Author: McKenna Furgurson, MD (EM Resident Physician, Parkland / UT Southwestern) // Reviewed by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
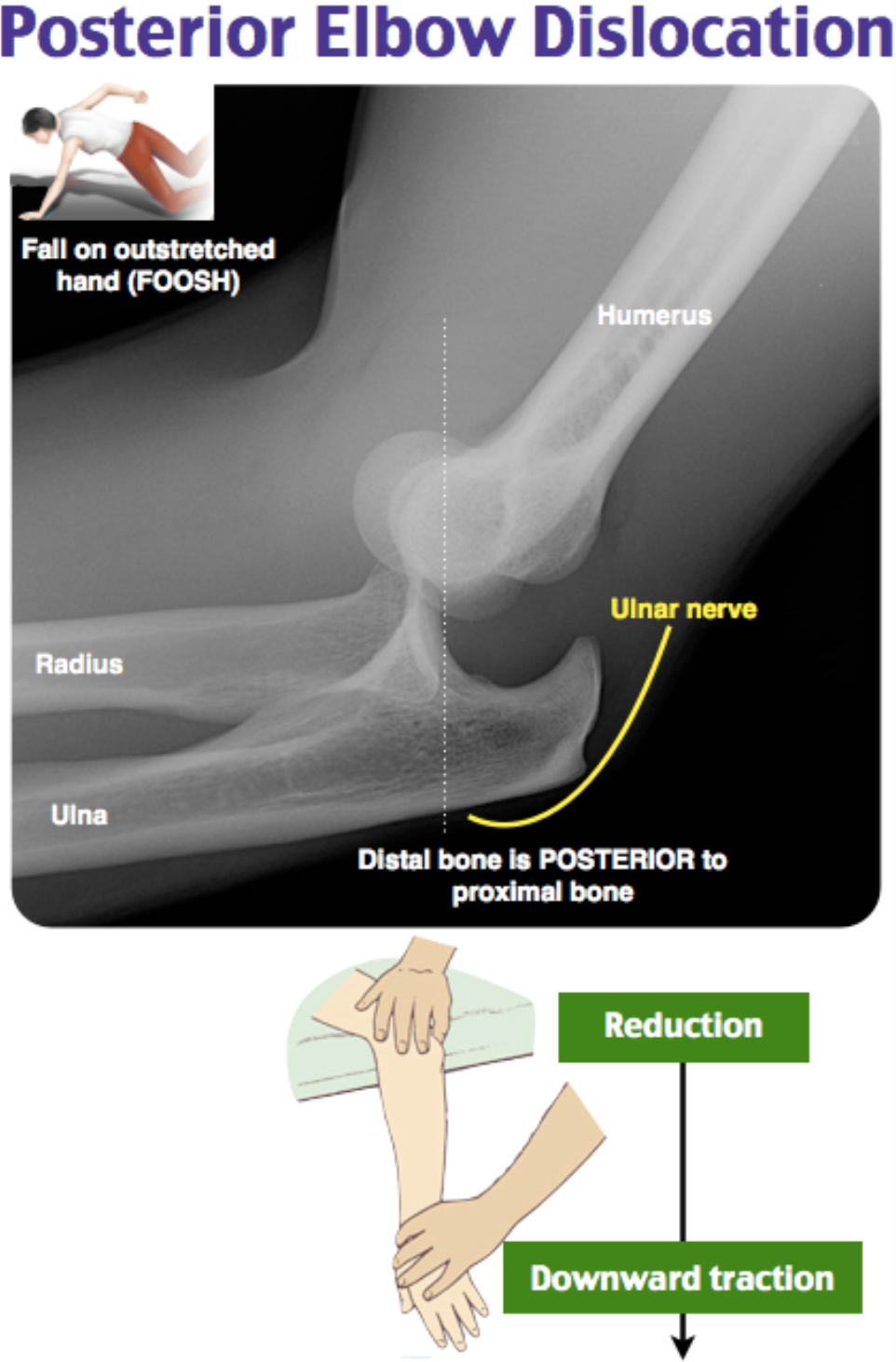
Case: A 15-year-old male with no past medical history comes in complaining of left arm pain. The patient was brought to the emergency department by his mother just after he fell while playing football. The patient is noted to have his arm held at 45-degree flexion. There is significant swelling over distal humerus, elbow, and proximal forearm with inability to extend at the elbow. What is most likely to be seen on radiographs?
