Authors: Lauren Cooke, MD (EM Resident Physician, UTSW Medical Center), Jupin Malhi, MD (Assistant Professor, UTSW Medical Center) // Edited by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case 1
A 27-year-old right hand dominant male presents to the emergency department with left wrist pain. He is accompanied by 3 friends, all of whom were on their way home on electric scooters after a night out. He endorses alcohol use this evening and recalls falling off his scooter and onto his outstretched left hand. He was not wearing a helmet, but denies head trauma. His wrist is tender, mildly swollen, with bony deformity. His x-rays are shown below. Have you seen this patient? What are the most common injuries that occur with electric scooter use?

Case 2
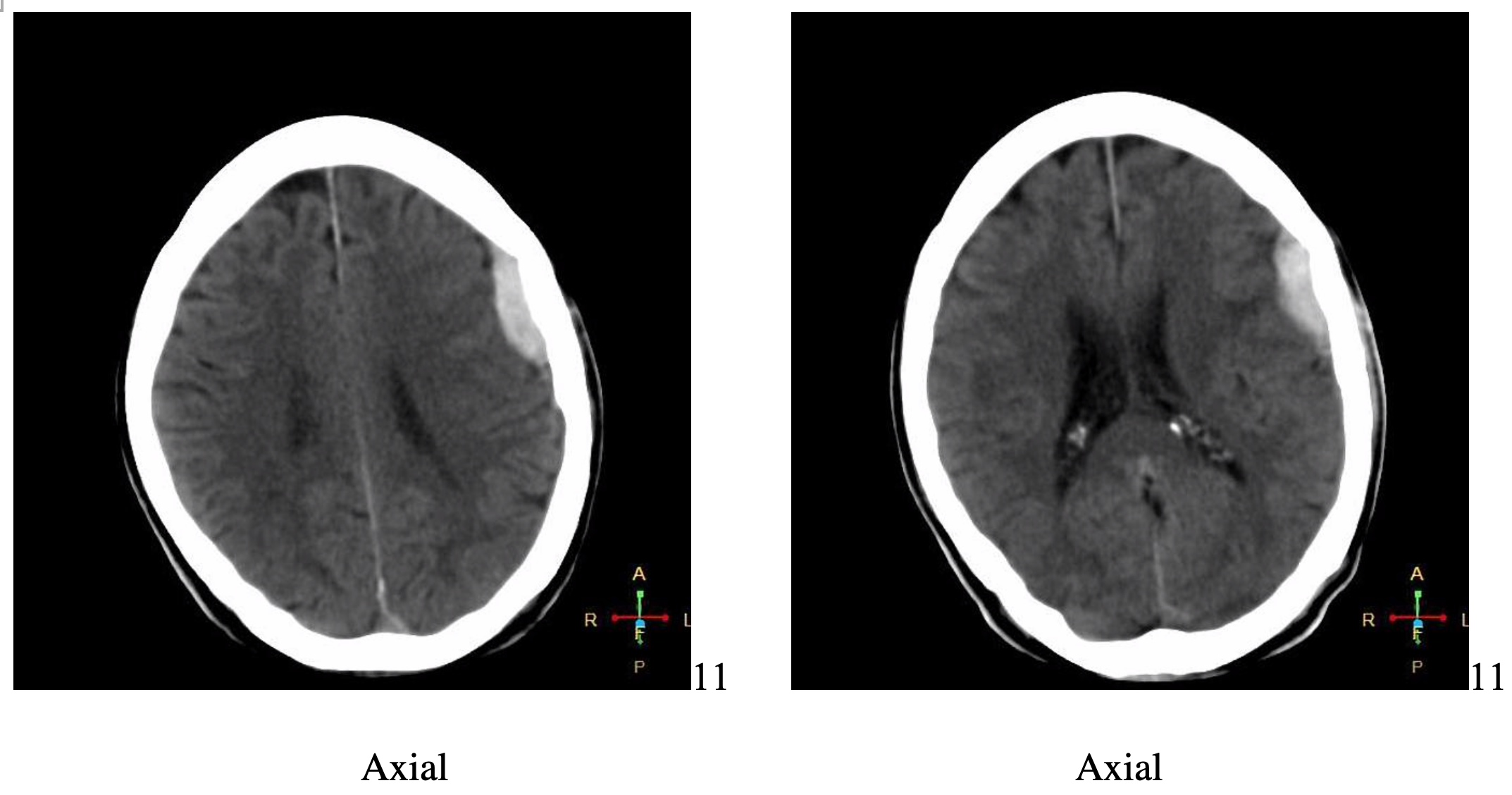
A 63-year-old female with a past medical history of hypertension and osteopenia presents to the emergency department with an eyebrow laceration, hematoma, and headache. She reports that she was walking down the sidewalk yesterday, was at a corner when she was struck by a teen riding an electric scooter, and fell striking the left side of her head on the pavement. Her head CT is shown. How often are pedestrians injured by electric scooters? Are there laws that the teen should have been following that may have protected this patient from her injury?
