Ultrasound-Guided Femoral Nerve Block
by Robert J. Strony DO, RDMS, RVT
(Program Director of Geisinger Emergency Medicine; Geisinger Health System POC US Director)
Grant Garbo MD
(EM Resident Physician at Geisinger Emergency Medicine Residency)
Edited by Alex Koyfman MD (@EMHighAK) and Stephen Alerhand MD (@SAlerhand)
Patient Case
A 72 year-old female with a past medical history of hypertension is brought in by EMS at 6 AM after a fall. The fall was witnessed by family and occurred after tripping over the dog. The patient did not hit her head, but is complaining of a left-sided hip pain. She appears to be in moderate to severe distress from the pain.
On examination, the left leg is shortened and slightly externally rotated. Fortunately, the extremity is neurovascularly intact. The patient is able to move her toes and ankle, but has severely limited range of motion of the entire leg secondary to severe pain.
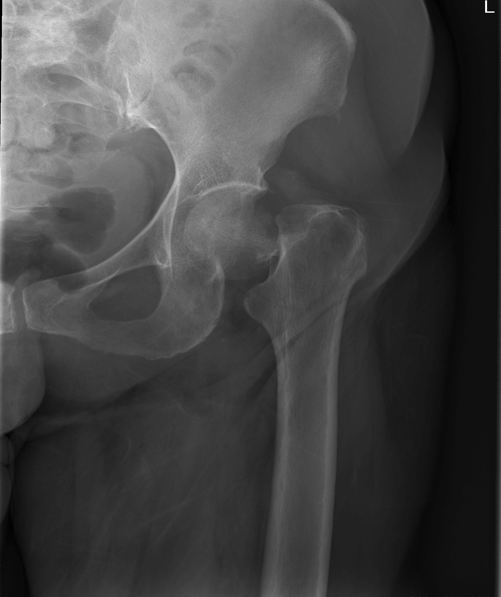
Being a caring physician and realizing that the pain must be unbearable, the resident gives the patient a weight-based dose of morphine and obtains a film of the hip. The x-ray demonstrates a left femoral neck hip fracture depicted in Figure A.
Figure A: Femoral neck fracture.
The resident goes to check on the patient and relays the unfortunate news that she has suffered a hip fracture. The patient continues to complain of significant pain in the hip and asks if there is anything else the physician can do to alleviate her pain. The morphine did very little to diminish her pain and made her very nauseated. Lucky for this patient, the physician is well versed in the art of Clinical Emergency Ultrasound!
Ultrasound Application
Reaching for their ultrasound machine and remembering the anatomy with the helpful pneumonic NAVEL (nerve, artery, vein, empty, lymphatics – from lateral to medial) the resident realizes that an ultrasound-guided femoral nerve block is just what the doctor ordered. The anatomy the physician identifies is pictured in Figure B (unlabeled) and Figure C (labeled). If done successfully, it could significantly decrease the patient’s pain score and eliminate the need for further parenteral opioid administration in this frail and elderly patient. Before proceeding, the physician ensures that the literature supports this ultrasound-guided emergency procedure.
Figure B: Unlabeled Ultrasound Depiction of the Femoral Nerve, Superficial Femoral Artery, Deep Femoral Artery, Femoral Vein and Fascia Lata. Lateral is depicted by the indicator mark P in the upper left corner of the image.
Figure C: Labeled Ultrasound Depiction of the Femoral Nerve (FN), Superficial Femoral Artery (SFA), Deep Femoral Artery (DFA), Femoral Vein (FV) and Fascia Lata. Lateral is depicted by the indicator mark P in the upper left corner of the image.
The Literature Review
Citation: Beaudoin FL, Nagdev A, Merchant RC, Becker BM. Ultrasound-guided femoral nerve blocks in elderly patients with hip fractures. Am J Emerg Med. 2010 Jan;28(1):76-81.
Type of Study: Prospective observational study (n=13)
Objective: Determine the effectiveness of ultrasound guided femoral nerve block as an adjunct for pain control in the emergency department.
Results: Decrease in pain scores of 44% and 67% at 15 minutes (p<0.002) and 30 minutes (p<0.001) post procedure respectively.
