Author: Brian Sumner, MD (@briansumner93; Resident Physician, Mount Sinai-St. Luke’s), Trent She (@trentshemd; Ultrasound Director, Mount Sinai-St. Luke’s) // Reviewed by: Stephen Alerhand, MD (@SAlerhand); Alex Koyfman, MD (@EMHighAK); and Manpreet Singh, MD (@MprizzleER)
Case
A 29-year-old female with a history of morbid obesity presents to the Emergency Department (ED) with a chief complaint of abdominal pain. Three days prior, she had undergone a Roux-en-Y procedure without complications. She went home yesterday morning after tolerating PO and passing flatus. Last night, she noted worsening pain across her entire abdomen and was feeling bloated. Since then, the pain has worsened and she now endorses fever, chills, and nausea. The patient has not passed flatus since leaving the hospital and has been unable to eat without regurgitating.
On arrival, the patient appears uncomfortable. Her vital signs are temperature of 101.4, heart rate 108, respiratory rate 16, blood pressure 135/67, and oxygen saturation 96% on room air. Her mucous membranes are dry and she has poor skin turgor. She is diaphoretic and diffusely tender on abdominal exam with guarding and rebound. Her incision sites are clean, dry, and intact without erythema or other signs of infection.
While the attending is putting in an order for a CT abdomen and pelvis, the intern on the team pulls over the ultrasound machine. The POCUS exam demonstrates an enhanced and well visualized echogenic line representing an enhanced peritoneal stripe. This is concerning for pneumoperitoneum.
Ultrasound
Pneumoperitoneum can be seen on ultrasound by two clear signs:
- The air within the peritoneal space rises and causes an enhanced peritoneal stripe sign (EPSS)– not to be confused with E-Point Septal Separation (EPSS) for left ventricular ejection fraction estimation. (See Image 1).

- Under normal circumstances, ultrasound waves course through the anterior abdominal wall and into the peritoneal fluid (or other solid organs) – this results in a thin peritoneal stripe that is echogenic to surrounding tissue.1
