Background
As of 2008, the Nation Emergency Medical Services Information System (NEMSIS) data from 16 states reported 4 million EMS activations with over 88,000 airway interventions ranging from bag valve mask to cricothyroidotomy.1 Although the bag valve mask and endotracheal tube remain the cornerstones of airway management, many alternatives have emerged in prehospital care. Availability of airway adjuncts will depend upon training and local department purchasing. This review will discuss the basics of extraglottic airway adjuncts available for prehospital airway management in adults and pediatrics.
Extraglottic devices, or supraglottic airways as they are commonly called, insert through the patient’s oropharynx and temporarily manage ventilation. The devices do not pass through the vocal cords and only act as a temporary, not definitive, airway. Some devices have both supraglottic and infraglottic structures, making the name extraglottic the most encompassing term. Aspiration of gastric contents can occur while the devices are in place, making the endotracheal tube (ETT) the only definitive airway.
The Laryngeal Mask Airway (LMA)
In 1981, Dr. Archie Brain invented the first extraglottic airway device, the LMA Classic. The cLMA, was first sold in the United Kingdom in 1988 and then in the United States in 1992 by LMA North America. The cLMA, a reusable device, exists for prehospital care as the LMA-Unique (disposable), LMA Fastrach (disposable with ability to intubate through), LMA ProSeal (additional gastric suction port), and LMA Supreme (Proseal plus biteblock). When inserted the LMA follows the path of a food bolus moving along the hard palate to the hypopharynx and then to the esophagus. Finally the LMA sits with the distal tip posterior to cricoid cartilage and masks the glottis for ventilation.2
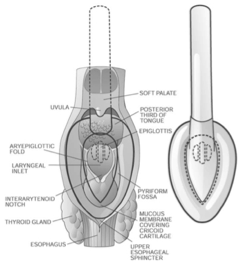
A meta-analysis of randomized trials in 1994 compared the LMA to the ETT and BVM. Compared to BVM, a LMA was easier to place by new trainees, and improved oxygen saturations. Compared to an ETT, the LMA increased speed of placement but the ETT demonstrated higher seal pressure and less gastric insufflation.3
In pediatrics the LMA also serves as a well documented rescue device for “can’t intubate, can’t ventilate” situations. Sizes for the LMA range from 1kg neonates to >70kg patients.4
Esophageal Tracheal Combitube (ETC)
Described in 1987, by Dr. Frass in Austria, the ETC, or commonly called the Combitube, functioned as a resuscitation rescue device from the beginning. Unlike the LMA which anesthesiologist used before prehospital providers, the Combitube focused primary on the prehospital and emergency environment. The Combitube, is a disposable double-lumen double cuffed device commonly inserted into the patient’s esophagus but 5% of the time inserted into the trachea. The provider blindly inserts the device and either via auscultation or capnometry confirms placement in the esophagus or trachea by ventilating trough one of the two ports. For tracheal intubation ventilation occurs via the more distal lumen and for esophageal placement ventilation occurs via the proximal lumen.
The major criticism of this device stems from the multi-lumen design. In stressful emergent situations prehospital providers must spend time determining the correct port for ventilation.5 The Combitube has no place in pediatric airway management since Covidien only produces two sizes for adults.
Laryngeal Tube (LT)
VBM Medizintechnik GmbH in Germany in 1999, created the LT in response to criticism regarding the multi-lumen difficulties of the Combitube. The LT gained in popularity in the United States for prehospital use when King Systems produced a disposable version in 2003. The LT by design eliminated the 5% of tracheal intubations that occurred when using the Combitube freeing prehospital providers from deciding which port to use for ventilation. The LT has an oropharyngeal end esophageal inflatable cuff and a single lumen ventilation lumen. Both cuffs inflate with one port.6 The LT constantly achieves esophageal intubation and but if tracheal intubation were to occur the provider could not ventilate the patient.7 Novice providers have also demonstrated rapid insertion times for the LT half as long as tradition ETT placement.8 King Systems currently produces a size two LT which accommodates patients as small as 12kg. Smaller pediatric disposable LT sizes have not been manufactured in the United States.
LMA Fastrach
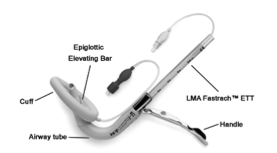
Stemming from the success of the LMA classic, Dr. Brain developed the Fastrach LMA (FT-LMA) to allow for blind intubation through the device. The FT-LMA, also referred to as the intubating LMA, has a larger internal diameter to accommodate a proprietary ETT, a rigid airway tube, an epiglottic elevating bar, and a tracheal tube guiding ramp.9 A multicenter study demonstrated a blind intubation success rate with the special manufacturer ETT of 96.2%.10 The FT-LMA does not accommodate sizes for pediatric use.
