Authors: Claire Milam, MD (Emergency Medicine Resident, Carolinas Medical Center), Ann-Jeannette Geib, MD (Associate Professor of Emergency Medicine, Carolinas Medical Center) // Reviewed by: Cynthia Santos, MD (@Cynthia Santos, MD); Alex Koyfman, MD (@EMHighAK); and Brit Long, MD (@long_brit)

Case Presentation:
A 32-year-old female presents to the ED via EMS with seizure activity for about 10 minutes. EMS has given her 10mg of intramuscular (IM) midazolam without termination of seizure activity, and further doses of intravenous (IV) midazolam in the ED are unsuccessful. A family member arrives and tells you that she is currently undergoing treatment for tuberculosis (TB) exposure with isoniazid (INH), but she is otherwise healthy.
Question:
What is your next step in treatment? What is the dose and route of administration?
Pearls:
Pyridoxine (Vitamin B6) with initial dose of 5g IV.
-
- These are likely seizures caused by acute (INH) toxicity.
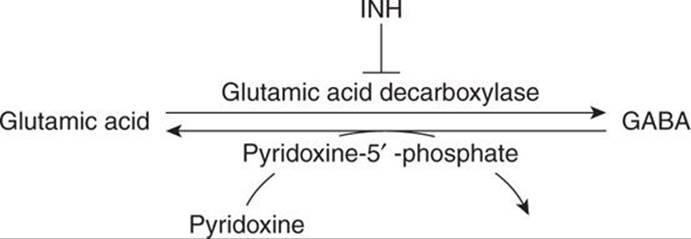
- INH toxicity causes a functional pyridoxine deficiency by inhibiting conversion of pyridoxine to its active metabolite pyridoxal 5’ phosphate (PLP), and it causes a quantitative deficiency by increasing renal excretion of pyridoxine and its metabolites. INH also inhibits glutamic acid decarboxylase (GAD), the enzyme that converts the stimulatory neurotransmitter glutamate to the inhibitory neurotransmitter GABA [1].
- Pyridoxine’s active metabolite PLP is a cofactor for the enzyme that converts glutamate (an excitatory neurotransmitter) to GABA (an inhibitory neurotransmitter).
- Pyridoxine/PLP deficiency causes seizures due to low levels of GABA and higher levels of glutamate. Giving pyridoxine will therefore work to restore GABA tone.
- Pyridoxine and benzodiazepines work synergistically as benzodiazepines rely on GABA to work, and giving pyridoxine is working to help synthesize GABA [1,2,3].
-
- The classic triad of toxicity is refractory seizures, coma, and metabolic acidosis with elevated lactate.
-
- Other early signs of acute toxicity include vomiting, dizziness, tachycardia, and slurred speech.
- Activated charcoal should be considered early on for GI decontamination, but remember these patients may require intubation and may not be protecting their airway. Hemodialysis is usually not needed given the short half-life, but could be considered to correct severe acidosis.
- The regular dose of INH for TB is 5 mg/kg/dose, usually 300 mg. Seizures usually occur with acute ingestion at concentrations greater than 20 mg/kg (1.5 g in a 70 kg adult) with inevitable seizure activity at greater than 35-40 mg/kg [1].
- Empiric dosing of pyridoxine when a known amount of INH is ingested is an equal amount of grams of IV pyridoxine. (For example: 1 g INH = 1 g pyridoxine)[1,3].
- Dosing of pyridoxine when an unknown amount of INH is ingested is 5 g IV and 70 mg/kg IV in pediatrics, repeated every 5-20 minutes [3].
- Asymptomatic patients with potentially toxic overdoses should still receive IV pyridoxine, especially within 2 hours of ingestion, which is when it reaches peak concentration [1,3].
- 5 g of pyridoxine is a large dose. The US recommended daily allowance of pyridoxine for adults ranges from about 1.3 mg-2 mg [4], and patients taking INH are usually given supplemental pyridoxine dosed at 50 mg per day to help prevent the chronic neurotoxic effects of pyridoxine, which is usually neuropathy[5]. Higher doses of pyridoxine (greater than 1 g per day) have also been shown to be neurotoxic causing severe neuropathy [6].
- If your hospital does not have large doses of IV pyridoxine, consider crushing tablets and placing an NG or OG tube for enteric pyridoxine at the same dose. Then, consider transferring to a higher level of care.
Main Point:
INH toxicity causes a pyridoxine deficient state in the brain, which decreases the concentration of the inhibitory neurotransmitter, GABA, and causes seizures. In seizures that are refractory to our usual treatment with benzodiazepines and first line anti-epileptics like levetiracetam and fosphenytoin, consider pyridoxine (B6) deficiency and treat with 5 g of IV pyridoxine (or 70 mg/kg in pediatrics). In patients with a known ingestion, treat 1 g of pyridoxine for every 1 g of INH. Consider crushing tablets of pyridoxine to give through enteral access or transfer your patient if your hospital does not have enough IV pyridoxine.
References:
- Hernon, Christina H., and Jeffrey T. Lai.. “Antituberculous Medications.” Goldfrank’s Toxicologic Emergencies, 11e Eds. Lewis S. Nelson, et al. New York, NY: McGraw-Hill, http://accesspharmacy.mhmedical.com.libproxy.lib.unc.edu/content.aspx?bookid=2569§ionid=210273291.
- Aronson, J. K. “Isoniazid.” Meyler’s Side Effects of Drugs, 16e, Elsevier, 2016, https://www-clinicalkey-com.ahecproxy.ncahec.net/#!/content/book/3-s2.0-B9780444537171009252?scrollTo=#hl0000026.
- Mofenson, Howard C., et al. “Medical Toxicology.” Conn’s Current Therapy 2020. Elsevier, 2020, https://www-clinicalkey-com.ahecproxy.ncahec.net/#!/content/book/3-s2.0-B9780323711845003177?scrollTo=#top.
- “Vitamin B6; Fact Sheet for Health Care Professionals.” Health Information, National Institute of Health; Office of Dietary Supplements , 19 Sept. 2019, https://ods.od.nih.gov/factsheets/VitaminB6-HealthProfessional/.
- Katirji, Bashar. “Disorders of Peripheral Nerves.” Bradley’s Neurology in Clinical Practice. 7th ed., Elsevier, 2016, https://www-clinicalkey-com.ahecproxy.ncahec.net/#!/content/book/3-s2.0-B9780323287838001071?scrollTo=%23hl0004305
- So, Yuen T. “Deficiency Diseases of the Nervous System.” Bradley’s Neurology in Clinical Practice. 7th ed., Elsevier, 2016, https://www-clinicalkey-com.ahecproxy.ncahec.net/#!/content/book/3-s2.0-B9780323287838000855?scrollTo=#top.





