Author: Brit Long, MD (@long_brit, EM Chief Resident at SAUSHEC, USAF) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital) and Erica Simon, DO (@E_M_Simon)
You’re wading through your third shift in a row in the pediatric area of your emergency department. The last two shifts have been full of coughs and colds. However, today is shaping up to be a completely different story.
Your first patient is five year-old male who presents after a fall with an obvious right forearm deformity. You order an Xray, expecting to sedate him for adequate reduction. Your second patient: a two year-old female who lost her battle with the corner of a table, suffering a four centimeter laceration to her cheek, presents with a Mom who is adamant that the repair is perfect.
What are your options for procedurally sedating these patients? This post will review sedation medications, and discuss their employment in varying ED clinical scenarios.
Background
Procedural sedation is the administration of a sedative or dissociative agent to produce a depressed level of consciousness, while maintaining cardiorespiratory function. When performed adequately, patients exhibit little or no response to, or memory of, the procedure undertaken.
Principles of Sedation
Pediatric sedations are commonly performed by the emergency physician, however, patient factors including obesity, psychiatric disorders, sleep apnea, recent upper respiratory infection, and ASA class 3 or greater (such as cardiac disease) predict the need for sedation in the OR due to increased risk of complications.
For procedural sedations to be performed in the ED, providers should obtain informed consent, anticipate a required level of sedation, and ensure adequate monitoring and rescue equipment (bag/valve mask, suction, airway equipment including intubation setup, cardiovascular monitoring, oximetry, capnography, and intubation medications) are available. As the rule goes, if you’re prepared for the worst, you won’t need it. If you don’t prepare, you can pretty much guarantee that something bad will happen.
Sedation Levels
The following chart offers a review of the differing levels of sedation. As emergency physicians, general anesthesia is what we try to avoid unless intubating.
| Minimal Sedation | Moderate Sedation | Deep Sedation | General Anesthesia | |
| Responsiveness | Normal response to verbal | Purposeful response to verbal or tactile stimulation | Purposeful response following repeated or painful stimulation | Unarousable even with painful stimulus |
| Airway | Unaffected | No intervention required | Intervention may be required | Intervention often required |
| Spontaneous Ventilation | Unaffected | Adequate | May be adequate | Frequently inadequate |
| Cardiovascular Function | Unaffected | Usually maintained | Usually maintained | May be impaired |
From the American Society of Anesthesiologists, 2014.
As an aside: Dissociative sedation is particular to ketamine. Patients appear in a trancelike state of profound analgesia and amnesia. Airway reflexes are generally protected.
Remember…Child life services can be department-savers in any sedation, procedure, or imaging examination. A little Dora the Explorer or SpongeBob on a tablet device can often times preclude the need for medications. If a caregiver’s presence comforts the patient, request that the caregiver remain in place for frightening aspects of the imaging exam or procedure. On the other hand, if the caregiver’s demeanor or appearance are worsening the child’s anxiety, respectfully request that he/she step out.
Treat Pain!
If there will be any pain involved, do not hesitate to give acetaminophen or ibuprofen PO shortly after arrival. If pain is severe, intranasal fentanyl at 1-3mcg/kg is a fast-acting option (onset within 2-3 minutes). What’s this intranasal route, you ask?
The Benefits of the Intranasal Route…
The intranasal route (IN) is relatively painless and has rapid onset. The blood supply to the nose is robust; the nares provide a large surface area for absorption, and the venous drainage of the nose ends in the SVC thereby avoiding the liver’s first pass metabolism. Volumes of 0.3mL per nostril are easily tolerated (the ideal medication for intranasal administration being highly concentrated).
Intranasal medications can allow you to complete a procedure or obtain an IV (which may be the procedure itself). Commonly utilized IN medications include midazolam and fentanyl.
When using intranasal medications:
- A higher concentration of medication formulation is advised (decreases the volume to be administered).
- Utilize both nostrils to increase the absorptive surface area.
Avoid intranasal medications in a patient with URI symptoms as nasal congestion and rhinorrhea may alter absorption.