Answer: Posterior elbow dislocation
Background
- At least 90% are posterior dislocations. [1]
- Often due to a fall on outstretched hand (FOOSH) with elbow hyperextension
- More common in adolescent men during sports [2]
- Anterior dislocations are much less common and more often associated with ligamentous injury, fractures, and brachial artery injury. [3]
Exam
- Patient often holding arm flexed at 45 degrees. [4]
- Painful, decreased ROM
- Varying degrees of swelling/deformity. May resemble a supracondylar fracture on exam with obscured landmarks due to swelling.
- Neurovascular exam:
- Ulnar nerve injury occurs in up to 20% of elbow dislocations. [3,4]
- Median nerve entrapment is less common.
- Brachial artery injury is more common in anterior or open dislocations.
Evaluation/Diagnosis
- Diagnosis often apparent on clinical evaluation, and can be confirmed with radiographs
- Lateral view: ulna and radius are displaced posteriorly.
- AP view: lateral or medial displacement, with ulna and radius in their normal relationship to each other

- Analyze for fractures
- Elbow dislocations are associated with fractures in 1/3 of cases. [3]
- Focus on radial head, coronoid process, and distal ulna.
- Terrible triad = elbow dislocation, fracture of coronoid process, and radial head fracture. This triad is difficult to treat and has poor outcomes in terms of mobility.
- Elbow dislocations are associated with fractures in 1/3 of cases. [3]
- Dislocation classifications
- Classify based on direction of displacement of ulna relative to humerus.
- Posterior and posterolateral are most common.
- Others: posteromedial, lateral, medial, anterior
- Instability is graded in stages. [1]
- Posterolateral rotary subluxation: reduces spontaneously
- Perched: incomplete posterolateral dislocation
- Dislocated: tearing of capsule and ligamentous stabilizers
- Simple v Complex: Simple if not associated with a fracture. Complex if associated with a fracture.
- Classify based on direction of displacement of ulna relative to humerus.
Management: Simple Dislocations
- Closed reduction under procedural sedation.
- Closed reduction Techniques [5]