- In the setting of free air in the abdomen, the ultrasound waves are interrupted after passing through the anterior abdominal wall. This interruption causes scattering of the ultrasound waves, resulting in high-amplitude linear echoes causing an enhancement of the normal peritoneal stripe sign. In other words, the interface between gas and soft tissue is highlighted.1
- In the setting of large amounts of free air, the ultrasound operator can visualize reverberation artifact deep to the peritoneal stripe, similar to A-lines seen in normal lung tissue (“A-lines in the abdomen”). (see Video 1)
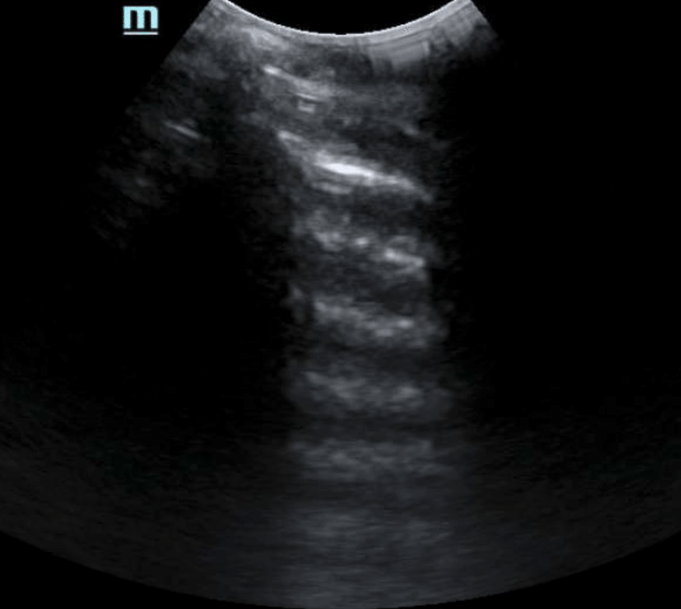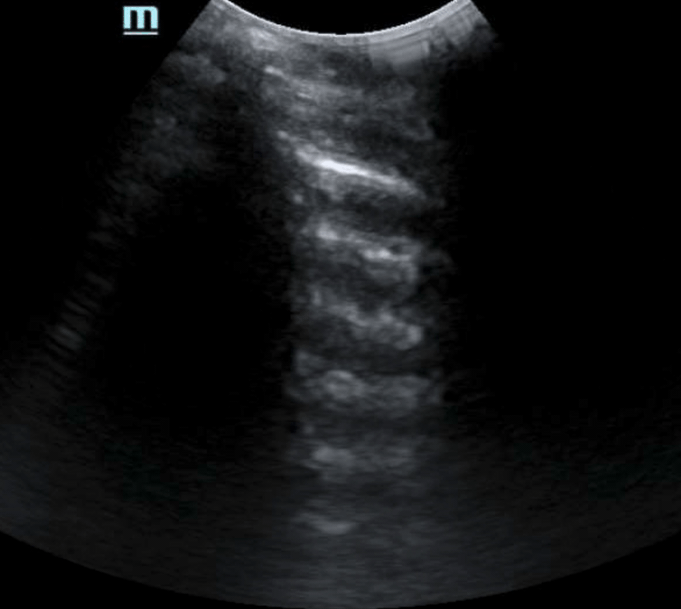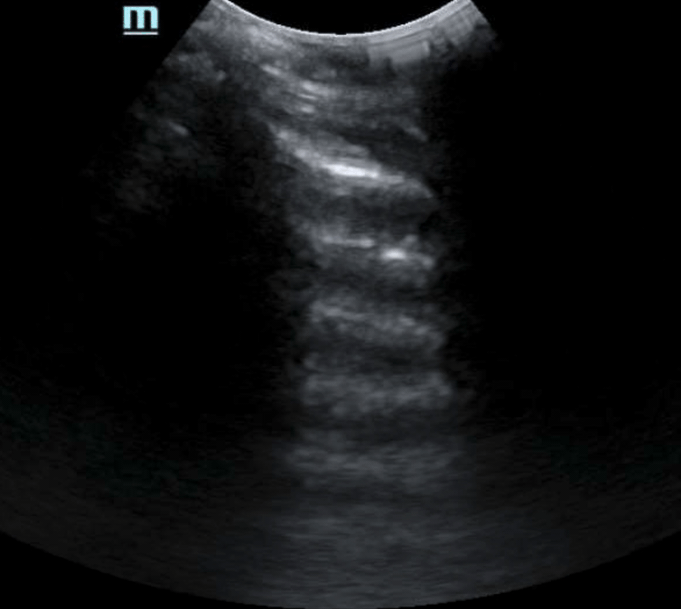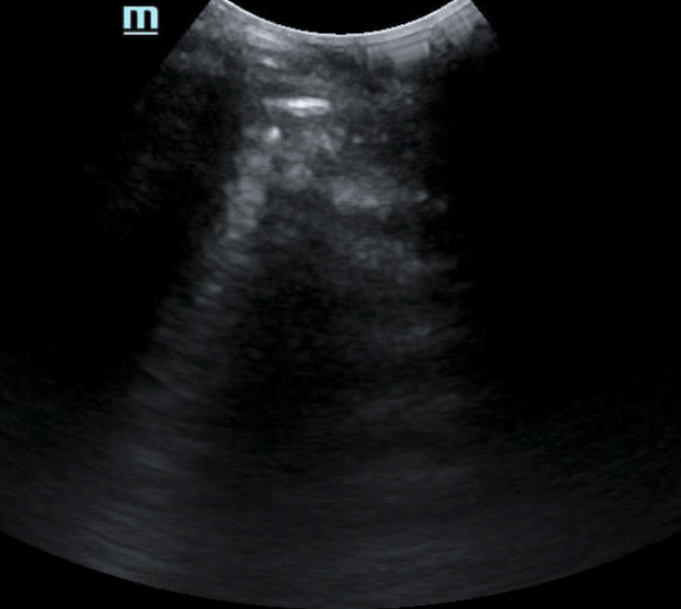
- Reverberation artifacts are repeated reflections through the image caused by an initial reflection at a highly reflective interface. One such example of this is the interface between the parietal and visceral lung pleura. In normal lung, you can see reflections down an entire image field. The strength of the reflected field tends to decrease with depth and dampens in echogenicity. Another scenario in which you can see reverberation artifact is pneumoperitoneum. In this scenario, as described above, the interface between the anterior abdominal wall and pleura becomes interrupted resulting in heavy reflection back towards the transducer. This can result in echogenic reflections throughout the image.2
Other signs to consider:
- Comet tail artifacts are echoes caused by reflections off highly reflective interfaces or within a highly reflective object. These internal reflections cascade ‘downward’ or in the direction of the ultrasound waves and dissipate with increased depth.2
- A quick note on gas within the lumen of bowel…it flows just like stool, so as the bowel peristalses, the gas will conform to its container. In general, we know that gas is HORRIBLE for ultrasound as sound waves do not particularly like traveling through it. This results in shadowing behind the gas which will change in position as the bowel contracts and relaxes (see Image 2 and Video 2 ).


