Today on the emDOCs cast with Brit Long, MD (@long_brit), we cover Thunderclap Headache.
Episode 40: Thunderclap Headache
- A thunderclap headache (TCH) is a headache that reaches 7 (out of 10) or more in intensity within less than one minute.
- TCH is often unexpected and not preceded by any warning signs or symptoms. While the duration and location of the headache are important parts of the history, they do not have a role in defining TCH and are nonspecific for TCH. When evaluating a patient with a headache, it is vital the Emergency Physician (EP) determine both the intensity and time it took the headache to reach maximum severity.
- The EP must keep in mind that a normal neurological exam and absence of any associated symptoms does not exclude a serious cause in a patient with a TCH, and the patient still requires a diagnostic workup for potentially deadly pathologic conditions. Pain relief with treatment does not exclude a serious cause.
- The classic teaching in medical school is that a “thunderclap” headache is pathognomonic for subarachnoid hemorrhage (SAH) from a ruptured intracranial aneurysm, but 11-25% of TCHs are due to SAH.
Differential Diagnosis
Subarachnoid Hemorrhage
- Most cases of SAH occur from a ruptured cerebral aneurysm (about 85% of cases), which occur most commonly at branch points in the Circle of Willis.
- The typical presentation of SAH is a sudden, severe headache that the patient describes as “the worst headache of my life.”
- A headache will be the primary symptom of SAH in 70% of patients, of which 50% will present with a TCH.
- The headache usually lasts for several days and very rarely resolves within a few hours.
- Accompanying signs and symptoms include loss of consciousness (one third of patients), seizures (6-9%), delirium (16%), stroke, visual disturbances, N/V, dizziness, neck stiffness, and photophobia.
- As TCH is a common presentation of a SAH, any patient that presents with TCH must be evaluated for SAH due to high morbidity and mortality. About 10% of patients with aneurysmal SAH die prior to hospital arrival, 25% die within the first 24 hours of SAH onset, and 45% die within 30 days.
- A sentinel headache is a headache that occurs days or weeks prior to a ruptured cerebral aneurysm. This is thought to arise from a small leak of blood into the subarachnoid space.
- Signs often accompanying SAH, such as a stiff neck, altered mental status, and focal neurological deficits, are usually absent in a sentinel headache. However, even if these signs are absent the patient still requires evaluation for a SAH.
Cerebral Venous Thrombosis
- A headache occurs in 75-95% of patients with cerebral venous thrombosis (CVT).
- While the onset of headache in CVT is usually gradual, about 2-13% of patients experience a TCH as the primary symptom.
- Other signs and symptoms include seizures (more commonly focal), papilledema, altered mental status, and focal neurological deficits.
- While CVT is a relatively rare disorder, 80% of patients with CVT are younger than 50. CVT is more common in women, especially in the peripartum period and in patients with recent surgery. CVT is also associated with hypercoagulable states including the use of oral contraceptives, hematologic disorders, factor V Leiden, protein C or S deficiency, and anti-thrombin III deficiency.
Cervical Artery Dissection
- A cervical artery dissection can result in an ischemic stroke, transient ischemic attack, or more rarely a SAH.
- Carotid or vertebral artery dissections are an especially important cause of strokes to consider in young and middle aged patients.
- A significant risk factor is a history of neck trauma, which can be minor (e.g. manipulation therapy of the neck or sports-related trauma). Other risk factors include connective tissue disease, large vessel arteriopathies, hypertension, and a history of migraines.
- Headaches are reported in 60-95% of patients with carotid artery dissections and 70% of patients with vertebral artery dissections. While headache onset is typically gradual, TCH occurs in about 20% of patients with a cervical artery dissection.
- According to the International Headache Society’s diagnostic criteria, headaches from cervical artery dissection must be ipsilateral to the dissected artery. The typical first symptom of a cervical artery dissection is unilateral headache (68%), neck pain (39%), or facial pain (10%). The headache from a carotid artery dissection is found most commonly in the frontotemporal region. About 25% of patients will experience a partial Horner’s syndrome (miosis and ptosis).
- A vertebral artery dissection presents with neck pain (66%) and headache (65%), which can be unilateral or bilateral. The headache is more commonly posterior in location.
- Many other symptoms may be present, including facial paresthesia, dizziness, vertigo, nausea/vomiting, visual disturbances (such as diplopia), ataxia, limb weakness or numbness, dysarthria, and hearing loss.