- Traction-Countertraction Technique
- Provider 1 stabilizes humerus. Provider 2 holds forearm supinated and 30 degrees flexed, then applies slow longitudinal traction while slowly flexing the elbow.
- Traction-Countertraction Technique
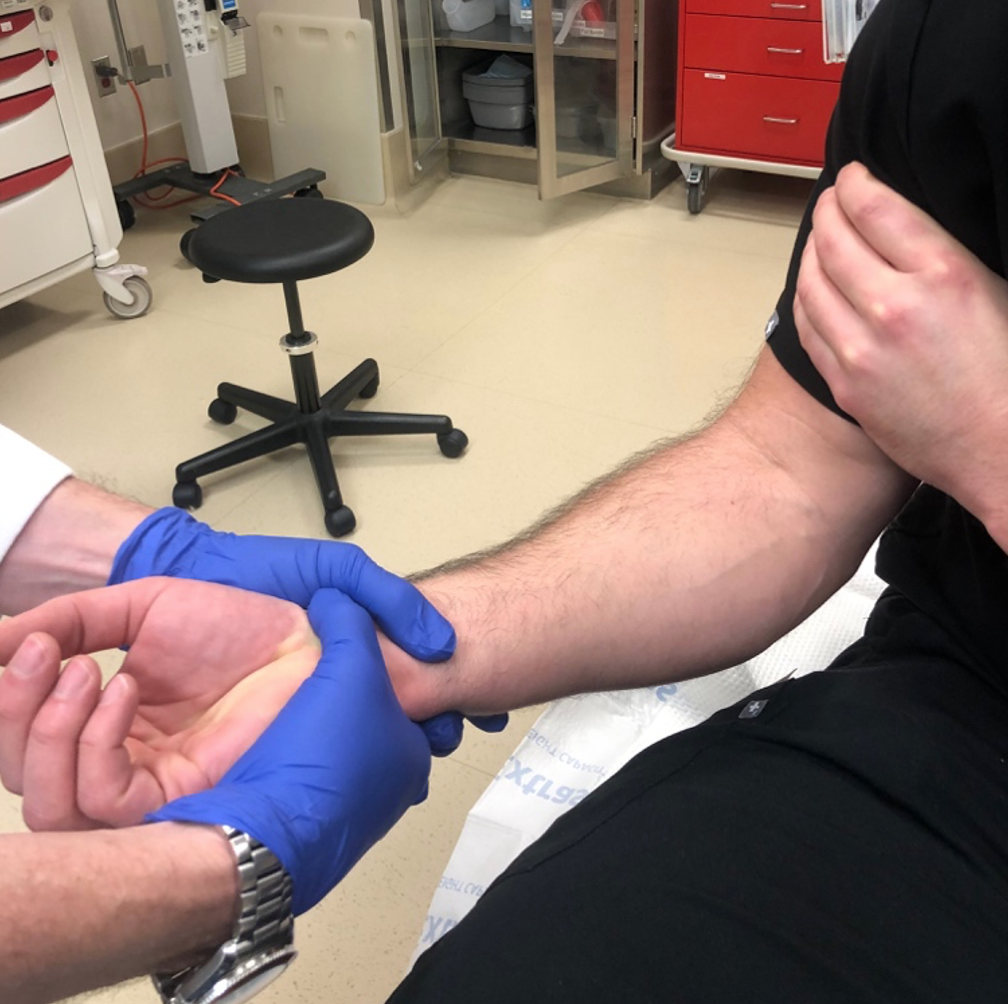
- Kumar Technique: patient-assisted counter traction
- Patient lays supine. Provider takes the patient’s arm across the chest (with olecranon pointing upwards), and applies traction on forearm. Can use other hand to manipulate olecranon.
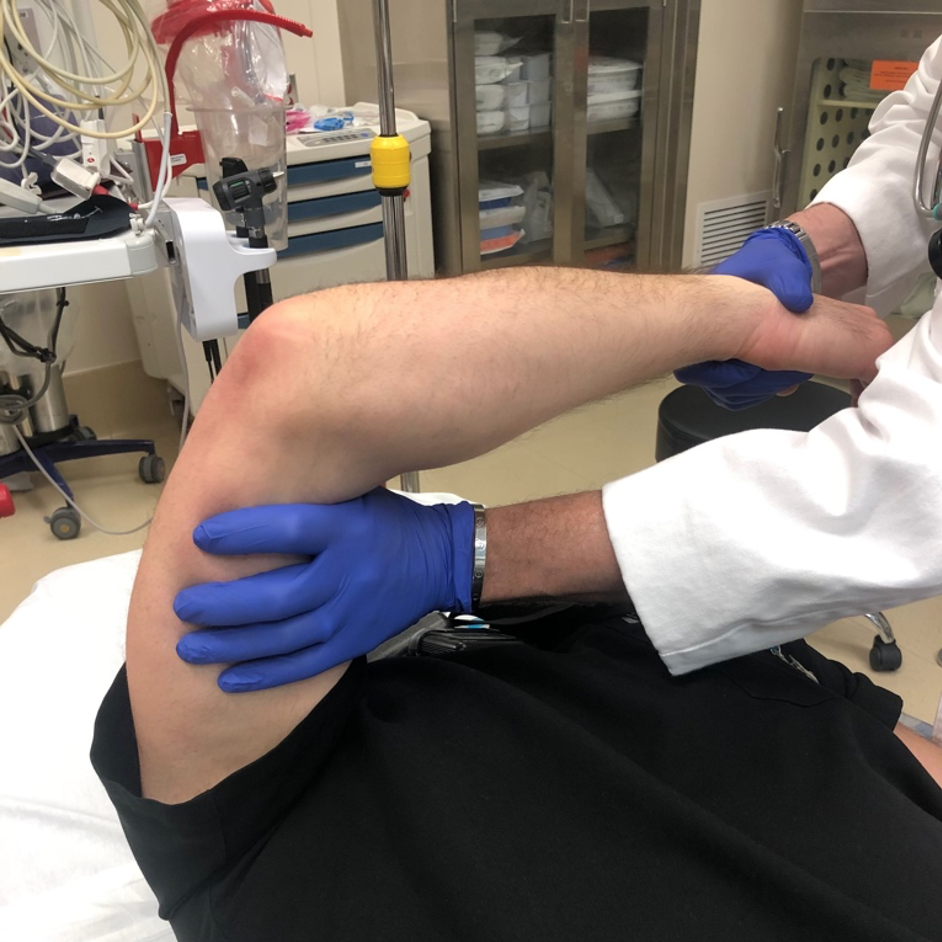
- Leverage Technique
- Patient’s elbow is flexed with forearm supinated. Provider places his/her own elbow at patient’s distal bicep, interlocks fingers with patient (can grab wrist if unable to reach fingers), and gradually flexes patient’s wrist using elbow as a fulcrum. Can use other hand to manipulate olecranon.
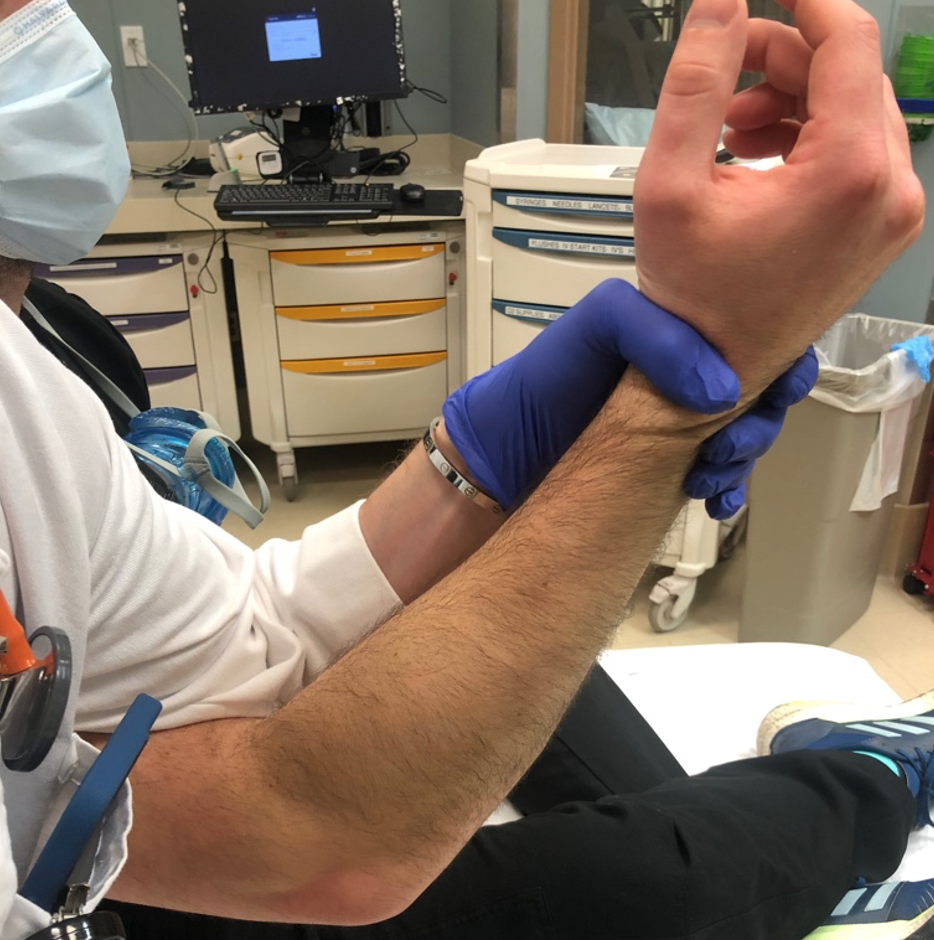
- Modified Simson Technique
- Patient lays prone with arm abducted and hanging over the side of the bed. Provider applies downward force. Can use other hand to manipulate olecranon.
