Author: Jamie Santistevan MD (@jamie_rae_EMDoc, EM Resident Physician, University of Wisconsin) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UT Southwestern Medical Center / Parkland Memorial Hospital) & Justin Bright, MD (EM Attending Physician, Henry Ford Hospital, @JBright2021)
Introduction
What if you could identify a patient with complete coronary vessel occlusion almost immediately after it occurs, before the ST segments begin to elevate? What if you could pick up the very subtle, early MI? We know that early recognition and intervention improves outcomes in patients with coronary artery occlusion. Sometimes patients presenting with ACS are obvious. Sometimes it seems that the patient has read the textbook. However, more often than not, patients are not obvious, especially in the early stages of ACS. That is why we are concerning ourselves with subtlety.
Welcome to Part II of a three-part series on subtle ECG findings in ACS. Last time we reviewed the ECG findings associated with left main coronary artery disease, where we discussed the meaning of ST elevation in lead aVR. Now we are going to turn our attention to the T-waves.
The T-wave represents the period of ventricular repolarization on the ECG. The normal T-wave appearance varies based on lead placement, age, and sex. In general, T-waves are tallest in leads II and V4 and will decrease in size with age. A normal T-wave usually has amplitude of less than 5mm in the precordial leads and less than 10mm in the limb leads [1]. The normal shape of a T-wave is asymmetric, with a slow upstroke and a rapid down stroke. Normal T-waves are always upright except in leads aVR and V1 and have a normal QT interval (QTc of 350-440ms in men or 350-460ms in women). Additionally, the R-wave amplitude should progress normally across the precordial leads.
In this post, we are going to review 4 causes of abnormal T-waves:
- Hyperacute T-waves in AMI
- The de Winter T-wave pattern
- Pseudonormalization of T-waves
- Hyperkalemia
Hyperacute T-waves
Immediately after coronary artery occlusion, the ECG undergoes predictable temporal changes. Classically, coronary vessel occlusion leads to elevation of the ST-segments (producing STEMI). However, the earliest findings on an ECG are subtle changes in the T-wave shape and size. When a coronary artery is occluded, within the first 30 minutes, the T-wave amplitude increases [2]. The next changes are ST-segment elevation and loss of the R-wave amplitude. If the vessel remains occluded, Q-waves develop. Without intervention, the ECG will then begin to exhibit T-wave inversions and eventually, the ST-segments will normalize [3]. Persistent ST-segment elevation suggests aneurysm formation.
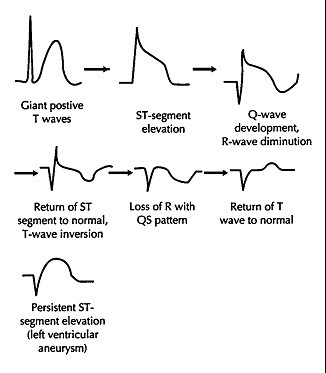
Early in the course of AMI, biochemical markers may not be elevated, although this may be changing in the era of highly sensitive troponin assays. Regardless, the development of T-wave changes is the first sign that we can see on the ECG and the ECG is fast, cheap, noninvasive, and readily available in the ED. In the early stages of MI, prior to the development of necrosis, the myocardium is suffering from ischemia. Timely revascularization may actually prevent complete infarction and death of the affected portion of the myocardium. Therefore, recognizing ACS early is beneficial because patients have improved outcome the timelier revascularization occurs [3], and delay to reperfusion causes larger infarction size and worse functional outcomes [4].
It is well known that new ST-segment elevation represents complete vessel occlusion and transmural infarct. However, the STEMI criteria have limited sensitivity in diagnosing coronary artery occlusion [5, 6, 7]. This means that some patients ultimately diagnosed with NSTEMI will also have complete coronary artery occlusion.