Sedative Agents
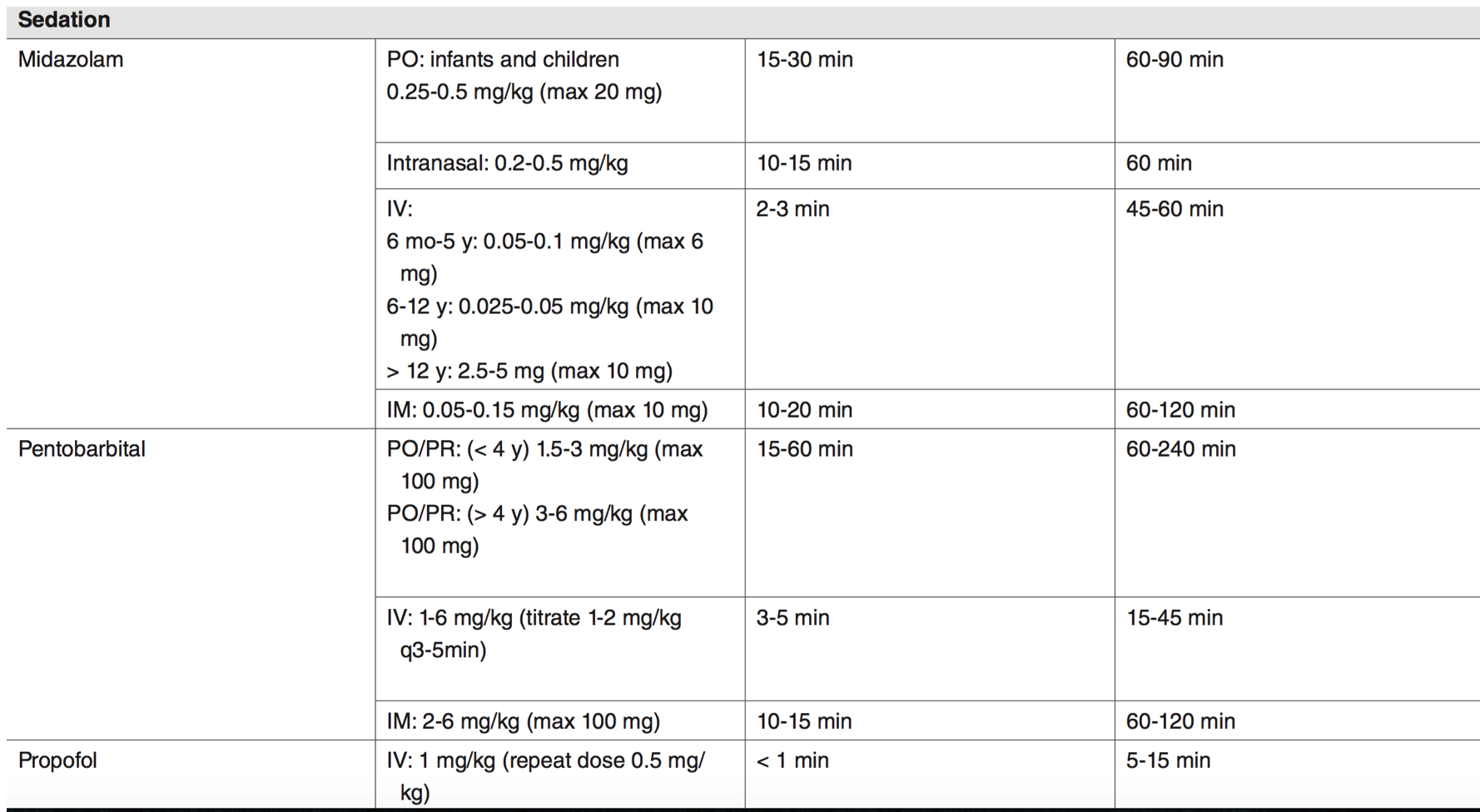
A vast array of medications and delivery routes exist for sedation (Table 1). No one agent is perfect, as multiple options and combinations can be employed. The provider must choose an agent with consideration of the clinical scenario, his/her personal comfort level with the medication, and resources available to him/her.
Table 1 – From EBmedicine.net, Elikashvili I, Vella AD. An Evidence-Based Approach to Pediatric Procedural Sedation. Emergency Medicine Practice 2012 Aug;9(8):1-16.
How do you choose an agent based on the clinical scenario?
The patient’s age and maturity should factor into your decision-making, and the following questions can help guide your choice of medication cocktail:
1. Goal(s) of procedure: Do you want anxiolysis? Do you want sedation? Do you want sedation deep enough to prevent patient movement? Do you want analgesia? Do you want amnesia?
2. Type of procedure: Not painful? Minimally painful? Painful?
3. Time of procedure: Short versus long?
4. Medication route: IV, IN, IM, PO?
From EBmedicine.net, Elikashvili I, Vella AD. An Evidence-Based Approach to Pediatric Procedural Sedation. Emergency Medicine Practice 2012 Aug;9(8):1-16.