Introduction
Motorized scooters were initially invented in 1915; however approximately a century later, they have now suddenly come to populate cities across the United States. [1] In July and September of 2017, two rideshare companies, Lime and Bird, introduced thousands of motorized scooters in cities across the U.S., starting initially in San Francisco, Los Angeles, and Washington D.C. [1, 7, 9] These scooters became a popular new mode of transportation seemingly overnight, presumably due to their ease of use, convenience, and low cost. [7, 9] Rideshare companies report >10 million rides since launch. [1, 5] These scooters have been featured frequently in the media, both in positive and negative lights; as both a revolutionary solution to the “last mile” issue of existing public transportation and as a societal nuisance causing a spike in injuries and even several deaths. [1, 4, 5, 6]
Electric scooters are typically scattered throughout a city and are located and unlocked using a downloaded smartphone application. A ride is paid for by the minute, and the ride can be ended anywhere by simply stopping the scooter and closing the ride in the smartphone application. Riders can accelerate or brake using triggers on the handlebars, to a maximum speed of 15-18 mph depending on the scooter model. [6, 8, 9]
In the rental agreement for the smartphone applications, riders must agree to comply with state and local laws, be at least 18 years old, have a valid driver’s license, and use a helmet. [9] There are no standardized federal laws or national policies outlining use requirements for electric scooters. Many states also do not have laws that apply specifically to electric scooter use; by the end of 2018, only 8 states had regulations in place. The laws that do exist typically require riders to wear helmets and outlaw use on sidewalks. However, California recently passed a state law removing helmet regulations for electric scooter riders over the age of 18. [8]
Given the recent spike in popularity of electric scooters, there is a limited amount of formally collected data reflecting riders’ use patterns. However, many riders seem to not comply with the smartphone application agreements or local laws. It appears that riders frequently ride on sidewalks, do not use helmets, and ride the scooters while intoxicated. [1, 2, 3, 7, 9] At UCLA a group of emergency medicine physicians observed a convenience sample of approximately 200 scooter riders in the community surrounding their hospitals and found that 94% of riders did not use a helmet (which was mandated at that time), 8% rode tandem, 9% did not comply with traffic laws, and 26% were riding on the sidewalk where scooter use is prohibited [9]. Each of the other retrospective studies performed reviewing electric scooter use cite that helmets are rarely used, and anywhere from 5% to 16% of patients presenting to emergency departments with injuries were intoxicated. [1, 2, 3, 7, 9]

Demographics
Despite a Consumer Reports study in February 2019 estimating a total of 1,500 electric scooter injuries since late 2017, there have only been a handful of studies performed to evaluate patients presenting to emergency departments with injuries related to e-scooters, most of which have been retrospective studies. [1, 2, 3, 5, 7, 8, 9] The majority of these studies have found that the most patients presenting to emergency departments are white (55% in one study) [1], with a male predominance (50%-61% across 4 studies). [ 1, 2, 7, 9] Although ages of injured patients vary widely, the majority in each study typically occurred in the 18 to 40-year-old age range. [2, 7, 9] Not surprisingly, the studies also found that more patients presented on weekend days compared to weekdays with the majority of patients presenting in the afternoon to evening hours. [1, 7, 9]
Injuries and Injury Patterns
The majority of patients presenting with electric scooter related injuries are riders, though approximately 10% of patients are pedestrians. [9] One study found that of the pedestrians injured, about half were struck by someone on an electric scooter, another quarter tripped over scooters, and the final quarter injured themselves while trying to lift and move a scooter not in use. [9] Those at increased risk of injury as a pedestrian by a motorized scooter include the elderly, young children, those with vision and/or hearing problems, and those distracted by cell phone use. [8]
Injuries to both riders and pedestrians include musculoskeletal injuries, head injuries, superficial soft tissue injury, and major intra-abdominal or intrathoracic injuries. [1, 2, 3, 7, 8, 9] The bulk of injuries are lacerations or extremity injuries, with upper extremity injury occurring more frequently than lower extremity injuries. [1, 7, 9] Spinal fractures can also occur, though more rarely. [7, 8, 9] Fractures are the most common type of injury to expect, however dislocations also occur. [7, 9] Many patients present with lacerations, abrasions or other soft tissue injuries. [1, 2, 3, 9] Patients may also present with intracranial hemorrhage, though minor head injuries including concussions are more common. [1, 2, 3, 7, 8, 9] Though death is rare, notably, an electric scooter rider not wearing a helmet fell off his scooter, struck his head, and died secondary to an intracranial hemorrhage in September 2018. [4, 7] As of June 2019, there have been 8 reported deaths tied to e-scooters in the United States. [4]
The majority of patients presenting to emergency departments following motorized scooter injury are discharged home; however, anywhere from 5% to 33% of patients will require hospital admission. [1, 2, 7, 9] In each study, a couple of patients required ICU care, and a number of patients required surgical interventions. [2, 7, 9]
Case 1, continued
Anyone working in an emergency department in a large city in the United States over the last 2 years has likely seen a patient like this 27-year-old. As in any patient with trauma, history and physical exam are critical. Ask about helmet use, head trauma, alcohol or drug use, scooter speed, and the mechanism of the injury. For any patient that is intoxicated, like this patient, it is highly important to err on the conservative side. If there is any question or sign of head trauma, image the head and c-spine. As demonstrated by the deaths from electric scooter use, the mechanism is significant enough to cause significant injury. [4] Expose the patient, perform a thorough exam, including not just the head and extremities, where this patient has an obvious injury, but also the chest, abdomen, and spine. Though less likely than other injuries, the location of the handlebars makes intra-abdominal and intrathoracic injury possible. [1, 7, 9] Numerous spinal fractures have been documented, and you cannot identify an injury without looking. [7, 8, 9]
After a thorough history and exam, you diagnose your right hand dominant 27-year-old male with a displaced left distal radius fracture. You perform a hematoma block, reduce the fracture, splint the patient, and discharge him with follow up with orthopedic surgery in 1 week. You also educate him on the dangers of electric scooter use while intoxicated without a helmet.

