Authors: Elise Alves Graber, MD (Pediatric Emergency Medicine Fellow, Atrium Health’s Carolinas Medical Center), Christine Murphy, MD (Emergency Medicine Attending, Medical Toxicologist, Atrium Health’s Carolinas Medical Center) // Reviewed by: Cynthia Santos, MD (@Cynthia Santos, MD); Alex Koyfman, MD (@EMHighAK); and Brit Long, MD (@long_brit)

Case presentation:
A 3-year-old male is brought into the emergency department by EMS after being found unconscious in a house fire. EMS states that firefighters on scene believe the fire started when a cigarette fell on a sofa covered in plastic. The patient is now awake and crying and is noted to have significant amount of soot covering his entire body. Initial labs reveal a lactate of 12 mmol/L.
Question:
What are the available treatments for cyanide toxicity, and how do I know which one(s) to use?
Background:
Cyanide is a very potent toxin that can cause life-threatening symptoms in small doses. Exposure to cyanide can happen in a variety of settings such as with smoke inhalation, laboratory/industrial accidents, suicide or homicide attempts, and accidental ingestion.1
Sources of cyanide can include:1
- Cyanide salts
- Hydrogen cyanide
- Organic compounds like acetonitrile
- Pharmaceuticals like nitroprusside
- Cyanogenic glycosides found in fruits with pits containing amygdalin (apricots, cherries, peaches) or improperly prepared cassava
Pearls:
- Toxicity is mainly due to cyanide’s inhibition of cytochrome oxidase in the electron transport chain which halts ATP production leading to acidosis and anaerobic metabolism despite an often oxygen rich environment.1

Electron transport chain. Image from LibreTexts. Accessed 4/14/2020. (Reference)
- With acute toxicity there is no reliable pathognomonic toxidrome or characteristic symptoms.
- Symptoms include:1
- CNS: headache, anxiety, agitation, confusion, lethargy, nonreactive dilated pupils, seizures, coma, centrally mediated tachypnea initially, with progression to bradypnea and apnea
- CV: Initial tachycardia and hypertension followed by bradycardia and hypotension
- Ventricular dysrhythmias have been reported
- Pulmonary: pulmonary edema, corrosive injury to the respiratory tract
- GI (mostly due to ingestion): nausea, vomiting, hemorrhagic gastritis causing abdominal pain
- Cutaneous: cherry-red skin
- Laboratory findings reflect altered mitochondrial function and include anion gap metabolic acidosis and an elevated lactate.
- Lactate > 8 mmol/L is 94% sensitive for cyanide toxicity2
- Blood cyanide concentrations may confirm exposure, but usually do not result in time to be clinically significant
- Treatment should include supportive care, decontamination of skin, NG/OG aspiration, consideration of activated charcoal if patient has intact or protected airway and giving one or more cyanide antidotes.1
- Ventricular dysrhythmias have been reported
How do I know which antidote to give?
There are several available treatments for cyanide toxicity, it is important to be familiar with what is available at your institution, as often that will dictate how you treat your patient. There are pros and cons to using each of the antidotes, and if you have all options available to you, your patient’s clinical picture will dictate which of the antidotes you should start with. Many providers prefer hydroxocobalamin due to the simplicity of delivery, however due to cost some hospitals do not routinely stock this medication or have a very limited supply.
-
Amyl Nitrite
- Highly volatile and readily absorbed from the lungs, amyl nitrite pearls are crushed and placed under the nose of cyanide toxic patient for inhalation
- Apply over nose and mouth for 30-60 seconds every 30-60 seconds for about 5 minutes4
- While effective, amyl nitrite pearls are no longer used due to:
- Short half life
- Risk for underdosing and excessive dosing
- Generation of unpredictable levels of methemoglobinemia
- Inadvertent provider exposure
- Highly volatile and readily absorbed from the lungs, amyl nitrite pearls are crushed and placed under the nose of cyanide toxic patient for inhalation
-
Sodium Thiosulfate1,5
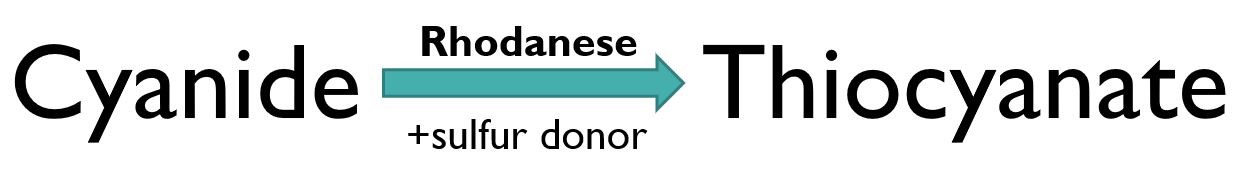
- The major intrinsic route of cyanide detoxification occurs via enzymatic conversion by rhodanese and a sulfur donor to thiocyanate, which is a harmless compound eliminated in the urine
-
- Sodium thiosulfate donates sulfur atoms for rhodanese to catalyze formation of thiocyanate