One thing to keep in mind is that bowel filled with gas can also result in reverberation artifact (A lines) – so what can you look for to improve likelihood you assess correctly for free air? First, the reflections of intraluminal gas will change as the bowel contracts and relaxes. Secondly, the reflections of reverberation artifact occur at equidistance points on the image starting from the transducer to the disrupted gas-soft tissue interface. Therefore, if the reflections start deeper in the abdomen as opposed to right near the parietal peritoneum interface with soft-tissue organs, then it is likely intraluminal in origin.
Discussion
Pneumoperitoneum is seen most commonly in cases of perforated hollow viscus, intraperitoneal gas insufflations, penetrating abdominal injury, infection with gas-forming organisms, and spontaneous pneumoperitoneum.3 When suspected, plain upright posterior-anterior (PA) radiographs were the first imaging modalities used as they were considered the most sensitive, being able to detect free intraperitoneal air at volumes as low as 1 cubic centimeter.4 However, Woodring and Heiser found that sensitivity for pneumoperitoneum diagnosis were 98% versus 80% for upright lateral chest radiographs and PA films, respectively.4 Therefore, it is now thought that the upright lateral film is the most sensitive radiograph for detecting free abdominal air. Abdominal radiographs can also detect free intraperitoneal air at volumes as low as 1 ml, but at a lower sensitivity than both the upright lateral or PA films.5 All in all, the sensitivity and specificity of radiographs with regard to detection of pneumoperitoneum are variable and rates vary from study to study.
The sensitivity and specificity for pneumoperitoneum by means of POCUS is 92% and 53% respectively.6 This level of sensitivity is competitive with levels seen for plain radiography films.3-5 Therefore, POCUS should be considered a reasonable adjunct to diagnosis of pneumoperitoneum at the bedside during initial assessment while waiting for confirmatory abdominal CT scans (~100% sensitivity).
When performing POCUS for intraperitoneal air, the operator can use either a linear (10-12MHz) or curvilinear (2-3MHz) transducer.3 As with other US studies, transducers that produce higher frequency waves, such as the linear transducer, produce higher quality images but are limited at greater depths, and vice versa for the curvilinear transducer. Selection of transducer will largely be defined by the body habitus of the patient though usage of the linear transducer when available and appropriate is preferable, as it is more sensitive and produces higher quality images in the near field.3
The most likely obstacle encountered when performing this exam will be mistaking intraluminal bowel gas for free air. It is prudent that the operator looks for peristalsis of the air as a marker for being within the bowel wall. One way to try and prevent this is by looking at the RUQ. The anterior aspect of the liver is adjacent to the anterior abdominal wall and is not occupied by bowel.8 Therefore, if one sees an EPSS with reverberation artifact, he or she can reasonable ensure they are not are mistaking bowel gas for free air. Ultrasonography findings of free air include:
- Enhanced peritoneal stripe sign8
- Reverberation artifact8
- Comet-tail reverberatory artifacts8
- Air bubbles in ascitic fluid9
One last notable comment on the technique of ultrasound for pneumoperitoneum is usage of the ‘scissor maneuver’10 (see Video 3):

“When slight pressure was applied to the abdominal wall using the same end (the caudal part) of the probe, the free intraperitoneal air was expelled from the region anterior to the liver to other parts of the peritoneal cavity, and consequently, the reverberation artifact became much less prominent. Conversely, when the pressure on the distal end of the probe was released, maintaining the contact of the probe with the skin surface, the free gas returned to the epigastric region and the artifact echo pattern became more prominent. On real-time US examination, repetition of this maneuver appears like the opening and closing of scissors, leading to the term ‘‘scissors maneuver’’.10
The utility of POCUS in the ED is wide-ranging and has expanded tremendously over recent decades. The American College of Emergency Physician (ACEP) policy statement outlines the importance of this imaging modality as well as the increasing scope of practice. The scope of practice currently includes utilization of ultrasound in Trauma, Pregnancy, Cardiac /Hemodynamic assessment, Abdominal aorta, Airway/Thoracic, Biliary, Urinary Tract, Deep Vein Thrombosis (DVT), Soft-tissue/Musculoskeletal (MSK), Ocular, Bowel, and Procedural Guidance.11 The inclusion of bowel POCUS in the position statement from ACEP should reinforce the need for emergency providers to use this tool where applicable to help diagnosis intraabdominal bowel pathology.