Painless Procedure
These procedures will likely involve an attempt to obtain diagnostic imaging in the uncooperative child. Ultimately, you will need sedation to control patient motion. This can be completed through several options:
Oral (PO): Midazolam at 0.2-0.5mg/kg/dose or pentobarbital at 3.5mg/kg/dose.
Intranasal (IN): As seen in Table 1, midazolam at 0.2-0.5mg/kg per dose has an onset of 10-20 minutes and lasts 45-60 minutes and can provide adequate anxiolysis.
Intravenous (IV): Propofol (1mg/kg), ketamine (1-2mg/kg), pentobarbital (2.5mg/kg initial bolus, followed by 1.25mg/kg dosing delivered twice to achieve sedation), and benzodiazepines such as lorazepam and midazolam are options.
A newer agent is dexmedetomidine, provided as an IV drip. This alpha-2 agonist protects airway reflexes, dissociates the patient, and allows for motion control. It provides analgesia, anxiolysis, and sedation. Dosing by textbook is 0.5-1 microgram/kg IV bolus, followed by 0.5 micrograms/kg/hr IV drip, however, caution should be observed as a bolus dose may result in hypotension and bradycardia.
Intramuscular (IM): Ketamine (3-5mg/kg) or midazolam (0.05-0.2mg/kg/dose) are options, however given the increased time to onset, IV administration is often preferred.
Of note, knowledge of the time of onset of these agents is paramount in obtaining desired sedation outcomes.
Maia Rutman discusses in-depth medications for sedation in her 2009 Pediatrics publication. She includes chloral hydrate, pentobarbital, methohexital, and thiopental (not addressed in detail here):
From Rutman MS. Sedation for emergent diagnostic imaging studies in pediatric patients. Curr Opin Pediatr 2009;21:306–312.
Short, Painful Procedure
Then there’s the short, painful procedure, such as a simple laceration repair. Here, the most important factors are anxiolysis and pain control, but patient age is vital in determining which agent to use. In an older child, procedural sedation is often unnecessary as the patient is able to understand the procedure, and can likely be treated with a topical anesthetic such as LET and/or lidocaine injection into the wound, followed by repair.
Contrast this patient to a three year-old who is virtually incapable of sitting still. In this circumstance, you will need sedation, motion control, analgesia, and amnesia. Intravenous ketamine or nebulized nitrous oxide (see below) will allow pain and motion control, as well as sedation and amnesia. Intranasal medications including fentanyl and midazolam are other options if the procedure can be completed within minutes. The downside is determining the optimal time for repair and managing additional dosing, if required.
What about N2O?
Nitrous oxide (N2O) is a weak dissociative agent that provides significant anxiolysis and moderate pain control with rapid recovery. N2O can work well when used to facilitate laceration repairs or orthopedic procedures such as a forearm reduction requiring minimal manipulation. N2O is delivered as nebulized, pre-mixed 50% N2O, 50% oxygen blend, with an onset of action of 3-5 minutes and a recovery time of 3-5 min post discontinuation of the nebulization. The fast onset and recovery times make this agent extremely useful in a busy ED (assuming the necessary equipment for administration is on hand). N2O can also be combined with other medications such as midazolam or fentanyl.
Unknown Procedure Time; Painful Condition
Procedures that are painful and may take an unknown time to complete often require sedation, amnesia, analgesia, and patient motion control.
Examples include:
- Reduction of complex fracture/dislocations
- Complex laceration repairs
- Lumbar punctures
- Central line placement/arterial line placement
Similar to the above section on painless procedures, many of the same medications can be utilized. PO or intranasal routes are optimal to initiate the road to sedation, but obtaining IV access is highly recommend given the ease of administration and ability to perform directed dosing according to observed patient response.
Intravenous Medications:
- Ketamine is one of the most frequently utilized medications for sedation in the ED. It is dosed at 1-2 mg/kg IV initial bolus with a duration of action of 30-60 minutes. Ketamine functions well as an analgesic, and is safe for use in patients suffering from head trauma or exhibiting signs of elevated ICP/IOP. Ketamine may cause emergence reactions and emesis, however, the prevalence of these side effects is very low. Many providers will offer pre-medication with ondansetron prior to ketamine administration in an attempt to reduce post-sedation emesis. Current literature does not support pre-treating with a benzodiazepine to reduce the risk of emergence reactions in pediatric patients.
