Written by: David Cisewski, MD (@DHCisewski – EM Resident Physician, Icahn School of Medicine at Mount Sinai) // Edited by: Manpreet Singh, MD (@MPrizzleER), Alex Koyfman, MD (@EMHighAK), and Brit Long, MD (@long_brit)
Today’s post in the Pain Profiles series by Dr. David Cisewski evaluates the intranasal route for analgesics.
Review of Intranasally Administered Medications for Use in the Emergency Department
Bailey AM, Baum RA, Horn K, Lewis T, Morizio K, Schultz A, et al. Review of Intranasally Administered Medications for Use in the Emergency Department. J Emerg Med. 2017;53(1):38-48.
One-liner
Intranasal (IN) delivery is a safe, simple and effective method to be utilized for the expeditious administration of analgesic medications in an emergency setting.
Clinical Pearls and Key Points
What are the benefits to intranasal (IN) medication delivery? IN medication delivery offers 6 major benefits compared to its IV/IM/PO alternatives:
- Safety– decreased risk of needlestick injury for both the patient and the health care provider.
- Direct– the nasal mucosa is a highly vascularized region offering a direct conduit to the CNS.
- Efficient– unlike oral delivery which requires enteric ingestion, the IN route avoids this delay as well as first-metabolism. This results in similar rates on onset to IV forms.
- Fast– unlike PO medications which take time and IV routes which require vascular access, IN results in rapid administration which can be essential in emergent situations such as seizures, trauma, and agitation.
- Easy– Unlike IV access which requires venous access, site preparation, and sterilization, IN delivery is independent of body habitus, clinical condition, level of cooperation, or poor venous access (sickle cell disease, IV drug users).
- Pain-free– without needles or bulky PO medications, IN offers an ideal administration route for pediatric patients.
Are their specific drugs that are ideal for IN delivery? Any drug with poor GI solubility or that undergoes extensive first-pass metabolism is ideal for IN delivery
How are IN medications delivered? Optimally both nostrils should be available to maximize absorption surface area. Unlike IV medications, no site sterilization is required with IN administration. Choose high-concentration formulations to avoid unwanted runoff from large volume delivery. IN medications can be delivered in one of several ways:
- Atomizers – reduce runoff, enhance delivery over a larger surface area
- Manual – topical administration
- Sniffing – decreased absorption as larger amounts land on external nostril
Is there an optimal method of delivery? Atomizers are optimal for IN delivery. They have maximum absorption, reduced run-off, increased patient comfort, and its use is independent of head position (ie, can be supine or upright).
Any contraindications to IN delivery? IN delivery should not be used in patients with abnormal neurologic exam or developmental delay, facial trauma, epistaxis, nasal obstruction (polyps, cystic fibrosis), or rhinitis.
What are the adverse side effect on IN delivery? Local irritation is the most common side effect. In addition, patients may experience dysgeusia (bad taste), increased lacrimation, and an occasional transient burning sensation.
What are the strategies for IN administration? There are 4 strategies to remember for effective IN administration:
- Concentrate (the medication) – ideally volumes <1 mL per nostril should be used (reduce run-off).
- Binasal delivery – Divide doses between both nostrils (optimize absorption).
- Don’t inhale – minimize lung delivery by sniffing but not inhaling.
- Don’t blow – Avoid post-administration nose blowing or sniffing (optimize mucosal absorption).
What are the commonly used IN medications in the ED? (see table below)
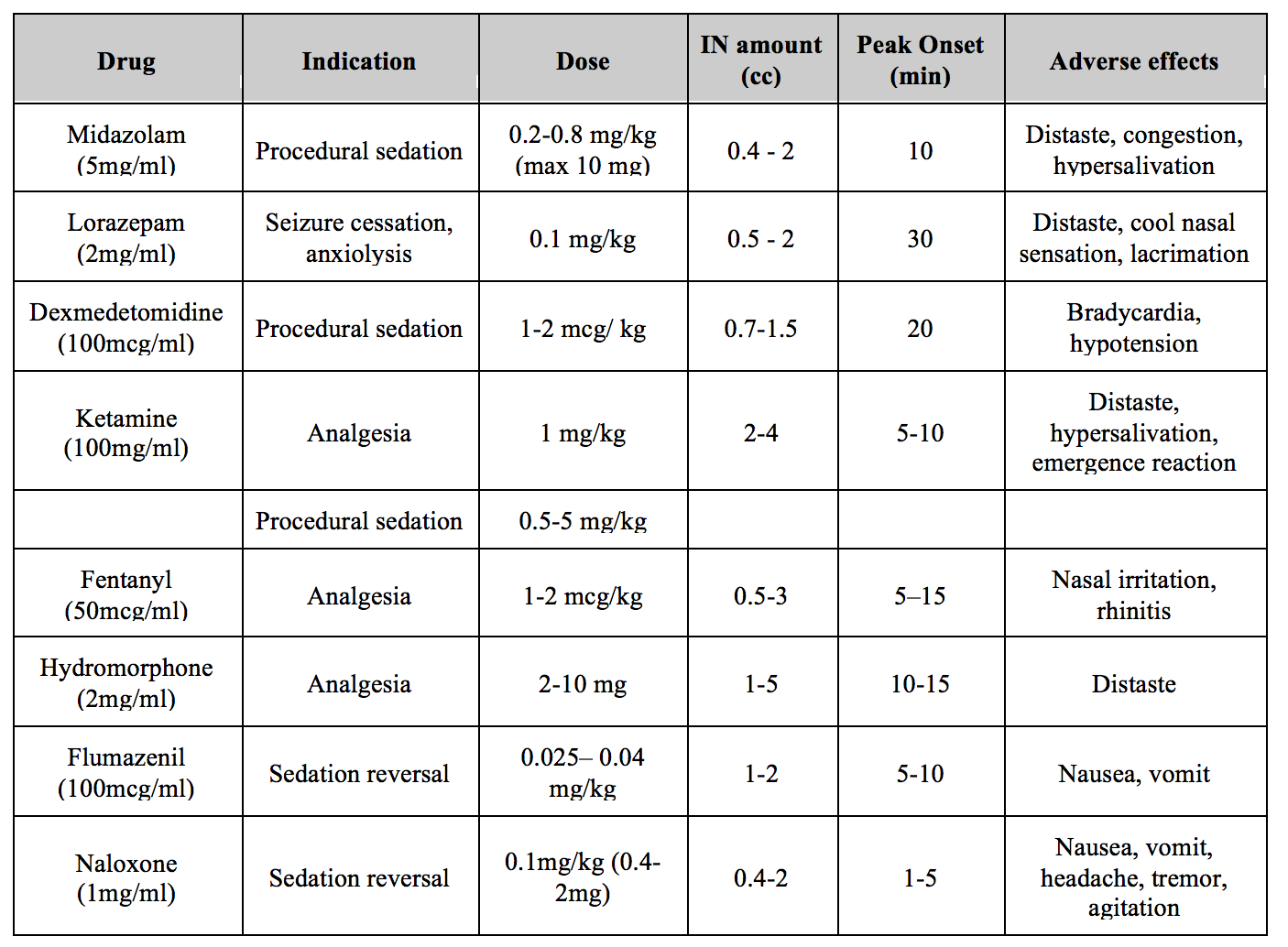
What are the specific uses for the IN medications listed above?