HTN Emergency and Posterior Reversible Encephalopathy Syndrome
- In a hypertensive emergency, while the diastolic pressure is often ≥ 120 mmHg, there is no specific threshold, as different patients will manifest signs of end-organ damage at varying blood pressures. While about 20% of patients with hypertensive crises have associated headaches, most of these are not a TCH but rather a throbbing headache.
- A hypertensive crisis may present with symptoms in addition to headache consistent with end-organ damage. These may include dizziness, dyspnea, vision change, chest pain, psychomotor agitation, change in urine output, fluid overload state, or focal neurological deficits.
- PRES is a clinical syndrome with radiographic findings that presents with headache, seizures, and visual loss often with extreme hypertension. Other symptoms include nausea/vomiting, focal neurological signs, or altered mental status.
- PRES may occur in conjunction with other disorders including eclampsia, thrombotic thrombocytopenic purpura or hemolytic uremic syndrome, and immunosuppressive therapy.
Ischemic Stroke
- About 25-34% of patients with stroke develop an associated headache.
- In 50% of these patients, the headache precedes any other neurological signs or symptoms.
- Typically, the headache is throbbing and ipsilateral to the side of the stroke.
- TCH associated with stroke is rare, but several case reports document patients presenting with TCH due to stroke.
Spontaneous Intracranial Hypotension
- The most common cause of spontaneous intracranial hypotension is CSF leakage from spinal meningeal defects or dural tears.
- This most commonly occurs after lumbar puncture, but can occur from minor trauma such as falls, lifting, coughing, or sports.
- Most commonly intracranial hypotension presents with a positional headache that improves after lying down and worsens when upright. However, 15% of patients will present with TCH.
- Other symptoms associated with spontaneous intracranial hypotension are nausea/vomiting, dizziness, auditory changes, diplopia, visual blurring, interscapular pain, or upper extremity pain.
Infections
- Meningitis can very rarely present with TCH. Consider meningitis if the patient is febrile, at increased risk for infection (immunocompromised), or has features of meningitis (e.g. stiff neck).
Pituitary Apoplexy
- Pituitary apoplexy occurs with hemorrhage or infarction of the pituitary gland.
- This most commonly occurs in the setting of a pituitary adenoma, but may occur in association with pregnancy, general anesthesia, bromocriptine therapy, or pituitary irradiation.
- Pituitary apoplexy usually presents with a combination of acute headache, ophthalmoplegia, decreased visual acuity, reduction in visual fields, and altered mental status. The headache is usually sudden and severe.
Retroclival hematoma
- A retroclival hematoma is usually seen as a rare manifestation of severe head and neck injuries in which there is atlantoaxial dislocation.
Third Ventricle Colloid Cyst
- A colloid cyst of the third ventricle can impede the flow of CSF leading to obstructive hydrocephalus.
- Third ventricle colloid cysts account for 0.5% of intracranial tumors and are most commonly diagnosed between the third and fifth decades of life.
- The most common symptom is headache, which occurs in 68-100% of patients.
- The headache of a third ventricle colloid cyst usually begins abruptly, lasts for seconds up to one day, and resolves quickly.
Temporal Arteritis
- Temporal arteritis is a very rare cause of TCH. Temporal arteritis should be suspected in older patients (>50) complaining of a new onset headache, temporal pain, visual symptoms, or jaw claudication.
- It is also associated with polymyalgia rheumatica, which occurs in 40-50 percent of patients with temporal arteritis.
Reversible Cerebral Vasoconstriction Syndrome
- Reversible Cerebral Vasoconstriction Syndrome (RCVS) includes conditions associated with TCH and diffuse, segmental, reversible vasospasm.
- RCVS is thought to account for most cases of TCH that are termed “benign,” or unexplained.
- Risk factors for RCSV include the postpartum period, history of migraine, and use of pharmacologic agents including ergotamine, triptans, SSRIs, pseudoephedrine, cocaine, amphetamines, ecstasy, cannabis, and bromocriptine.
- The hallmark of RCVS is multiple thunderclap headaches that recur every day or every few days. These headache recurrences can occur for up to four weeks. Other symptoms include altered mental status, motor or sensory deficits, seizures, visual changes, ataxia, speech abnormalities, and N/V.
- While RCVS is usually self-limiting, it is not always benign. A minority of patients can experience residual effects including seizures or strokes.
Evaluation of TCH
- Every patient with TCH must be assumed to have a life-threatening intracranial condition.
- Management of patients presenting with TCH starts with the ABCs. O
- nce the patient is stabilized, diagnostic evaluation is initiated beginning with specific evaluation for SAH.