Below are the AHA criteria that define STEMI [7]:

Of course, it is important to recognize an obvious STEMI, but patients may present initially with only subtle ECG changes and minimal ST-segment elevation they may not meet the official criteria. These “subtle STEMI” patients have higher rates of inappropriate ED discharge and significant delays to reperfusion [8, 9, 10]. It is true that more ST elevation indicates a larger area of infarcted myocardium, however patients with subtle ST elevation MI experience similar functional outcomes and mortality rates as those with obvious STEMI [10]. Furthermore, approximately 25% of patients who do not meet the STEMI criteria, and are diagnosed with NSTEMI, have a completely occluded artery on angiography [11]. Some experts would argue that patients with subtle findings of coronary vessel occlusion should be treated as expeditiously as patients with obvious STEMI [10].
The T-wave is often the first deflection on the ECG to change in acute vessel occlusion. Initial changes to the T-wave are straightening of the ST-segment and enlargement of the T-wave height and width. The T-wave becomes disproportionately large when compared to the QRS. The prominent T-waves seen early in coronary vessel occlusion are called hyperacute T-waves. They were first described in 1947 as an early marker of coronary artery occlusion [2].
Hyperacute T-waves are often bulky, and wide at the base and are localized to an anatomic area of infarct. The widening of the T-wave may also lengthen the QT interval. It must be emphasized that hyperacute T-waves are not necessarily always tall, they may only be relatively large when compared to the R-wave. This means that even a small T-wave can still be hyperacute if paired with a low-voltage QRS. It is important to note that there is no acceptable universal definition of hyperacute T-waves, but there can be other clues on the ECG. During the development of hyperacute T-waves, there can be associated ST-segment depression in the reciprocal leads.
Here is an example of an ECG with hyperacute T-waves localized to the anterior region:

