Platelets and ddAVP in the Management of Intracranial Hemorrhage
By Jeremy Kim MD
EM Resident Physician
Mount Sinai Medical Center
Edited by Alex Koyfman, MD (@EMHighAK) and Stephen Alerhand, MD
Clinical Scenario:
You are caring for a 72-year-old M with CAD (taking aspirin/clopidogrel) who was brought to the ED after a fall. He is alert and oriented with a benign neurological exam. The non-contrast CT reveals a subdural hematoma. What are some special considerations in the management of this patient?
Introduction
Are patients taking anti-platelet agents at higher risk of developing intracranial hemorrhage (ICH)?
- Thrift et al, 1999: a case-control study with 331 patients with ICH showed an odds ratio of 3.05 for aspirin use in moderate-to-high doses (defined as >1225 mg/wk), whereas an increased odds ratio was not demonstrated in the use in low-to-moderate doses.
- Saloheimo et al, 2006: a population-based study of 208 subjects with ICH identified regular aspirin use (median dose of 250mg) as an independent risk factor for 3-month mortality (RR 2.5).
- Toyoda et al, 2005: similarly, a review of 251 patients with ICH identified anti-platelet therapy as an independent predictor for “hematoma enlargement, emergent death, and evacuation surgery.”
Furthermore, the use of aspirin in combination with clopidogrel was demonstrated to produce a significantly greater anti-platelet effect compared to the use of aspirin alone, demonstrated by biochemical studies in a randomized trial of 70 patients with ischemic strokes (Serebruany et al, 2005).
Background
Platelets are recruited to the site of endothelial damage and adhere to subendothelial collagen by vWF and GP1b. Further platelet recruitment/aggregation is propagated by key components including COX-1, TXA2, ADP, and GPIIb-IIIa.
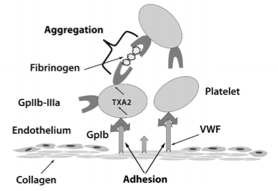
[Picture source: Beshay et al, 2010]
- Aspirin = an irreversible COX-1 inhibitor à dec TXA2 production à dec platelet activation/aggregation. It is rapidly metabolized into ineffective metabolites leading to a short duration of effect.
- Thienopyridines (clopidogrel, ticlopidine, prasugrel) = class of drugs that acts as an ADP-receptor inhibitor. These drugs have active metabolites leading to a longer duration of effect of up to 5-7 days (Beshay, 2010).
- ddAVP (desmopressin): thought to contribute to platelet activation pathway by promoting vWF production. Side effects may include hyponatremia, seizures, and elevated ICP (Campbell, 2010).
Reversal of anti-platelet agents
The concern for patients taking anti-platelet therapy who develop an ICH is that the hemorrhage can expand and lead to worse clinical outcomes. However, the literature does not consistently demonstrate that the use of anti-platelet agents prior to an ICH leads to poor clinical outcomes nor does it consistently demonstrate that reversal leads to improved outcomes.
- Sansing et al, 2009: a randomized control of 282 patients showed that the use of anti-platelet therapy was not associated with “increased hemorrhage volumes, hemorrhage expansion or clinical outcome at 90 days.”
- Downey et al, 2009: a multicenter retrospective review of older adult patients who sustained head injury while using aspirin or clopidogrel. Comparing the 166 patients who received platelet transfusions and the 162 who did not, there was no significant difference in mortality.
- Gratz et al, 1992: a randomized double-blind study of 65 patients (randomized to receiving ddAVP 0.3 mcg/kg or to receiving placebo) showed a significant reduction in postoperative blood loss in the ddAVP group.