Conclusion: Ultrasound guided femoral nerve blocks result in significant and sustained decreases in pain scores in elderly patients with a hip fracture.
Citation: Haines L, Dickman E, Ayvazyan S, Pearl M, Wu S, Rosenblum D, Likourezos A. Ultrasound-guided fascia iliaca compartment block for hip fractures in the emergency department. J Emerg Med. 2012 Oct;43(4):692-7.
Type of Study: Prospective observational study (n=20)
Objective: Does ultrasound-guided fascia iliaca compartment block provide an adjunct or alterative to intravenous morphine in emergency department patients with a hip fracture.
Results: All patients reported a 76% decrease in pain score at 120 minutes as well as all other time points (p=0.0001).
Conclusion: Ultrasound-guided fascia iliaca compartment block provided excellent analgesia without complications.
Citation: Beaudoin FL, Haran JP, Liebmann O. A comparison of ultrasound-guided three-in-one femoral nerve block versus parenteral opioids alone for analgesia in emergency department patients with hip fractures: a randomized controlled trial. Acad Emerg Med. 2013 Jun;20(6):584-91.
Type of Study: Blinded, randomized controlled clinical trial (n=18 in each group)
Objective: Superiority design looking at whether patients who receive an US-guided femoral nerve block in addition to opioids have superior pain relief compared with patients who receive parenteral opioids alone.
Results: Numerical rating scale of pain showed a pain-intensity difference of 36.9% in the study group and 13.4% in the control group. (p<0.001) Additionally, the control group required significantly more rescue morphine post procedure with an average of 5.0 mg versus 0 mg. (p=0.028)
Conclusion: US guided femoral nerve blocks as an adjunct to morphine resulted in significantly reduced pain over 4 hours, decreased the amount of rescue analgesia, and showed no appreciable difference in adverse events when compared to morphine alone.
Citation: Turner AL, Stevenson MD, Cross KP. Impact of ultrasound-guided femoral nerve blocks in the pediatric emergency department. Pediatr Emerg Care. 2014 Apr;30(4):227-9.
Type of Study: Retrospective, preimplementation and postimplementation of US guided femoral block study (p=81)
Objective: Determine if use of US-guided femoral nerve block in the pediatric ED significantly altered the duration of analgesia and need for pain medications in patients with a femoral fracture.
Results: Next dose of analgesia was 2.2 hours in preimplementation and 6.1 hours in the postimplementation patients. There was a median total dose of morphine of 14.8 mcg/kg per hour versus 6.5 mcg/kg per hour respective.
Conclusion: Patients who underwent US-guided femoral nerve block had longer duration of analgesia, required fewer doses of analgesic medications, and needed fewer nursing interventions compared with those who used analgesia alone.
Citation: Oberndorfer U, Marhofer P, Bösenberg A, Willschke H, Felfernig M, Weintraud M, Kapral S, Kettner SC. Ultrasonographic guidance for sciatic and femoral nerve blocks in children. Br J Anaesth. 2007 Jun;98(6):797-801. Epub 2007 Apr 21
Type of Study: Randomized controlled trial (n=46)
Objective: Comparison of nerve stimulator guidance versus ultrasound guidance for lower extremity nerve blocks in children.
Results: Two failures of therapy in nerve stimulator guided blocks, no failures in the ultrasound guided blocks. Duration of block was longer with ultrasound guidance (508 vs 335 min). Volume of local anesthetic was reduced when using the ultrasound compared to the nerve stimulator (0.15 vs 0.3 ml/kg respectively)
Conclusion: Ultrasound guidance for sciatic and femoral nerve blocks resulted in increased duration as well as decreased volume of anesthetic.
Citation: Orebaugh SL, Kentor ML, Williams BA. Adverse outcomes associated with nerve stimulator-guided and ultrasound-guided peripheral nerve blocks by supervised trainees: update of a single-site database. Reg Anesth Pain Med. 2012 Nov-Dec;37(6):577-82.
Type of Study: Retrospective Review (n=9301)
Objective: Evaluate safety of ultrasound versus nerve stimulator in performing a peripheral nerve block.
Results: Four peripheral nerve injuries were documented. US guided technique was used in one case and nerve stimulator was used in the other three. One seizure associated with local anesthetic systemic toxicity occurred with the nerve stimulator.
