Author: Pablo Zertuche, MD (Internal Medicine / Pediatrics Resident, Rutgers NJMS) // Reviewed by: Cynthia Santos, MD (@CynthiaSantosMD, Assistant Professor, Emergency Medicine, Medical Toxicology, Rutgers NJMS); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Case:
A 19-year-old male with history of mild intermittent asthma, ADHD, and anxiety (not on medication) presents with worsening difficulty breathing for the past 2 day. He started with fever, congestion, and non-productive cough 3 days prior to admission with a Tmax of 102F at home. He saw his primary care physician 2 days ago and was prescribed azithromycin. His symptoms worsened, he developed intermittent nausea and emesis, and his mom noticed that the patient was turning blue, which prompted today’s ED visit.
The patient “vapes” intermittently. He recently bought re-filled cartridges off the street with “THC containing juice”.
On exam the patient is in acute respiratory distress, with peripheral cyanosis and tachypnea to 50-60 RPM. Temp 98.7, HR 118, BP WNL. Crackles on right subscapular region are noted, as well as subcostal retractions. He also has intermittent cough with blood-tinged sputum and an O2 saturation 89% on 12L non-rebreather.
While in the ED, he goes into acute hypoxic respiratory failure, is intubated, and is transferred to the ICU.
CT chest showing bilateral diffuse ground glass opacities.
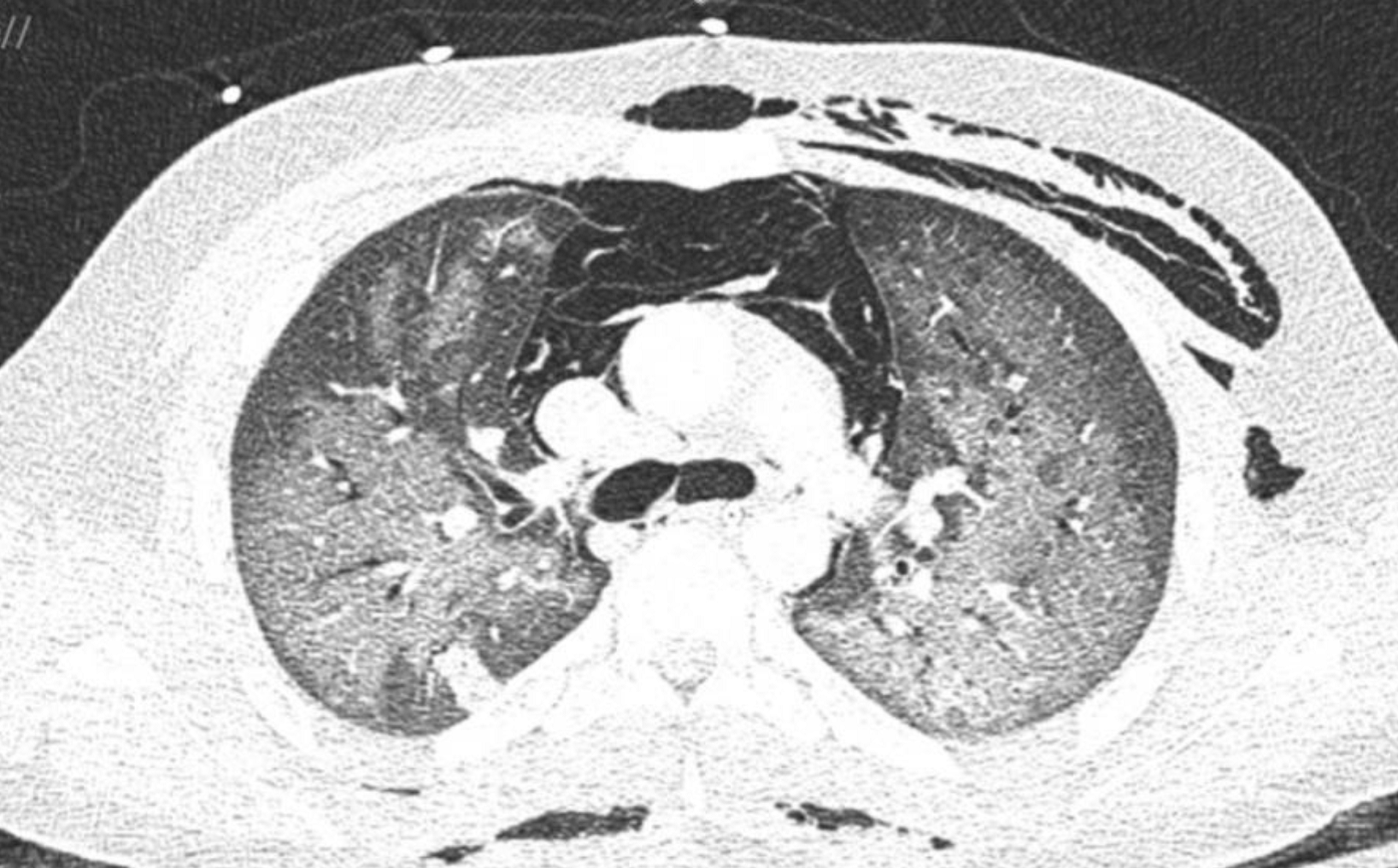
Questions:
- What work up should you order?
- What is the most likely diagnosis?
- Should you report the case?
Background:
Several environmental agents can cause acute or subacute inhalation injury. Toxic inhalation pneumonitis is a group of injuries to the lung parenchyma and upper respiratory tract secondary to chemicals. The clinical presentation depends on the characteristics of the toxic compound inhaled (type and amount) and symptoms can range from minor respiratory discomfort to acute respiratory injury and failure.1