Pearls and Pitfalls
- Don’t be afraid to utilize POCUS for evaluation of pneumoperitoneum.
- Differentiate pneumoperitoneum from intra-luminal air. Check for movement of A-lines with peristalsis.
- Look for EPSS, reverberation artifacts, and comet tail artifacts.
- Departments can be busy; utilize POCUS at the bedside to help guide treatment plans and expedite decision-making for advanced imaging and formal consults.
References/Further Reading:
- Indiran, V., Kumar, R. V., & Jefferson, B. (2018, May 3). Enhanced peritoneal stripe sign. Abdominal Radiology, 43, 3518-3519.
- Paushter, D. M. (2015). Primer and Clinical Significance of Artifacts in Ultrasound. American Association of Physicists in Medicine.The University of Chicago Medicine and Biological Sciences.
- Henfy, A. F., & Abu-Zidan, F. M. (2011, Oct-Dec). Sonographic diagnosis of introperitoneal free air. Journal of Emergencies, Trauma, and Shock, 4(4), 511-519.
- Woodring, J. H., & Heiser, M. J. (1995). Detection of pneumoperitoneum on chest radiographs: comparison of upright lateral and posteroanterior projections. American Journal of Roentgenology, 165(1), 45-47.
- Gans, S. L., Stoker, J., & Boermeester, M. A. (2012, June 13). Plain abdominal radiography in acute abdominal pain; past, present, and future. International Journal of General Medicine, 5, 525-533.
- Chen, S. C., Yen, Z. S., Wang, H. P., Lin, F. Y., Hsu, C. Y., & Chen, W. J. (2002). Ultrasonography is superior to plain radiography in the diagnosis of pneumoperitoneum. British Journal of Surgery, 89, 351/354.
- Smith-Bindman, R., Lipson, J., Marcus, R., Kim, K. P., Mahesh, M., Gould, R., . . . Miglioretti, D. L. (2009, Dec 14). Radiation Dose Associated with Common Computed Tomography Examinations and the Associated Lifetime Attributable Risk of Cancer. Archives of Internal Medicine, 169(22), 2078-2086.
- Chao, A., Gharahbaghian, L., & Phillips, P. (2014, December 23). Diagnosis of Pneumoperitoneum with Bedsite Ultrasound. Western Journal of Emergency Medicine, 16(2).
- Kricun, B. J., & Horrow, M. M. (2012, June). Pneumoperitoneum. Ultrasound Quarterly, 28(2)
- Karahan, O. I., Kurt, A., Yikilmaz, A., & Kahriman, G. (2004, October). New Method for the Detection of Intraperitoneal Free Air by Sonography: Scissors Maneuver. Journal of Clinical Ultrasound, 32(8), 381-385.
- American College of Emergency Physicians. (2016). Ultrasound Guidelines: Emergency, Point-of-care, and Clinical Ultrasound Guidelines in Medicine.Dallas: ACEP.






1 thought on “US Probe: Ultrasound for Diagnosis of Pneumoperitoneum”
Thanks for presenting this case! Great info. I’ve had many FAST scans that residents felt like they “couldn’t see anything” and it was because of perforated bowel from abdominal trauma. A-lines in the RUQ is bad! Thanks again.