- The initial imaging modality is a noncontrast head CT. CT scan has a high sensitivity and specificity for SAH. When conducted within 6 hours of onset of TCH, CT has a specificity of 98% and sensitivity nearing 100%. As time from headache onset increases, the sensitivity of CT for SAH declines: 86% on day two, 76% after two days, and 58% after five days.
- Unfortunately, CT can miss many causes of TCH including SAH (especially if after 12 hours), CVT, CVA dissection, acute hypertensive crisis/PRES, intracranial hypotension, meningitis, pituitary apoplexy, and retroclival hematoma. For CVT, the initial CT may be normal in up to 25-30% of patients. In a patient with CVA dissection without an ischemic stroke, head CT is usually normal. CT is typically unrevealing in patients with acute hypertensive crisis, intracranial hypotension, meningitis, pituitary apoplexy, and retroclival hematoma.
- For patients with an acute hypertensive crisis or PRES, while neuroradiographic changes may be apparent on CT, they are best visualized on MRI.
- Some authors recommend always performing a CTA or MRA after negative CT noncontrast. If the patient has a SAH, a CTA can detect a ruptured aneurysm. One method is for the TCH patient to receive a CT and CTA, as CTA will additionally further evaluate for SAH or an aneurysm, CVA dissection, stroke, and RCVS.