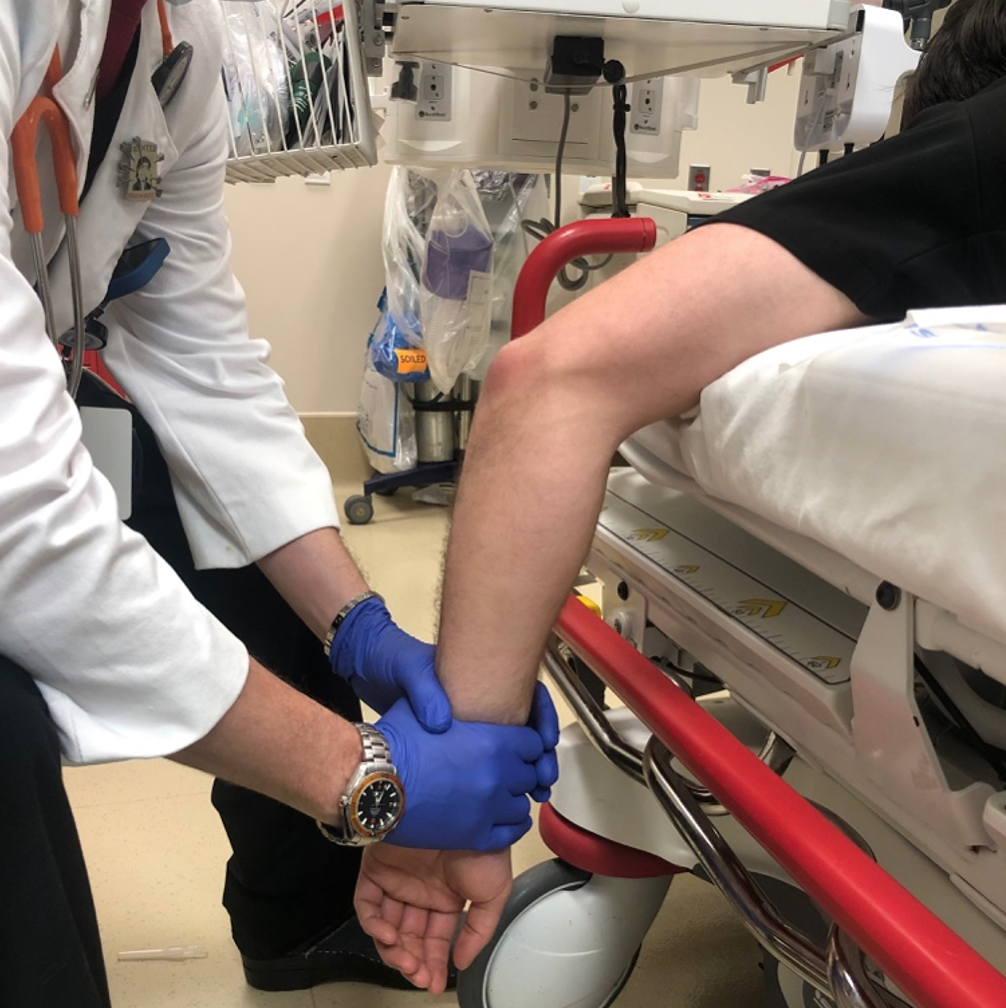
- Repeat neurovascular exam and full range of motion to assess stability.