I-Gel

In 2003, in the UK, Intersurgical Ltd. developed the i-gel. The device similar to the LMA differs mainly by the lack of an inflatable laryngeal mask. Intersurgical manufactures the device from thermoplastic elastomer to conform precisely to the laryngeal and laryngeal anatomy. The device in theory should provide a greater seal pressure and increased speed of insertion by not requiring inflation.12 A recent study on hands off time in CPR during a cardiac arrest did not demonstrate a time savings using the i-gel vs. other extraglottic devices.13 The i-gel similar to the LMA supports sizes down to neonates.
Air-Q
In 2004, Dr. Daniel Cook, founder of Cookgas developed an alternative to the FT-LMA. The Air-Q, similar to the FT-LMA allows for blind intubation once the device has been placed. Unlike the FT-LMA the air-Q has a shorter and larger bore ventilating lumen with a removable ventilation connector. The modifications were designed to eliminate the difficulty many providers experienced when intubating through the FT-LMA. A shorter ventilation lumen should allow easier removal of the device over the ETT once in place. Also the air-Q does not require a proprietary ETT, but supports the standard polyvinyl chloride tube found in most intubation kits.11 The air-Q supports sizes down to neonates.
Current Controversies
Within the last 10 years large scale prehospital trials have focused on neurologic outcomes in out of hospital cardiac arrest (OHCA) among different airway interventions. It is not enough to have return of spontaneous circulation if there is significant morbidity as a result. In Japan, a nationwide observational study of all out-of-hospital cardiac arrest between 2005-2007 demonstrated slightly poorer one-month neurologic outcomes in the patients whose airways were managed with extraglottic devices. Neurologically favorable one month survival was associated with slightly, but significantly, poorer neurological outcomes compared with tracheal intubation.15 A more recent study with a greater number of OHCAs in Japan from 2005-2010 demonstrated that any ETT, ETC, LMA, or LT was associated with a decreased neurologically favorable survival.16 For pediatrics (age ≤12) no clear neurologic or survival benefit has been demonstrated between ETI and BVM in prehospital airway management.13
Overview
With a multitude of extraglottic devices on the market the LMA and LT remain the most common in the prehospital setting due to simplicity of use and reliability. For pediatric use, the LMA has the largest range of sizes and clinical literature backing its use, although no large prehospital studies have been performed. BVM should still function as the best and most reliable means of ventilating a child in the prehospital environment.19 Future extraglottic devices for prehospital use may include the FT-LMA and Air-Q. Both allow the option to attempt blind intubation through the device. No studies have demonstrated benefits of converting from an extraglottic device to an ETT. None of the new devices such as FT-LMA, i-gel, or air-Q, have any adult or pediatric prehospital data to support their widespread adoption. For austere environments the Combitube requires the most force to dislodge (28.3lbs of force) while the King is most easily dislodged (12.5lbs of force). The Army equips field medics with LTs and Combitubes. Just as with endotracheal intubation proficiency and successful placement requires continue practice on patients and during simulation. Lastly, 2010 American Heart Association recommend chest compressions take priority over establishing a patients airway as to minimize hands off time during cardiac arrest.
References / Further Reading
- Wang HE, Mann NC, Mears G, Jacobson K, Yealy DM. Out-of-hospital airway management in the United States. Resuscitation. 2011:378–385. http://www.ncbi.nlm.nih.gov/pubmed/21288624
- Laryngeal Mask Airway. Published Dec. 2012. Accessed Dec. 2012 http://emedicine.medscape.com/article/82527-overview
- Brimacombe JR. The advantages of the LMA over the tracheal tube or facemask: a meta-analysis. Can J Anaesth. 1995;42(11):1017–1023. http://www.ncbi.nlm.nih.gov/pubmed/8590490
- Pediatric Anesthesia. Accessed Dec. 2012. http://openanesthesia.org/index.php?title=Pediatric_Anesthesia
- Combitube – Airway Device Difficult Airway Tutorial. Created Feb. 2007. Accessed Dec. 2012. http://vam.anest.ufl.edu/airwaydevice/combitube/index.html
- Emergency Airway Management: Other Supraglottic devices. Accessed Dec 2012.