Do not be distracted by the first-degree AV block or by the PVCs. This ECG shows very prominent, broad-based T-waves in the anterior leads (V2-6). Notice also the loss of R-wave height throughout the precordium and the how the T-waves are massive in comparison to the QRS complexes. This ECG is concerning for LAD occlusion.
The patient underwent repeat ECG 40 minutes later, which showed obvious anterior ST elevation:
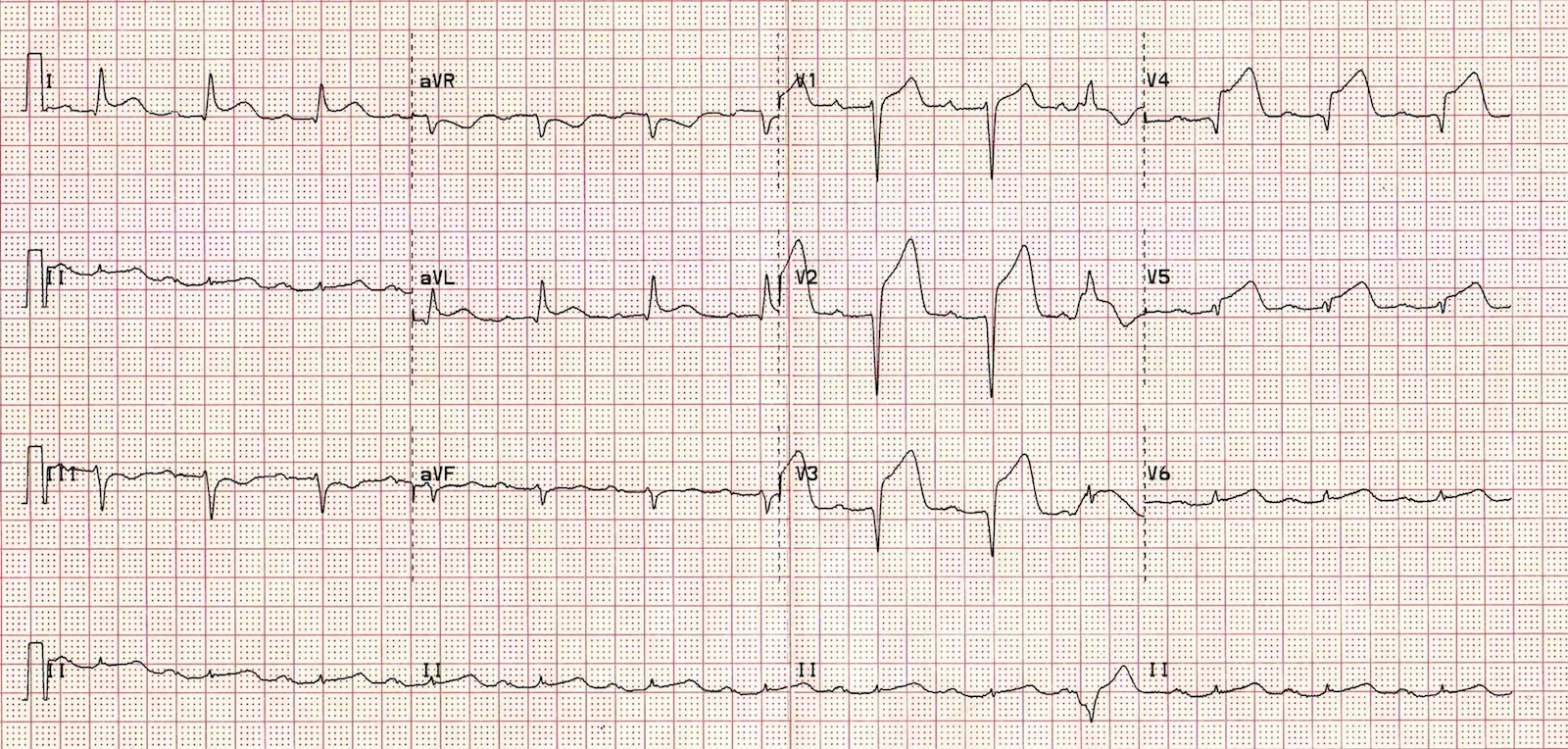
Now there is obvious ST elevation in the anterior leads (V2 and V3), as well as ST elevation in the lateral leads (I, aVL, V5 and V6) with reciprocal depression in lead III. Also, the Q-waves are deepening in the leads V2 and V3.
Here is another example of hyperacute T-waves, this time in the inferior leads. This is the ECG of a 75 year-old woman presenting with chest pain:

Notice the large T waves in the inferior leads. The total height of the T-waves is not all that impressive, but when compared to the QRS complexes, especially in aVF, the T-wave is massive. The ST-segments are straighter than normal and there is subtle ST elevation in lead III, aVF, V5-V6. Notice the subtle reciprocal ST depression and T-wave inversion in aVL. The machine read this ECG as Early Repolarization. Her Troponin I came back slightly elevated (0.07 ng/mL). She was found to have complete occlusion of the RCA on angiogram and was diagnosed with “NSTEMI”.
De Winter T-waves
An interesting variant of hyperacute T-waves are those paired with J-point depression. This causes a T-wave takeoff point that is below the isoelectric line. This “depressed T-wave takeoff” pattern was first described in 2009 by Verouden and colleagues and was found to represent complete LAD occlusion (a STEMI-equivalent) [15]. This pattern of up sloping ST-segment depression paired with a tall, prominent T-wave is present in about 2% of patients with LAD occlusion [15]. It was initially postulated that these findings are not dynamic, but rather that they remain static throughout coronary vessel occlusion until the time of reperfusion [15, 16]. However, some experts have documented de Winter T-waves developing during anterior STEMI and would argue that these findings may represent subtotal occlusion of the LAD. Regardless, these patients require immediate reperfusion.
