Jia Jian Li, MD (Ultrasound Fellow, Yale University; @JjMDUS), Zachary Boivin, MD (Ultrasound Fellow, Yale University; @ZachBoivinMD), Stephen Alerhand, MD (@SAlerhand – Emergency Physician and Ultrasound Fellow, Icahn School of Medicine at Mount Sinai) // Edited by: Manpreet Singh, MD (@MPrizzleER – Assistant Professor in Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center)
Case
A 42-year-old female with no prior medical or surgical history presents to the Emergency Department reporting intense pain in the right upper quadrant (RUQ) of her abdomen that started a few hours prior. She characterizes the pain as sharp and persistent, exacerbated postprandially, and has not resolved. Abdominal examination reveals RUQ tenderness with guarding and a positive Murphy’s sign.
Considering her symptoms and examination, she warrants an evaluation for biliary pathology, specifically cholecystitis. While there are three imaging modalities to assess for cholecystitis: a radiology-performed RUQ ultrasound, a biliary point-of-care ultrasound (POCUS), or a CT abdomen and pelvis, physicians should utilize biliary POCUS given its accuracy in detecting cholelithiasis and cholecystitis.1 Furthermore, POCUS decreases ED length of stay compared to radiologist-performed ultrasound, with reductions of 11% during the day and up to 20% after hours.2
A biliary POCUS was performed, and showed the following:
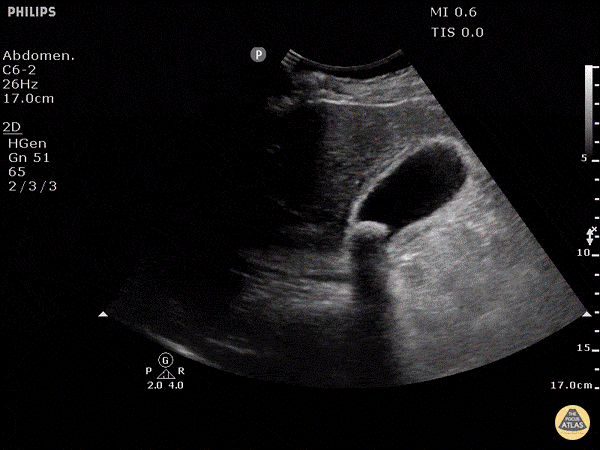
Making the Diagnosis?
Acute cholecystitis is defined by an acute inflammation of the gallbladder. In many cases, the underlying cause is the obstruction of the cystic duct due to an impacted stone in either the neck of the gallbladder or the cystic duct, leading to acute calculous cholecystitis.3
There are four sonographic findings that suggest acute cholecystitis:3
- Stones or sludge in the gallbladder neck
- Positive sonographic Murphy sign
- Anterior wall thickening
- Pericholecystic fluid
Gallstones appear as hyperechoic rounded structures with acoustic shadowing posteriorly. A stone in the neck is defined as an immobile stone lodged in the neck of the gallbladder without anechoic space between the neck and the stone it contains. It remains lodged in that position regardless of patient positioning. This finding, along with a positive sonographic murphy sign, is highly suggestive of cholecystitis, even in the absence of other ultrasonographic signs of infection.4

Gallbladder sludge can also appear in the gallbladder as low-amplitude homogeneous echoes, layering on the posterior wall, often forming a fluid-fluid level with anechoic bile above it, and will not shadow unless gallstones are also present.5 Both gallstones and sludge may move with changes in patient position, but a stone in the neck causing cholecystitis will be impacted in the gallbladder neck and have no movement.

