Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 57-year-old male presents with hematemesis. He has a history of cirrhosis from alcohol abuse. He appears toxic and is rushed to the resuscitation bay.
Initial VS include T 37.2C, HR 122, BP 88/41, RR 24, SpO2 90% RA.
Exam reveals an ill-appearing patient with intermittent episodes of hematemesis. You rapidly obtain bilateral IV access.
What are your next steps, and what is the likely diagnosis?
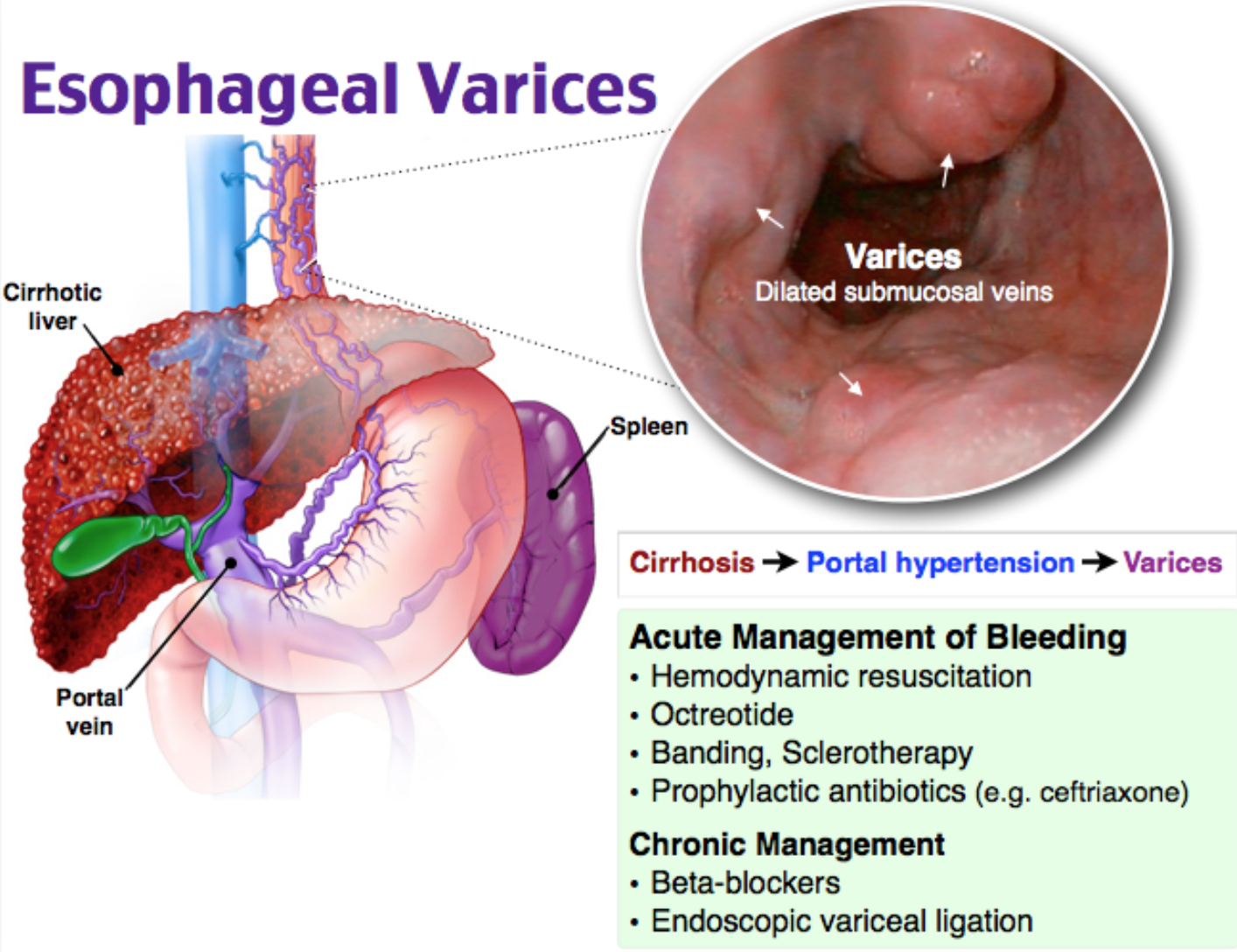
Answer: Gastroesophageal varices, upper GI hemorrhage
- Background: Gastroesophageal varices correlate with severe liver disease and cirrhosis, and bleeding from these varices possesses a mortality rate approaching 20-30%.