- Midazolam – pediatric procedures, laceration repair, anxiolysis, seizures, adjunct to ketamine (procedural)
- Lorazepam – anxiolysis, nausea/vomiting (add-on therapy), seizures
- Dexmedetomidine – analgesia, anxiolysis, procedural sedation
- Ketamine – analgesia, headache (migraine), depression, procedural sedation
- Fentanyl – acute or breakthrough analgesia, postoperative pain, dressing changes in burn patients (peds)
- Hydromorphone – sickle cell crisis, trauma-related analgesia
- Flumazenil – benzodiazepine overdose
- Naloxone – opioid overdose
Quality Assessment
This was a well-thought, comprehensive review of IN medications conducted by a team of researched and trained PharmD’s. The review offered discussion on each relevant IN medication used in the ED and derived optimal dosing and use based on an extensive literature review of each medication. Though a discussion on how the literature was evaluated and potential studies identified in the discussion was not identified, the review did include a significant number of randomized control trials and prospective studies relevant to the area of intranasal medication administration research.
The Upshot
Increased wait times and understaffed ED’s have resulted in prolonged patient analgesic delivery and decreased patient care satisfaction. Any method which effectively improves pain management while maintaining patient safety should be considered. Bailey, et al have given health care providers a detailed discussion on an instrument for the analgesic toolbox that requires little training or expertise beyond our core knowledge of analgesic pharmacology that works to prevent delays in analgesic administration. High concentrations of low-volume analgesics are well-tolerated by patients with minimal adverse side effects and were described to be just as efficacious as IV administration.
IN medication delivery offers my two most favored characteristics of an analgesic regimen – ‘quick and painless’. I see great utility of this within an emergency setting, beyond just the well-discussed pediatric population. In my experience, sickle cell crisis patients often suffer through long ED wait times, hematology or pain management consults, and multiple IV access attempts, often requiring ultrasound guidance. Administration of IN analgesics while being triaged and worked up could result in an effective bridge prior to initiation of an individualized treatment regimen. This is but one example of IN utilization I envision incorporating into my own pain management practice and I appreciate the overview this article provided to do so.
Further Reading:
- Pediatric EM Morsels by Sean Fox, MD – Intranasal Analgesia
- PEM Playbook by Tim Horeczko, MD – Intranasal Medications and You
- Emergency Physicians Monthly article by Tim Veloriate and Amy Levine, MD** – Nose Candy ** award goes to Amy and Tim for best article title in the category of intranasal analgesia
- Mucosal atomizer device (MAD) instructional video
- An incredibly comprehensive website on all-things intranasal – Intranasal.net
- The use of intranasal analgesia for acute pain control in the emergency department: A literature review. Sin B, Wiafe J, Ciaramella C, Valdez L, Motov SM. Am J Emerg Med. 2018;36(2):310-8.








4 thoughts on “Pain Profiles: Review of Intranasally Administered Medications for Use in the Emergency Department”
Can you elaborate on the avoidance of IN medications in patients with developmental delay?
On the surface this seems like a patient population that could benefit from IN administration.
Pingback: Intra-Nasal Anagesia & Sedation – Anesthesia and Critical Care Update & CME
Great point Joel – it is worth noting that with the exception of a true allergic reaction, all contraindications are relative (potential) contraindications. Optimal effect of administration depends on available surface area for absorption and sufficient delivery, and anything that could preclude intranasal delivery should be considered in context when choosing the delivery option. Though I could not find literature to support a specific case of challenging delivery in patients with development delay, my takeaway was that a development delay has the potential to limit the understanding of the delivery technique and lead to less precise quantities of delivery (ie, variable analgesic effect). Again, this is only relative – trials has demonstrated the successful delivery of intranasal insulin in developmentally delayed patients. And you’re absolutely correct – if sniffing, blowing, and run off can be successfully avoided in these patients, one could argue the safety over an IV needle stick!
Pingback: emDOCs.net – Emergency Medicine EducationPain Profiles: Intranasal Analgesics: What's Your Pick? - Part I - emDOCs.net - Emergency Medicine Education