A sonographic Murphy’s sign is elicited by centering the transducer over the gallbladder, in the right subcostal region and applying pressure, and should not be performed over the ribs to ensure accuracy. It differs from the physical examination Murphy’s sign, where maximal pain is elicited by pressing directly over the sonographically visualized gallbladder. While pain medication may increase a patient’s pain tolerance, a sonographic Murphy sign can still be evaluated. The reported prevalence of this sign is more than 95% in patients with acute cholecystitis.6

An anterior wall thickness greater than 3 mm is considered abnormal.7 This should be measured on the anterior wall of the gallbladder, as posterior acoustic enhancement (i.e. increased echogenicity posterior to a fluid-filled structure) can artificially increase the measurement of the posterior wall.
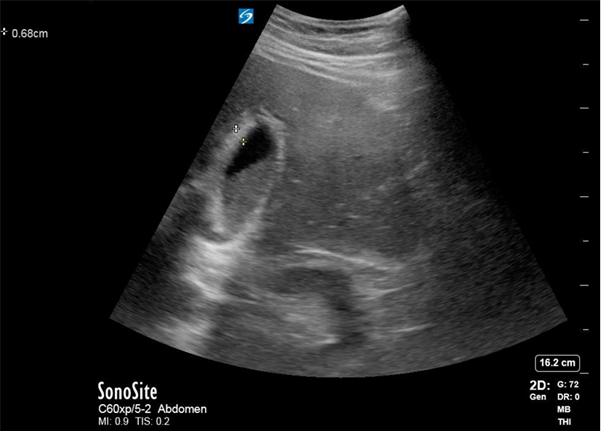
Pericholecystic fluid refers to the presence of serous fluid within the inflamed gallbladder wall, and should be included within the measurement of the gallbladder wall based on prior studies, although this is not uniform across all studies and may be institutionally dependent. 8

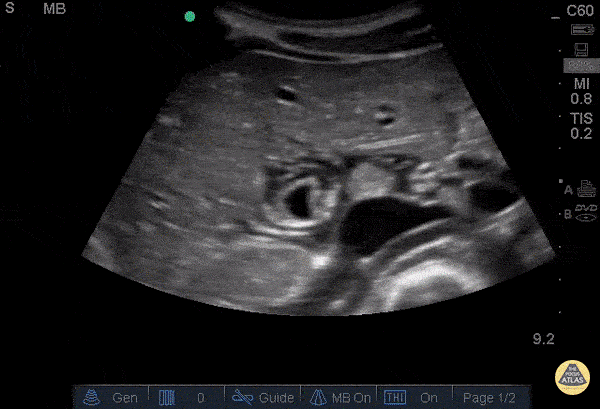
If the liver appears hyperechoic and there are no other findings suggestive of cholecystitis, it could be an artifact called focal fatty sparing, which is a hypoechoic area of the liver along the superior border of the gallbladder.9

