Authors: Joseph R. Peters, DO, RDMS, FACOEP, FACEP, FACOI and Matt DeGroot, DO (Academic Department of Emergency Medicine, University of Illinois College of Medicine, Peoria, IL, OSF St Francis Medical Center Emergency Department) // Reviewed by: Stephen Alerhand, MD; Manny Singh, MD (@MPrizzleER); Brit Long, MD (@long_brit)
Case
A 65-year-old male arrived to the Emergency Department (ED) via EMS with a complaint of severe bilateral knee pain after a fall. The patient reported walking down the basement stairs to retrieve his dog when his feet suddenly slipped out from under him on the last two steps. He landed on the basement floor in the standing position, with both quadriceps immediately going into severe spasm, causing him to initially fall backward onto the stairs. Attempting to stand up, he experienced severe bilateral knee pain causing him to fall forward over a gate at the bottom of the stairs, landing in the prone position but without head trauma or loss of consciousness. As a result of the pain and the inability to get up, he used his cellular phone to call EMS for transport to the ED. He denied any other acute injury, other medical conditions, daily medications, or prior knee conditions. He denied chronic steroid use or fluoroquinolone use.
Physical exam demonstrated excessive swelling and tenderness of each knee. He resisted passive range of motion of the knee. Active attempts to perform straight-leg raises revealed ability to slightly elevate the knees but inability to raise either foot off the bed.
With suspicion of a bilateral extensor mechanism injury of his knees, POCUS of each patellar tendon was performed utilizing a 12-4mhz transducer, obtaining long-axis views of each infrapatellar region. POCUS confirmed bilateral patellar tendon avulsions. Knee x-rays were performed subsequently, revealing small bone chips, bilateral patella alta, but no other major fractures.
Orthopedic surgery was consulted, the patient was placed in bilateral knee immobilizers and admitted for surgery the next day. On the basis of the mechanism of injury, physical exam, x-rays and confirmatory POCUS findings, the surgeon did not require an MRI to confirm the diagnosis.
Discussion
In the ED, musculoskeletal soft tissue injuries can be difficult to diagnose, given that acute pain limits the physical exam and standard radiologic modalities (X-ray, CT). Ligamentous and tendon injuries are particularly difficult to confirm as many EPs do not have immediate access to MRI.
Patellar tendon avulsion is one of four extensor mechanism injuries of the knee, which also include avulsion of the quadriceps tendon from the superior patella, transverse fracture of the patella, and avulsion fracture of the tibial tuberosity (1). Injury of the patellar tendon is the third most common injury of the knee extensor mechanism, surpassed in number by patellar fractures and quadriceps tendon rupture (2). The most common area of injury of the patellar tendon is a proximal tendon avulsion from the inferior pole of the patella bone (2). The injury most often occurs in patients less than age 40 and is associated with physical activities (2). Tendinopathy induced by repetitive microtrauma or systemic conditions including collagen vascular disease, diabetes, chronic renal disease, chronic steroid use, and fluoroquinolone use, predispose older individuals to the injury (1,2,3,5,9). Obesity is considered a predisposing factor in knee extensor mechanism injuries (2). Patellar tendon rupture is considered rare (5).
Extensor mechanism injury of the knee occurs via indirect and direct forces (1,5). The more common indirect injury results from forced flexion of the knee when the quadriceps is contracted (1,4,5). One study noted that it takes 17.5 times body weight force to avulse the tendon in healthy adults (2). Our patient described a mechanism of forced flexion of both knees as his quadriceps likely contracted when landing on his feet at the bottom of the stairs. The less common direct injury occurs with violent impact on the anterior surface of the knee and is more common in children and adolescents (2).
Physical exam findings of extensor mechanism injuries of the knee include swelling, loss of tone of the tendon, high-riding patella, and inability to perform active extension of the knee. Patella alta, or high-riding patella, can be seen on examination and knee radiographs. It is not specific for extensor mechanism injuries, however, and several other conditions are known to be associated with patella alta including, idiopathic retropatellar pain, recurrent dislocation of the patella, chondromalacia patella, knee joint effusion, spastic cerebral palsy (6).
On lateral knee radiographs, measuring the Insall-Salvati ratio is one way to diagnose patella alta (Image 1). This is performed most often by the radiologist, comparing the patella tendon length (LT)/patella bone length (LP) ratio. An abnormal LT/LP ratio is >1.2 (normal 0.8 to 1.2) (7). However, the accuracy of the ratio requires standard positioning with the knee flexed at 30 degrees. Acute pain and limited mobility of the knee may affect standard positioning. Off-angle x-ray beam or non-standard position may create a spuriously abnormal ratio (6). Shape of the patella bone also affects the ratio (8).