- Hyperosmolar compound resulting in significant sodium load to patient
- Adult dose: 50 mL (12.5 g) IV over 10 to 30 min6
- Pediatric dose: 1-1.65 mL/kg up to 50 mL IV6
- Adverse effects include: nausea, vomiting, prolonged bleeding time, hypotension
- Sodium thiosulfate donates sulfur atoms for rhodanese to catalyze formation of thiocyanate
-
Sodium Nitrite1,5
- Initiates methemoglobin formation
- Cyanide has a higher affinity for the ferric iron in methemoglobin than for cytochrome oxidase
- Administered over 2–4 minutes
- Adult dose: 10 mL (300 mg) IV7
- Pediatric dose: 0.2 mL/kg (6 mg/kg) up to 10 mL (300 mg) IV7
- Dosing adjustments can be made to pediatric dosing for significant anemia; the pediatric dosing, as listed above, is safe for a hemoglobin of 7 g/dL8
- Adverse effects: excessive methemoglobinemia, potent vasodilation leading to transient hypotension and tachycardia
- Initiates methemoglobin formation
-
Hydroxocobalamin1,9
- Trade names: Cyanokit, Hydro Cobex, Hydroxy Cobal
- A metalloprotein with a central cobalt atom that complexes cyanide forming cyanocobalamin
-
- Adult dosing: 5 g IV over 15 minutes
- Pediatric dosing: 70 mg/kg up to 5 g IV
- Adverse effects: allergic reaction, transient red discoloration of the skin/mucus membranes/urine/secretions, moderate elevation in blood pressure, renal injury
- Elevations in blood pressure may be a beneficial side effect if the patient is hypotensive
- Red discoloration can last from several days to 1-2 weeks and causes interference with laboratory studies and hemodialysis10,11
- There are several reports of acute renal injury related to hydroxocobalamin use and renal function should be monitored closely for 7 days after receiving this medication12
- A recent retrospective study of smoke inhalation victims identified AKI was associated with patients receiving hydroxocobalamin. Further investigation of this is warranted.13
Comparing the Antidotes
- Most research uses swine models of acute cyanide toxicity
- Key studies:
- Evaluation of IV hydroxocobalamin plus IV sodium thiosulfate vs IV sodium nitrite plus IV sodium thiosulfate14
- Faster return to baseline MAP in hydroxocobalamin plus sodium thiosulfate group
- No difference in mortality, serum acidosis, or serum lactate
- Evaluation of IV hydroxocobalamin vs IV sodium thiosulfate vs IV hydroxocobalamin plus IV sodium thiosulfate15
- Sodium thiosulfate alone failed to reverse cyanide-induced shock in a swine model of severe cyanide toxicity and resulted in 100% mortality
- In this model, hydroxocobalamin alone was effective in reversing cyanide induced shock in the setting of severe cyanide toxicity
- The addition of sodium thiosulfate to hydroxocobalamin did not improve mortality, hemodynamics, or biochemical markers
- To our knowledge there are no studies published to date evaluating the efficacy of IV hydroxocobalamin vs IV sodium nitrite plus IV sodium thiosulfate
- Evaluation of IV hydroxocobalamin plus IV sodium thiosulfate vs IV sodium nitrite plus IV sodium thiosulfate14

Cyanide Antidote Kit. Image used with permission. Credit: Russ Kerns, MD, Emergency Medicine Attending and Medical Toxicologist, Atrium Health’s Carolinas Medical Center.
Using the antidotes in combination
Given that sodium nitrite, sodium thiosulfate and hydroxocobalamin all work to reverse cyanide toxicity via different mechanisms, it is possible to use them in combination.
- Sodium nitrite and sodium thiosulfate are typically given together as they have synergistic action against cyanide3
- These drugs can be found as individual components or together in a kit
- The traditional Cyanide Antidote Kit contained amyl nitrite, sodium nitrite, and sodium thiosulfate1
- The current version of this, the Nithiodote kit, contains sodium nitrite and sodium thiosulfate.
- Hydroxocobalamin can be used independently, in conjunction with sodium thiosulfate alone, or with both sodium thiosulfate and sodium nitrite.
- Some providers will also recommend giving sodium thiosulfate initially for stable patients while awaiting lactate results to determine need for additional antidotal therapy (i.e. hydroxocobalamin or sodium nitrite).
Main Points
- Empiric treatment with a cyanide antidote in a fire victim should be considered, especially when there was a history of loss of consciousness or the patient has significant acidosis.