- An LP with opening pressure can aid in diagnosis. LP is the gold standard for the diagnosis of SAH, especially if the patient presents after 12 hours of headache onset. CSF studies including glucose, protein, white cells, and differential are used for diagnosing viral and bacterial meningitis. Additionally, opening pressure can be utilized to detect increased or decreased pressures. CVT may be associated with an elevated opening pressure, while intracranial hypotension is associated with a low opening pressure.
- The majority of evidence states that conventional angiography is not necessary in patients with a normal head CT and LP. Angiography has a small risk of transient and permanent neurological complications.
- The role of MRI for imaging of the brain and cerebral vasculature has not yet been defined in patients with TCH, especially in the ED. An MRI can help further evaluate for CVT, pituitary apoplexy, PRES, or intracranial hypotension.
- Even with a thorough workup, studies estimate that a diagnosis is made in only 27-71% of patients with TCH. The most common diagnosed cause of TCH is SAH. Other vascular causes are the second most common diagnosed cause, which includes cervical artery dissection, CVT, and RCVS.
Table 2. Features of TCH that aid with diagnostic evaluation
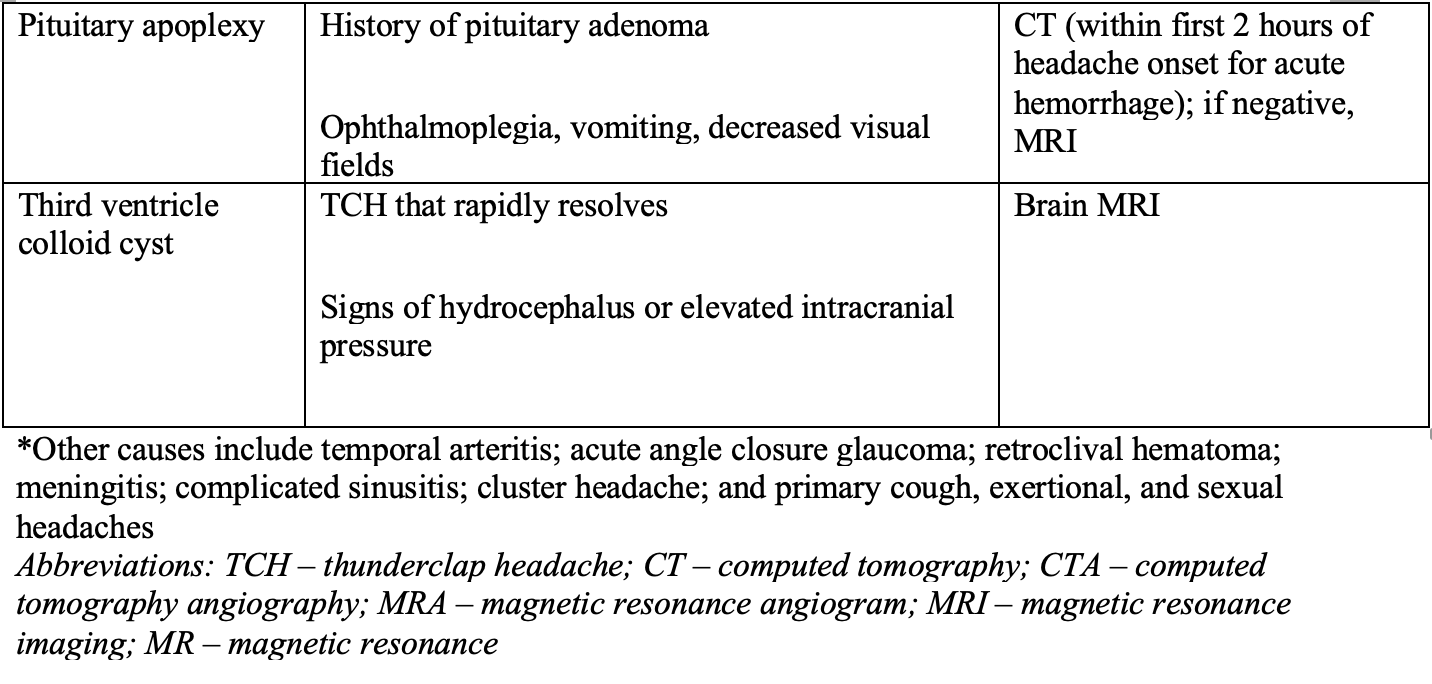