A gallstone in the gallbladder neck and a positive sonographic Murphy sign are the only two sonographic findings to diagnose cholecystitis, with wall thickening and pericholecystic fluid being late findings.7
Pitfalls to Diagnosing Cholecystitis
- Missing the stone in the neck by looking at the gallbladder body and not completely fanning through.
- Mistaking an edge artifact, generated by the curve of the gallbladder, for shadowing of the stone. Trace the shadow back to either a hyperechoic curved structure (stone) or the gallbladder wall (edge artifact). Also try to visualize the gallbladder from another angle.
- Calling a sonographic Murphy’s sign in a patient who is tender throughout the abdomen, not just over the gallbladder.
- Focal fatty sparing in a patient with hepatosteatosis can mimic pericholecystic fluid, but there will be no other abnormalities of the gallbladder, and the liver often appears hyperechoic with hepatosteatosis.
- A contracted gallbladder can appear to have a thickened wall.
- The gallbladder wall can also appear in conditions such as cirrhosis, congestive heart failure, and renal failure, among others.
- Measuring the posterior wall, which is artificially thickened due to posterior acoustic enhancement.
Conclusion
This patient was found to have a positive sonographic Murphy’s sign, a stone in the neck of the gallbladder, and a thickened gallbladder wall. She was admitted to the surgical team and had an uncomplicated cholecystectomy the same day.
References:
- Wertz JR, Lopez JM, Olson D, Thompson WM. Comparing the Diagnostic Accuracy of Ultrasound and CT in Evaluating Acute Cholecystitis. AJR. American journal of roentgenology. 2018;211:W92-w97.
- Blaivas M, Harwood RA, Lambert MJ. Decreasing length of stay with emergency ultrasound examination of the gallbladder. Acad Emerg Med. 1999;6:1020-1023.
- Indar AA, Beckingham IJ. Acute cholecystitis. BMJ. 2002;325:639-643.
- Nelson M, Ash A, Raio C, Zimmerman M. Stone-In-Neck phenomenon: a new sign of cholecystitis. Critical ultrasound journal. 2011;3:115-117.
- Jain R. Biliary Sludge: When Should It Not be Ignored? Curr. Treat. Options Gastroenterol. 2004;7:105-109.
- Hilsden R, Leeper R, Koichopolos J, et al. Point-of-care biliary ultrasound in the emergency department (BUSED): implications for surgical referral and emergency department wait times. Trauma Surg Acute Care Open. 2018;3:e000164.
- Gupta P, Marodia Y, Bansal A, et al. Imaging-based algorithmic approach to gallbladder wall thickening. World J. Gastroenterol. 2020;26:6163-6181.
- Joseph A. Gallstones [Rapid Response]. BMJ. 2014;348.
- Chen K, Hiramatsu Y, Yunoki M, Hirano Y. [Focal sparing around the gallbladder in fatty liver: an useful sign in the diagnosis of borderline cases by CT]. Nihon Igaku Hoshasen Gakkai Zasshi. 1989;49:146-152.
Additional Useful Literature:
- Blaivas M, Harwood RA, Lambert MJ. Decreasing length of stay with emergency ultrasound examination of the gallbladder. Acad Emerg Med. 1999;6(10):1020-1023. doi:10.1111/j.1553-2712.1999.tb01186.x
- Summers SM, Scruggs W, Menchine MD, et al. A prospective evaluation of emergency department bedside ultrasonography for the detection of acute cholecystitis. Ann Emerg Med. 2010;56(2):114-122. doi:10.1016/j.annemergmed.2010.01.014
- Ross M, Brown M, McLaughlin K, et al. Emergency physician-performed ultrasound to diagnose cholelithiasis: a systematic review. Acad Emerg Med. 2011;18(3):227-235. doi:10.1111/j.1553-2712.2011.01012.x
- Dumbrava BD, Bass GA, Jumean A, Birido N, Corbally M, Pereira J, Biloslavo A, Zago M, Walsh TN. The Accuracy of Point-of-Care Ultrasound (POCUS) in Acute Gallbladder Disease. Diagnostics (Basel). 2023 Mar 26;13(7):1248. doi: 10.3390/diagnostics13071248. PMID: 37046466; PMCID: PMC10093186.
- Koichopolos J, Hilsden R, Myslik F, Thompson D, Vandelinde J, Leeper R. Surgeon attitudes toward point of care ultrasound for biliary disease: a nationwide Canadian survey. Can J Surg. 2020 Jan 9;63(1):E9-E12. doi: 10.1503.cjs/010218. PMID: 31916431; PMCID: PMC7828949.
- Yang FJ, Kohen B, Sanapala S, Halperin M. A Potential Pitfall in POCUS of the Gallbladder: Beware of the Duodenum. POCUS J. 2022 Nov 21;7(2):188-189. doi: 10.24908/pocus.v7i2.15632. PMID: 36896391; PMCID: PMC9983711.
- Al-Khouja F, Mazumder P, Moeller J, Lahham S. A Case Report on Detecting Porcelain Gallbladder form Wall-Echo-Shadow Sign on Point-of-Care Ultrasound. J Educ Teach Emerg Med. 2021;6(2):V25-V29. Published 2021 Apr 19. doi:10.21980/J8164G
- van Breda Vriesman AC, Engelbrecht MR, Smithuis RH, Puylaert JB. Diffuse gallbladder wall thickening: differential diagnosis. AJR Am J Roentgenol. 2007;188(2):495-501. doi:10.2214/AJR.05.1712
- Woo MY, Taylor M, Loubani O, Bowra J, Atkinson P. My patient has got abdominal pain: identifying biliary problems. Ultrasound. 2014;22(4):223-228. doi:10.1177/1742271X14546181
Video Resources
- 5 minute sono – https://coreultrasound.com/gallbladder/
- https://www.thepocusatlas.com/hepatobiliary





