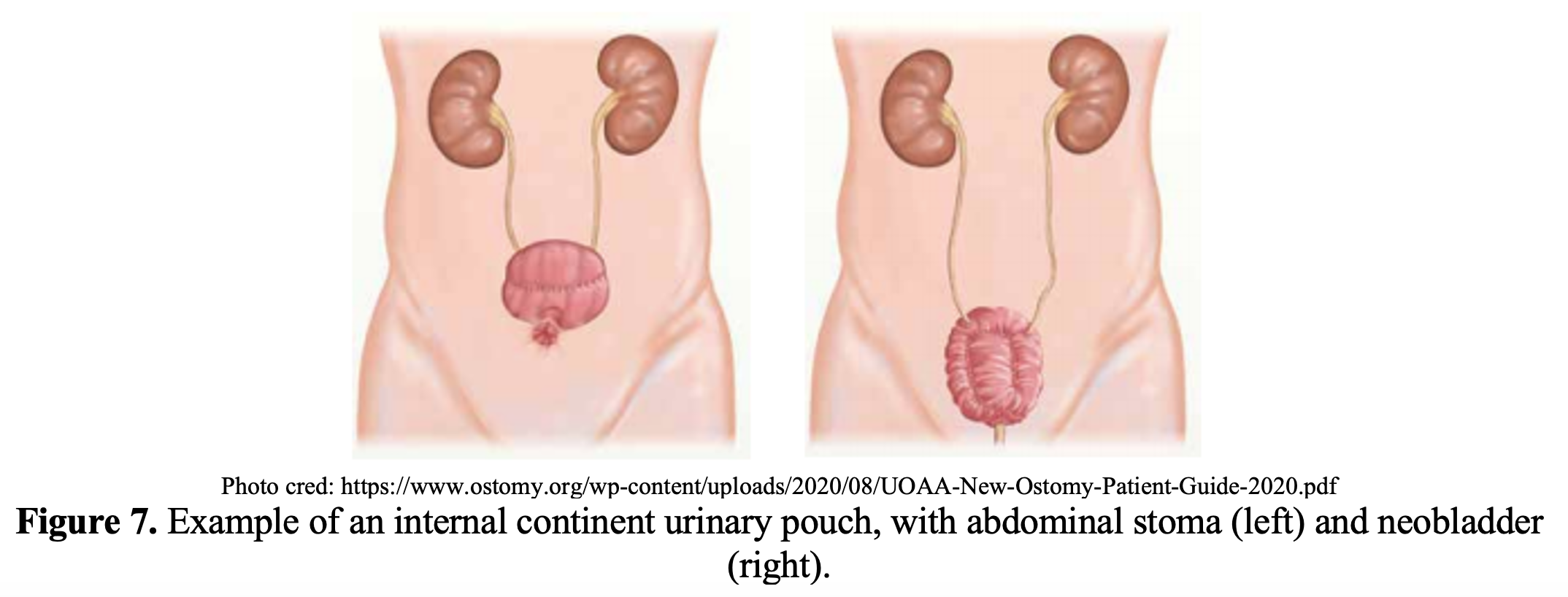
Common Indications: Bladder cancer, severe cystitis, bladder dysfunction, congenital defect, neurogenic bladder, radiation enteritis, and interstitial cystitis.7
General urostomy parts and care: Largely similar to what is noted above for gastrointestinal ostomies except unlike gastrointestinal ostomies, urostomies with external pouches will have a tap or spout at the end to drain urine and a valve to prevent backflow.7
Urostomy Complications and ED management
Many urostomy complications are similar to GI ostomy complications. Below are a few complications that are more specific to urostomies:
- Infection/UTI/pyelonephritis7
- Etiology: Most common early complication. Typically due to bacteria that normally colonize intestinal segments, incomplete voluntary voiding, or intermittent catheterization.
- Clinical Presentation: Fever, leukocytosis, CVA tenderness, cloudy urine.
- ED Management: Antipyretics, antibiotics, IV fluids. May need to consider a short admission for IV antibiotics depending on the clinical appearance of the patient.
- Impaired Renal Function12
- Etiology: Chronic urinary tract obstruction, stone, and/or chronic infections.
- Clinical Presentation: Fever, leukocytosis, decreased GFR, elevated creatinine, hydronephrosis.
- ED Management: Consider antibiotics if a septic stone is suspected. Consider a CT abdomen and pelvis without contrast to evaluate for a possible stone. Consult urology for stone removal and/or urostomy revision.
- Nutritional and metabolic abnormalities
- Etiology: Resection of the ileum or colon may result in malabsorption of bile salts and Vit B12.
- Clinical Presentation: Vit B12 deficiency symptoms (megaloblastic anemia, glossitis, oral ulcers, ataxia, impaired vibration), chronic diarrhea (malabsorption bile salts), hyperchloremic metabolic acidosis, osteomalacia, cholelithiasis.
- ED Management: Sodium bicarbonate replacement for chronic metabolic acidosis, vitamin B12 supplementation.
