Written by: Jacqueline Tin MD, Cailey Simmons MD, Jared Ditkowsky MD (Emergency Resident Physicians, Icahn School of Medicine at Mount Sinai), Stephen Alerhand, MD (@SAlerhand – Instructor of EM and Ultrasound Fellow, Icahn School of Medicine at Mount Sinai) // Edited by: Manpreet Singh, MD (@MPrizzleER – Assistant Professor in Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center)
23 year-old female with a history of prior shoulder dislocations presents to the ED after sustaining a shoulder injury while playing basketball earlier in the day. The patient reports she was going up for a rebound with her harm outstretched overhead. She heard her shoulder pop and was immediately unable to move her shoulder due to pain.
Physical exam is remarkable for deformity and tenderness at the right shoulder joint. Her arm is held in abduction and external rotation.
You are concerned for an anterior shoulder dislocation. You prepare the room for conscious sedation, with all the medications, protocols, and checklists at the ready. Then you call over one physician to administer the ketamine and monitor the cardiopulmonary status, another physician to assist you in physically relocating the shoulder, and a nurse to assist with medications and keep a timesheet.
The ketamine is administered and you wait for the patient’s dissociation. Somewhat surprisingly, it takes more ketamine that expected to achieve the required condition, during which time the patient has a brief period of apnea requiring your colleague to perform a jaw-thrust. Eventually, you attempt to reduce the shoulder, and after awhile of pulling and tugging, you think that the shoulder might be back in—but you are not sure.
WHAT NOW?
You have two options:
- Wait for the sedation to wear off and send the patient around the corner to x-ray (or perform a portable x-ray).
- If reduced, great.
- If not reduced, then you (and your colleagues) have to repeat the whole time-consuming and potentially dangerous process all over again.
- ULTRASOUND!
Or what if you never had to use conscious sedation in the first place, by using an ultrasound-guided intro-articular block for adequate analgesia?
INTRODUCTION/ANATOMY
The glenohumeral joint is comprised of a shallow ball-in-socket articulation with a large range of motion and minimal tendinous support on its inferior aspect; consequently, it is prone to dislocation. Comprising about 50% of major joint dislocations and 200,000 ED visits each year, glenohumeral dislocation is a common patient presentation to the ED (1-3). The incidence of anterior shoulder dislocation far outweighs that of posterior. While anterior dislocations are generally caused by a force pushing the humeral head inferior to the glenoid fossa, posterior dislocations are generally due to internal rotation and adduction (i.e. caused by trauma, electrical shock and seizure) (4).
Typically, plain film radiography is utilized to diagnose shoulder dislocation and evaluate for fractures. However pre-reduction radiographs may be unnecessary if fracture risk is low (i.e., young age, history of multiple dislocations, atraumatic mechanism). Relative to radiography, POCUS potentially allows for greater diagnostic efficiency, improved accuracy for detection, and a decreased error rate (5-9). In a prospective observational study of 73 patients, POCUS was 100% sensitive and specific for the diagnosis of dislocation (3). Furthermore, POCUS can be used to help guide intra-articular anesthetic injections (10), and evaluate whether attempts at reduction have been successful in real time.
APPROACH
• Stand behind the patient’s affected shoulder.
• Support the patient’s elbow inferiorly while the humerus is in adducted position.
• Find the scapular spine and palpate laterally just until you reach the glenohumeral space.
• Place curvilinear probe (or high frequency linear-array probe, depending on patient habitus) in transverse position parallel and just inferior to the scapular spine with probe marker to patient’s left.

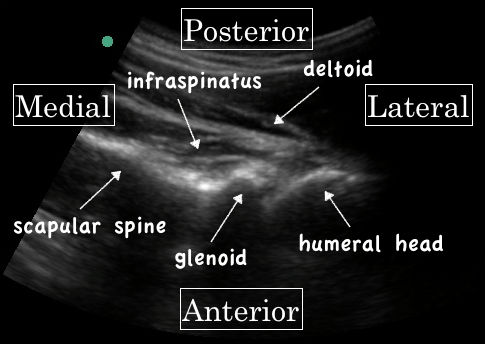
• Continue to move laterally until you find the glenoid and have a good view of the humeral head. You may need to adjust the depth so that both glenoid and humeral head are well visualized.

