Originally published at CoreEM.net, who are dedicated to bringing Emergency Providers all things core content Emergency Medicine available to anyone, anywhere, anytime. Reposted with permission.
Follow Dr. Swaminathan and CORE EM on twitter at @EMSwami and @Core_EM
Written by: Anand Swaminathan, MD (@EMSwami) // Edited by: Reuben Strayer, MD (@emupdates)
Definition: A wide-complex (QRS complex > 120 msec) tachydysrhythmia that originates within or below the bundle of His.
- Nonsustained VT: Short episodes of VT lasting < 30 seconds
- Sustained VT: prolonged episodes of VT lasting > 30 seconds
Differential to Consider
- SVT (or atrial flutter) with aberrancy (i.e. WPW)
- Sinus tachycardia with a bundle branch block
Mimics (typically, wide with rate < 110 bpm) (Hollowell 2005)
- Hyperkalemia
- Na Channel Blocking Agent Overdose
- Accelerate Idioventricular Rhythm (AIVR)
Diagnosis
There are a number of algorithms that can be used to diagnose VT with the Brugada criteria being the most widely used. The derivation study of this algorithm found a sensitivity of 98.7% and specificity of 96.5%. (Brugada 1991). However, the study was not performed under ED circumstances (patients were taken off cardiac meds prior to EKG, not acute presentations etc). There is no algorithm that has 100% sensitivity or specificity.
Common EKG Findings
- Atrioventricular (AV) dissociation: atria and ventricles do not activate in a synchronous fashion. The EKG reveals P waves that are not conducted or linked to the QRS complexes.
- Fusion beats: a hybrid complex resulting from the collision of a supra ventricular and ventricular impulse
- QRS > 140 msec
Critical Point: It is safer to assume all wide-complex, regular tachydysrhtyhmias as VT, because the treatment of SVT with aberrancy (the most common alternate diagnosis) as if it is VT is safe but misdiagnosing VT as SVT with aberrancy is potentially life-threatening.
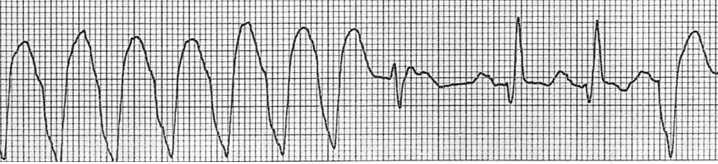
Ventricular Tachycardia EKGs – See CORE EM Website for list
Immediate Management: The primary goal is to convert the patient back to sinus rhythm and then, to address the underlying cause (most likely ischemic heart disease)
Basics: ABCs, IV, O2, Cardiac Monitor and 12-lead EKG
Directed Management
- Establish patient stability
- Pulseless: If the patient has no pulse or blood pressure, proceed immediately to defibrillation and chest compressions.
- Unstable: Evidence of end-organ (brain, heart) malperfusion or hypotension. This may manifest as altered mental status, severe shortness of breath or chest pain. If the patient is unstable, proceed directly to electrical cardioversion
- Stable: If the patient is stable, you may pursue electrical or chemical cardioversion
- Electrical Cardioversion
- Synchronized cardioversion is indicated for unstable patients with VT who have a pulse.
- Synchronized cardioversion should also be strongly considered in stable patients with VT as it is safe and both more effective and more rapid than chemical cardioversion.
- Dose: Biphasic 100 – 200 Joules (Monophasic 200 – 360 Joules)
- Unless patient in extremis, consider sedation /analgesia for procedure
- Chemical Cardioversion
- Lidocaine
- Class 1B antidysrhythmic agent
- Dose
- Bolus: 1.0-1.5 mg/kg (repeat 0.5 – 0.75 mg/kg up to total of 3 mg/kg)
- Infusion: 1-4 mg/min
- Lidocaine
- Procainamide
- Class 1A antidysrhythmic agent
- Dose: 30-50 mg/min IV until dysrhythmia terminated (max of 18 mg/kg)
- Amiodarone
- Dose
- Bolus: 150 mg IV over 10 min
- Infusion: 1 mg/min IV X 6 hours then 0.5 mg/min X 18 hours
- Dose
Critical Point: Although amiodarone is touted as the 1st line drug for chemical cardioversion of VT in ACLS, evidence suggests that it has poor efficacy in terminating VT. (Marill 2006, Tomlinson 2008, deSouza 2013).
Disposition: The vast majority of patients with an episode of ventricular tachycardia should be admitted to the hospital (preferably a high-acuity setting) for further workup with cardiology or electrophysiology. Patients with a properly functioning AICD may be discharged, usually after device interrogation and discussion with cardiology.
Take Home Points
- In the patient with a regular, wide-complex tachydysrhythmia, it is safer to treat the patient as VT.
- Consider VT mimics when the rate is < 120 bpm.
- Although chemical cardioversion is an option, electrical cardioversion should be considered in stable VT as it is safe, more effective and more rapid in returning the patient to sinus rhythm.
References
Hollowell H et al. Wide-complex tachycardia: beyond the traditional differential diagnosis of ventricular tachycardia vs supra ventricular tachycardia with aberrant conduction. Am J Emerg Med 2005; 23: 876-89. PMID: 16291445
Brugada P et al. A new approach to the diagnosis of regular wide complex tachycardia. Circulation 1991; 83: 1649-59. PMID: 2022022
Marill KA et al. Amiodarone is poorly effective for the acute termination of ventricular tachycardia. Ann Emerg Med 2006; 47: 217-24. PMID:16492484
Tomlinson DR et al. Intravenous amiodarone for the pharmacological termination of haemodynamically-tolerated sustained ventricular tachycardia: is bolus dose amiodarone an appropriate first-line treatment? Emerg Med J 2008; 25: 15-18. PMID: 18156531
deSouza IS et al. Antidysrhythmic drug therapy for the termination of stable, monomorphic ventricular tachycardia: a systematic review. Emerg Med J 2013; PMID: 24042252
Yealy D, Kosowsky JM: Dysrhythmias, in Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 8. St. Louis, Mosby, Inc., 2010, (Ch) 79: p 1034-63.








2 thoughts on “Core EM: Ventricular Tachycardia”
Hi Swami
Great post!
What about aVR evaluation? http://dx.doi.org/10.1016/j.hrthm.2007.09.020
Thanks
Roberto
Hi Swami
Great post!
What about aVR evaluation? http://dx.doi.org/10.1016/j.hrthm.2007.09.020
Thanks
Roberto