Proposed management in ICH
1) Expert opinion (Weingart, 2013)
Any patient who took anti-platelets agents in last 24 hours (including aspirin and clopidogrel)
- 6 units of platelets (or single-donor packed platelets)
- ddAVP 0.3 mcg/kg x 1 (20 mcg in 50 cc NS over 15-30 mins)
2) Campbell et al. produced a 2010 clinical review of literature regarding emergency reversal of anti-platelet agents and proposed the following algorithm for the management in ICH (whether traumatic or spontaneous in etiology):
- If patient takes aspirin alone: give 5 units of platelets
- If patient takes any thienopyridine:
- Small ICH – give 10 units of platelets
- Large ICH – give ddAVP and 10 units of platelets; followed by 10 units of platelets q12h x 48 hrs
Take-Home Points
- Anti-platelet agents are commonly used by patients, particularly those with history of CAD or CVA
- Aspirin is an irreversible COX-1 inhibitor with ineffective metabolites, leading to short duration of effect. Clopidogrel has active metabolites, leading to a longer duration of effect.
- Current literature is not conclusive for management/reversal of anti-platelet agents
- For patients with ICH or highly suspected to have ICH, consider administering:
- 1-2 single-donor packed platelets and ddAVP (0.3 mcg/kg)
- Consider further platelet transfusions and ddAVP doses for larger bleeds or for dual anti-platelet therapy
Additional References
- 1) Beshay JE, Morgan H, Madden C, Yu W, Sarode R. “Emergency reversal of anticoagulation and antiplatelet therapies in neurosurgical patients.” J Neurosurg. 2010; 112:307-318.
- 2) Campbell PG, Sen A, Yadia S, Jabbour P, Jallo J. “Emergency reversal of antiplatelet agents in patients presenting with an intracranial hemorrhage: a clinical review.” World Neurosurg. 2010 Aug-Sep;74(2-3): 279-85.
- 3) Downey DM, Monson B, Butler KL, Fortuna GR, Saxe JM, Dolan JP, Markert RJ, McCarthy MC. “Does platelet administration affect mortality in elderly head-injured patients taking antiplatelet medications.” Amer Surg. 2009 Nov; 75(11):1100-1103.
- 4) Gratz I, Koehler J, Olsen D, Afshar M, DeCastro N, Spagna PM, Ablaza SG, Larijani GE. “The effect of desmopressin acetate on postoperative hemorrhage in patients receiving aspiring therapy before coronary artery bypass operations.” J of Thor and Cardiovasc Surg. 1992; 104(5):1417-1422.
- 5) Nishijima DK et al. “Immediate and delayed traumatic intracranial hemorrhage in patients with head trauma and pre-injury warfarin or clopidogrel use.” Ann Emerg Med. 2012 Jun;59(6):460-8.
- 6) Saloheimo P, Ahonen M, Juvela S, Pyhtinen J, Savolainen ER, Hillbom M. “Regular aspirin-use preceding the onset of primary intracerebral hemorrhage is an independent predictor for death.” Stroke. 2006 Jan;37(1)129-33.
- 7) Sansing LH, Messe SR, Cucchiara BL, Cohen SN, Lyden PD, Kasner SE. “Prior antiplatelet use does not affect hemorrhage growth or outcome after ICH.” Neurology. 2009 Apr; 72(16):1397-1402.
- 8) Serebuany VL, Malinin AI, Ziai W, Pokov AN, Bhatt DL, Alberts MJ, Hanley DF. “Effects of clopidogrel and aspirin in combination versus aspirin alone on platelet activation and major receptor expression in patients after recent ischemic stroke: for the Plavix use for Treatment of Stroke (PLUTO-Stroke) trial.” Stroke. 2005; 36:2289-2292.
- 9) Thrift AG, McNeil JJ, Forbes A, Donnan GA. “Risk of primary intracerebral haemorrhage associated with aspirin and non-steroidal anti-inflammatory drugs: case-control study. BMJ. 1999;318:759.
- 10) Toyoda M, Okda Y, Minematsu K, Kamouchi M, Fujimoto S, Ibayashi S, Inoue T. “Antiplatelet therapy contributes to acute deterioration of intracerebral hemorrhage.” Neurology. 2005 Oct;65(7):1000-1004.
- 11) Weingart S. “EMCrit Podcast 17 – Reversal of anti-coagulant and anti-platelet drugs in head bleeds. EMCrit Blog. <http://emcrit.org/podcasts/reversal-head-bleeds/> Last updated 8/2013. Viewed 8/2014.