- Combination therapy includes an analgesic and sedative. Remember, propofol, phenobarbital/pentobarbital, benzos, and etomidate are not analgesics, thus, you are sedating, but not treating the patient’s pain. A combination benzodiazepine and analgesic was the staple for sedation years ago, however, as compared to the options of today, this cocktail has greater risk of cardiorespiratory depression, and should only be utilized if other alternatives do not exist.
- Analgesia with fentanyl or newer fentanyl-like medications are key if not using a dissociative agent. Remifentanil is an ultra-short opioid analgesic with potency equal to fentanyl. It is commonly utilized as a continuous infusion, as its short half-life makes bolus dosing difficult. Dosing ranges from 0.1-0.15 micrograms/kg/min.
- Propofol is the fastest acting sedation medication, with an almost immediate time of onset, and recovery time of 8-10 minutes. Initial dosages range from 0.5-1.0 mg/kg IV. Propofol functions only as a sedative and anti-emetic, not an analgesic. Providing an analgesic, such as fentanyl, 15-20 minutes prior to propofol sedation is a commonly utilized technique. (Care should be taken as to avoid the co-administration of propofol and analgesics as significant respiratory depression may occur).
- Etomidate is dosed at 0.1 mg/kg IV and has no intrinsic analgesic properties. Etomidate reduces the rate of cerebral metabolic oxygen consumption, making it ideal in settings of increased ICP and reduced myocardial function. Etomidate is not ideal, however, in settings in which the absence of patient movement is desired, as its administration may result in myoclonus. Etomidate has a rapid onset and last approximately 10 minutes after administration of the first dose. Similar to propofol, pre-treatment with an analgesic is recommended.
- Benzodiazepines such as midazolam (0.05-0.2 mg/kg IV) and lorazepam (0.05-0.1mg/kg IV) are often used in combination with remifentanil, as benzo’s do not treat pain. Unfortunately, in the young these medications may result in cardiorespiratory depression and paradoxical excitation.
- Pentobarbital has a rapid onset (1-2 minutes) but a prolonged duration of action of 2-4 hours (2.5mg/kg IV initial bolus). If the bolus dose is ineffective, a 1.25mg/kg IV dose may subsequently be given.
What about Ketofol?
Ketofol, administered by IV, is a combination of propofol and ketamine. Given alone, ketamine may cause vomiting, hypersalivation, and agitation during the recovery period, and as previously mentioned, administered alone, propofol may cause respiratory depression/apnea and hypotension. Current studies demonstrate these side effects as dose-dependent, therefore it is thought that combining the two agents decreases side-effect occurence. Ketofol can be prepared in varying ratios (ketamine to propofol 1:1, 1:4, 1:2, 2:1, etc.). All regimens are safe, however, a 2015 study by Miner, et al. found an increased propofol ratio (1:4 ketamine to propofol) to be associated with improved anesthesia, anxiolysis, and patient satisfaction. There was, however, an increase in respiratory depression (treated with jaw thrust, and stimulation of the patient). Increases in the ketamine component (1:1 ratio) resulted in fewer respiratory events, but increased agitation during recovery. Ultimately, similar to identifying an appropriate sedation agent for the clinical scenario, the ketamine-to-propofol ratio is at the user’s discretion.
Lumbar Puncture
Many providers may not provide analgesia prior to performing a lumbar puncture, as it’s a common myth that neonates do not feel pain. Nociception develops around 30 weeks of gestation, and adequate pain control will maximize your success in this often-important procedure. Topical lidocaine such as LMX 4%, is recommended and has an onset of 30 minutes, so it is important to apply this anesthetic to the potential site while completing the history, physical examination, and orders if feasible.
For young infants, oral sucrose is an effective agent. For patients > 6 months of age, IN or PO midazolam can assist with anxiolysis and amnesia.
After utilizing the above medications, remember that local lidocaine injection is useful.
Rapid Control for Behavior/Psychiatric Complaint
This situation produces a great deal of anxiety amongst providers. Unlike an agitated adult patient, an unruly pediatric patient requiring sedation so as to avoid harm to self or others, is a rare occurence in the ED. If the disruptive patient was previously diagnosed with an anxiety or behavioral disorder, and prescribed PO pharmacotherapy, it is important to utilize the medication that he/she is taking to treat acute symptomatology, in order to limit side effects and drug-drug interactions.