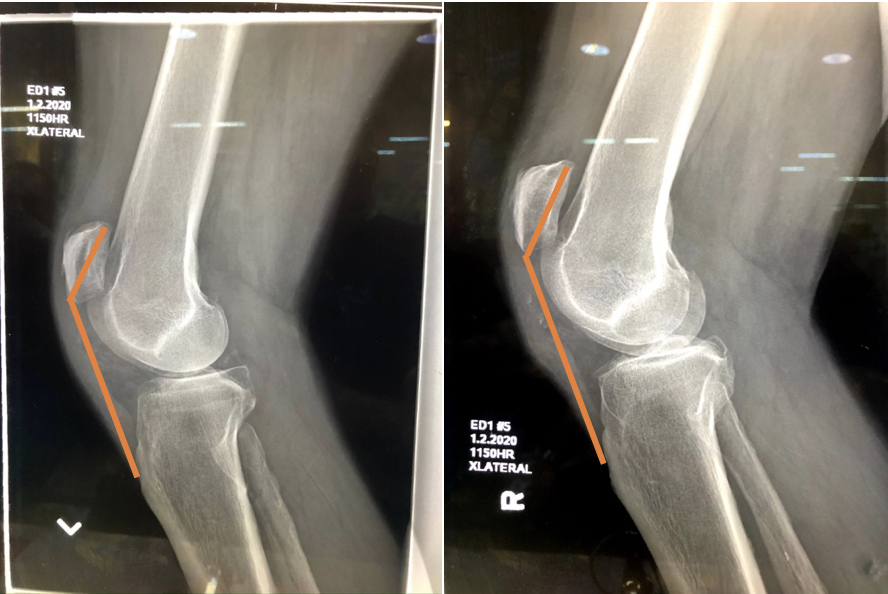
Image 1: Our patient, “Patella Alta” Bilateral
Timely diagnosis is important because prognosis depends in part on the interval between injury and repair (9). POCUS is an ideal modality to diagnose patella tendon avulsion because it is a bedside modality that lacks radiation, the extensor mechanism anatomy is superficial and easily identified, and it is low cost. Ultrasound visually confirms the diagnosis, mobilizing consultants and definitive care rapidly.
Tendons are described as a bright echogenic (white) fibrillar appearing linear band, without defects, when imaged at a perpendicular angle in the long axis (10, Image 2). Tendons have the property of anisotropy which means that the brightness and fibrillar appearance varies depending on the angle of the ultrasound beam (10). When not imaged in perpendicular fashion, a tendon can appear disrupted, when in fact the less-than perpendicular beam angle creates hypoechoic (black) artifact within the fibrils, appearing as an avulsion or tear (10). Adjusting the beam angle to perpendicular over the tendon will eliminate anisotropic artifact.
The exam is performed by placing the ultrasound transducer in the long axis balanced between the inferior aspect of the patella bone and the tibial tuberosity (image 2, video1). The probe can be maneuvered side-to-side and cephalad-caudad to image the patellar tendon in its entirety. The patellar tendon is visible and attached to the patella bone and tibial tuberosity, highlighting it is actually a ligament (Image 2).