- Antidote availability will, in a large part, dictate what you use
- Options for treatment include:
- Hydroxocobalamin
- Hydroxocobalamin + sodium thiosulfate
- Sodium nitrite + sodium thiosulfate
- Exercise caution when using sodium nitrite in patients who are already hypotensive
- Don’t use hydroxocobalamin and sodium thiosulfate together in the same line
References
- Holstege CP, Kirk MA. Cyanide and Hydrogen Sulfide. In: Nelson LS, Howland M, Lewin NA, Smith SW, Goldfrank LR, Hoffman RS. Eds (2019). Goldfrank’s Toxicologic Emergencies. 11the New York: McGraw-Hill. http://accesspharmacy.mhmedical.com.libproxy.lib.unc.edu/content.aspx?bookid=2569§ionid=210264536. Accessed April 27, 2020.
- Baud, F. J., et al. Value of lactic acidosis in the assessment of the severity of acute cyanide poisoning. Critical Care Medicine. 2002;30(9):2044–2050. doi: 10.1097/00003246-200209000-00015.
- Howland MA. Nitrites (Amyl and Sodium) and Sodium Thiosulfate. In: Nelson LS, Howland M, Lewin NA, Smith SW, Goldfrank LR, Hoffman RS. Eds (2019). Goldfrank’s Toxicologic Emergencies. 11the New York: McGraw-Hill. http://accesspharmacy.mhmedical.com.libproxy.lib.unc.edu/content.aspx?bookid=2569§ionid=210264055. Accessed April 27, 2020.
- Chen KK, Rose CL.Nitrite and thiosulfate therapy in cyanide poisoning. J Am Med Assoc. 1952;149:113-119.
- Marrs TC. Antidotal treatment of acute cyanide poisoning. Adv Drug React Acute Poisoning Rev. 1988;4:179-206.
- Sodium thiosulfate [package insert] Manufactured by Cangene BioPharma, Inc, Baltimore, MD, for Hope Pharmaceuticals, Scottsdale, AZ; 2012. https://www.accessdata.fda.gov/drugsatfda_docs/label/2012/203923s000lbl.pdf Accessed 4/26/2020
- Sodium Nitrite [package insert]. Manufactured by Cangene BioPharma, Inc, Baltimore, MD, for Hope Pharmaceuticals, Scottsdale, AZ; 2011. https://www.accessdata.fda.gov/drugsatfda_docs/label/2012/203922s000lbl.pdf Accessed 4/26/2020.
- Berlin CM. The treatment of cyanide poisoning in children. Pediatrics. 1970;46(5);793-796.
- Howland MA. Hydroxocobalamin. In: Nelson LS, Howland M, Lewin NA, Smith SW, Goldfrank LR, Hoffman RS. Eds (2019). Goldfrank’s Toxicologic Emergencies. 11the New York: McGraw-Hill. http://accesspharmacy.mhmedical.com.libproxy.lib.unc.edu/content.aspx?bookid=2569§ionid=210264007. Accessed April 27, 2020.
- Carlsson CJ, Hansen HE, Hilsted L, Malm J, Odum L, Szecsi PB. An evaluation of the interference of hydroxocobalamin with chemistry and co-oximetry tests on nine commonly used instruments. Scand J Clin Lab Invest. 2011;71(5):378-386.
- Lim K, Heher E, Steele D, et al. Hemodialysis failure secondary to hydroxocobalamin exposure. Proc (Bayl Univ Med Center). 2017;30(2):167-168.
- Hydroxocobalamin [package insert]. Manufactured by McKesson. a.s., Semoy, France and distributed by Meridian Medical Technologies, Inc, Columbia, MD; March 2017. https://www.accessdata.fda.gov/drugsatfda_docs/label/2018/022041s019,%20020lbl.pdf Accessed 5/4/2020
- Dépret, F., Hoffmann, et al. Association between hydroxocobalamin administration and acute kidney injury after smoke inhalation: a multicenter retrospective study. Critical Care. 2019;23(1). doi: 10.1186/s13054-019-2706-0
- Bebarta, V., Tanen, D.A., Lairet, J. et al. Hydroxocobalamin and sodium thiosulfate versus sodium nitrite and sodium thiosulfate in the treatment of acute cyanide toxicity in a swine (sus scrofa) model. Ann Emerg Med. 2010; 55(4): 345–351
- Bebarta, V. S., Pitotti, R. L., Dixon, P., Lairet, J. R., Bush, A., & Tanen, D. A. Hydroxocobalamin versus sodium thiosulfate for the treatment of acute cyanide toxicity in a swine (sus scrofa) model. Annals of Emergency Medicine. 2012;59(6): 532–539. doi: 10.1016/j.annemergmed.2012.01.022






2 thoughts on “ToxCard: Cyanide Toxicity and Treatment”
Pingback: Quiz 68, May 22th, 2020
Pingback: Cyanide Poisoning in Children — Pediatric EM Morsels