For patients without previously prescribed medications, use lorazepam 0.05mg/kg/dose PO/IV/IM, diazepam 0.04-0.2mg/kg/dose PO/IV/IM, or diphenhydramine 1mg/kg/dose PO/IM/IV to control anxiety.
For psychosis, aggression, or loss of impulse control, use risperidone 0.25 mg PO, olanzapine 2.5mg PO, ziprasidone 10mg IM (for teenagers), or haloperidol 0.025-0.075 mg/kg/dose IM.
Finally, ketamine is a great option for rapid control of all behavioral issues and is dosed at 1 mg/kg IV or 4-5 mg/kg IM. A prior emDocs post provides a succinct summary of adult, pediatric, and geriatric medications for acute behavior control: http://www.emdocs.net/the-art-of-the-ed-takedown/.
Adverse Side Effects/Contraindications:
Here’s a quick run down and recap of the side effects and contraindications of the sedation medications highlighted:
Conclusion
Procedural sedation for pediatric patients is common in the ED setting. Treating pain and utilizing distraction techniques are vital to success. Ultimately, medications employed should be chosen based upon: the patient’s age, the duration of the procedure, the desired patient response to sedation, the determined need for analgesia, the patient’s co-morbidities (see contraindications), medication availability, and your own personal comfort level with the agent.
*Note: We did not discuss rectal forms of medications, though they are listed in the tables above.
References/Further Reading:
-Ali S, Mcgrath T, Drendel AL. An Evidence-Based Approach to Minimizing Acute Procedural Pain in the Emergency Department and Beyond. Pediatr Emerg Care. 2016;32(1):36-42.
-Del Pizzo J1, Callahan JM. Intranasal medications in pediatric emergency medicine. Pediatr Emerg Care. 2014 Jul;30(7):496-501; quiz 502-4.
-Elikashvili I, Vella AD. An Evidence-Based Approach to Pediatric Procedural Sedation. Emergency Medicine Practice 2012 Aug;9(8):1-16.
-Godwin SA, Burton JH, Gerardo CJ, et al. Clinical policy: procedural sedation and analgesia in the emergency department. Ann Emerg Med. 2014;63(2):247-58.e18.
-Grunwell JR, Mccracken C, Fortenberry J, Stockwell J, Kamat P. Risk factors leading to failed procedural sedation in children outside the operating room. Pediatr Emerg Care. 2014;30(6):381-7.
-Migita RT, Klein EJ, Garrison MM. Sedation and analgesia for pediatric fracture reduction in the emergency department: a systematic review. Arch Pediatr Adolesc Med. 2006;160(1):46-51.
-Miner, JR et al. Randomized, double-blinded, clinical trial of propofol, 1:1 propofol/ketamine, and 4:1 propofol/ketamine for deep procedural sedation in the emergency department. Ann Emerg Med. 2015 May;65(5)479-488.
-Roback MG, Wathen JE, Bajaj L, Bothner JP. Adverse events associated with procedural sedation and analgesia in a pediatric emergency department: a comparison of common parenteral drugs. Acad Emerg Med. 2005;12(6):508-13.
-Rutman MS. Sedation for emergent diagnostic imaging studies in pediatric patients. Curr Opin Pediatr 2009;21:306–312.
-Stevens B, Yamada J, Lee GY, Ohlsson A. Sucrose for analgesia in newborn infants undergoing painful procedures. Cochrane Database Syst Rev. 2013;1:CD001069.
-Tobias J and Leder M. Procedural sedations: a review of sedative agents, monitoring, and management of complications. Saudi J Anaesth. 2011; 5(4):395-410.
-Quality Management and Departmental Administration. Continuum of depth of sedation: definition of general anesthesia and levels of sedation/analgesia. American Society of Anesthesiologists. 2014. Available at http://www.asahq.org/~/ media/Sites/ASAHQ/Files/Public/Resources/standards-guidelines/continuum-of-depth-of-sedation-definition-of-general-anesthesia-and-levels-of-sedation-analgesia.pdf
-Zier JL, Liu M. Safety of high-concentration nitrous oxide by nasal mask for pediatric procedural sedation: experience with 7802 cases. Pediatr Emerg Care. 2011;27(12):1107-12.













2 thoughts on “Pediatric Procedural Sedation: What are your options?”
Pingback: emDOCs.net – Emergency Medicine EducationJournalFeed Weekly Wrap-Up - emDOCs.net - Emergency Medicine Education
Pingback: Conference Recap 8/23/2023 – BMC EM Blog