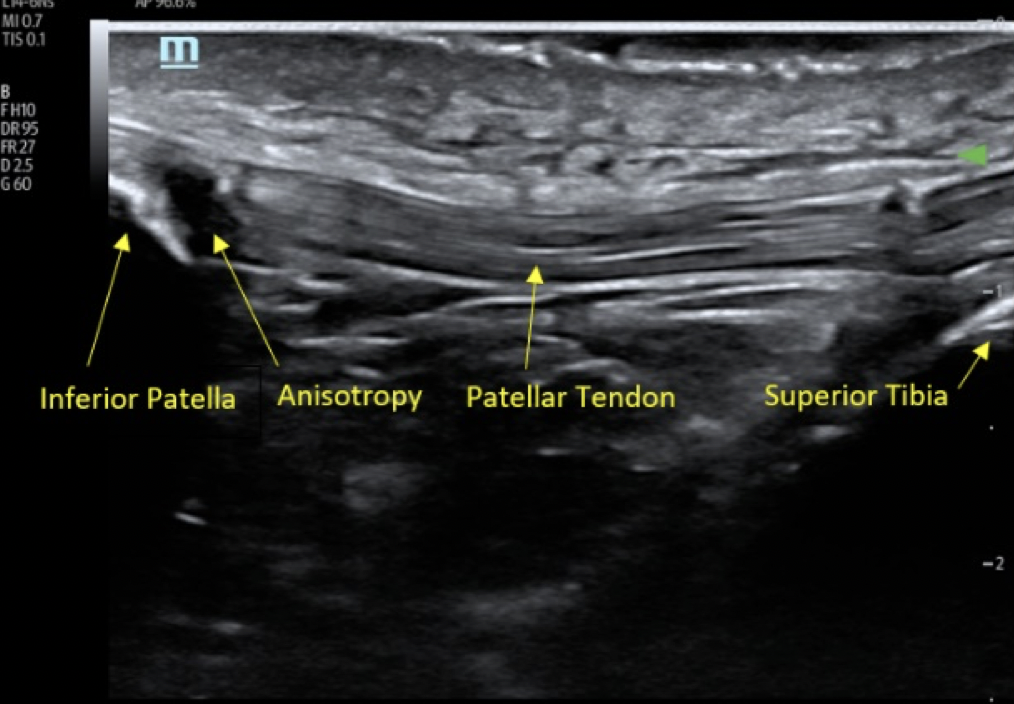
Image 2

Video 1
When a true avulsion or tear is present, the defect will be visualized at multiple beam angles. Additionally, bone fragments, blunt edges of tendon, and hematoma (black fluid) will often be seen with patellar tendon avulsion. These findings were present in our patient (Images 3,4 and video 2,3).

Image 3
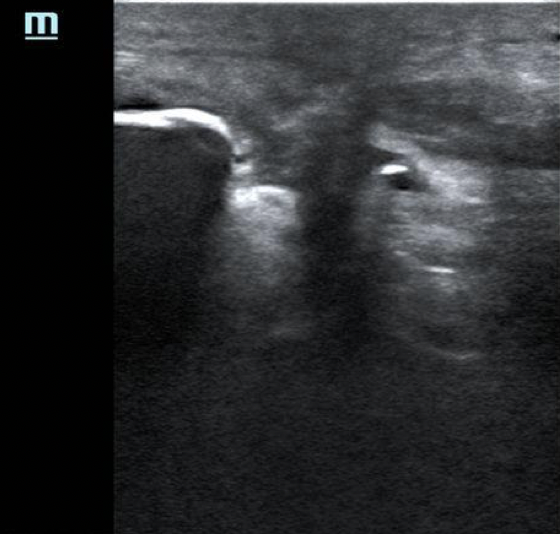
Image 4

Video 2
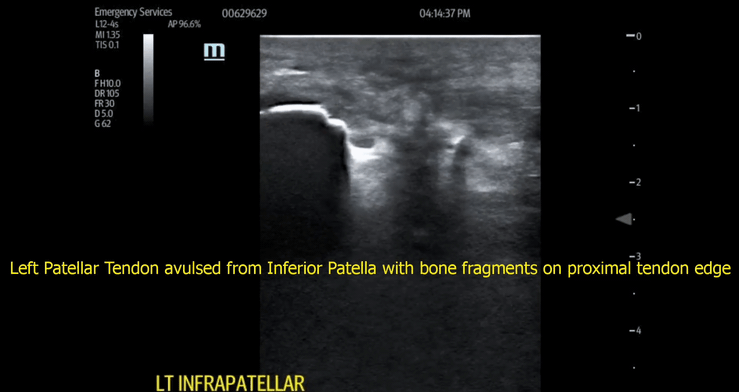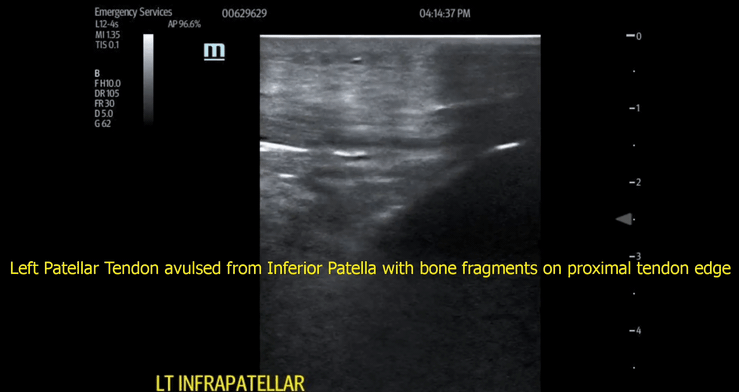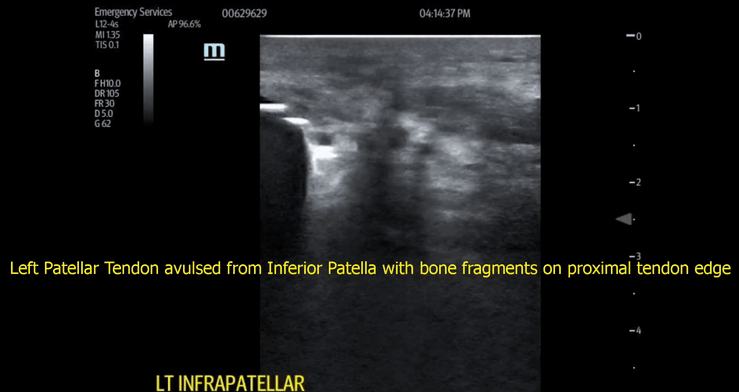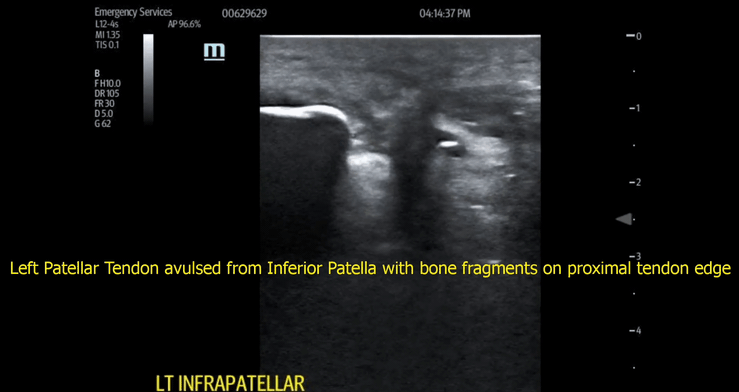
Video 3
Our patient was placed in bilateral knee immobilizers and admitted to the hospital for operative repair. The history and physical exam, combined with POCUS and knee x-rays diagnosing bilateral patellar tendon avulsions, expedited orthopedic consultation and surgery.
Conclusion
This is a case presentation of bilateral patellar tendon avulsion diagnosed by the recognition of typical exam findings, X-ray findings, and confirmed by POCUS. When combined with history and exam, POCUS can assist in the diagnosis of musculoskeletal injuries, including extensor mechanism injuries of the knee.
References/Further Reading:
- Simon K., Koenigsknecht S. Emergency Orthopedics the Extremities, McGraw-Hill, pgs 449-450, 4th, 2001.