- Reservoir rupture13
- Etiology: Poor compliance with catheterization of continent cutaneous reservoir, acute/chronic neobladder overdistention, inability to self-catheterize for prolonged period of time. This typically occurs with internal continent urinary pouches.
- Clinical Presentation: Acute abdominal pain, peritoneal signs if severe.
- ED Management: CT abdomen and pelvis with contrast, both through IV and injected into the pouch (EM docs can do this) via the catheter patients use to self-cath (usually a 12-14 French catheter), to evaluate for extravasation of fluid in the abdomen/peritonitis. Consult urology urgently for surgical revision.
Case Conclusion:
IV normal saline was started given the patient’s severe dehydration. The work up was reviewed and showed hyponatremia, hypokalemia, hypomagnesemia, and metabolic acidosis. CT abdomen and pelvis with contrast revealed collection around the anastomotic site and intestinal obstruction. Surgery was consulted and the patient underwent emergency laparotomy for revision of anastomotic leak and started on total parenteral nutrition (TPN). The patient was discharged home once the ileostomy started functioning and was transitioned back to oral feeds after TPN was tapered off. One week later, he was readmitted to the intensive care unit again for high-output failure and severe hyponatremia with a sodium of 118, which was determined to be due to hypovolemic hypoosmotic hyponatremia due to high-output loss. His sodium was corrected with careful titration of mixture of 3% hypertonic saline and normal saline. He was started on loperamide after clostridium difficile infection was ruled out and started on pantoprazole to limit GI secretions. His oral fluids were restricted to 1.5 L/day and electrolytes were repleted as needed.
Pearls:
- Ileostomies tend to be on the right side of the abdomen and have loose liquid stool; colostomies tend to be on the left side of the abdomen and have more formed stool; urostomies tend to be on the right side of the abdomen and produce urine.
- High output failure
- Be aware of this in the dehydrated patient with a new gastrointestinal ostomy who is putting out 1.5-2 L fluid/day.
- IV fluid resuscitation and electrolyte replacement are essential. Pay particular attention to signs of severe hyponatremia, hypokalemia, and hypomagnesemia.
- Consider advanced imaging to assess for complications such as anastomotic leak, obstruction, or paralytic ileus.
- Stomal necrosis, incarcerated parastomal hernias, and internal reservoir ruptures are surgical emergencies – do not delay in resuscitating your patient and calling your surgical consultants early.
- Not all patients with urostomies and evidence of bacteriuria require antibiotics – it is common for their urine to be colonized with bacteria from the ileal conduit. Reserve antibiotics for patients with systemic signs of infection.
References/Further Reading:
- Settlemire I. New Ostomy Patient Guide. Ostomy.org. https://www.ostomy.org/wp-content/uploads/2020/08/UOAA-New-Ostomy-Patient-Guide-2020.pdf. Published 2020. Accessed January 9, 2020.
- Rajaretnam N, Lieske B. Ileostomy. In: Treasure Island (FL); 2020.
- Maria A, Lieske B. Colostomy Care. In: Treasure Island (FL); 2020.
- Lyon CC, Smith AJ, Griffiths CE, Beck MH. The spectrum of skin disorders in abdominal stoma patients. Br J Dermatol. 2000;143(6):1248-1260. doi:10.1046/j.1365-2133.2000.03896.x
- Cancer.org. Types of Colostomies And Pouching Systems. American Cancer Society.
- Shabbir J, Britton DC. Stoma complications: a literature overview. Color Dis Off J Assoc Coloproctology Gt Britain Irel. 2010;12(10):958-964. doi:10.1111/j.1463-1318.2009.02006.x
- Berti-Hearn L, Elliott B. Urostomy Care: A Guide for Home Care Clinicians. Home Healthc now. 2019;37(5):248-255. doi:10.1097/NHH.0000000000000792
- Bafford AC, Irani JL. Management and complications of stomas. Surg Clin North Am. 2013;93(1):145-166. doi:10.1016/j.suc.2012.09.015
- Mountford CG, Manas DM, Thompson NP. A practical approach to the management of high-output stoma. Frontline Gastroenterol. 2014;5(3):203-207. doi:10.1136/flgastro-2013-100375
- Suwanabol PA, Hardiman KM. Prevention and Management of Colostomy Complications: Retraction and Stenosis. Dis Colon Rectum. 2018;61(12):1344-1347. doi:10.1097/DCR.0000000000001246
- Husain SG, Cataldo TE. Late stomal complications. Clin Colon Rectal Surg. 2008;21(1):31-40. doi:10.1055/s-2008-1055319
- Zabell JR, Adejoro O, Konety BR, Weight CJ. Risk of end stage kidney disease after radical cystectomy according to urinarydiversion type. J Urol. 2015;193(4):1283-1287. doi:10.1016/j.juro.2014.10.103
- Knight RB, Thomas B, Tsiotras A, Kasprenski M. Spontaneous rupture of continent urinary reservoir with extrophy-epispadias complex. J Surg case reports. 2019;2019(6):rjz172. doi:10.1093/jscr/rjz172