Electronic cigarettes or e-cigarettes are battery-powered devices that allow the inhalation of aerosolized substances which tend to contain fewer toxic chemicals than conventional cigarette smoke. They are used to inhale nicotine but also tetrahydrocannabinol (THC), cannabidiol (CBD) and butane hash oils (dabs). Published cases have linked e-cigarette use with pulmonary illnesses, however, there had been no large clusters identified until the recent 2019 outbreak which has reached epidemic proportions and has several departments of health investigating reported cases in multiple states and the CDC coordinating public health response.2
No culprit has been yet identified; however, electronic cigarette fluids have been shown to contain at least six groups of potentially toxic compounds (nicotine, carbonyls, volatile organic compounds (such as benzene and toluene), particles, and trace metal elements. The effects of adding THC or CBD to the liquid mix still needs to be investigated.1
Case definition of Vaping Associated Pulmonary Injury by the CDC:3
- Respiratory symptoms: cough, dyspnea, fatigue
- Symptoms worsened over days to weeks prior to admission
- Other symptoms: fever, chest pain, weight loss, nausea, diarrhea
- Chest radiograph with bilateral opacities
- CT with diffuse ground-glass opacities with often sub-pleural sparing
- Negative infectious work up
- Some with progressive respiratory failure requiring mechanical ventilation, improved with corticosteroids
- All patients reported vaping weeks to month prior to presentation
- Many with recent use of THC containing products (no specific product)
Outbreak:4
The surge in cases represent a public health threat given the increasing popularity and prevalent use of electronic cigarettes.
The recent outbreak in numbers:
- Started with 8 suspected cases on July 25, 2019 in Wisconsin.
- By August 28, 2019, there were 119 confirmed and suspected cases in 16 states.
- By September 6, 2019, the number had risen to 288 in 39 states.
- By September 20, 2019, there were 908 cases across 45 states and the US Virgin Islands (495 cases confirmed and 413 suspected).
- Total of 8 deaths by September 20, 2019.
- The breakout has now reached epidemic proportions, and further surveillance is necessary.


What we know:5
- Most patients report using e-cigarette products containing THC, many report using THC and nicotine, and some report using only products containing nicotine.
- All reported cases include history of using e-cigarette products or vaping.