- Cirrhosis is the irreversible scarring of the liver, resulting in liver failure. Most commonly results from alcohol abuse and hepatitis B or C, as well as autoimmune disease, NASH, and other diseases.
- This results in increased portal blood flow, increased collateral vessel formation, splanchnic arteriolar vasodilatation, and increased portal flow pressures. These changes in turn are associated with gastroesophageal varices.
- Varices form at a rate of 5-15% per year, and 1/3 of patients with varices will experience hemorrhage over their lifetime.
- Hemorrhage risk is related to vessel wall diameter and wall tension.
- For patients with cirrhosis and upper GI bleed, over 50% of bleeds are due to gastroesophageal varices.
- Bleeding from varices stops spontaneously in 50% of patients (unlike other upper GI bleeds, where the majority stop on their own).
- Patients are often on long-term therapies to reduce portal pressures (nadolol).
- Evaluation: History and exam are important, but may be limited based on patient hemodynamic status.
- History: Prior complications, medications, recent changes in medications, fever, abdominal/chest pain, vomiting, melena, syncope/pre-syncope, hematemesis (bright red or coffee-ground), allergies, surgeries, cause of cirrhosis, prior interventions on varices, weights.
- Exam: Evaluate hemodynamic status immediately. Patients with cirrhosis and liver disease are typically hypotensive at baseline. Look for signs of chronic liver disease – spider angiomata, palmar erythema, jaundice, ascites (shifting dullness, fluid wave, etc.), coagulopathy (petechiae, purpura), ENT exam (pharynx), CV, pulmonary, extremities, mental status.
- Obtain: ECG, CBC, T&S/T&C, renal function, VBG/lactate, CXR, electrolytes, liver function, fibrinogen. NG tube likely not helpful for diagnosis of upper GI bleed.
- Differential Diagnosis: Assume worst first (hemorrhage from varices)! Other causes of upper GI bleed include peptic ulcer disease, gastritis/esophagitis, Mallory-Weiss tear, malignancy, aortoenteric fistula, Boerhaave, malignancy, Dieulafoy’s lesion, angiodysplasia, hemobilia, dengue, pancreatitis, splenic rupture, cavernous hemangiomas.
- Mimics of Upper GI Bleeding: Hemoptysis, ENT bleed (epistaxis), dietary.
- Management: Multiple goals. First obtain bilateral IV access (large bore advised), monitors, supplemental oxygen. Wear personal protective equipment. For more on the sick cirrhotic, see this post.
- Airway: This is one of the most difficult airways to management due to shock state, difficulty with visualization, rapid desaturation with sedative/paralytic, and extensive blood loss.
- Resuscitate before you intubate! (See below).
- Start preoxygenation with NO DESAT (facemask, nasal cannula). Use delayed sequence intubation if needed.
- Use NG tube to decompress stomach (remove the ticking time bomb), but not diagnose upper GI bleed. May use metoclopramide 10 mg or erythromycin 250 mg IV to assist in moving blood through GI tract
- Elevate head of bed 45 degrees. Have multiple section devices ready.
- Use shock-dosed sedative and paralytic.
- If first pass fails, slow and gentle BVM breaths at 10/min. Place in Trendelenberg if vomiting (keep blood out of lungs).
- Use meconium aspirator hooked up to ETT for large bore suctioning.
- Be prepared for SIRS-like response from aspiration, which may require pressors and fluids.
- For more on intubating the hypotensive patient with GI bleed, see these posts: SALAD from EMCrit and EMCrit Episode 5. http://www.emdocs.net/intubating-critically-ill-patient/
- Bleeding and Circulation: Three goals – Resuscitate, Stop the Bleed, Prevent and Treat Complications.
- 1. Hemostatic Resuscitation: Liver produces clotting factors, fibrinolytic proteins, anticoagulants. New hemostatic balance is obtained in chronic liver disease, but much more fragile. Do not rely on PT/PTT/INR to assess coagulation status. See this emDocs post for more. Consider use of TEG instead. Be judicious with fluids and blood, but may need to start Massive Transfusion Protocol (RBC:FFP:Platelets), with cryoprecipitate targeting fibrinogen 150-200 mg/dL. Target Hgb 7 (not reliable in massive bleeding). Use TXA 1g IV. Target resuscitation end points of mentation, capillary refill, MAP, urine output. Avoid over-resuscitation, which can increase portal pressures. Many of these patients are hypotensive at baseline.