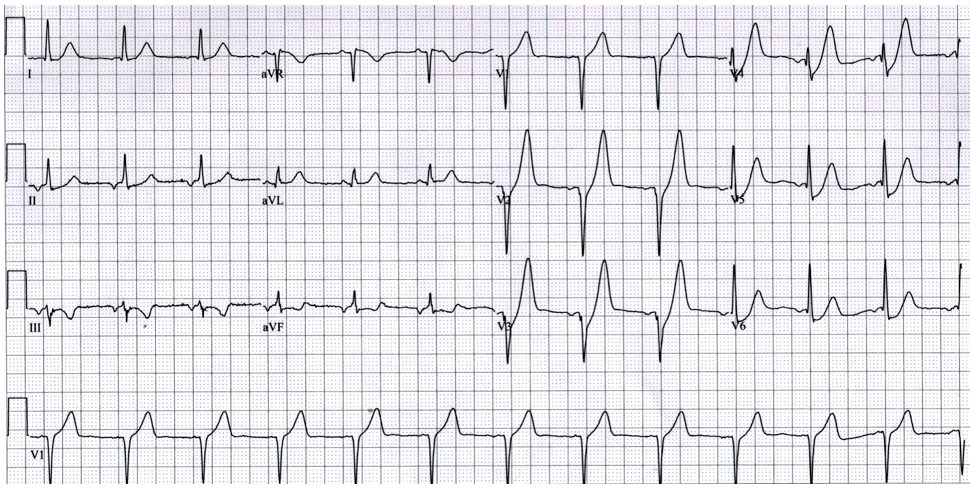
Notice the up sloping ST depression seen in leads V2-V6 followed by very tall and symmetric T-waves. Notice also the subtle reciprocal depression in the inferior leads (II, III, and aVF).
For an interesting case of the de Winter T-wave pattern occurring in a patient who initially presented with an obvious anterior STEMI, read this case on Dr. Smith’s ECG blog: http://hqmeded-ecg.blogspot.com/2014/07/is-lad-really-completely-occluded-when.html.
Pseudonormalization
Another interesting phenomenon of the T-waves is the pseudonormalization in AMI. This occurs when a patient with baseline T-wave inversions presents with acute coronary occlusion. Hyperacute T-waves in these patients manifest as upright T-waves, which may be confused for a normal ECG. This finding highlights the fact that it is not solely the height, but rather the increase in positive amplitude, that signifies a hyperacute T-wave [2]. The other scenario for pseudonormalization is a patient who presents with re-occlusion of a recently reperfused artery, also known as Wellens’ Syndrome.
Here is the classic appearance of Wellens’ syndrome, type A (left) and type B (right):

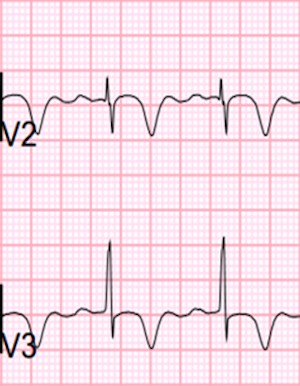
These images originally appeared at: http://lifeinthefastlane.com/ecg-library/wellens-syndrome/
It is important to note that this pattern appears when the patient is asymptomatic because this represents a reperfusion pattern on ECG. Type A, the biphasic T-waves, are seen immediately upon reperfusion. As the artery remains open, the T-waves evolve to be more deeply inverted, a Type B pattern. When the patient becomes symptomatic it is because the vessel re-occludes. When that happens the T-waves become upright (pseudonormalization) and if it remains occluded, ST-segment elevation will appear. These lesions are unstable because the vessel can re-occlude at any time and the patient requires revascularization.
Hyperkalemia
Perhaps the most well known cause of prominent T-waves is the peaked T-waves seen with hyperkalemia, and they can be confused with the hyperacute T-waves of ACS. There is no exact correlation between serum potassium and onset of ECG changes but about 80% of patients begin to exhibit ECG changes at 6.8-7.0mEq/L. The typical progression of ECG changes in hyperkalemia is first the development of peaked T-waves, followed by decreased P-wave amplitude, widening of the QRS complex and finally development of a sine wave. But, as we know, hyperkalemia can cause a myriad of ECG changes including AV and bundle branch blocks, bradycardias, and even a STEMI mimic. Here are the typical changes with hyperkalemia.

Although the T-waves of early hyperkalemia are very tall and prominent, the key differentiator from hyperacute T-waves is the shape of the T-wave. Hyperacute T-waves are fat and wide with a more blunted peak. The T-waves of hyperkalemia are very pointy, peaked or “tented” with a narrow base, they have sharp apex and tend to be extraordinarily symmetric [1].
Here is the ECG of a patient with a history of type I diabetes who presented with nausea and vomiting. EMS reported that the patient was in sinus tachycardia with a rate of 300.