Conclusion: Ultrasound is a safe method of obtaining a peripheral nerve block.
Citation: Barrington MJ, Watts SA, Gledhill SR, Thomas RD, Said SA, Snyder GL, Tay VS, Jamrozik K. Preliminary results of the Australasian Regional Anaesthesia Collaboration: a prospective audit of more than 7000 peripheral nerve and plexus blocks for neurologic and other complications. Reg Anesth Pain Med. 2009 Nov-Dec;34(6):534-41.
Type of Study: Prospective (n=7156 blocks)
Objective: Determine the rate of neurologic injury following peripheral nerve block
Results: 30 (0.5%) met criteria for a neurologic assessment based on symptom complaints. Of these 30 patients 3 of the patients were found to have an injury related to the nerve block. Eight patients (0.1%) experienced symptoms of local anesthetic toxicity.
Conclusion: Nerve block is a safe procedure with rare complications of neurologic injury and local anesthetic toxicity.
Performing the Ultrasound Guided Femoral Nerve Block
As the physician suspects, the literature demonstrates decreased pain scores, good efficacy, sustained effects, and minimal complications. The femoral nerve is derived from the second, third, and fourth lumbar nerve roots. After passing below the inguinal ligament the nerve bifurcates into anterior and posterior branches providing sensation to the anterior and lower medial portion of the thigh, femur, and knee. Articular nerves from the femoral nerve are responsible for sensation to the hip.
At the femoral crease, the nerve lies beneath the fascia lata and the fascia iliaca as depicted again in Figure B and C. The patient is placed into a supine position with slight abduction and slight Trendelenburg. The probe is placed along the femoral creases with the goal of locating the femoral artery. Following self-orientation, the probe is moved cephalad and caudad to further delineate the surrounding anatomy.
The nerve will appear as triangular in shape and should also be traced to confirm that it is not a lymph node. The nerve can be located above the bifurcation of the femoral artery (separating into the the superficial femoral artery and the deep femoral artery) or between the superficial femoral nerve and the deep femoral nerve as depicted in this case. Once the nerve location has been confirmed, the skin should be prepped. A local skin wheal can be made with a 27-gauge needle at the lateral aspect of the probe equidistant to the depth of the nerve. For instance if the nerve lies 2 cm deep, the anesthetic and needle entry should be 2 cm lateral to the probe indicator.
As depicted in the video file Figure D below, an 18-gauge needle can then be used to puncture the skin followed by the insertion of a 22-guage Whitacre noncutting spinal needle into the puncture site. The Whitacre needle reduces the risk of neurologic and vascular injury. This should be inserted at a 45-degree angle using the in-plane technique to optimize needle tip visualization. Injection of approximately 20 ml of local anesthetic should be performed along the lateral and inferior aspect of the nerve with visualization of filling of the fascia iliaca compartment. Manual pressure should then be held for 5 minutes below the injection site. The use of pressure and Trendelenburg position facilitate the spread of anesthetic in a cephalad direction anesthetizing the obturator, lateral cutaneous, and the femoral nerve.
femoral nerve block
(video file)
Figure D: Real time clip of in-plane needle administering local anesthetic around the femoral nerve. Note the nerve “peeling” away from the femoral artery confirming entry into the fascia lata.
Indications
- Hip fractures
- Femur fractures
- Knee arthroscopies
- ACL reconstruction
- Patellar ligament realignment
- Patellar fracture
Advantages
- Quick and Effective
- Decreased reliance on opioids in the elderly and pediatric patients
- Safe and Rare complications
- ED physicians are already proficient in the use of procedural ultrasound








5 thoughts on “Ultrasound-Guided Femoral Nerve Block”
An alternative is the fascia iliaca block which can be performed with or without ultrasound guidance with the advantage of greater distance from the vascular structures
Pingback: LITFL Review 191 | LITFL: Life in the Fast Lane Medical Blog
Agree – FICB is probably easier for novice users. Especially when echogenic needles are used for improved visibility during the procedure
Pingback: Articles of the year (EMU 2018) – First10EM
Pingback: Femoral nerve blocks for hip fractures: the evidence – First10EM