FINDINGS
The humeral head will appear as a circular structure immediately lateral to the glenoid fossa (see figure A). If the shoulder is not dislocated, the patient should freely internally and externally rotate the arm while adducted and movement of the humeral head in the glenoid fossa should be clearly visualized (7).
 .
.
With anterior dislocations, the humeral head will be seen deeper on the screen. .
.
With the probe, consider giving an intra-articular lidocaine injection for pain control. This approach involves localizing the glenoid and humeral head. Sterilize the skin overlying the deltoid muscle, and place local anesthetic with small bore needle. Next, using the ultrasound transducer in long axis, guide a 20G spinal needle through the deltoid muscle into the joint space (notice how the needle approaches from the side of the screen, as opposed to from the top left corner). Inject approximately 20 cc lidocaine 1% and wait 10-20 minutes before proceeding with reduction (2,5,10).

Posterior dislocations will appear more superficial on the screen as the dislocation is closer to the probe. (see figure B). Further, there may be some hyperechoic area suggesting hemarthrosis when there is a shoulder dislocation (5,6).
CONCLUSION
POCUS is a valuable tool to aid in the diagnosis and management of shoulder dislocation. From preliminary studies, POCUS can be used to reliably diagnose dislocation, aid in intra-articular joint injections, and confirm successful relocation.
References
1. Wolfson AB, Hendey GW, Ling LJ, Rosen CL, Schaider JJ, Sharieff GQ. Harwood-Nuss’ Clinical Practice of Emergency Medicine. Lippincott Williams & Wilkins; 2012.
2. Marx, John A, Robert S. Hockberger, Ron M. Walls, Michelle H. Biros, Daniel F. Danzl, Marianne Gausche-Hill, Andy Jagoda, Louis Ling, Edward Newton, Brian J. Zink, and Peter Rosen. Rosen’s Emergency Medicine: Concepts and Clinical Practice. , 2014. Chapter 53, 618-642.e2
3. Gottlieb M, Russell F. Diagnostic Accuracy of Ultrasound for Identifying Shoulder Dislocations and Reductions: A Systematic Review of the Literature. Western Journal of Emergency Medicine. 2017;18(5):937-942. doi:10.5811/westjem.2017.5.34432.
4. Kowalsky MS, Levine WN. Traumatic posterior glenohumeral dislocation: classification, pathoanatomy, diagnosis, and treatment. Orthop Clin North Am. 2008;39(4):519-33-viii.
5. Abbasi S, Molaie H, Hafezimoghadam P, et al. Diagnostic accuracy of ultrasonographic examination in the management of shoulder dislocation in the emergency department. Ann Emerg Med. 2013:1-6.
6. Beck S, Chilstrom M. Point-of-care ultrasound diagnosis and treatment of posterior shoulder dislocation. Am J Emerg Med. 2013;31(2):449.e3-449.e5.
7. Blakeley CJ, Spencer O, Newman-Saunders T, et al. A novel use of portable ultrasound in the management of shoulder dislocation. Emerg Med J. 2009;26(9):662-663.
8. Kowalsky MS, Levine WN. Traumatic posterior glenohumeral dislocation: classification, pathoanatomy, diagnosis, and treatment. Orthop Clin North Am. 2008;39(4):519-33-viii.
9. Weishaupt, D., Berbig, R., Prim, J., & Brühlmann, W. (1997). Sonographische Befunde nach Schulterluxation. Ultraschall in der Medizin, 18(03), 129-133
10. Emergency Ultrasound: Musculoskeletal Shoulder Dislocation. Emergency March;48(3):128-129- Author(s): Jehangir Meer, MD Sierra Beck, MD Todd Taylor, MD – http://www.mdedge.com/emed-journal/article/107209/imaging/emergency-ultrasound-musculoskeletal-shoulder-dislocation









2 thoughts on “US Probe: Ultrasound for Shoulder Dislocation and Reduction”
Pingback: LITFL Review 315 | Edwin M. Thames
Pingback: LITFL Review 315 • LITFL Medical Blog • FOAMed Review