- In a recent MMWR report, interviews about e-cigarette use were completed with 86 patients in Illinois and Wisconsin. Use of THC-containing e-cigarette products, the majority of which were prefilled cartridges obtained from informal sources, was reported by 87% of patients during the 3 months preceding illness.8
- The CDC has released interim recommendations for healthcare providers, health departments and the public.
Case definition by CDC:6


Recommendations by CDC for patients:5
- If you are concerned about specific health risks, refrain from using e-cigarettes and vaping products, especially those containing THC.
- If you are using these products to quit smoking, do not go back to cigarettes.
- If you have any symptoms like the ones reported and you have recently used these products, see a healthcare provider.
- Do not buy products off the street, do not modify or add substances to them
- Youth and young adults should not use e-cigarettes.
- Pregnant women should not use e-cigarettes.
- Adults who do not currently use tobacco products should not start using e-cigarettes.
Recommendations by CDC for physicians:7
- Consider e-cigarette-associated pulmonary disease as one possible etiology in the differential of pulmonary disease and history of e-cigarette use.
- Evaluate and treat for other possible causes of illness (infectious, rheumatologic, neoplastic, other) as clinically indicated.
- Report possible cases to local or state health department for further investigation and guidance as needed.
- If e-cigarette product use is suspected as a cause of pulmonary injury, get detailed history of substances used, the sources and devices used.
- Determine if any remaining product, devices or liquids are available for testing.
- State public health officials should promptly notify CDC about possible cases and refer to CDC for most recent version of surveillance case definitions, reporting guidelines and case investigation forms.
What are the implications for public health practice?8
“The cause of this outbreak is unknown but might be related to prefilled THC cartridges. While this investigation is ongoing, CDC recommends that persons consider refraining from using e-cigarette, or vaping, products, particularly those containing THC. Additional information from product testing and traceback could help determine the source of the outbreak and prevent future illnesses.”
References/Further Reading:
- Christiani DC. Vaping-Induced Lung Injury. New England Journal of Medicine. 2019;0(0):null. doi:10.1056/NEJMe1912032
- Layden JE, Ghinai I, Pray I, et al. Pulmonary Illness Related to E-Cigarette Use in Illinois and Wisconsin — Preliminary Report. New England Journal of Medicine. 2019;0(0):null. doi:10.1056/NEJMoa1911614
- CDC Clinical Outreach and Communication Activity. https://emergency.cdc.gov/newsletters/coca/081619.htm. Accessed September 21, 2019.
- Hswen Y, Brownstein JS. Real-Time Digital Surveillance of Vaping-Induced Pulmonary Disease. New England Journal of Medicine. 2019;0(0):null. doi:10.1056/NEJMc1912818
- Health CO on S and. Smoking and Tobacco Use; Electronic Cigarettes. Centers for Disease Control and Prevention. https://www.cdc.gov/tobacco/basic_information/e-cigarettes/severe-lung-disease.html. Published September 19, 2019. Accessed September 20, 2019.
- For State and Local Health Departments. Centers for Disease Control and Prevention. https://www.cdc.gov/tobacco/basic_information/e-cigarettes/severe-lung-disease/health-departments/index.html. Published September 19, 2019. Accessed September 20, 2019.
- Severe Pulmonary Disease Associated with Electronic-Cigarette–Product Use — Interim Guidance, Centers for Disease Control and Prevention, MMWR. https://www.cdc.gov/mmwr/volumes/68/wr/mm6836e2.htm?s_cid=mm6836e2_w. Accessed September 21, 2019.
- Ghinai I, Pray IW, Navon L, O’Laughlin K, et al. E-cigarette Product Use, or Vaping, Among Persons with Associated Lung Injury — Illinois and Wisconsin, April–September 2019. Centers for Disease Control and Prevention, MMWR. https://www.cdc.gov/mmwr/volumes/68/wr/mm6839e2.htm?s_cid=mm6839e2_w. Accessed September 28, 2019.







1 thought on “TOXCard: Vaping Associated Pulmonary Injury, 2019 outbreak”
Pingback: REBEL Core Cast 23.0 - Vaping Associated Pulmonary Injury - REBEL EM - Emergency Medicine Blog