Case 2, continued
This 63-year-old female patient is less common than our 27-year-old; however, as discussed above, a significant portion of patient’s presenting with injuries from electric scooter use are NOT riders. Unfortunately given that many riders are riding scooters on sidewalks, pedestrians are at risk of injury. Additionally, the fact that there does not exist a clear docking location for the scooters puts pedestrians at risk of tripping or running into stationary scooters. Though these pedestrians are not themselves moving at significant speeds, they too are at risk of significant injury. The majority of data does not subdivide injuries of riders versus pedestrians; however, there is a case study of a pedestrian struck by an e-scooter’s handlebars, suffering an acute lumbar compression fracture requiring surgical intervention. [8]
Thus, for this patient, the injured pedestrian, it is just as important to be thorough. This includes all points mentioned above: a thorough history and physical exam with the understanding that the mechanism can indeed cause significant injury.
You find the above epidural hematoma, consult neurosurgery, and your 63-year-old female is admitted to the hospital for observation.
Take home points
- Patients may be both riders as well as pedestrians. Either type of these patients may have significant injury.
- Be sure to ask about helmet use, intoxication, and the mechanism of injury.
- The most common injuries are head injuries and injuries of the upper extremities and distal lower extremities.
- Do a thorough physical exam, and do not forget to expose the patient. Patients may require trauma activation.
References/Further Reading
- Aizpuru M, Farley K, Rojas J, Crawford R, Moore T, Wagner E. Motorized scooter injuries in the era of scooter-shares: A review of the national electronic surveillance system. The American Journal of Emergency Medicine. 2019;37:1133-1138.
- Badeau A, Carman C, Newman M, Steenblik J, Carlson M, Madsen T. Emergency department visits for electric scooter-related injuries after introduction of an urban rental program. The American Journal of Emergency Medicine. 2019 May 16. pii: S0735-6757(19)30297-9.doi: 10.1016/j.ajem.2019.05.003. [Epub ahead of print]
- Bresler A, Hanba C, Svider P, Carron M, Hsueh W, Paskhover B. Craniofacial injuries related to motorized scooter use: A rising epidemic. American Journal of Otolaryngology. 2019 May 20. pii: S0196-0709(19)30421-1. doi: 10.1016/j.amjoto.2019.05.023. [Epub ahead of print]
- Felton, R. 8 Deaths Now Tied to E-Scooters. Consumer Reports. https://www.consumerreports.org/product-safety/deaths-tied-to-e-scooters/. Published June 03, 2019.
- Felton, R. E-Scooter Ride-Share Industry Leaves Injuries and Angered Cities in its Path. Consumer Reports. https://www.consumerreports.org/product-safety/e-scooter-ride-share-industry-leaves-injuries-and-angered-cities-in-its-path/. Published February 06, 2019.
- Felton, R. Safety Glitch Lets Some Shared Electric Scooters Exceed Local Speed Limits. Consumer Reports. https://www.consumerreports.org/product-safety/safety-glitch-lets-some-electric-scooters-exceed-local-speed-limits/. Published June 07, 2019.
- Mayhew L, Bergin C. Impact of e‐scooter injuries on Emergency Department imaging. Journal of Medical Imaging and Radiation Oncology. 2019 Apr 11. doi: 10.1111/1754-9485.12889. [Epub ahead of print]
- Sikka N, Vila C, Stratton M, Ghassemi M, Pourmand A. Sharing the sidewalk: A case of E-scooter related pedestrian injury. The American Journal of Emergency Medicine. 2019 Jun 8. pii: S0735-6757(19)30394-8. doi: 10.1016/j.ajem.2019.06.017. [Epub ahead of print]
- Trivedi TK, Liu C, Antonio AL, Wheaton N, Kreger V, Yap A, Schriger D, Elmore J. Injuries associated with standing electric scooter use. JAMA Network Open. 2019; 2:
- Image courtesy of: Samir, Benoudina, MD, “Distal Third Radial Fracture”,https://radiopaedia.org/cases/distal-third-radius-fracture?lang=us
- Image courtesy of: Abdelmonem, MD, “Epidural Hematoma”. https://radiopaedia.org/cases/epidural-haematoma-5?lang=us
- Image courtesy of Bird Facebook page: https://www.facebook.com/bird
- Image courtesy of Lime: https://www.li.me