- http://www.airwaycam.com/other-devices.html
- Russi CS, Wilcox CL, House HR. The laryngeal tube device: a simple and timely adjunct to airway management. Am J Emerg Med. 2007;25(3):263–267. http://ems.pgpic.com/pdf/kingairway_airway_management_independent.pdf
- Brain AI, Verghese C, Addy EV, Kapila A. The intubating laryngeal mask. I: Development of a new device for intubation of the trachea. British Journal of Anaesthesia. 1997;79(6):699–703. http://bja.oxfordjournals.org/content/79/6/699.full.pdf
- Baskett PJ, Parr MJ, Nolan JP. The intubating laryngeal mask. Results of a multicentre trial with experience of 500 cases. Anaesthesia. 1998;53(12):1174–1179. http://onlinelibrary.wiley.com/doi/10.1046/j.1365-2044.1998.00614.x/abstract
- Emergency Airway Management: Laryngeal Masks Accessed Dec. 2012 http://www.airwaycam.com/Supraglottic-airways.html
- Ruetzler K, Gruber C, Nabecker S, et al. Hands-off time during insertion of six airway devices during cardiopulmonary resuscitation: a randomised manikin trial. Resuscitation. 2011;82(8):1060–1063. http://www.resuscitationjournal.com/article/S0300-9572(11)00221-8/abstract
- Gausche M, Lewis RJ, Stratton SJ, et al. Effect of out-of-hospital pediatric endotracheal intubation on survival and neurological outcome: a controlled clinical trial. JAMA. 2000;283(6):783–790. http://jama.jamanetwork.com/article.aspx?articleid=192366
- Highlights of the 2010 American Heart Association Guidelines for CPR and ECC. Accessed Dec. 2012. http://www.heart.org/idc/groups/heart-public/@wcm/@ecc/documents/downloadable/ucm_317350.pdf
- Tanabe S, Ogawa T, Akahane M, et al. Comparison of Neurological Outcome between Tracheal Intubation and Supraglottic Airway Device Insertion of Out-of-hospital Cardiac Arrest Patients: A Nationwide, Population-based, Observational Study. J Emerg Med. 2012:1–9.
- Hasegawa K, Hiraide A, Chang Y, Brown DFM. Association of prehospital advanced airway management with neurologic outcome and survival in patients with out-of-hospital cardiac arrest. JAMA. 2013;309(3):257–266. doi:10.1001/jama.2012.187612.






5 thoughts on “Supraglottic Airway Review”
Nice review! I’m not sure why, maybe someone can comment on it, but I’ve seen a lot of Combitubes placed in the last few months by EMS in the field. Because of it I’ve had to learn more about them. There’s actually a ton of literature about these compared to other devices and this is probably b/c they’ve been around since the late 80s, like you mention. Some of the things I’ve learned are:
1) Combitubes are realllllly meant for esophageal placement BUT if you do get a tracheal intubation then thats fine–it will function okay that way, but it’s pretty rare to place it in the trachea.
2) If you do intubate the trachea, a bougie at some point should become your best friend. You can pass a bougie through, deflate BOTH balloons before removing Combitube, and then pass an ETT over bougie. I’ve only done this once…and it worked relatively smoothly.
3) The sizing is not weight or age based, its actually height based. You use the smaller size for smaller persons (4ft to 5.5ft) and larger size for anyone taller.
4) These are large and those big balloons can cause pressure necrosis so the Combitube eventually needs to be changed out.
Glad you like the review. I touched on a little more of the combitube use in this paper https://dl.dropboxusercontent.com/u/12858/History%20of%20Supraglottic%20airways.pdf
Hopefully your EMS agency is just using them due to stocking issues and aren’t moving away from the LT. LT has speed, sizing, and easy of use advantages over the combitube. Only argument for a combitube is it may be a little more secure because of the dual balloons but no one has shown a clinical outcome and that was only demonstrated in a cadaver
Nice review! I’m not sure why, maybe someone can comment on it, but I’ve seen a lot of Combitubes placed in the last few months by EMS in the field. Because of it I’ve had to learn more about them. There’s actually a ton of literature about these compared to other devices and this is probably b/c they’ve been around since the late 80s, like you mention. Some of the things I’ve learned are:
1) Combitubes are realllllly meant for esophageal placement BUT if you do get a tracheal intubation then thats fine–it will function okay that way, but it’s pretty rare to place it in the trachea.
2) If you do intubate the trachea, a bougie at some point should become your best friend. You can pass a bougie through, deflate BOTH balloons before removing Combitube, and then pass an ETT over bougie. I’ve only done this once…and it worked relatively smoothly.
3) The sizing is not weight or age based, its actually height based. You use the smaller size for smaller persons (4ft to 5.5ft) and larger size for anyone taller.
4) These are large and those big balloons can cause pressure necrosis so the Combitube eventually needs to be changed out.
Pingback: ERcast 08 – Máscara Laríngea, o início… – Emergência Rules