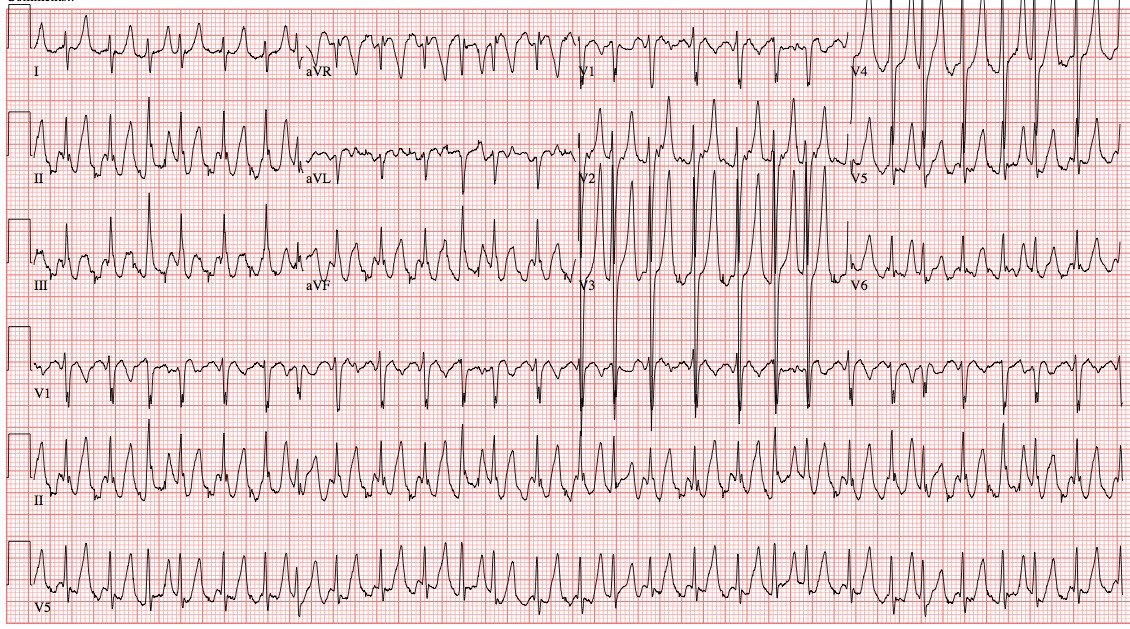
Notice the very tall, pointy T waves, which have a narrow base and are extremely symmetric. This patient was found to be in severe DKA, with a pH of 7.17 and a potassium of 7.1 mmol/L. The tall T-waves were likely being mistaken for QRS complexes and cardiac monitor misread the rate to be 300, when in fact it is about 150.
Conclusion
The earliest changes on an ECG after acute vessel occlusion are hyperacute T-waves and patients with coronary vessel occlusion can present with only subtle ECG changes. The ECG is an important tool, but should not always be used in isolation (unless clearly diagnostic). The clinical picture and adjunctive information should always be considered. If suspicious for vessel occlusion by the appearance of the ECG, it is important to look carefully for reciprocal changes and get serial ECGs every 15 minutes (not in an hour or two) and look for evolving changes because ACS is a dynamic process. Other adjuncts that may help diagnose ACS in patients with subtle ECG changes include continuous ST-segment monitoring, echocardiogram to evaluate for wall motion abnormality, and cardiac biomarkers.
TAKE HOME POINTS
- Hyperacute T-waves are often the first manifestation of complete vessel occlusion; they are wide, bulky and prominent.
- Hyperacute T-waves are not necessarily tall, and small T-waves can still be hyperacute when paired with a low-amplitude QRS complex.
- De Winter T-waves represent LAD occlusion (a STEMI equivalent) requiring immediate revascularization.
- Previously inverted T-waves can appear normal and upright in the setting of acute vessel occlusion. This is known as pseudonormalization.
- The tall T-waves associated with hyperkalemia are sharp, pointy, symmetric, and have a narrow base.
- When in doubt, get serial ECGs (every 15 minutes) and use adjunctive information.