- Albuquerque et al, Epidemiological Study on Tendon Ruptures of the Knee Extensor Mechanism at a level 1 Hospital. Rev Bras Ortop. 2015 Nov 4;47(6):719-23. doi: 10.1016/S2255-4971(15)30028-8. PMID: 27047890; PMCID: PMC4799490
- Rosa B, Campos P, Barros A, Karmali S, Gonçalves R. Spontaneous bilateral patellar tendon rupture: case report and review of fluoroquinolone-induced tendinopathy. Clinical Case Reports. 2016 Jul;4(7):678-681. DOI: 10.1002/ccr3.592.
- Sochart DH, Shravat BP. Bilateral patellar tendon disruption–a professional predisposition?.J Accid Emerg Med. 1994;11(4):255-256. doi:10.1136/emj.11.4.255
- Pengas IP, Assiotis A, Khan W, Spalding T. Adult native knee extensor mechanism ruptures. Injury. 2016 Oct;47(10):2065-2070. doi: 10.1016/j.injury.2016.06.032. Epub 2016 Jun 27. PMID: 27423309.
- TY Jin and Y Weerakkody et al, https://radiopaedia.org/articles/patella-alta?lang=us
- D Roberts and F Gaillard et al, https://radiopaedia.org/articles/insall-salvati-ratio?lang=us
- Grelsamer RP, Meadows S. The modified Insall-Salvati ratio for assessment of patellar height. Clinical Orthopaedics and Related Research. 1992 Sep(282):170-176.
- Matava MJ. Patellar Tendon Ruptures. J Am Acad Orthop Surg. 1996 Nov;4(6):287-296. doi: 10.5435/00124635-199611000-00001. PMID: 10797196.
- Moore, A Practical Guide to Sonography of the Extremities, pg intro 5, 3rd ed, 2007






1 thought on “POCUS diagnosis: simultaneous bilateral patellar tendon avulsions”
Very informative, thank you for this good case.