- 2. Source Control: Emergency GI and IR consults. EGD within 6-24 hours is associated with reduced mortality and improved outcomes. Resuscitate before endoscopy. May use erythromycin or metoclopramide to improve view for EGD. Use octreotide 50 mcg IV bolus, 50 mcg/hr IV infusion (or vasopressin with nitroglycerin), which is associated with decreased products transfused. EGD fails in 10-20% of cases. Be ready with other devices: Sengstaken-Blakemore, Minnesota, Linton-Nachlas tubes.
- 3. Prevent and Treat Complications: Infection associated with 25-65% of upper GI bleeds from varices (UTI, SBP, pneumonia). Ceftriaxone 1 g IV or cefotaxime 2 g IV associated with NNT of 22 to prevent death and NNT of 4 to prevent infection. Albumin also useful in patients meeting certain criteria (Cr 1.5, BUN > 30, bilirubin > 4). If you have not taken airway, consider in those significantly altered. Consider NG tube placement for stomach decompression. Beware of renal failure and encephalopathy, which are further complications.
- PPI’s do not assist in reducing bleeding from gastroesophageal varices, but can help in reducing stigmata of bleeding from ulcers.
- Please see a prior emDocs post on managing the unstable GI bleeder, with a step-by-step approach: http://www.emdocs.net/unstable-patient-gi-bleed/
- Airway: This is one of the most difficult airways to management due to shock state, difficulty with visualization, rapid desaturation with sedative/paralytic, and extensive blood loss.
- Disposition: Admit patients with upper GI bleed from varices; these patients likely require ICU.

A 62-year-old man with a history of cirrhosis presents after vomiting blood twice. EMS personnel report that the vomit was large in volume and bright red. On inspection, you note caput medusae and palmar erythema. His abdomen is not tender to palpation. His vital signs are stable. Which of the following medications is recommended to help decrease bleeding from the most likely source?
A. Ceftriaxone
B. Octreotide
C. Omeprazole
D. Vasopressin
Answer: B
Patients with evidence of cirrhosis on examination or by history are at risk of developing portal hypertension and subsequent esophageal varices. Bleeding from esophageal varices is a life threatening emergency as patients vomit and lose large quantities of blood. Patients often require aggressive fluid and blood resuscitation in addition to intubation for airway protection. Octreotide is a synthetic octapeptide which acts on somatostatin receptors causing inhibition of the release of chemicals that cause vasodilation of the portal venous system, thereby decreasing blood flow to the varices.
Ceftriaxone (A) is administered prophylactically to patients with variceal bleeding and has been shown to decrease mortality in these patients. With variceal bleeding and cirrhosis, there is an increased risk of bacterial infection associated with worse outcomes. Omeprazole (C) is used in the treatment of upper GI bleeds secondary to peptic ulcer disease. Vasopressin (D) is a potent splanchnic vasoconstrictor not used in the treatment of GI bleeding. At higher doses, it is used as a pressor agent when it acts on peripheral vasoconstrictor receptors.
(No podcast link available)
http://www.emdocs.net/approach-to-the-sick-cirrhotic-patient/
http://www.emdocs.net/intubating-critically-ill-patient/
http://www.emdocs.net/chronic-liver-disease-hemostasis-2/
http://www.emdocs.net/unstable-patient-gi-bleed/
SALAD from EMCrit and EMCrit Episode 5
Emergency Medicine Cases Part 1 and Part 2.
References:
- Long B, Koyfman A. The emergency medicine evaluation and management of the patient with cirrhosis. Am J Emerg Med. 2018 Apr;36(4):689-698.
- Liou IW. Management of end-stage liver disease. Med Clin North Am 2014;98:119–52.
- Garcia-Tsao G, Sanyal AJ, Grace ND, CareyW, Practice Guidelines Committee of the American Association for the Study of Liver Diseases, Practice Parameters Committee of the American College of Gastroenterology. Prevention and management of gastroesophageal varices and variceal hemorrhage in cirrhosis. Hepatology 2007;46(3):922–38.
- Nusrat S, Khan MS, Fazili J, et al. Cirrhosis and its complications: evidence based treatment. World J Gastroenterol 2014 May 14;20(18):5442–60.
- Garcia-Tsao G. Current management of the complications of cirrhosis and portal hypertension: variceal hemorrhage, ascites, and spontaneous bacterial peritonitis. Dig Dis 2016;34:382–6.