Well, that concludes this post on hyperacute T-waves and other T-wave abnormalities. Please stay tuned for the third installment on subtle ECG findings: the subtle anterior STEMI mimicking benign early repolarization!
References / Further Reading
- Somers, MP et al. The prominent T wave: electrocardiographic differential diagnosis. Am J Emerg Med. 2002 May;20(3):243-51.
- Dressler, W and Roesler, H. High T waves in the earliest stage of myocardial infarction. Am Heart J. 1947 Nov;34(5):627-45.
- Nable, JV and Brady, W. The evolution of electrocardiographic changes in ST-segment elevation myocardial infarction. Am J Emerg Med. 2009 Jul;27(6):734-46.
- Keeley, EC et al. Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Lancet. 2003 Jan 4;361(9351):13-20.
- Zarling, EJ et al. Failure to diagnose acute myocardial infarction: The clinicopathologic experience at a large community hospital. JAMA. Sep 1983;250(9):1177-81.
- Scott, PJ et al. Optimization of the precordial leads of the 12-lead electrocardiogram may improve detection of ST-segment elevation myocardial infarction. J Electrocardiol. Jul-Aug 2011;44(4):425-31.
- Thygesen, K et al; Third universal definition of myocardial infarction. Circulation. Oct 2012;126(16):2020-2035.
- Pope, JH et al. Missed diagnoses of acute cardiac ischemia in the emergency department. N Engl J Med. Apr 2000;20;342(16):1163-70.
- Sharkey, SW et al. Impact of the electrocardiogram on the delivery of thrombolytic therapy for acute myocardial infarction. Am J Cardiol. Mar 1994;15;73(8):550-3.
- Martí, D et al. Incidence, angiographic features and outcomes of patients presenting with subtle ST-elevation myocardial infarction. Am Heart J. Dec 2014;168(6):884-90.
- Wang, TY et al. Incidence, distribution, and prognostic impact of occluded culprit arteries among patients with non-ST-elevation acute coronary syndromes undergoing diagnostic angiography. Am Heart J. Apr 2009;157(4):716-23.
- “ECG changes in acute MI”. Doctors Gates Blog. 22 Oct 2015. Web. http://doctorsgates.blogspot.com/2011/01/ecg-changes-in-acute-mi.html
- “Anterior Myocardial Infarction” Life in the Fast Lane Medical Blog. 22 Nov. 2015. Web. http://lifeinthefastlane.com/ecg-library/anterior-stemi/
- “Is the LAD really completely occluded when there are de Winter’s waves? Dr. Smith’s ECG Blog. 22 Nov. 2015. Web. http://hqmeded-ecg.blogspot.com/2014/07/is-lad-really-completely-occluded-when.html.
- Verouden, NJ et al. Persistent precordial “hyperacute” T-waves signify proximal left anterior descending artery occlusion. Heart. 2009 Oct;95(20):1701-6.
- de Winter, RW et al. Precordial junctional ST-segment depression with tall symmetric T-waves signifying proximal LAD occlusion, case reports of STEMI equivalence. J Electrocardiol. 2015 Oct 13.
- “Hyperkalemia” Life in the Fast Lane Medical Blog. 02 Dec 2015. Web. http://lifeinthefastlane.com/hyperkalemia/
- “De Winter’s T-waves”. Life in the Fast Lane Medical Blog. 02 Dec 2015. Web. http://lifeinthefastlane.com/ecg-library/de-winters-t-waves/
- “Wellens’ Syndrome”. Life in the Fast Lane Medical Blog. 02. Dec 2015. Web. http://lifeinthefastlane.com/ecg-library/wellens-syndrome/






3 thoughts on “Subtle ECG findings in ACS: Part II Hyperacute T-Waves”
Great post, a link to part’s I and III might be helpful, as I had hard time searching for them.
Pingback: emDOCs.net – Emergency Medicine EducationECG Pointers: Hyperacute T-Waves - emDOCs.net - Emergency Medicine Education
Pingback: LITFL Review 220 • LITFL Medical Blog • FOAMed Review