Author: Jamie Santistevan, MD (@jamie_rae_EMdoc – EM Physician, Presbyterian Hospital, Albuquerque, NM) // Edited by: Manpreet Singh, MD (@MPrizzleER – Assistant Professor of Emergency Medicine / Department of Emergency Medicine – Harbor-UCLA Medical Center)
Welcome to this edition of ECG Pointers, an EMDocs series designed to give you high yield tips about ECGs to keep your interpretation skills sharp. For a deeper dive on ECGs, we will include links to other great ECG FOAMed!
The Case:
An 80 year old female presents with one hour of sudden-onset, burning chest pain radiating to her back with associated nausea.

An old ECG from 6 months prior:

She receives aspirin and sublingual nitroglycerine and continues to have pain. A repeat ECG several minutes later:
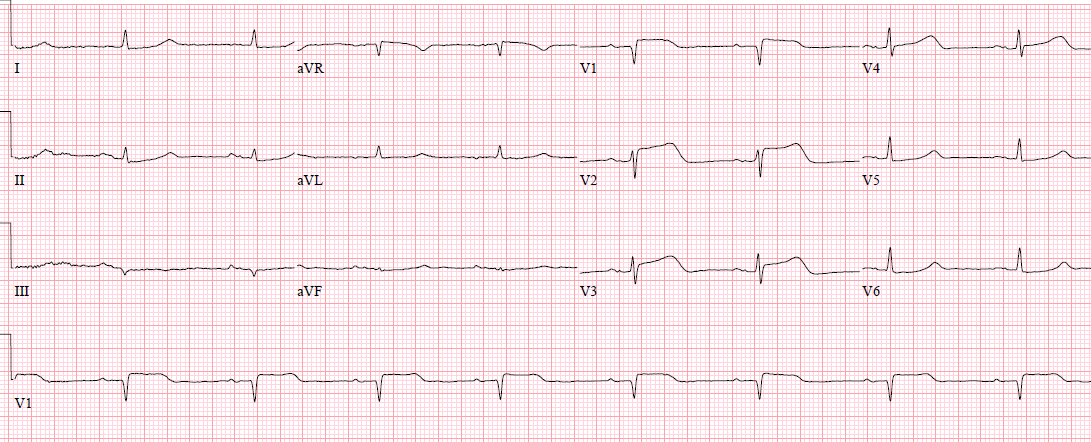
What are hyperacute T waves?
When a coronary artery becomes occluded, the ECG begins to change over time in a predictable way. The earliest changes are in T-wave shape and size. Within 30 minutes of artery occlusion the T-wave height and width increases. This is followed by ST-segment elevation and subsequent decrease in R-wave amplitude and Q-wave development.
This means that early in arterial occlusion, the T-wave becomes disproportionately large when compared to the QRS complex. These tall, broad T-waves are called “hyperacute” because they are the first sign of arterial occlusion.

What are ECG findings to look for?
- T-waves that are prominent and bulky
- Widening of the base of the T-wave and subsequent increase in the QT interval.
- T-waves that are relatively large when compared to the R-wave.
- Decrease in R-wave amplitude
- ST depression in the reciprocal leads (it may be subtle).
Case conclusion:
Look again at our patients initial ECG:
There is 1mm ST elevation in V1-V2. In leads V1-V4, the T-waves are broad-based and are very tall relative to the small R-waves. There is also slight reciprocal ST depression in lead II.
The ED provider was concerned and repeated the ECG, which then showed the development of an anterior STEMI. The cath lab was activated, which found complete (100%) occlusion of the LAD. A single stent was placed to the LAD.
The patient presented 1 hour after symptom onset and initial serum Troponin I was below detection (<0.017ng/mL). Remember: hyperacute T-waves may be the first sign of arterial occlusion and troponin levels may not be elevated yet. The diagnosis of acute coronary occlusion can be made by ECG findings alone – do NOT rely on troponin levels and get serial ECGs.
What are the main ECG Pointers for Hyperacute T-waves?
- Hyperacute T-waves are the first sign of arterial occlusion
- They are wide and prominent and localized to the anatomic region of infarct
- They are disproportionately large when compared to the R-waves in the affected leads
- There may be subtle reciprocal ST depression – look carefully for it
- When in doubt, obtain serial ECGs!
But wait, here’s some more ECG FOAM content:
For several examples of hyperacute T-waves in early coronary artery occlusion check out these cases on Dr. Smith’s ECG blog:
For a deep dive on abnormal T-waves here’s another great EMDocs post from the past:
Special thanks to Dr. Marci Gambarota for sharing these ECGs and interesting case with me!
References:
- Dressler, W and Roesler, H. High T waves in the earliest stage of myocardial infarction. Am Heart J. 1947 Nov;34(5):627-45.
- Nable, JV and Brady, W. The evolution of electrocardiographic changes in ST-segment elevation myocardial infarction. Am J Emerg Med. 2009 Jul;27(6):734-46.
- “ECG changes in acute MI”. Doctors Gates Blog. 22 Oct 2015. Web. http://doctorsgates.blogspot.com/2011/01/ecg-changes-in-acute-mi.html






1 thought on “ECG Pointers: Hyperacute T-Waves”
Pingback: Länkar v1-3 | Internmedicin