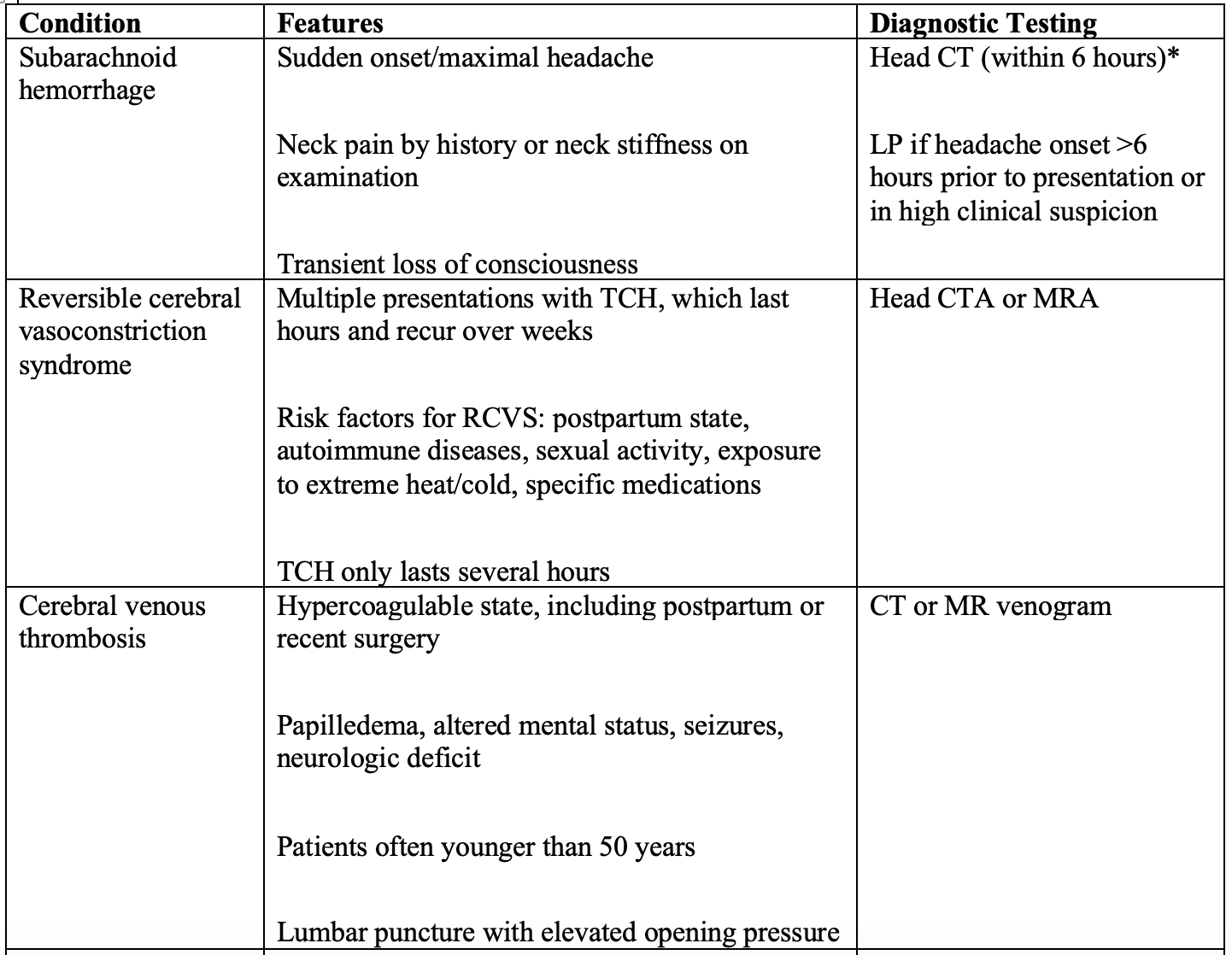
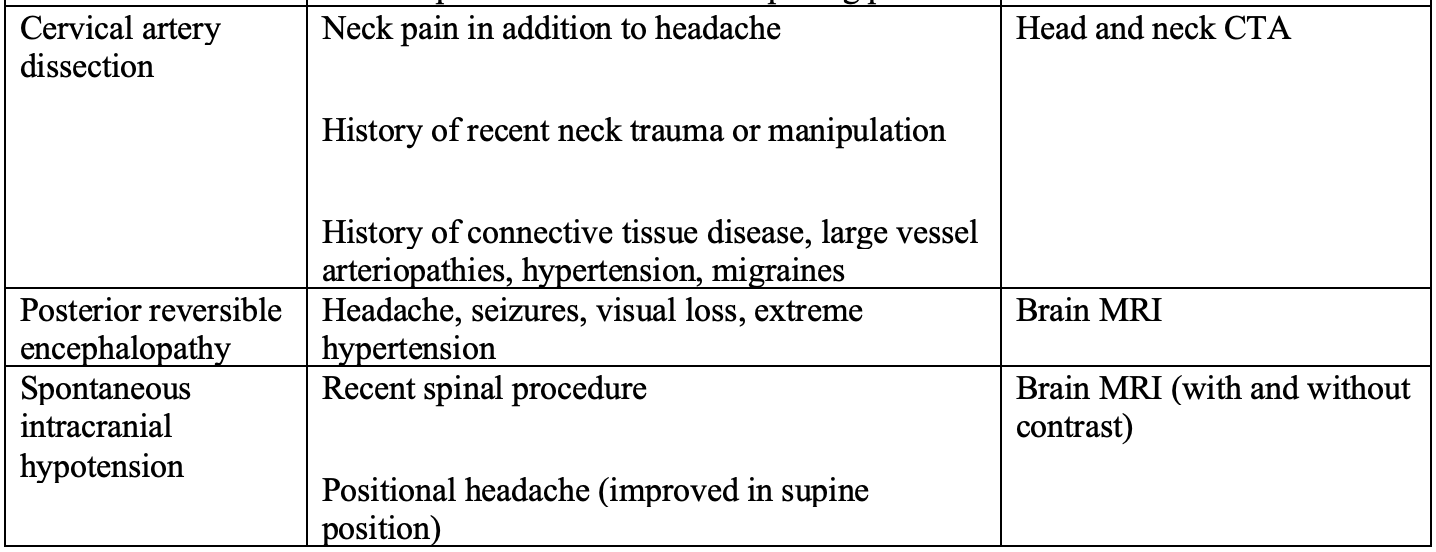

Take Homes
- A thunderclap headache (TCH) is a headache that reaches 7 (out of 10) or more in intensity within less than one minute.
- Every patient presenting with TCH must be assumed to have a life-threatening intracranial condition. As many conditions can present with TCH (most commonly SAH or RCVS), a thorough history is essential in evaluating for risk factors for other conditions.
- The Emergency Physician must keep in mind that the absence of associated symptoms and a normal physical and neurological exam does not exclude a serious cause in a patient with a TCH; the patient still requires a diagnostic workup.
- Due to the high morbidity and mortality of subarachnoid hemorrhage, any patient that presents with TCH must be evaluated for SAH.
- A noncontrast head CT has a sensitivity for SAH nearing 100% if performed within 6 hours of headache onset.
- We recommend TCH patients to receive a CTA with the initial head CT, as this will further evaluate for an aneurysm, cervical artery dissection, stroke, or RCVS.
- Decisions on further imaging and diagnostic evaluation should be made in conjunction with neurology and possibly neurosurgery.










1 thought on “emDOCs Podcast – Episode 40: Thunderclap Headache”
Pingback: Quiz 133, November 12th, 2021 – The FOAMed Quiz