- Immobilize in a long arm posterior splint just under 90 degrees flexion, and sling. [1]
- Even if elbow is self-reduced prior to imaging, the elbow still needs immobilization due to associated ligament disruption.
- Repeat radiographs.
- Orthopedic follow up in 1 week. If unstable after reduction, will need urgent follow up in 3 days.
- Resume full ROM in 5-7 days. [1]
Management: Complex Dislocations
- Orthopedic consultation with possible operative management.
Disposition
- Patient can be discharged if there is no neurovascular complications, fractures, or joint instability.
- Orthopedic consult if there is open dislocation, associated fracture, anterior dislocation, or dislocation with persistent neurovascular compromise after reduction.
Pearls
- Simple dislocations can be reduced and splinted in long arm splint in ED with orthopedic follow up in 1 week.
- Encourage early ROM (5-7 days) to improve mobility of joint.
- Complicated dislocation (with fracture) or any neurovascular compromise needs orthopedic consult while in ED.

What is the most common type of elbow dislocation?
A) Anterior
B) Lateral
C) Medial
D) Posterolateral
Answer: D
The elbow is the second most commonly dislocated major joint in the body, following the shoulder. In an elbow dislocation, the radius and ulna, held together by the strong annular ligament and the interosseous membrane, displace as a unit from the humerus. Dislocations are described with the distal component relative to the proximal one. In this example, dislocations are described with the relative position of the ulna to the humerus. A posterolateral dislocation, in which the ulna becomes malpositioned posterior and lateral to the humerus, is the most common type of dislocation. The ulna may also dislocate anteriorly, medially or laterally from the humerus, but this is less common. Because significant force is required to dislocate the elbow, many dislocations are associated with fractures of adjacent structures. A fracture-dislocation is termed a complex elbow dislocation. Most elbow dislocations occur following a fall onto an outstretched arm that is hyperextended at the time of impact. On examination, patients with a posterior dislocation have marked prominence of the olecranon. A careful neurovascular exam must be performed since the brachial artery and ulnar nerve are subject to injury. Posterior dislocations should be reduced immediately, especially if there is neurovascular compromise. Intra-articular analgesic injection and procedural sedation is usually necessary to facilitate reduction. To reduce the dislocation, an assistant should stabilize the humerus in 30 degrees of flexion and apply countertraction while the provider applies traction to the supinated distal forearm. Following reduction, patients should be immobilized in a posterior splint with close orthopedic follow-up.
Anterior (A), lateral (B), and medial (C) dislocations are less common than posterior elbow dislocations.
Further Reading:
FOAM reading
Core EM: “Elbow Dislocation” https://coreem.net/core/elbow-dislocation/
Life In The Fast Lane: “Elbow Dislocation” https://litfl.com/elbow-dislocation/#:~:text=The%20elbow%20is%20one%20of,to%20dislocation%20of%20the%20shoulder.
References
- Goldflam K. Evaluation and treatment of the elbow and forearm injuries in the emergency department. Emerg Med Clin North Am. 2015;33(2):409-421. doi:10.1016/j.emc.2014.12.010
- Stoneback J, Owens B, Sykes J, Athwal G, Pointer L, Wolf J. Incidence of Elbow Dislocations in the United States Population. The Journal of Bone and Joint Surgery-American Volume. 2012;94(3):240-245. doi:10.2106/jbjs.j.01663
- Hanlon DP, Mavrophilipos V. The Emergent Evaluation and Treatment of Elbow and Forearm Injuries. Emerg Med Clin North Am. 2020;38(1):81-102. doi:10.1016/j.emc.2019.09.005
- Chow YC, Lee SW. Chapter 270: Elbow and Forearm Injuries. In: Tintinalli JE, Ma O, Yealy DM, Meckler GD, Stapczynski J, Cline DM, Thomas SH. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 2020. McGraw-Hill
- Gottlieb M, Schiebout J. Elbow Dislocations in the Emergency Department: A Review of Reduction Techniques. J Emerg Med. 2018;54(6):849-854. doi:10.1016/j.jemermed.2018.02.011






